case NEC 1.pptx
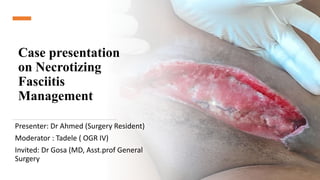
- 1. Case presentation on Necrotizing Fasciitis Management Presenter: Dr Ahmed (Surgery Resident) Moderator : Tadele ( OGR IV) Invited: Dr Gosa (MD, Asst.prof General Surgery
- 2. Objective Case Summary Discussion References Contents Dr Ahmed NEC 2 4/28/2023
- 3. Case Presentation On Necrotizing Fasciitis
- 4. Objective
- 5. Objective To discuss on management necrotizing Fasciitis taking case as entry point Dr Ahmed NEC 5 4/28/2023
- 6. Case summary
- 7. Case Summary
- 8. Case Summary • Identification:- • Name M.N • Age :31 year • Residency : Wanji • Marital status: Married • MRN:1321024 • Date of admission :23/07/2015 • Date of discharge : 12/08/2015 Dr Ahmed NEC 8 4/28/2023
- 9. Case summary C/C: Surgical wound discharge/3days HPP • P I(CD alive) mother on 8th Post op day after LUST C/S was done for indication of prolonged LFSOL +NRFHP(P. tachycardia) • Currently she come with referral with the Dx. of SSI+ abdominal cellulitis +8th post C/D • She has hx of pain & offensive discharge from surgical site. • She has hx of high grade intermittent fever, chills and riggers Dr Ahmed NEC 9 4/28/2023
- 10. cont’d • Otherwise she has no hx of • headache ,epigastric pain and bluring of vision • No hx urinary frequency, urgency • No hx of hypertension and DM Dr Ahmed NEC 10 4/28/2023
- 11. Physical examination G/A: ASL V/S BP= BP=90/60mmHg PR=102/min RR=22 T=37.5 HEENT: pale conjunctiva, NIS ABD: Tenderness and darkish skin discoloration which started from edge of incision site on lower abd. Indurated skin and crepitation on palpation with offensive discharge from surgical site, 18 weeks sized uterus and contracted Dr Ahmed NEC 11 4/28/2023
- 12. cont’d GUS: Offensive discharge on examining finger with cervical motion tenderness MS=No deformity and no edema CN/S: COTPP Pelvic U/S • Uterus empty • Measure 12cmx9cm • 8x4cm of pelvic collection Dr Ahmed NEC 12 4/28/2023
- 13. Cont’d • Ass= : Deep SSI with pelvic collection+ ?Necrotizing fasciitis + Puerperal sepsis 2 to endomyometritis + 8th post C/D Plan –To do CBC,BG, Prepare for re-laparotomy + debridement Consult surgical side Ceftriaxone 1gm IV BID Metronidazole 500mg IV TID Gentamycin 80mg IV TID Dr Ahmed NEC CBC: WBC=7.4000, G=78.8%, HGB =9.2g/dl, PLT=215 13 4/28/2023
- 14. Operation note • Operation Note written as usual. • Type of Anesthesia:-General Anesthesia • Type of operation:-Debridement and lavage • Indication: Deep SSI with necrotizing fasciitis Dr Ahmed NEC 14 4/28/2023
- 15. • Intra OP Findings • There was around 300ml of offensive puss in the pelvic cavity, • with darkish necrotic tissue involved skin, • subcutaneous tissue and fascia on lower abdomen more on Rt side • Uterus & incision site of Uterus & bowel looks normal 4/28/2023 Dr Ahmed NEC 15
- 16. Cont’d • Done : • Puss was sucked out • Debridement of necrotic tissue • The wound was thoroughly washed with H2O2 and normal saline • Drainage tube was kept • Fascia was approximated • Wound left open for wound care and dressed Dr Ahmed NEC 16 4/28/2023
- 17. Post op order • Keep NPO till bowel active • MF:NS,DNS,RL over 24 hour • Ceftrazone 1gm IV BID • Metrinidazole 500mg IV TID • Gentamycin 80mg IV TID • Tramadol 100mg IV TID • Diclofenac 75mg IMBID • Wound care after 24 hours and then BID Dr Ahmed NEC 17 4/28/2023
- 18. Vital signs 23 to 30/7/2015 Dr Ahmed NEC 18 4/28/2023
- 19. Vital sign follow up chart 1/8/15-09/8/15 4/28/2023 Dr Ahmed NEC 19
- 20. Progress note • Progress note was written on, 25,28/7/15 & 2/08/15 and there is no derangement interms of V/S & clinical status of the patient & she was improving • IV antibiotics was discontinued on 02/08/15. • The wound was on a daily wound care with wet to dry dressings applied and after surgical re-assessment, confirmed that the wound is clean and ready for closure, on 15 days postoperatively Dr Ahmed NEC 20 4/28/2023
- 21. Progress • The wound was finally closed with using delayed primary closure17 days postoperatively • The patient was discharged 19 days after the operation with follow up appointment. Dr Ahmed NEC 21 4/28/2023
- 22. Case Discussion
- 23. List of problems Necrotizing fasciitis Deep SSI Puerperal sepsis Dr Ahmed NEC EPIDEMIOLOGY PRESENTATION RISK FACTORS INVESTIGATIONS 23 4/28/2023
