Patent-Ductus-Arteriosis-Discuss.pptx
- 2. • Patent ductus arteriosus (PDA) is a persistent opening between the two major blood vessels leading from the heart. Where this connection doesn't close after birth as it's supposed to. This means that extra blood is pumped into the lungs, forcing the heart and lungs to work harder. • A small patent ductus arteriosus often doesn't cause problems and might never need treatment. However, a large patent ductus arteriosus left untreated can allow poorly oxygenated blood to flow in the wrong direction, weakening the heart muscle and causing heart failure and other complications. • Treatment options for a patent ductus arteriosus include monitoring, medications, and closure by cardiac catheterization or surgery.
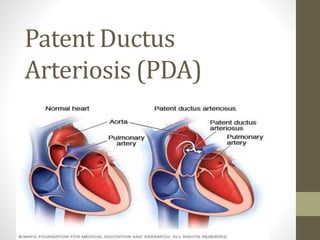
- 3. PATHOPHYSIOLOGY Schematic diagram of a left-to-right shunt of blood flow from the descending aorta via the patent ductus arteriosus (PDA) to the main pulmonary artery.
- 4. • Closing the PDA can now usually be performed by catheter coil placement or other device insertion to plug the abnormal communication. • Surgery may be the best treatment option for some patients. • An incision is made in the left side of the chest, between the ribs. The PDA is closed by tying it with suture (thread-like material) or by permanently placing a small metal clip around the PDA to squeeze it closed. Occasionally in the adult, a surgical patch is used. If there's no other heart defect, this restores the circulation to normal.
- 5. Symptoms • Patent ductus arteriosus symptoms vary with the size of the defect and whether the baby is full term or premature. A small PDA might cause no signs or symptoms and go undetected for some time — even until adulthood. A large PDA can cause signs of heart failure soon after birth. • Your baby's doctor might first suspect a heart defect during a regular checkup after hearing a heart murmur while listening to your baby's heart through a stethoscope. • A large PDA found during infancy or childhood might cause: • Poor eating, which leads to poor growth • Sweating with crying or eating • Persistent fast breathing or breathlessness • Easy tiring • Rapid heart rate
- 6. Causes • Congenital heart defects arise from problems early in the heart's development — but there's often no clear cause. Genetic factors might play a role. • Before birth, a vascular connection (ductus arteriosus) between two major blood vessels leading from the heart — the aorta and pulmonary artery — is necessary for a baby's blood circulation. The ductus arteriosus diverts blood from a baby's lungs while they develop, and the baby receives oxygen from the mother's circulation. • After birth, the ductus arteriosus normally closes within two or three days. In premature infants, the connection often takes longer to close. If the connection remains open, it's referred to as a patent ductus arteriosus. • The abnormal opening causes too much blood to circulate to the baby's lungs and heart. Untreated, the blood pressure in the baby's lungs might increase (pulmonary hypertension) and the baby's heart might enlarge and weaken.
- 7. Risk factors • Risk factors for having a patent ductus arteriosus include: • Premature birth. Patent ductus arteriosus (PDA) occurs more commonly in babies who are born too early than in babies who are born full term. • Family history and other genetic conditions. A family history of heart defects and other genetic conditions, such as Down syndrome, increase the risk of having a PDA. • Rubella infection during pregnancy. If you contract German measles (rubella) during pregnancy, your baby's risk of heart defects increases. The rubella virus crosses the placenta and spreads through the baby's circulatory system, damaging blood vessels and organs, including the heart. • Being born at a high altitude. Babies born above 10,000 feet (3,048 meters) have a greater risk of a PDA than babies born at lower altitudes. • Being female. PDA is twice as common in girls.
- 8. Prevention There's no sure way to prevent having a baby with a patent ductus arteriosus. However, it's important to do everything possible to have a healthy pregnancy. Here are some of the basics: • Seek early prenatal care, even before you're pregnant. Quitting smoking, reducing stress, stopping birth control — these are all things to talk to your doctor about before you get pregnant. Also discuss medications you're taking. • Eat a healthy diet. Include a vitamin supplement that contains folic acid. • Exercise regularly. Work with your doctor to develop an exercise plan that's right for you. • Avoid risks. These include harmful substances such as alcohol, cigarettes and illegal drugs. Also avoid hot tubs and saunas. • Avoid infections. Update your vaccinations before becoming pregnant. Certain types of infections can be harmful to a developing baby. • Keep diabetes under control. If you have diabetes, work with your doctor to manage the condition before and during pregnancy.
- 9. NURSING MANAGEMENT AND CONSIDERATIONS • Medical Follow-up Patients with a small PDA need periodic follow-up with a cardiologist. • Activity Restrictions Most patients with a small unrepaired PDA or a repaired PDA don't need any special precautions and can participate in normal activities without increased risk. Limitations on physical activity for a short time even if there's no pulmonary hypertension. • Exercise restriction is recommended for patients with pulmonary hypertension related to PDA.