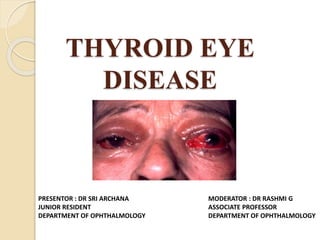
Thyroid eye disease
- 1. THYROID EYE DISEASE MODERATOR : DR RASHMI G ASSOCIATE PROFESSOR DEPARTMENT OF OPHTHALMOLOGY PRESENTOR : DR SRI ARCHANA JUNIOR RESIDENT DEPARTMENT OF OPHTHALMOLOGY
- 2. INTRODUCTION • Thyroid eye disease (TED) is an autoimmune inflammatory disorder . • It is also called as Thyroid orbitopathy, Thyroid associated ophthalmopathy (TAO), Thyroid ophthalmopathy • It is the commonest cause of both unilateral and bilateral proptosis in adults
- 3. RISK FACTORS Fourth to fifth decade Female to Maleratio4:1 Cigarette smoking ( modifiable risk factor) Treatment with radioactive iodine
- 4. ETIOLOGY Graves’ disease (90%) Euthyroidism (6%) Hyperthyroidism – other causes (Toxic nodular goiter, Hashimoto’s thyroiditis (3%), Factitious hyperthyroidism, Thyroid malignancy) Hypothyroidism (1%)
- 5. PATHOGENISIS Thyroid eye disease is an organ specific autoimmune- mediated inflammation of the extraocular muscle and periorbital connective tissue. Target antigen is shared between thyroid follicular cells and orbital fibroblast Orbital fibroblast are the primary target of inflammatory attack
- 6. Lymphocytic infiltration of orbital tissue Release of cytokines (IL – 1) Stimulation of fibroblasts, Proinflamatory genes upregualted(IL6,IL8,PGE2) Synthesis of Glicosaminoglycans(GAG) Hyaluronan attracts water, GAG accumulates in fatty connective tissue Increase in osmotic load Muscle odema, Proptosis, Fibrosis of muscle fibres, Atrophy
- 7. PATHOGENISIS
- 8. GROSS PATHOLOGY EOM enlargement confined to bellies and sparing tendons
- 9. HISTOPATHOLOGY The extraocular muscle fibres are separated by an accumulation of granular material consisting of collagen fibrils and glycosaminoglycans, among which hyaluronan predominates Focal and perivascular inflammatory mononuclear cell Muscle replaced by fibrous connective tissue with a scattering of mononuclear inflammatory cells in late disease
- 10. CLINICAL PRESENTATION • Retrobulbar discomfort • Grittiness • Red eyes • Lacrimation • Photophobia • Puffy lids
- 11. EYE SIGNS FACIAL SIGN: Joffroy’s sign—Absent creases in the forehead on superior gaze. JOFFROY’S SIGN
- 12. EYELID SIGNS • Kocher’s sign—Staring appearance • Vigouroux sign—Eyelid fullness or puffiness • Rosenbach’s sign—Tremors of eyelids (when closed) • Riesman’s sign—Bruit over the eyelids KOCHER’S SIGN VIGOUROUX SIGN
- 13. UPPER EYE LID SIGNS • Von Graefe’s sign—Upper lid lag on downgaze • Dalrymple’s sign—Upper eyelid retraction • Stellwag’s sign—Incomplete and infrequent blinking • Grove sign—Resistance to pulling the retracted upper lid VON GRAEFE’S SIGN DALRYMPLE’S SIGN
- 14. • Boston sign—Uneven, jerky movements of the upper lid on inferior gaze • Gellinek’s sign—Abnormal pigmentation of the upper lid • Gifford’s sign—Difficulty in everting the upper lid • Means sign—Increase superior scleral show on upgaze GELLINEK’S SIGN GIFFORD’S SIGN
- 15. LOWER EYE LID SIGNS • Enroth’s sign—Edema of the lower lid • Griffith’s sign—Lower lid lag on upward gaze. ENROTH’S SIGN
- 16. EXTRAOCULAR MOVEMENT SIGNS • Moebius’ sign—Unable to converge eyes • Ballet’s sign—Restriction of one or more extra ocular muscle • Suker’s sign—Poor fixation on abduction • Jendrassik’s sign—Paralysis of all EOMs. MOEBIUS’ SIGN BALLET’S SIGN
- 17. CONJUNCTIVAL SIGNS • Goldzeiher’s sign—Conjunctival injection. PUPILLARY INVOLVEMENT SIGNS • Knies’ sign—Uneven pupillary dilatation in dim light • Cowen’s sign—Jerky contraction of pupil to light. KNIES’ SIGN
- 18. Soft tissue involvement Periorbital and lid swelling Chemosis Conjunctival hyperaemia Superior limbic keratoconjunctivitis
- 19. EYELID SIGNS Eyelid retraction (mc clinical feature) Retraction due to - Sympathetic overstimulation of Muller’s muscle - Fibrotic contracture of the levator palpebrae and inferior rectus muscles - Secondary overaction in response to hypo- or hypertropia produced by fibrosis.
