Exploring the Path Forward in Nontuberculous Mycobacterial Lung Disease: A MasterClass on Risk Factors, Diagnosis, and Treatment
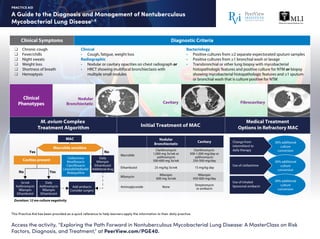
- 1. A Guide to the Diagnosis and Management of Nontuberculous Mycobacterial Lung Disease1-5 PRACTICE AID This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice. Clinical Symptoms Clinical Phenotypes Chronic cough Fever/chills Night sweats Weight loss Shortness of breath Hemoptysis Diagnostic Criteria Clinical • Cough, fatigue, weight loss Radiographic • Nodular or cavitary opacities on chest radiograph or • HRCT showing multifocal bronchiectasis with multiple small nodules Bacteriology • Positive cultures from ≥2 separate expectorated sputum samples • Positive cultures from ≥1 bronchial wash or lavage • Transbronchial or other lung biopsy with mycobacterial histopathologic features and positive culture for NTM or biopsy showing mycobacterial histopathologic features and ≥1 sputum or bronchial wash that is culture positive for NTM Nodular Bronchiectatic Cavitary Fibrocavitary M. avium Complex Treatment Algorithm Initial Treatment of MAC Medical Treatment Options in Refractory MAC MAC Cavities present Yes Yes No No Clofazimine Moxifloxacin Ciprofloxacin Linezolid/tedizolid Bedaquilline Daily Rifampin Ethambutol Additional drug Add amikacin Consider surgery Daily Azithromycin Rifampin Ethambutol 3x/wk Azithromycin Rifampin Ethambutol Macrolide sensitive Nodular Bronchiectatic Cavitary Clarithromycin 1,000 mg 3x/wk or azithromycin 500-600 mg 3x/wk Macrolide Clarithromycin 500-1,000 mg/day or azithromycin 250-500 mg/day 25 mg/kg 3x/wkEthambutol 15 mg/kg day Rifampin 600 mg 3x/wk Rifamycin Rifampin 450-600 mg/day NoneAminoglycoside Streptomycin or amikacin 30% additional culture conversion Change from intermittent to daily therapy 30% additional culture conversion Use of clofazimine 30% additional culture conversion Use of inhaled liposomal amikacin Duration: 12 mo culture negativity Access the activity, “Exploring the Path Forward in Nontuberculous Mycobacterial Lung Disease: A MasterClass on Risk Factors, Diagnosis, and Treatment,” at PeerView.com/PGE40.
- 2. erm(41): erythromycin ribosomal methylase (41); MAC: Mycobacterium aviumcomplex; NTM: nontuberculous mycobacteria. 1. Griffith DE et al. AmJRespirCritCareMed. 2007;175:367-416. 2. Koh WJ et al. AntimicrobAgentsChemother. 2015;59:4994-4996. 3. Jarand J et al. Chest. 2016;149:1285-1293. 4. Olivier KN et al. AmJRespirCritCareMed.2017;195:814-823. 5. Haworth CS et al. Thorax. 2017;72(Suppl 2):ii1-ii64. A Guide to the Diagnosis and Management of Nontuberculous Mycobacterial Lung Disease1-5 PRACTICE AID Treatment of M. abscessus Interpretation of Extended Clarithromycin Susceptibility Results for M. abscessus M. abscessus Subspecies Any M. massiliense M. abscessusa M. abscessus M. bolletii Clarithromycin Susceptibility Days 3-5 Susceptible Resistant Susceptible Resistant Resistant Susceptible Macrolide Susceptibility Phenotype Inducible macrolide resistance High-level constitutive macrolide resistance Macrolide susceptible Genetic Implication 23S ribosomal RNA point mutation Dysfunctional erm(41) gene Functional erm(41) gene Macrolide Effect Immunomodulatory Immunomodulatory Antimycobacterial Clarithromycin Susceptibility Day 14 Macrolide ≥1 other drug IV amikacin M. abscessus Macrolide? ≥2 other drugs IV amikacin Macrolide ≥1 other drug Inhaled amikacin Macrolide? ≥2 other drugs Inhaled amikacin Imipenem (IV) Cefoxitin (IV) Tigecycline (IV) Linezolid/tedizolid Clofazimine Moxifloxacin Bedaquiline Consider surgery for focal disease. Duration: 12 mo culture negativity. “Functional” erm(41) gene Yes No 2+ mo 1-2+ mo M. massiliense M. abscessus M. bolletti a 15%-20% of M. abscessus will have a dysfunctional erm(41) gene (c28 sequevar). Access the activity, “Exploring the Path Forward in Nontuberculous Mycobacterial Lung Disease: A MasterClass on Risk Factors, Diagnosis, and Treatment,” at PeerView.com/PGE40.