- 24. Introduction Dr Ahmed NEC • NF is a rapidly progressive soft tissue infection that involves the superficial and deep fascia, • leading to thrombosis of the cutaneous vessels and gangrene of the underlying tissue. • Is also known as flesh-eating disease • Initially, the overlying tissue can appear unaffected which makes difficult to diagnose without direct visualization of the fascia. 24 4/28/2023
- 25. Epidemiology Dr Ahmed NEC • It is a rare infection • Estimated incidence of 0.4 per 100,000 in the general population and a mortality rate of up to 34% • Both sexes are affected equally • Become more severe in older and immune compromised 25 4/28/2023
- 26. Epidemiology Dr Ahmed NEC • Necrotizing fasciitis had been earlier described by Hippocrates in the 5th century BC. • Its association with caesarean section was first reported 1962. • Since then, in an 8-year retrospective analysis of 5048 caesarean deliveries reported 9 cases, giving an incidence rate of 1.8 per 1000 caesarean deliveries. 26 4/28/2023
- 27. Case report of necrotizing fasciitis after caesarean Article May 2017 • 19-year-old para II mother. On her 4th pod after CS • She complained of lower abdominal pains. • On examination, she was afebrile (temperature 37.1°C); other vital signs were within normal ranges. • The incision site was clean with no evidence of surgical site infection. • She was managed with analgesics (tramadol) and ampicillin was continued as part of her routine postoperative care. 4/28/2023 Dr Ahmed NEC 27
- 28. Cont’d • By day 5 postop, she developed an acute abdomen. • The incision site had become very tender and soft tissue crepitation was noted on either side of the incision • Investigated with WBC=39.800cells/mm3, RBS=116mg/dl, HIV negative, HGB=8.3g/dl • A decision to do an exploratory laparotomy was taken. 4/28/2023 Dr Ahmed NEC 28
- 29. Operation note • Upon reopening the lower segment incision (Pfannenstiel) • IOF • A pungent and offensive greenish seropurulent discharge oozed from the site. • Revealed abundant foul smelling ascites and an extensive spread of greyish necrotic tissues involving the skin, subcutaneous tissue, recti muscles, fascia, and anterior serosa of myometrium. • The hysterotomy site was nondraining and hyperemic. 4/28/2023 Dr Ahmed NEC 29
- 30. Done: • An intraoperative diagnosis of necrotizing fasciitis was made. • All necrotic tissues were excised; • Peritoneal cavity was thoroughly washed out. • Two drainage tubes were also inserted. • Anterior abdominal wound was left open to heal by secondary intention. 4/28/2023 Dr Ahmed NEC 30
- 31. Done: • She was transfused a whole blood in the immediate postoperative period. • Empiric broad spectrum intravenous antibiotics (metronidazole, ceftriaxone, and gentamycin) • Daily wound care was kept 4/28/2023 Dr Ahmed NEC 31
- 32. • She was deteriorated subsequently (septic shock) managed by continuation of empiric antibiotics and IV crystalloids: • There was abundant drainage, and continual progression of necrosis, • the wound was extensively debrided approximately 2 cm beyond the bleeding edges to ensure adequate resection on day 6 after laparotomy. • The large defect with neither recti muscles nor fascia was covered with the improvised abdominal mop after each daily wound dressing 4/28/2023 Dr Ahmed NEC 32
- 33. • Finally as routine daily wound care did not show further necrosis, and there were decreased drainage and a marked improvement in her overall clinical status. • In addition to her regular daily meals, & nutritional support. • Two weeks after extensive debridement, a granulating and healthy looking wound was seen. • By the 15th week, the abdominal defect had closed. • She was discharged to be followed up on an outpatient basis 4/28/2023 Dr Ahmed NEC 33
- 34. Presentation Dr Ahmed NEC Symptoms • early • localized abscess or cellulitis with rapid progression • minimal swelling • no trauma or discoloration • late findings • severe pain • high fever, chills and rigors • tachycardia. 34 4/28/2023
- 35. Presentation Dr Ahmed NEC Physical exam • skin bullae • discoloration • ischemic patches • cutaneous gangrene • swelling, edema • dermal induration and erythema • subcutaneous emphysema (gas producing organisms) 35 4/28/2023