- 20. Marginal reflex distance (MRD) MEASURMENT OF LID RETRACTION
- 21. PROPTOSIS • Occurs in about 50% • Axial, unilateral/bilateral •Symmetrical or asymmetrical •Patients < 40 years of age are more likely to exhibit proptosis related to fat expansion in the apparent absence of muscle involvement
- 22. PLASTIC RULER LUEDDE’S EXOPHTHALMOMETER HERTEL’S EXOPHTHALMOMETER CLINICAL METHODS FOR MEASUREMENT OF PROPTOSIS NAUGLE’S EXOPHTHALMOMTER
- 23. RESTRICTIVE MYOPATHY 30% to 50% of cases Ocular motility initially restricted by inflammatory edema and later by fibrosis Involvement of the inferior, medial, superior, and lateral rectus muscle are encountered in decreasing frequency
- 24. RESTRICTIVE MYOPATHY Elevation defect Abduction defect Depression defect Adduction defect
- 25. OPTIC NEUROPATHY 5% of cases Compression of optic nerve or its blood supply at the orbital apex by congested and enlarged recti and swollen orbital tissue Visual acuity is reduced Colour desaturation Visual Field defects : central and paracentral scotoma
- 26. GRADING SEVERITY Werner’s Classification: Class 0- No signs and symptoms Class 1- Only signs Class 2- Soft tissue involvement Class 3- Proptosis Class 4- EOM involvement Class 5- Corneal involvement Class 6- Sight loss due to optic neuropathy It is not useful for determining the severity of the disease, for prognostication, or for planning management.
- 27. VISA CLASSIFICATION It has been proposed for classifying severity of disease Each category has subjective and objective items, and each category is scored both by the clinician and the patient The management is decided according to the score in each category V—Vision, and Assessment of Optic Neuropathy I—Inflammation S—Strabismus A—Appearance (Proptosis, Lid Retraction) and Exposure
- 28. CLINICAL ACTIVITY SCORE (CAS) Described to measure the activity of disease at a given time. Total score is noted by giving a score of 1 for each of the following features CAS >= 3/10 suggests active TED
- 29. EUGOGO CLASSIFICATION Severity of the Ophthalmopathy. Management depends on degree of severity of the ophthalmopathy The disease is classified as 1. Mild TED: characteristics of TED have a minimum impact on the patient's life present with one or more of the following signs: • Minor lid retraction ( <2 mm). • Mild soft tissue involvement.
- 30. Exophthalmos <3 mm Transient or no diplopia. Corneal exposure responsive to lubricants. 2. Moderate-to-severe TED : - Patients without sight-threatening TED - Eye disease has sufficient impact on daily life to justify the risks of immunosuppression ( if active) or surgical intervention (if inactive). Patients usually present one or more of the following signs: • Lid retraction (>2mm). • Moderate or severe soft tissue involvement.
- 31. Exophthalmos >3 mm • Inconstant, or constant diplopia. 3 Sight threatening TED: patients with • Dysthyroid optic neuropathy • Corneal breakdown due to severe exposure • Severe forms of frozen eye • Choroidal folds This category warrants immediate intervention .
- 32. CLINICAL COURSE TED is a self-limiting disease, becoming quiescent within 3–5 years of its onset 1. Congestive or Active phase : - Lasts for 6-18 months - Characterized by active inflammation with marked lid edema, conjunctival chemosis and congestion and increasing exophthalmos 2. Static phase : majority of cases, starts to regress and most of the signs slowly settle down.
- 33. 3. Fibrotic or Inactive phase: - Also known as quiescent or burnt-out phase, ensues after the regression phase. - In this phase, eyes are white, however, a painless motility defect may be present.
