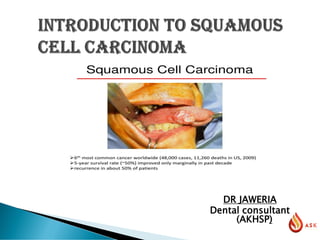
"Oral Squamous Cell Carcinoma"
- 2. SQUAMOUS CELL CARCINOMA Introduction Epidemiology Clinical Features Diagnosis Treatment plan
- 3. Definition: It’s a malignant neoplasm of stratified squamous epithelium in the oral cavity capable of local destructive growth and distant metastasis.
- 4. Epidemiology: Accounts for 90% or more of all oral malignant neoplasms. 30-40% occurs in South East Asia. Incidence rates tend to be higher in urban as opposed to rural communities. Fourth commonest cancer in men and sixth commonest in women. Sixth commonest form of malignant disease in both sexes. Eighth in incidence for all cancers in developed countries
- 5. Third in incidence in developing countries. 98% of patients are over the age of 40. More common in men. Incidence of oral cancer rises steeply with age and with an ageing population. May occur on any part of the oral mucosa, but buccal mucosa is the most frequent site.
- 6. Possible aetiological factors: Tobacco smoking in the form of pipes, cigars cigarettes, bidis, reverse smoking.40 cigarettes/day, R/R increaes upto 10 to 20 times Smokeless tobacco in the form of snuff dipping, tobacco sachets and tobacco chewing like betel chewing and betel quid. Smoking is considered to be a major aetiological factor, particularly in association with alcohol. Main carcinogens in tobacco are N-nitrosamines derived from nicotine Alcohol may enhance transport of carcinogens across mucosal barrier.
- 7. Nutritional deficiencies in alcoholics may impair mucosal barrier. Deficiencies of Vitamin A,C,E and iron are contributory factors. High fruit consumption decreases the risk of oral cancer. Poor oral hygiene, faulty restorations, sharp edges of teeth and ill fitting dentures. Sun/ultraviolet light is thought to be an important factor. Human papilloma viruses (HPV) types 16 and 18, Epstien-Barr virus (EBV) and Human immunodeficiency virus (HIV) are an important factor Immunosuppression
- 8. Genetic mutations are responsible for generation of malignant cells. Mutation may resuklts in abnormal quantity and/or function of protein products that regulate cell growth , division and repair.
- 9. Oncogenes These are abnormal form of normal genes (protooncogenes) that regulate cell growth. These genes encode for range of growth- promoting proteins found in normal cells. - GFR protein - signal transmitting protein - stimulatory cell cycle regulating proteins - Growth factors - intracellular signal transduction pathways
- 10. Are inherent genes that play a role in cell division and DNA repair and are critical for detecting in appropriate growth signals in cells. If they are mutated genetic mutation in other genes can proceed unchecked, leading to neoplastic transformation.
- 11. Tumour suppressor-genes that encode for growth inhibitory protiens. - p 53 - p 54 Under normal circumstances cellular proliferation is controlled by the balance between these growth- promoting and growth-inhibiting genes.
- 12. During carcinogenesis a proto-oncogene may undergo mutation and become an activated oncogene resulting an enhanced activity and tumour formation.
- 13. Clinical Presentation: Early lesions are usually asymptomatic. White patch with small exophytic growth which in the early stages may show no uleration or erythema. Small indolent ulcer or an area of erythroplakia. Pain is seldom present. Persistent ulceration, induration and fixation of affected tissue to underlying structures and underlying bone destructions should arouse suspicion of an early carcinoma.
- 14. Unusual surface changes sudden tooth mobility without apparent cause Unusual oral bleeding or epistaxis Prolonged hoarseness of voice
- 15. as an exophytic growth
- 16. As carcinoma enlarges it may develop into a raised nodule or become ulcerated. Induration results from inflammation and fibrosis and infiltration of the tissues. By the time a carcinoma has formed an indurated ulcer with the typical rolled border. Ulceration may cause soreness or stinging pain when sharply flavoured food is eaten. Bleeding, either spontaneously or from mild trauma.
- 17. Paraesthesia or anaesthesia of the lip or tongue Airway obstruction Chronic earache Trismus/ dysphagia Altered vision Epiphora Lymphadenopathy
- 18. As a white patch
- 19. Indolent ulcer
- 20. Sites of Oral Cancer: Lower lip is the most frequent site of oral cancer overall. Tongue is the most frquently affected site within the mouth. In the oral cavity, the majority of oral cancers are concentrated in the lower part of the mouth, particularly the lateral borders of the tongue, adjacent floor of the mouth and lingual aspect of the alveolar margin. Hard palate and dorsum of the tongue are rarely affected.
- 22. As a red patch
- 23. Spread of Oral Carcinoma: Carcinoma invades adjacent tissue by direct extension. Bone initially forms a barrier but is eventually destroyed, usually by superficial erosion, but once the cortex is breached carcinoma may invade laterally along the medullary cavity. Metastatic spread is primarily through the lymphatics to the regional lymph nodes. Blood stream is an uncommon, late feature of the disease.
