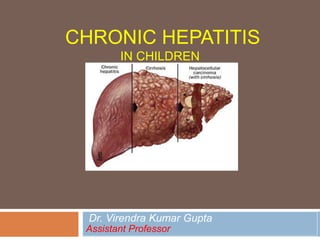
Chronic hepatits in children
- 1. CHRONIC HEPATITIS IN CHILDREN Dr. Virendra Kumar Gupta Assistant Professor
- 2. DEFINITION Chronic hepatitis means ongoing inflammation of the liver persisting for more than six months that is detectable by biochemical and histologic means.
- 3. CAUSES 1.Chronic viral hepatitis Hepatitis B, C, D 2.Autoimmune liver disease Autoimmune hepatitis Sclerosing cholangitis/primary biliary cirrhosis Overlap syndrome with sclerosing cholangitis and autoantibodies Systemic lupus erythematosus Coeliac disease
- 4. 3.Drug-induced hepatitis 4.Metabolic disorders associated with chronic liver disease Wilson disease Nonalcoholic steatohepatitis α1-Antitrypsin deficiency Tyrosinemia Niemann-Pick disease type 2 Glycogen storage disease type iv Cystic fibrosis Galactosemia Bile acid biosynthetic abnormalities
- 6. Clinical presentation Can present with acute decompensation Asymptomatic Signs of chronic liver disease/failure
- 8. Hepatitis B Chronic hepatitis : HBsAg positivity for >6 mo Risk : >90% infected <1yr , 30% children & 2% of adults infected will become chronic carriers. Three phases of this chronic infection include 1. Immunotolerant phase - active viral replication and minimal liver damage.HBsAg & HBeAg are positive and anti Hbe is negative. HBV DNA load is high. ALT normal
- 9. 2. Immuno active phase- host tries to resolve infection HBsAg & HBeAg are positive and anti Hbe is negative. HBV DNA load is low. ALT high & with flares 3. Inactive carrier phase- HBsAg & anti Hbe are positive and HBeAg is negative. HBV DNA load is very low. ALT normal. Sometimes may lead to resolution with HBsAg being negative and Anti HBs positive.
- 10. Symptomatic Infection Chronic Infection Age at Infection Chronic Infection (%) SymptomaticInfection(%) Birth 1-6 months 7-12 months 1-4 years Older Children and Adults 0 20 40 60 80 100100 80 60 40 20 0 Outcome of Hepatitis B Virus Infection by Age at Infection ChronicInfection(%)
- 11. Sexual - sex workers and homosexuals are particular at risk. Parenteral - IVDA, Health Workers are at increased risk. Perinatal - Mothers who are HBeAg positive are much more likely to transmit to their offspring than those who are not. Perinatal transmission is the main means of transmission in high prevalence populations. Hepatitis B Virus Modes of Transmission Keeffe EB, et al. Clin Gastroenterol Hepatol. 2006;4:936–962.
- 12. Diagnostic Interpretations of Hepatitis B markers HBsAg Non infectious component of viral coat Indicator of disease. If > 6 months: chronic HBV Anti-HBs Antibody response to HBsAg Indicates recovery and/or immunity HBeAg Antigen that correlates with replication and infectivity High level of infectivity and replication Anti-HBe Antibody response to HBeAg Decreasing level of replication Remission/resolution Anti-HBc IgM Non protective antibody to the HBcAg Recent HBV infection Anti-HBc IgG As above Remote exposure to HBV HBV DNA Replictative genetic material of HBV; infectious agent Viral replication and continues infection
- 13. Diagnostic Interpretations of Hepatitis B markers HBsAg Non infectious component of viral coat Indicator of disease. If > 6 months: chronic HBV Anti-HBs Antibody response to HBsAg Indicates recovery and/or immunity HBeAg Antigen that correlates with replication and infectivity High level of infectivity and replication Anti-HBe Antibody response to HBeAg Decreasing level of replication Remission/resolution Anti-HBc IgM Non protective antibody to the HBcAg Recent HBV infection Anti-HBc IgG As above Acute or remote exposure to HBV HBV DNA Replictative genetic material of HBV; infectious agent Viral replication and continues infection
- 14. Symptoms HBeAg anti-HBe Total anti-HBc IgM anti-HBc anti-HBsHBsAg 0 4 8 12 16 20 24 28 32 36 52 100 Acute Hepatitis B Virus Infection with Recovery Typical SerologicCourse Weeks after Exposure Titre
- 15. IgM anti-HBc Total anti-HBc HBsAg Acute (6 months) HBeAg Chronic (Years) anti-HBe 0 4 8 12 16 20 24 28 32 36 52 Years Weeks after Titre Progression to Chronic Hepatitis B Virus Infection Typical Serologic Course
- 16. HBV Scenarios HBsAg anti-HBs anti-HBc IgM anti-HBc IgG HBeAg DX + - + + + + - - + + - + - - - - + - + - - - + - - - - - + - Acute infection Carrier Vaccinated Exposed Immune Acute Window Exposed Ab lost
- 17. 17 Possible Outcomes of HBV Infection Acute hepatitis B infection Chronic HBV infection 3-5% of adult- acquired infections 95% of infant- acquired infections Cirrhosis Chronic hepatitis 12-25% in 5 years Liver failureHepatocellular carcinoma Liver transplant 6-15% in 5 years 20-23% in 5 years DeathDeath