- 34. INVESTIGATION Biochemical Profile Thyroid stimulating hormone Free and total triiodothyronine Free and total thyroxine Thyroid hormone binding ratio (THBR) Radioiodine uptake (RAIU) Imaging Magnetic resonance imaging Computed tomography scanning Ultrasonography
- 35. CT ORBIT CT is helpful in assessing the relationship between the EOM and optic nerve at the orbital apex and can aid in surgical planning Allows identification of even minimally enlarged recti There is bilateral fusiform enlargement of the extra-ocular muscles, with smooth borders and sparing of the tendons, is the classic finding ( Coca-cola sign)
- 37. MRI ORBIT •MRI helps to identify the typical fusiform rectus muscle enlargement and orbital fat expansion •Helps in early diagnosis of compressive optic neuropathy
- 38. USG B - SCAN •B scan can demonstrate inflammatory changes which occur in orbital fat and extraocular muscles
- 39. MANAGEMENT Management of thyroid eye disease includes : Supportive therapy during the active phase Management of sight-threatening conditions in severe disease Functional and cosmetic rehabilitation during the quiescent phase
- 40. MANAGEMENT PLAN FOR THYROID EYE DISEASE Mild to moderate disease, within first year of onset: - Stop smoking - Lubricants - Elevate head end of bed - Cool compresses Severe sight threatening disorder at any point (optic neuropathy, exposure keratitis): - Systemic steroids–methylprednisolone - Tarsorrhaphy or induction of ptosis with botulinum toxin.
- 41. If severe disease is non-responsive to medical therapy - Surgical decompression, orbital radiotherapy. Moderate or severe disease, stable, inactive is treated with surgical correction. - Orbital decompression - Extraocular muscle surgery - Lid correction.
- 42. Use of steroids: Benefit from intravenous methyl-prednisolone, 1 gm per day for three days. A recurrent disease may need pulse doses of steroids every three to six weeks. Less severe disease may respond to oral steroids( Prednisone 1mg/kg/day then taper ) Intra-orbital injection of long-acting steroid such as Triamcinolone 40 mg may have some beneficial effect.
- 43. Use of immunosuppressants: Patients not responding to steroids, or intolerant of steroids - Methotrexate (7.5–15 mg one day a week) - Azathioprine (initial dose 1.0 mg/kg/day, increased weekly till minimum effective dose is achieved) - Cyclophosphamide (0.1–0.2 mg/kg/day). These drugs have serious side effects, and need to be used with careful monitoring under supervision
- 44. Radiotherapy: A dose of 2000 cGy used It may act by decreasing the T lymphocyte population in the orbit. Radiation is contraindicated in diabetic patients, as it can adversely affect the retinopathy.
- 45. SURGICAL MANAGEMENT Orbital decompression Extraocular muscle surgery Eyelid surgery
- 46. ORBITAL DECOMPRESSION Expands the orbital volume to create more space for swollen soft tissues Primary indications for orbital decompression - Compressive optic neuropathy - Excessive proptosis (can manifest as globe subluxation, corneal ulceration, and cosmetic disfigurement) - Steroid dependence - Intractable pain
- 47. Types ◦ Two – wall : floor and medial wall (3–7 mm) ◦ Three – wall : floor, medial and lateral wall (6–10 mm) ◦ Four – wall : floor, medial and lateral walls with part of sphenoid (apex) and lateral part orbital roof (10–17 mm)
- 49. STRABISMUS SURGERY Goal of strabismus treatment is to achieve single binocular vision in primary and downgaze positions TED quiescent with stable eye muscle function without corticosteroids for at least 6 months The most frequently performed surgical procedure strabismus is recession of the restricted medial rectus or inferior rectus muscle
- 50. EYELID SURGERY Lagophthalmos can be treated in the active phase by Botulinum toxin injection In the stable phase, levator recession, or lid lengthening by use of spacers Indications for repair -ocular discomfort -keratitis, -corneal ulceration -cosmesis.
- 51. Eyelid surgery should be undertaken after orbital decompression and extraocular muscle surgery, because both procedures can affect eyelid position Upper eyelid retraction is treated by recessing Müller’s muscle and/or the levator aponeurosis. Lower eyelid retraction and lower eyelid entropion are treated by recessing the lower eyelid retractors
- 52. REFERENCES Principle and practice of ophthalmology by Albert and Jakobie’s Volume 3 , Edition 3 Comprehensive Ophthalmology by A K Khurana, 7th Edition Kanski’s Clinical Ophthalmology 9th edition Postgraduate Ophthalmology by Zia Chaudhuri, First Edition
- 53. THANK YOU