- 36. Risk factors & Etiology • immune suppression • diabetes • AIDS • cancer • obesity • bacterial introduction • IV drug use • hypodermic therapeutic injections • insect bites • skin abrasions • Abdominal and perineal surgery In obstetrics, it can follow cesarean delivery but can also • Complicate perineal wounds • Episiotomies • Vulvar infections in diabetic and immunosuppressed women. Dr Ahmed NEC 36 4/28/2023
- 37. Classification Dr Ahmed NEC • Based on the microbiological pathogens, necrotizing fasciitis is classified into 4types 37 4/28/2023
- 38. Dr Ahmed NEC • Is caused by aerobic and anaerobic bacteria. • At least one anaerobic species most commonly • Bacteroides, Clostridium, or Peptostreptococcus is isolated • In combination with Enterobacteriaceae eg Escherichia coli, Enterobacter, Klebsiella, Proteus • And one or more facultative anaerobic streptococci (other than group A Streptococcus [GAS]) . Type I (poly microbial) 38 4/28/2023
- 39. Dr Ahmed NEC • Obligate aerobes (such as Pseudomonas aeruginosa) are rarely components of such mixed infections. • Uncommonly, fungi (predominately Candida species) are recovered in (type I) necrotizing infection 39 4/28/2023
- 40. Dr Ahmed NEC • Usually caused by GAS or other beta-hemolytic streptococci. • Infection may also occur as a result of Staphylococcus aureus • Infection with no clear portal of entry occurs in about half of cases • In such circumstances, the pathogenesis of infection likely consists of hematogenous translocation of GAS from the throat (asymptomatic or symptomatic pharyngitis) to a site of blunt trauma or muscle strain. • Cause toxic shock syndrome Monomicrobial (type II) 40 4/28/2023
- 41. Dr Ahmed NEC • The causes of type III necrotizing infection include • Vibrio vulnificus • Gramm negative rods • Infections due to these pathogens typically occur in the setting of traumatic injury associated with sea water. Type IV • MRSA Type III 41 4/28/2023
- 42. Investigations • Blood cultures (two sets) should be obtained prior to administration of antimicrobial therapy. • Reasonable serum laboratory testing includes • CBC, RBS, Chemistries. Liver function tests , Creatinine, Coagulation studies, Creatine kinase concentration, Lactate concentration, and inflammatory markers (C-reactive protein and/or erythrocyte sedimentation rate). Dr Ahmed NEC 42 4/28/2023
- 43. LRINEC Scoring system • score > 6 has PPV of 92% of having necrotizing fasciitis • CRP (mg/L) • ≥150: 4 points • WBC count (×103/mm3) • <15: 0 points • 15–25: 1 point • >25: 2 points Dr Ahmed NEC 43 4/28/2023 • Hemoglobin (g/dL) • >13.5: 0 points • 11–13.5: 1 point • <11: 2 points • Sodium (mmol/L) • <135: 2 points • Creatinine (umol/L) • >141: 2 points • Glucose (mmol/L) • >10: 1 point
- 44. Investigations • Radiologic studies are only considered as adjunct measures for doubtful cases and cannot be used to exclude NF. • A plain X-ray could show subcutaneous gas. • CT-scan and MRI images could show asymmetrical fascial thickening, fat stranding, and gas tracking along fascial planes. • A gas on plain was revealed only 35% of radiographic studies. Dr Ahmed NEC 44 4/28/2023
- 45. • Biopsy • emergent frozen section can confirm diagnosis in early cases • histological findings • necrosis of fascial layer • microorganisms within fascial layer • PMN infiltration • fibrinous thrombi in arteries and veins and necrosis of arterial and venous walls Dr Ahmed NEC 45 4/28/2023
- 46. Why is early diagnosis important? • Delays in diagnosis associated with increased morbidity and mortality • Predictors of mortality in NF : – Time to first debridement – Extent of tissue involvement – # Failed organs on admission – Inadequate first debridement – Age > 60 years – Bacteremia – Elevated lactate Dr Ahmed NEC 46 4/28/2023
- 47. Treatment Dr Ahmed NEC • NF is a medical emergency requiring prompt surgical exploration and administration of intravenous broad spectrum antibiotics. • Aggressive and extensive debridement is the mainstay of treatment. 47 4/28/2023
- 48. Antibiotics Dr Ahmed NEC • At the initiation of surgery, and with re-dosing intraoperative, as determined by the length of the procedure. • Acceptable empiric antibiotic regimens include • A carbapenem or beta-lactam-beta-lactamase inhibitor plus • An agent with activity against methicillin- resistant S. aureus (MRSA; such as vancomycin or linezolid plus Clindamycin, for its antitoxin effects against toxin-elaborating strains of streptococci and staphylococci (600 to 900 mg intravenously [IV] every eight hours in adults; 48 4/28/2023
