VTE
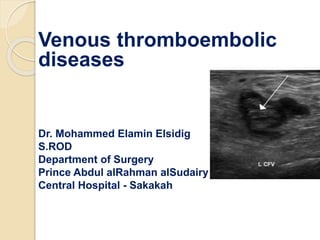
- 1. Venous thromboembolic diseases Dr. Mohammed Elamin Elsidig S.ROD Department of Surgery Prince Abdul alRahman alSudairy Central Hospital - Sakakah
- 3. Key priorities for implementation - Diagnosis - Treatment Pharmacological interventions Thrombolytic therapy Mechanical interventions - Thrombophilia
- 4. Diagnosis Diagnostic investigations for DVT (NICE) signs or symptoms of DVT 1- history and a physical examination 2- two-level DVT Wells score
- 5. Two-level DVT Wells score 1Active cancer (treatment ongoing, within 6 months, or palliative) 1Paralysis, paresis or recent plaster immobilization of the lower limbs 1Recently bedridden for 3 days or more or major surgery within 12 weeks requiring general or regional anesthesia 1Localized tenderness along the distribution of the deep venous system 1Leg swollen (Entire) 1 Calf swelling at least 3 cm larger than asymptomatic side 1 Pitting edema confined to the symptomatic leg 1 Collateral superficial veins (non-varicose) 1 Previously documented DVT 2
- 6. Clinical probability simplified score DVT likely 2 points or more DVT unlikely 1 point or less
- 7. DVT likely Either : Doppler U/S scan within 4 hours. If negative do D- dimer test Or: AD-dimer test and anticoagulant with Doppler u/s within 24 hours.
- 8. Repeat the proximal leg vein Doppler u/s 6–8 days later for all patients with a positive D- dimer test and a negative proximal leg vein Doppler u/s .
- 9. DVT unlikely D-dimer test and if the result is positive Doppler ultrasound scan carried out within 4 hours Parenteral anticoagulant and Doppler u/s within 24 hours
- 10. Consider alternative diagnoses Unlikely Wells score Negative D-dimer test Positive D-dimer test and a negative Doppler u/s. Likely Wells score Negative Doppler u/s + negative D-dimer Repeat negative Doppler u/s
- 11. Advise patients in these two groups that it is not likely they have DVT, and discuss with them the signs and symptoms of DVT and when and where to seek further medical help.
- 12. Diagnostic investigations for PE signs or symptoms of PE 1- history, physical examination and a chest X-ray . 2- two-level PE Wells score to estimate the clinical probability of PE.
- 13. Two-level PE Wells score 3Clinical signs and symptoms of DVT (minimum of leg swelling and pain with palpation of the deep veins) 3An alternative diagnosis is less likely than PE 1.5Heart rate > 100 beats per minute 1.5Immobilisation for more than 3 days or surgery in the previous 4 weeks 1.5Previous DVT/PE 1Haemoptysis 1Malignancy (on treatment, treated in the last 6 months, or palliative)1
- 14. Clinical probability simplified scores PE likely More than 4 points PE unlikely 4 points or less
- 15. PE likely Immediate CTPA parenteral anticoagulant flowed by CTPA , if a CTPA cannot be carried out immediately
- 16. Consider a proximal leg vein ultrasound scan if the CTPA is negative and DVT is suspected.
- 17. PE unlikely a D-dimer positive Immediate CTPA parenteral anticoagulant flowed by CTPA , if a CTPA cannot be carried out immediately
- 18. If not available, ANTICOAGULATE Allergy or risk from irradiation V/Q SPECT V/Q planar scan
- 19. V/Q SPECT
- 20. Diagnose PE and treat patients with a positive CTPA or in whom PE is identified with a V/Q SPECT or planar scan
- 21. Advise these patients that it is not likely they have PE and discuss with them the signs and symptoms of PE, and when and where to seek further medical help. consider alternative diagnoses unlikely Wells score negative D- dimer test positive D- dimer test and a negative CTPA likely Wells score negative CTPA & no suspected DVT
- 22. Treatment (NICE) Pharmacological interventions parenteral anticoagulant DVT OR PE LMWH IN CASE OF Renal impairment or ESRD. Increase risk of bleeding. Hemodynamic instability. UFH
- 23. Start oral VKA and continue parenteral anticoagulant for at least 5 days or until the (INR) is 2 or above for at least 24 hours, whichever is longer. Oral VKA to be started in DVT or PE within 24 hours of diagnosis and continued for 3 months. At 3 months, assess the risks and benefits of continuing VKA treatment .
- 24. Thrombolytic therapy (NICE) CDTT In symptomatic iliofemoral DVT less than 14 days life expectancy of 1 year or more low risk of bleeding good functional status
- 25. Thrombolytic therapy (NICE) PE haemodynamic instability systemic thrombolytic therapy haemodynamic stability NO systemic thrombolytic therapy
- 26. Mechanical interventions (NICE) Compression stockings Wearing for at least 2 years Replaced two or three times per year Worn only on the affected leg Inferior vena caval filters Not tolerate anticoagulation treatment Remove the inferior vena caval filter when the patient becomes eligible for anticoagulation treatment. Recurrent proximal DV Tor PE despite increasing target INR to 3–4
- 27. Patient information (NICE) How to use anticoagulants. Duration. Side effects Adverse effects Monitoring. Effect on dental treatment Taking anticoagulants in pregnancy. effect on sports and travel when and how to seek medical help. 'anticoagulant information booklet' and an 'anticoagulant alert card' Be aware for patients who have concerns about using animal products. Correct application and use of below-knee graduated compression stockings.
- 28. Thrombophilia Congenital Factor V Leiden Protein S deficiency Protein C deficiency Antithrombin III deficiency Familial dysfibrinogenemia Blood group Acquire d Antiphospholipid syndrome HIT Sickle-cell disease Polycythemia Cancer IBD Obesity Pregnancy Unclear elevated levels of: factor VIII factor IX factor XI fibrinogen
- 29. Thrombophilia testing (NICE) Not for patients on anticoagulation treatment. Testing for antiphospholipid antibodies in patients with unprovoked DVT or PE if it is planned to stop anticoagulation treatment. Testing for hereditary thrombophilia in patients with unprovoked DVT or PE and who have a first-degree relative who has had DVT or PE if it is planned to stop anticoagulation treatment. Do not offer to patients with provoked DVT or PE. Not routine in first-degree relatives in DVT or PE pt with thrombophilia.
- 30. Investigations for cancer (NICE) All patients with unprovoked DVT or PE who are not known to have cancer: Physical examination. Chest X-ray. Blood tests. Urinalysis. Consider abdomino-pelvic CT scan (and a mammogram for women) in all patients aged over 40 years with a first unprovoked DVT or PE who do not have signs or symptoms of cancer based on initial investigations.