- 25. 25 Main lymph node groups in the neck. Level I: nodes of the submandibular and submental triangles. Level II: nodes of the upper cervical (jugular) chain. Level III: nodes of the mid-cervical (jugular) chain. Level IV: nodes of the lower cervical (jugular) chain. Level V: nodes of the posterior triangle of the neck. Level I is bounded by the digastric muscle. Levels II, III, and IV nodes lie deep to the upper, mid, and lower thirds of the sternocleidomastoid muscle and are related to the internal jugular vein. The omohyoid muscle separates level lII and IV.
- 26. 26
- 28. TX Primary tumor cannot be assessed. T0 There is no evidence of primary tumor. Tis Carcinoma is in situ. T1 Tumor is 2 cm or less in greatest dimension. T2 Tumor is more than 2 cm but not greater than 4 cm in greatest dimension. 28
- 29. T3 Tumor is more than 4 cm in greatest dimension. T4 (lip) Tumor invades through cortical bone, inferior alveolar nerve, floor of mouth, or skin of face—i.e., chin or nose. T4a (oral Tumor invades adjacent structures (e.g., through cavity) cortical bone, into deep [extrinsic] muscle of tongue
- 30. [genioglossus, hypoglossus, palataglossus, and styloglossus], maxillary sinus, skin of face). T4b Tumor invades masticator space, pterygoid plates, or skull base and/or encases the internal carotid artery. Note: Superficial erosion alone of bone/tooth socket by gingival primary is not sufficient to classify as T4.
- 31. ▪ NX Regional lymph nodes cannot be assessed. ▪ N0 There is no regional nodes metastasis. ▪ N1 Metastasis is in a single ipsilateral lymph node, 3 cm or less in ▪ greatest dimension. ▪ N2 Metastasis is in a single ipsilateral lymph node, more than 3 ▪ cm but not more than 6 cm in greatest dimension; or metastasis ▪ is in multiple ipsilateral lymph nodes, none more that 6 cm in 31
- 32. greatest dimension; or metastasis is in bilateral or contralateral lymph nodes, none greater than 6 cm in greatest dimension. N2a Metastasis is in a single ipsilateral lymph node, more than 3 cm but not more than 6 cm in greatest dimension.
- 33. N2b Metastasis is in multiple ipsilateral lymph nodes, none more than 6 cm in greatest dimension. N2c Metastasis is in bilateral or contralateral lymph nodes, none more than 6 cm in greatest dimension. N3 Metastasis is in a lymph node more than 6 cm in greatest dimension.
- 34. Distant Metastasis (M) MX Distant metastasis cannot be assessed. M0 There is no distant metastasis. M1 There is distant metastasis.
- 35. ▪ Stage 0 Tis N0 M0 ▪ Stage I T1 N0 M0 ▪ Stage II T2 N0 M0 ▪ Stage III T3 N0 M0 ▪ T1 N1 M0 ▪ T2 N1 M0 ▪ T3 N1 M0 ▪ Stage IVA T4a N0 M0 ▪ T4a N1 M0 ▪ T1 N2 M0 ▪ T2 N2 M0 ▪ T3 N2 M0 ▪ T4a N2 M0 ▪ Stage IVB T4b Any N M0 ▪ Any T N3 M0 ▪ Stage IVC Any T Amy N M1
- 36. WELL DIFFERENTIATED MODERATELY DIFFERENTIATED POORLY DIFFERENTIATED 36
- 37. In well-differentiated tumours, the neoplastic epithelium is obviously squamous in type and consists of masses of prickle cells with a limiting layer of basal cells around the periphery. Intercellular bridges are readily recognizable. 37
- 38. Keratin pearls are often found within the masses of infiltrating cells, each pearl consisting of a central area of keratin surrounded by whorls of prickle cells. Nuclear and cellular pleomorphism is not prominent and there are relatively few mitotic figures. 38
- 39. Moderately differentiated tumours show less keratinization and more nuclear and cellular pleomorphism and mitotic activity, but are still readily identified as squamous in type. In contrast, in poorly differentiated tumours keratinization is usually absent and the cells show prominent nuclear and cellular pleomorphism and abundant, often bizarre, mitoses. 39
- 40. In poorly differentiated tumours the cells may be so abnormal as to hardly be recognizable as epithelial cells. In such cases,immunohistochemistry to demonstrate cytokeratins (intermediate filament proteins that characterize epithelia) is particularly valuable
- 44. HISTORY CLINICAL EXAMINATION INVESTIGATIONS - RADIOLOGICAL - Plain radiographs - CT, MRI, PET - LAB - HISTOPATHOLOGICAL - HEAMATOLOGICAL 44
- 45. TREATMENT PLANNING SURGERY RADIOTHERAPY CHEMOTHERAPY COMBINATION TREATMENTS 45
- 55. · early diagnosis is the major factor determining prognosis · site and late onset of symptoms adversely affect early diagnosis · prognosis decreases with increasing clinical stage (related to early diagnosis) · histopathological features influence prognosis 55
- 57. THANK YOU
