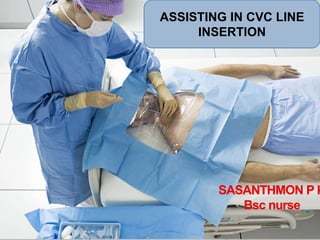
Assisting in CVC Line Insertion: A Guide for Nurses
- 1. ASSISTING IN CVC LINE INSERTION
- 2. DEFINITION A catheter (tube) that is passed through a vein to end up in the thoracic (chest) portion of the vena cava (the large vein returning blood to the heart) or in the right atrium of the heart. ... The central venous line may be inserted for the short term or long term.
- 3. INDICATIONS Central venous pressure monitoring. Emergency venous access (due to difficult peripheral intravenous access) Long-term parenteral nutrition, especially in chronically ill person Long-term pain medications Chemotherapy Drugs that are prone to cause phlebitis in peripheral veins (caustic), such as: Calcium chloride,Chemotherapy Hypertonic salinePotassium chloride (KCl),Amiodarone Vasopressors (for example, epinephrine, dopamine
- 4. ROLE OS ASSISTING NURSE •Assist in positioning the patient as directed depending on the site of insertion. • Jugular/Subclavian - Place the patient in slight trendelenburg or flat, remove head of the bed (optional). May place rolled towel between scapulae. Note: This position distends the vein for easier insertion and decreases the risk of venous air embolism. • Femoral - Place patients flat. •Assist the physician as required with placement of drapes and catheter insertion. •Administer medications as ordered. •Prepare CVP monitoring system for short term CVC
- 5. •Ensure CVC is not accessed until xray of placement is confirmed, or in an emergency until placement is confirmed by blood return. •Document date, time, catheter type (single, multi- lumen), site, physician inserting catheter and patient’s tolerance in the progress notes •Any medications used during the procedure on appropriate record. Report Report to physician any signs or symptoms of complications of insertion: Dyspnea, cardiac arrhythmias, hematoma, excessive bleeding
- 6. THE PHYSICIAN WILL: •Obtain verbal consent and prescribe any medications as needed during the procedure •Optimal positioning of the patient depending on the site of insertion •Perform hand hygiene prior to doing PPE. •Use a 2% chlorhexidine-based antiseptic for skin preparation. Providone-iodine may be used if patient allergic to chlorhexidine. Note: The antiseptic solution must be allowed to dry prior to making the skin puncture. •Full sterile drapes are placed on the client.
- 7. •CVC inserted by physician. •Suture/secure the CVC in place following insertion •Cleanse insertion site with 2% chlorhexidine-based solution following insertion, allow to dry, apply sterile dressing using aseptic technique. •Connect needleless adaptors to each unused lumen. Flush and lock unused lumen(s). • Perform hand hygiene after doffing PPE. •Order X-ray to confirm placement •Prescribe IV solution and rate to commence after x-ray verification of the catheter tip location. •Document procedure in EPR.
- 8. • DISTEL PORT(BROWN)-16 G LEUMEN THE LUMEN THAT OPENS UP AT THE VERY TIP-END OF THE CATHETER IT’S THE LARGEST PORT CVP MONITORING HIGH VOLUME FLUIDS BLOOD SAMPLING • MEDIAL PORTS(BLUE)-18G LEUMEN FOR TPN AND MEDICATIONS • PROXIMAL PORT(WHITE)-18 G LEUMEN MEDICATIONS AND BLOOD PRODUCTS ADMINISTRATION USE OF EACH LEUMEN IN CVC
- 9. NURSING CARE Closely monitor the site of insertion for any redness or discharges. Monitor and record vital signs. Follow strict aseptic techniques to minimize the risk of infection Use transparent dressing to visualize the site. Label the CVC lines with drugs or fluids …etc ,to minimize the risk of accidental boluses. Dressing should be changed whenever soiled ,loose or as per date of dressing. (Tegaderm with Cholrhexidine gel to change after 7 days or whenever soiled)