Leptospirosis Protocol for NABH accredition
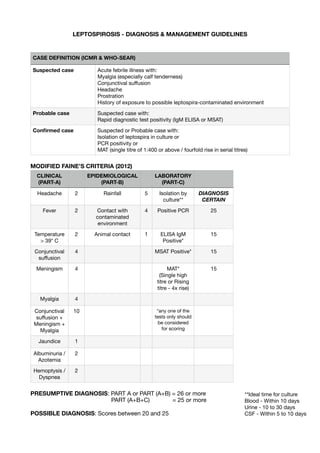
- 1. LEPTOSPIROSIS - DIAGNOSIS & MANAGEMENT GUIDELINES MODIFIED FAINE’S CRITERIA (2012) PRESUMPTIVE DIAGNOSIS: PART A or PART (A+B) = 26 or more PART (A+B+C) = 25 or more POSSIBLE DIAGNOSIS: Scores between 20 and 25 CASE DEFINITION (ICMR & WHO-SEAR) Suspected case Acute febrile illness with: Myalgia (especially calf tenderness) Conjunctival su ff usion Headache Prostration History of exposure to possible leptospira-contaminated environment Probable case Suspected case with: Rapid diagnostic test positivity (IgM ELISA or MSAT) Con fi rmed case Suspected or Probable case with: Isolation of leptospira in culture or PCR positivity or MAT (single titre of 1:400 or above / fourfold rise in serial titres) CLINICAL (PART-A) EPIDEMIOLOGICAL (PART-B) LABORATORY (PART-C) Headache 2 Rainfall 5 Isolation by culture** DIAGNOSIS CERTAIN Fever 2 Contact with contaminated environment 4 Positive PCR 25 Temperature > 39* C 2 Animal contact 1 ELISA IgM Positive* 15 Conjunctival su ff usion 4 MSAT Positive* 15 Meningism 4 MAT* (Single high titre or Rising titre - 4x rise) 15 Myalgia 4 Conjunctival su ff usion + Meningism + Myalgia 10 *any one of the tests only should be considered for scoring Jaundice 1 Albuminuria / Azotemia 2 Hemoptysis / Dyspnea 2 **Ideal time for culture Blood - Within 10 days Urine - 10 to 30 days CSF - Within 5 to 10 days
- 2. Leptospirosis - Suspected / Probable / Con fi rmed 90% of cases are Mild Leptospirosis (Fever, myalgia, conjunctival suffusion, headache BUT NO JAUNDICE) Around 10% cases are Moderate / Severe Leptospirosis (Fever, myalgia, conjunctival suffusion, headache + JAUNDICE +/- Multi-organ involvement Based on clinical spectrum OP Treatment Doxycycline 100mg PO BD x 7 days or Amoxicillin 500mg PO TDS x 7 days or Ampicillin 500mg PO TDS x 7days or Azithromycin 500mg PO OD x 3 days Other supportive Rx* *advise adequate hydration, bed rest, antipyretics etc. RED FLAG SIGNS (tachypnea, tachycardia disproportionate to fever, shock, altered sensorium, oliguria, bleeding manifestations etc.) IP Treatment (Antibiotic Rx +/- Organ speci fi c Rx) Antibiotic therapy: Penicillin 1.5 million units IV QID x 7 days or Ceftriaxone 1g IV BD x 7 days or Doxycycline 200mg IV stat, then 100mg IV BD x 7days (Doxycycline contraindicated in pregnancy) Organ speci fi c therapy: RENAL: renal involvement is common. Mild - only proteinuria and no RFT derangement: No intervention Severe - AKI: Fluid management +/- diuretics, electrolyte correction, avoid nephrotoxic drugs, avoid hypotension and hypovolemia +/- RRT (if indicated by standard RRT guidelines) HEPATIC: acute liver failure is rare. Avoid precipitating factors of hepatic encephalopathy - drugs (hepatotoxic drugs, sedatives etc.), hypovolemia, hypokalemia, alkalosis, constipation, UGI bleeding. Jaundice, Hepatomegaly: No intervention Hepatic encephalopathy: lactulose, rifaximin etc. LUNG: Most dangerous complication ARDS / Pulmonary hemorrhage: Continuous O2 therapy, Mechanical ventilation (if indicated) HEART: Myocarditis / Arrhythmia: treatment of speci fi c arrhythmia Shock: treat hypovolemia with fl uid replacement. If not responding, add dopamine or dobutamine. HEMATOLOGICAL: Thrombocytopenia: Platelet transfusion (if indicated) Coagulopathy: Vit.K 5-10mg IV x 3 days +/- Fresh Frozen Plasma DIC: FFP +/- blood transfusion NEUROLOGICAL: Aseptic meningitis: Symptomatic and supportive management. Hypokalemic paralysis: IV Potassium supplementation MUSCULOSKELETAL: Myalgia / Myositis / Rhabdomyolysis : Monitor CPK levels, adequate hydration, monitor urine output and serum electrolytes. Arthralgia: No intervention +/- analgesic-antipyretics All Absent Any one or more is present Always rule out other tropical diseases. Mixed infections are common. Important differential diagnosis include: -Malaria -Scrub typhus -Dengue -Hepatitis -Enteric fever etc.
- 3. Leptospirosis Zoonotic Pathogenic spirochete – Leptospira interrogans Rodents and Cattle excrete these organisms in their urine, which contaminates soil and waterbodies Mode of transmission: contact of abraded skin or mucous membrane with contaminated environment Incubation period: Average 5-14 days with a range 2- 30 days Risk factors: o Heavy rainfall and water logging o Natural disasters like floods o Seasonal – at the onset of monsoon o Farmers o Agricultural field workers o Fishermen o Sewer workers o Livestock handlers o Mason o Residence in endemic area Presentation spectrum: o Anicteric Leptospirosis: (90%) – Mild form presents like Acute undifferentiated fever o Icteric Leptospirosis: (5-10%) – Moderate-Severe form o Weil’s Disease (0-5%) – Severe form When to suspect Leptospirosis? o Acute febrile illness + Risk factors + one or more of the following: Headache Myalgia Prostration Calf muscle tenderness Conjunctival suffusion Oliguria / Frothy urine Jaundice Haemorrhagic manifestations Meningeal irritation Nausea, Vomiting, Abdominal pain, Diarrhoea Lab investigations to support diagnosis: (Blood, CSF, Urine sample) o MAT titre of 100/200/400 or above based on endemicity (preferred) o IgM based immune assays o Seroconversion or Four-fold rise in MAT titre between acute and convalescent sera o Direct isolation of organism o PCR test
- 4. Lab investigations to assess severity: o CBC, ESR o RFT, LFT o S. Electrolytes o Urine Routine examination o CPK o CXR, ABG Management: o IVF and correction of electrolytes o Mild cases: Tab. Doxycycline 100mg PO BD X 7 days (preferred) or Tab. Azithromycin 500mg PO OD X 3 days o Moderate / Severe cases: Inj. Penicillin 1.5 million units IV or IM Q6H X 7 days or Inj. Ceftriaxone 2g IV OD X 7 days o Chemoprophylaxis: Tab. Doxycycline 200mg PO once a week or Tab. Azithromycin 250mg PO once/ twice a week
- 5. DIAGNOSTIC: A + B = /> 26 OR A + B + C = /> 25 POSSIBLE: A + B = Between 20 to 25 CRITERIA
