rickets & osteomalacia (1).pptx
- 1. Rickets and Osteomalacia Shekha fathima
- 2. Rickets Disease of the growing skeleton. Characterised by failure of normal mineralisation. Seen prominently at the growth plate. Resulting in softening of the bones and deformities.
- 3. Causes Mainly two types. 1. Type l 2. Type II TYPE I - deficiency of vit D or defect in its metabolism. *Due to deficiency of vit D. -diminished intake eg: malnutrition -diminished absorption eg: lack of 25 hydroxylation of vit D Increased degradation of vit D – anti convulsive therapy Lack of 1 hydroxylation (autosomal recessive)
- 4. Type ll . Defective absorption of phosphates through renal tubules -hypophosphataemic rickets -fanconi syndrome - renal tubular acidosis . Diminished intake or absorption of phosphate. Nutritional deficiency continues to be the most common causes of rickets in developing countries because of poor socio economic conditions.
- 5. Clinical features Craniotabes – pressure over the soft membraneous bones of skull gives the feeling of a ping pong ball being compressed and released. Bossing of skull- bossing of the frontal and parietal bones becomes evident after the age of 6 months. Broadening of ends of long bones-prominently around wrists and knees. Delayed teeth eruption
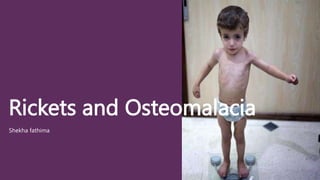
- 6. Harrison’s sulcus- a horizontal depression, along the lower part of the chest corresponding to the insertion of diaphragm. Pigeon chest-The sternum is prominent. Rachitic rosary-The costochondral junctions on anterior chest wall becomes prominent, giving rise to appearance of a rosary. Muscular hypotonia- the child’s abdomen becomes protuberant (pot belly) because of marked muscular hypotonia.Visceroptosis and lumbar lordosis occurs. Deformities –deformities of the long bones resulting in knock knees or bow legs.
- 7. Radiological Features. Delayed appearance of epiphyses. Widening of the epiphyseal plates Cupping of the metaphysis. Splaying of the metaphysis Rarefaction of the diaphyseal cortex occurs late. Bone deformities: knock knees, bow legs, coxa vara.
- 9. Other Investigations Serum calcium- normal or low Serum phosphate – low Serum alkaline phosphate - high
- 10. Treatment Medical and orthopaedic treatment. Medical treatment: . Administration of vit D 6,00,000 units as a single dose induces rapid healing. . If line of healing not seen on x ray within 3-4 weeks of therapy-same dose is repeated. . Child responds to therapy: maintenance dose of 400IU of vit D is given per day. . Child doesn’t respond even after 2nd dose: REFRACTORY RICKETS.
- 11. Orthopaedic Treatment For correction of deformities by conservative or operative methods. A. Conservative methods A. Mild deformities correct spontaneously. B. Designed split(mermaid splint) C. Orthopaedic shoes B. Operative methods A. Moderate or severe deformities require surgery. B. Done after 6 months of starting medical treatment C. Corrective osteotomies done.
- 12. Osteomalacia Adult counterpart of rickets. Softening of bones. Primarily due to deficiency of vit D. Failure to replace the turnover of calcium and phosphorus in the organic matrix of bone. Bone content is demineralised and the bony substance is replaced by soft osteoid tissue
- 13. Etiology Women wearing purda- lack of exposure to sunlight. Dietary deficiency Under nutrition during pregnancy Mal absorption syndrome After partial gastrectomy.
- 14. Clinical features. Bone pains-skeletal discomfort ranging from back ache to diffuse bone pain. Bone tenderness is common. Muscular weakness-patient feels weakness. Difficulty in climbing up and down stairs. Waddling gait. Tetany manifests as carpopedal spasm and facial twitching. Spontaneous fractures- occurs in spine and results in kyphosis.
- 15. Investigations Radiological examinations: 1. Diffuse rarefaction of bones 2. Looser’s zone- radiolucent zones occuring at site of stress. Common sites are pubic rami, axillary border of scapula, ribs and medial cortex of neck of femur. Caused by rapid resorption and slow mineralisation and may be surrounded by a collar of callus. 3. Triradiate pelvis in females. 4. Protrusio-acetabuli i.e. the acetabulum protruding into pelvis. Bone biopsy: Uncalcified osteoids Serum: calcium- low, phosphates- low, alkaline phosphatase- high
- 17. Treatment Due to defective intake: vit D supplementation Vit D daily maintenance dose of 400 IU. In case of malabsorption: high dose or intramuscular dose. In patients with renal disease: alfacalcidol may be used. Calcium supplementation Underlying cause treated.
- 18. THANK YOU