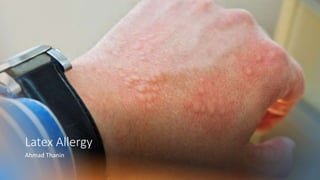
Latex Allergy
- 2. Introduction Latex allergy is a reaction to certain proteins found in natural rubber latex; a product made from the rubber tree. Healthcare workers are at an increased risk of developing a latex allergy.
- 3. Latex Allergy Prevention Latex Definition • According to the Webster's Dictionary, the term "latex" refers to natural rubber latex (NRL), the product manufactured from a milky fluid derived from the rubber tree, Hevea brasiliensis. • Several types of synthetic rubber are also referred to as "latex," but these do not release the proteins that cause allergic reactions
- 4. Workers who are exposed to latex gloves and other products that contain natural rubber latex may develop allergic reactions.
- 5. Latex Allergies Allergy to latex was first recognized in the late 1970s. Since then, it has become a major health concern as an increased number of people in the workplace are affected. Health care workers exposed to latex gloves or medical products containing latex are especially at risk. It is estimated that 8-12% of health care workers are latex sensitive.
- 6. Who is at risk ? • Workers in the health care industry (physicians, nurses, dentists, technicians, etc.) are at risk for developing a latex allergy because they use latex gloves frequently. • Workers with less frequent glove use (hairdressers, housekeepers, food service workers, etc.) and workers in industries that manufacture latex products are also at-risk for having a latex allergy.
- 7. Workers who are exposed to latex gloves and other products that contain natural rubber latex may develop some of the following allergic reactions: • skin rashes (such as hives) • nasal, eye, or sinus symptoms (sneezing, itchy eyes, or wheezing from exposure to airborne latex particles) • asthma • shock (rarely)
- 8. Types of Reactions Irritant contact dermatitis Allergic contact dermatitis (Type IV delayed hypersensitivity) IgE/histamine- mediated allergy (Type I immediate hypersensitivity)
- 9. Irritant Contact Dermatitis • When gloves are associated with skin wounds, the most common reaction is irritant contact dermatitis. • Irritant contact dermatitis may be due to direct irritation from gloves or glove powder. • It may also be due to other causes, such as the following: • soaps and detergents • incomplete hand drying • other chemicals
- 10. Irritant Contact Dermatitis Irritant contact dermatitis presents as dried, cracked, split skin. Although irritant contact dermatitis is not an allergic reaction, the breaking of the intact skin barrier due to these lesions may afford a pathway for other natural rubber latex (NRL) proteins to gain access, which can cause a development of sensitivity. Additionally, irritant contact dermatitis lesions disrupt the barrier function that intact skin provides to inhibit passage of various chemicals and pathogens.
- 11. Allergic Contact Dermatitis The second type of reaction that may be associated with glove use is allergic contact dermatitis. When glove use has been associated with this reaction, the majority of cases appear to be due to the chemicals used in processing NRL or other glove materials. Allergic contact dermatitis has an appearance similar to the typical poison ivy reaction, with blistering, itching, crusting, oozing lesions. Like poison ivy, this dermatitis appears 24-72 hours after the use of gloves or exposure to other sources of chemical sensitizers.
- 12. IgE/histamine- mediated Allergy The third and potentially most serious type of reaction associated with glove use is Type I or IgE/histamine-mediated allergy to allergenic glove protein. This type of reaction can involve mild, more-sever, or life-threatening symptoms.
- 14. Mild Symptoms: Localized reactions occur at the site of exposure. Itching Skin Redness Hives or Rash
- 15. More-Severe Symptoms: Systemic symptoms that may indicate a serious latex allergy include the following: Sneezing or Coughing Runny Nose Itchy, Watery Eyes Scratchy Throat Difficulty Breathing or Wheezing
- 16. Life-Threatening Symptoms: • The most serious allergic reaction to latex is anaphylaxis. • An anaphylaxis reaction develops immediately after latex exposure in highly sensitive people. • It rarely happens the first time someone is exposed.
- 17. Signs and symptoms of anaphylaxis include: Difficulty breathing or Wheezing Hives or Swelling Nausea and Vomiting Drop in blood pressure or Rapid/weak pulse Confusion, Dizziness, or Loss of consciousness If any of these symptoms develop following an exposure to latex, medical treatment must be initiated immediately.