- 49. Approach to Surgical Debridement Dr Ahmed NEC • OR as soon as the diagnosis is suspected • Approach based upon tissues involved • A circular pattern of debridement is advocated, starting at the most severely involved region and progressively working outwards until healthy soft tissue is encountered • Ensure adequate tissue perfusion and viability • Prevent fluid pooling or collections • Re-evaluate/return to OR in 24 hour • Operative exploration is the gold standard modality for diagnosis of NF 49 4/28/2023
- 50. Approach to Surgical Debridement Dr Ahmed NEC • Intravascular volume should be maintained with infusions of crystalloid, • Electrolyte abnormalities should be corrected. • The abdominal wall, rectus sheath, omentum, diverting colostomy for perineal/perianal involvement and hysterectomy are also required for extensive treatment, however in some cases reported preservation of uterine. 50 4/28/2023
- 51. Approach to Surgical Debridement Dr Ahmed NEC • At the initial and each subsequent debridement, specimens at the margins of the wound should also be sent for pathologic examination • Once the debridement is completed, an antiseptic dressing should be applied. • We use an initial dressing of sodium hypochlorite 0.025% (1:20 Dakin solution [ie, 0.5% sodium hypochlorite] diluted in sterile water or saline), covered by absorptive layers of gauze secured in place. 51 4/28/2023
- 52. Approach to Surgical Debridement Dr Ahmed NEC Does time to re-debridement matter? 64 patients with NF at USC-LAC over 6 years Practice algorithms by 2 different services Short duration (24-48 hrs) vs Extended duration (> 48 hrs) until second debridement Short duration associated with lower AKI and mortality 52 4/28/2023
- 53. Conclusion • Necrotizing fasciitis is a rapidly progressive, often lethal, infectious disease process that requires early aggressive debridement. • Any patient with inordinate pain and edema in the pelvis, especially in the puerperium, should be suspected of having this disease 4/28/2023 Dr Ahmed NEC 53
- 54. Cont’d • Radiographic studies are often diagnostic of this condition. • The triad of, pain of out of proportion, edema, and any sign of septicemia carries an extremely grave prognosis and mandates immediate surgical intervention. 4/28/2023 Dr Ahmed NEC 54
- 55. comments • Strength • Diagnosis of necrotizing fasciitis to OR time is early • Surgical side involved in management • Antibiotic started early Dr Ahmed NEC 55 4/28/2023
- 56. comments • Weakness • Basic Investigations not determined • RBS • OFT, • C-reactive protein (CRP) • Lactate • procalcitonin (PCT) • Sample was not sent to pathology • Drug sensitivity culture not done • Resuscitation points not mentioned Dr Ahmed NEC 56 4/28/2023
- 57. Reference Dr Ahmed NEC • Schwartz’s Principles of Surgery 11th Edition • Sabiston Textbook of Surgery 21st Edition • Bailey and love’s short practice of surgery • Uptodate 2022 • American journal of obstetrics and gynecology, 57 4/28/2023
Editor's Notes
- Necrotizing soft tissue infection was first documented by Fornier in1883. However, the term of necrotizing fasciitis (NF) was first used by Wilson in 1952.
- Necrotizing soft tissue infection was first documented by Fornier in1883. However, the term of necrotizing fasciitis (NF) was first used by Wilson in 1952.
- Necrotizing soft tissue infection was first documented by Fornier in1883. However, the term of necrotizing fasciitis (NF) was first used by Wilson in 1952.
- Necrotizing soft tissue infection was first documented by Fornier in1883. However, the term of necrotizing fasciitis (NF) was first used by Wilson in 1952.
- Necrotizing soft tissue infection was first documented by Fornier in1883. However, the term of necrotizing fasciitis (NF) was first used by Wilson in 1952.
- NF is difficult to diagnose in the early stage because of nonspecific signs such as tenderness, swelling, erythema, and pain at the affected site that mimic non-severe soft tissue infection. Severe pain and systemic toxicity should rise the suspicion of NF in advanced patients.
- NF is difficult to diagnose in the early stage because of nonspecific signs such as tenderness, swelling, erythema, and pain at the affected site that mimic non-severe soft tissue infection. Severe pain and systemic toxicity should rise the suspicion of NF in advanced patients.