- 3. PRACTICE AID This Practice Aid has been provided as a quick resource for healthcare professionals to provide to their patients. Key Facts About NTM Nontuberculous mycobacterium are organisms naturally found in soil and water In some susceptible people, an NTM organism infects the airways and lung tissue leading to disease NTM infections can become chronic and require ongoing treatment Success of your NTM treatment relies on YOU, your healthcare providers, and your medications You can play an ACTIVE ROLE in the progress of your treatment: Engage actively with your healthcare providers; ask questions and keep your doctor informed of any change in your condition Make any necessary lifestyle changes (eg, exercise and hydration) Seek the support of family and friends Implement and adhere to the treatment plan and medications you and your doctor have agreed on, and follow through with full commitment M E D I C A T I O N S You will likely need to take multiple medications for a long period of time. Adhere to your prescribed dosing schedule, and do not stop when you begin to feel better. The doctor will tell you when the bacteria have been controlled long enough to stop taking your medications. Your medications may have some side effects. Call your doctor to discuss any side effects and determine whether any medication or dosage changes are required. If you are having a severe reaction, call your doctor or pharmacist immediately. However, unless your reaction is life-threatening, do not stop taking any of your medications (doing so can lead to your infection becoming drug resistant). Certain combinations of antibiotics work better together because they attack the bacteria in more than one way. Drug combinations are often prescribed to effectively treat a specific strain of NTM. It is important that your sputum samples be sent to a qualified lab for precise species identification and sensitivity testing. Depending on the strain of NTM, medications may be added or changed. Oral (pills, liquids) Make sure you understand how often/what time of day to take the medications and whether they should be taken before, after, or with meals Medications infused by IV via a port or “PICC” line (either hospital or home) Ensure you know how often IV medications need to be administered (duration of treatment may vary from weeks to more than a year) It is important to learn how to care for your central catheter (port or PICC line) to avoid introducing any other infections Inhaled medications (eg, antibiotics, anti-inammatories such as steroids or bronchodilators, which may potentially minimize side effects or complications) Learn how to care for the nebulizer to maintain sterile conditions and avoid introducing other bacteria/infections into your lungs; run the unit to clear and dry the tubing, and sterilize the nebulizer mouthpiece regularly Access the activity, “Exploring the Path Forward in Nontuberculous Mycobacterial Lung Disease: A MasterClass on Risk Factors, Diagnosis, and Treatment,” at PeerView.com/PGE40. Nontuberculous Mycobacterial (NTM) Lung Disease: A Patient’s Guide1,2
- 4. EKGs: electrocardiograms; IV: intravenous; PICC: peripherally inserted central catheter. 1. https://www.ntminfo.org/wp-content/uploads/2018/04/englishpamphlet_ntminfo.pdf. Accessed January 30, 2019. 2. https://www.lung.org/lung-health-and-diseases/lung-disease-lookup/nontuberculosis-mycobacteria/. Accessed January 30, 2019. PRACTICE AID Access the activity, “Exploring the Path Forward in Nontuberculous Mycobacterial Lung Disease: A MasterClass on Risk Factors, Diagnosis, and Treatment,” at PeerView.com/PGE40. Other Important Treatment Elements and Considerations NTM lung disease is a serious infection that can have a significant impact on your life: Join a support group or online support community! NTM Info & Research: https://www.ntminfo.org/forums/ American Lung Association: 1-800-LUNGUSA Hearing, Vision, and Other Testing • Some antibiotics can affect your hearing or vision; ask your doctor about getting baseline tests before beginning treatment • Regular hearing and vision checkups are recommended to ensure any problem is detected before it progresses • Patients with certain heart conditions may be at risk of developing a dangerous irregular heart rhythm when taking some types of antibiotics • Speak with your doctor about getting evaluated for these heart conditions and having regular EKGs, if taking one of these medications Clear Your Lungs and Sinuses (Airway Clearance) • You and your doctor or respiratory therapist may have selected one or more ways to clear the mucus from your lungs: Chest physical therapy with postural drainage Use of an airway clearance device Inhaled saline solution • REMEMBER, every time you cough out infected mucus, there is that much less in your lungs to do damage and that much less for the antibiotics to overcome Stay Well Hydrated • Patients with NTM disease need adequate fluids • Fluid is essential for thinning mucus secretions, which in turn helps you clear mucus from your airways • It also helps the kidneys and liver process medications • Try to minimize drinks such as alcohol, coffee, and tea, which act as diuretics (promote urination) and can result in dehydration Exercise • Exercise is important to help maintain and improve overall endurance • Some patients report that the hard breathing associated with exercise helps them clear their lungs • Weight training can also help your muscles become more efficient at extracting oxygen from the blood • Exercise is a recommended part of most treatment plans, but you must discuss the extent and type with your doctor before starting an exercise regimen Nontuberculous Mycobacterial (NTM) Lung Disease: A Patient’s Guide1,2
