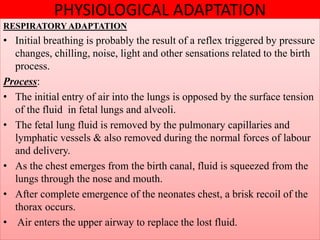
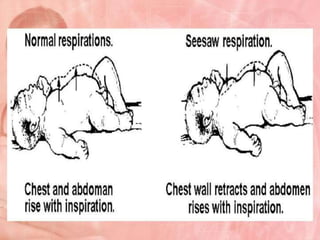
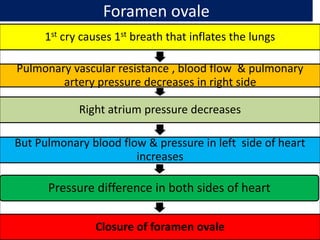
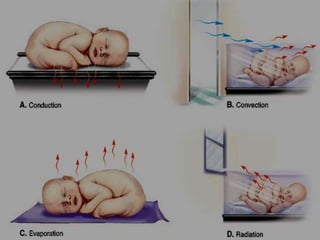
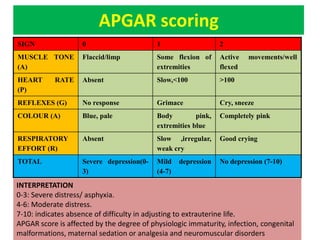
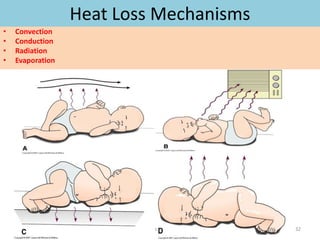
This document provides an overview of assessing and caring for normal newborns. It discusses physiological adaptation after birth including respiratory, cardiovascular, thermoregulation and more. It also covers initial assessment using APGAR scoring, transitional assessment during periods of reactivity, and a full physical examination from head to toe. Key aspects include establishing independent breathing, circulation changes, temperature regulation challenges, and developmental immaturity of various organ systems in the first days of life. Ongoing monitoring of vital signs and growth measurements are also emphasized.