- 18. Treatment Only useful for immunoactive phase as it will reduce risk of hepatic cancer and cirrhosis Treatment for children is only by : Interferon(IF alpha 2b,peg IF) AND lamivudine after thorough investigations and classification of stage of disease. Adefovir ,entecavir and tenofovir are used in older children(>12 years)
- 19. Chronic hepatitis C Prevalence low in children Risk of perinatal transmission:5% Increases to 20% if mother coinfected with HIV Poses 85 % risk of developing chronicity but no good evidence in children
- 20. Mostly asymptomatic with fluctuating /normal transaminases levels Slow progression to fibrosis/cirrhosis/CLD Associated with extrahepatic manifestations
- 21. Natural History of Hepatitis C Exposure No infection Acute Chronic Spontaneous clearance (early) •Cirrhosis (20-40%) •HCC (1-4%/year) <75% >20%
- 22. Diagnosis: HCV RNA and genotype , liver biopsy Treatment: PEG INTERFERON ALPHA 2b and RIBAVIRIN (in > 3yrs of age) for 2 year duration
- 23. Autoimmune liver disease Autoimmune liver disease is a clinical constellation that suggests an immune- mediated process characterized by : hypergammaglobulinemia, circulating autoimmune antibodies, necro inflammatory histology & responsive to immunosuppressive therapy . They include autoimmune hepatitis, autoimmune sclerosing cholangitis & de novo hepatitis.
- 24. Pathophysiology Triggering factors : molecular mimicry, infections, drugs, environment (toxins) in a genetically susceptible host Inflammatory cells invades the surrounding parenchyma. HLA DR3, DR4, and DR7 isoforms confer susceptibility to autoimmune hepatitis
- 26. Clinical manifestations Acute viral hepatitis like picture(40%) can progress to ALF esp in Type 2 Insidious onset of liver disease with fatigue, relapsing or prolonged jaundice. Chronic liver disease and its complications Extrahepatic manifestations: arthritis, vasculitis, nephritis, throiditis, anemia, rash
- 27. Management Diagnosis is done by: elevated transaminases, positive auto antibodies , raised gammaglobulins and IgG levels, liver biopsy, absence of known etiology and response to immunosuppressive drugs. Steroids, Azathioprine are first line drugs Cyclosporine and mycophenolate mofetil are second line drugs Liver transplantation as and when required.
- 28. Drug induced liver disease Drugs commonly used in children that can cause chronic liver injury include isoniazid, methyldopa, pemoline, nitrofurantoin, dantrolene, minocycline, pemoline, and the sulfonamides. Anti tubercular and anticonvulsant drugs are major causes Can be chemical hepatotoxicity/idiosyncratic heapatotoxicity
- 29. They can mimic any form of liver disease(acute &chronic hepatitis, ALF, portal hypertension) Good history taking and high index of suspicion is required Treatment is by withdrawal of drug and supportive care
- 30. Metabolic causes Can account for 15-20% of liver diseases in India Most common is Wilsons disease. Most symptoms are due o hepatocyte injury or secondary to hypoglycemia or hyperammonemia Treatment is cause specific.
- 31. Wilsons disease a/k/a hepatolenticular degeneration Toxic accumulation of copper in liver,brain,cornea and other tissues Due to abnormal gene, ATP 7B in chromosome 13
- 32. Clinical features Various forms of hepatic disease: Asymptomatic hepatomegaly subacute/chronic hepatitis Acute hepatic failure with/without hemolytic anemia Others: neuropsychiatric disease, KF Ring,sunflower cataract , coombs negative hemolytic anemia, arthritis, pancreatitis, nephrolithiasis, cardiomyopathy ,endocrinopathies
- 33. diagnosis Serum ceruloplasmin(<20mg/dl) 24 hr urinary copper excretion(>100mcg/day) with penicillamine challenge test(>1600mcg/day) KF ring(slit lamp) Liver biopsy: hepatic copper (>250mcg/g) Family screening
- 34. Treatment Dietary restriction of copper Copper chelating agents(penicillamine/triethylene tetramine hydrochloride, zinc, ammonium tetrathiomolybdenate) Liver transplantation
- 35. Nonalcoholic steatohepatitis Usually associated with obesity and insulin resistance Most children are asymptomatic May have vague abdominal pain. o/e: hepatomegaly , features of insulin resistance like striae, acanthosis nigricans obesity and hepatomegaly. It can progress to cirrhosis.
- 36. Diagnosis is usually clinicopathological correlation . Other causes to be excluded Treatment is by weight reduction and dietary modifications. Ursodeoxycholic acid and vitamin E have promising results
- 37. THANK YOU
