Management of hysteroscopic complication
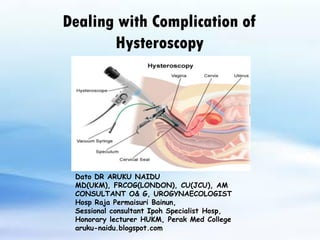
- 1. Dealing with Complication of Hysteroscopy Dato DR ARUKU NAIDU MD(UKM), FRCOG(LONDON), CU(JCU), AM CONSULTANT O& G, UROGYNAECOLOGIST Hosp Raja Permaisuri Bainun, Sessional consultant Ipoh Specialist Hosp, Honorary lecturer HUKM, Perak Med College aruku-naidu.blogspot.com
- 2. Complication of Hysteroscopy • Complication rate 2% ( Assoc. Gynaecologic Laparoscopists, AAGL, 1993) • Prospective randomize trial by Jansen et. Al, 13,600 procedures, Netherland Diagnostic hysteroscopy: 0.13% Operative hysteroscopy: 0.95%
- 3. Complication of hysteroscopy (directly related ) • Cervical injury • Uterine perforation • Haemorrhage • Infection • Injury to bladder, bowel and blood vessels • Thermal damage by electrical current
- 4. • Medical complications resulting from reactions to drugs or anesthetic agents - anaphylaxis • Complications due to distending media – CO2 : Acidosis, Arrhythmia, Embolism – Dextran : Anaphylaxis, Pulmonary oedema – NS: Pulmonary oedema, hyponatraemia – Dextose : Pulmonary oedema, hypoglycaemia Complication of hysteroscopy ( Indirect)
- 5. • Accidental perforation of the uterus is the most common complication • generally diagnosed by direct visualization suspected in cases of unexplained rapid increase in the fluid deficit, uncontrolled hemorrhage, and hemodynamic instability 1. UTERINE PERFORATION
- 6. UTERINE PERFORATION • Can occur during: – Cervical dilatation – Surgery – Retrieval of tissue • Action: – Observation – Laparoscopy – Laparotomy
- 7. Hemostatic uterus perforation By uterine sound, cervical dilator, hysteroscope, or blunt instrument may be managed conservatively: scan to exclude haemorrhage, antibiotics, iv oxytocin Consider Laparoscopy/ Laparotomy if: Perforations through the posterior or lateral uterus sharp or electrocautery instruments - In view of potential for injury to the pelvic viscera or vasculature UTERINE PERFORATION
- 8. 2. Haemorrhage May be encountered during or after hysteroscopy. Exclude uterine perforation 1st Mild bleeding is typically self-limited and generally does not require intervention Electrocautery may be used to coagulate small vessels If conservative approached failed: Foley catheter or intrauterine balloon can be inserted into the cavity and inflated to tamponade the hemorrhage Packing of uterus with roller gauze +/- vasopressin IV oxytocin, inj vasopressin paracervical Rarely embolisation, ligation or hysterctomy
- 9. 3. Injury to viscus/organs Bowel Bladder Omentum Lateral uterine wall ( Haematoma) Can be detected immediately or post-op Direct visualization with hysteroscopy Presence of abd pain, fever, leucocytosis, pertonitis after surgery= injury till proven other vice
- 10. Injury to viscus/organs Bowel The emanation of foul smelling gas through pneumoperitoneal needle is a helpful diagnostic sign Minilaparotomy and repair of perforation Laparoscopically, perforation may be sutured using laparoscopic stapler Colostomy
- 11. Injury to viscus/organs Bladder Diagnosis: appearance of blood and gas on Foley’s catheter bag Check cystoscopy…. Place an indwelling catheter for 7-10 days Prophylaxis antibiotic If defect is larger, repaired by a figure of 8 suture through muscularis of bladder and second suture to close peritoneum
- 12. Complication due to Distending Media 1.Fluid Overload 2.Gases embolism ( Co2, Air)
- 13. Fluid overload may be due to: • Intravasation • Transtubal loss • Uterine perforation 1 2 3 1. Fluid Overload Fluid overload may cause pulmonary edema Mostly occur in cases with excessive intravasation of isotonic fluids
- 14. Mechanism of fluid overload Uterine cavity- a potential space Minimum pressure • 30 mmHg to separate uterine walls • 45-80 mmHg to expand uterine cavity, rarely >100 mmHg MAP ~ 100 mmHg
- 15. Fluid Overload ( 0.2%) Electrolyte free distension media can cause rapid and profound hyponatremia if absorbed in large quantities. • Abrupt changes in the serum sodium level may cause – altered mental status – Seizures – Coma – Death Action: If Na< 125, correct with Intravenous 3% sodium chloride furosemide should be used to achieve the appropriate amount of diuresis.
- 16. FLUID MONITORING DURING HYSTEROSCOPY Inflow/outflow charts Adjust intrauterine pressure Measurement of serum Na+ Measurement of plasma osmolality CVP measurement Patient weight
- 17. 2. CO2 Embolism Symptoms of embolism • A sudden decrease in PCO2, especially when accompanied by a decrease in blood pressure • A decrease in oxygen saturation • Arrhythmias, tachycardia, Cardiovascular collapse • Sustained hypotension not explained by hypovolemia alone • Electrocardiography changes
- 18. Electrocardiographic changes Bradycardia or tachycardia, Premature ventricular contractions Heart block ST-segment depression ECG Monitoring
- 19. If suspected gas embolism (CO2): • Rapid identification, stop procedure • Prevention of further gas entrainment by closing the point of air entry. • give 100% oxygen • Put the patient in a reverse trendelenburg position • The Durant maneuver- With this maneuver the patient is placed on the left side while using Trendelenburg position
- 20. The complication are extremely rare if the correct insufflator is used. The hysteroflator delivers CO2 at a rate of not more than 100ml per minute whereas the laparoflator can deliver 1-6 litres in the same time A laparoflater should NEVER be used for hysteroscopy. Prevention of gas embolism
- 21. Monitoring During Operating Hysteroscopy Standard monitoring • pulse oximetry, • 3-lead electrocardiography, • blood pressure measurements • PCO2 monitoring • standard ventilatory monitoring. • Strict inflow / out flow chart
- 22. Post operative complications Secondary haemorrhage, rare, haemataoma Infection ( 1-2%)= fever & pelvic pain with 72 hrs after hysteroscopy Thermal injuries(Adjacent organs) presence of abd pain, fever, leucocytosis, pertonitis after surgery= injury till proven other vice
- 23. Conclusion • Current hysteroscopic surgery is safe • BUT complications are related to experience of surgeons • Proper instruments essential to reduce complications • Right distention media & right energy source essential • Proper training essential get good outcome & reduce complications
- 24. THANK YOU