- 18. Diagnosing Latex Allergy A latex allergy should be suspected in anyone who develops symptoms after latex exposure. Any exposed worker who experiences the known symptoms should be evaluated by a physician as soon as possible. • Further exposure could result in a serious allergic reaction. Taking a complete medical history is the first step in diagnosing a latex allergy. • Blood tests approved by the Food and Drug Administration (FDA) are available to detect latex antibodies.
- 19. Diagnosing Latex Allergy Testing is also available to diagnose allergic contact dermatitis. • In this FDA-approved test, a special patch containing latex additives is applied to the skin and checked over several days. • A positive reaction is shown by itching, redness, swelling, or blistering where the patch covered the skin. In some cases, tests may fail to confirm a worker who has a true allergy to latex. • In other instances, tests may suggest latex allergy in a worker with no clinical symptoms. • Therefore, test results must be evaluated by a knowledgeable physician.
- 20. Latex Allergy Protection Use non-latex gloves for activities that are not likely to involve contact with infectious materials. When handling infectious material, such as blood, use powder-free gloves with a reduced protein content. When wearing latex gloves, do NOT use oil-based hand creams or lotions, as they can cause the glove to deteriorate. Frequently clean work areas contaminated with latex dust, such as carpets and ventilation ducts. Learn to recognize the symptoms of a latex allergy. Take advantage of all latex allergy education and training provided by your employer.
- 21. Developing Symptoms If you develop symptoms of a latex allergy, avoid direct contact with latex gloves and other latex-containing products until you can see a physician experienced in treating latex allergies. If you have a latex allergy, your health care professional or physician may discuss the following precautions: • Avoiding contact with latex gloves and products. • Avoiding areas where you might inhale the powder from latex gloves worn by other workers. • Telling your employer and health care providers (physicians, nurses, dentists, etc.) that you have a latex allergy. • Wearing a medical alert bracelet.
- 22. Remember • Latex allergy in the workplace can result in potentially serious health problems for workers, who are often unaware of the risk of latex exposure.
- 23. Barrier Protection • It is extremely important that barrier protection be used when hands would otherwise contact infectious materials or hazardous chemicals, such as latex.
- 24. OSHA's OSHA's Bloodborne Pathogens Standard (29 CFR 1910.1030) requires that gloves be worn when it is reasonably anticipated that hand contact may occur with blood, other potentially infectious materials, mucous membranes, non-intact skin, or contaminated items or surfaces, as well as when performing vascular access procedures [except as specified in paragraph (d)(3)(ix)(D)]. When gloves are being worn to protect against bloodborne pathogens, the standard requires that employers provide readily accessible alternatives, such as glove liners, for employees who are allergic to the gloves normally provided.
- 25. Reducing Exposure and Risk Reducing Exposure • Reducing exposure has been the primary prevention method to protect workers with latex allergies. • Gloves made of NRL as well as alternative materials have been cleared by the FDA for marketing as medical gloves. Reducing Risk • A prudent risk reduction strategy involves an initial survey and assessment, with a coordinated effort to identify and catalogue all NRL products used in the workplace. • An ongoing program involves close coordination between both resources and management staff. • This will help monitor NRL content of incoming products so management can be prepared to choose appropriate alternatives to protect at-risk employees.
- 26. Controlling Exposure and Risk • Employers should follow the well-known hierarchy of controls to help prevent or mitigate exposure and the risk of latex allergies in the healthcare setting. • The strategies in the hierarchy for latex protection include elimination, substitution, administrative controls, and PPE.
- 27. The strategies in the hierarchy for latex protection Elimination. Substitution. Administrative controls PPE.
- 30. Elimination & Substitution Eliminating exposure to latex is the most effective method of control. Unnecessary latex-containing materials should be eliminated. When materials, such as gloves and bandages, are required, a non-latex version should be substituted to replace the latex-containing version.
- 31. Administrative controls Healthcare facilities should implement administrative controls, which include policies and procedures, to reduce the risk of allergic NRL reactions.
- 32. For example: Creating so-called "safe zones" to protect those employees who are already sensitized to NRL allergenic proteins might be necessary. •"Safe zones" are areas where non-NRL products are used and NRL allergenic proteins have been removed from the environment. Ensuring workers use good housekeeping practices to remove latex-containing dust from the workplace. Policies are developed to: •identify areas contaminated with latex dust for frequent cleaning (upholstery, carpets, and ventilation ducts); and •make sure workers change ventilation filters and vacuum bags frequently in latex-contaminated areas. Providing workers with education programs that include instruction and hands-on training about latex safety. Periodically screening high-risk workers for latex allergy symptoms. Detecting symptoms early and removing symptomatic workers from latex exposure are essential for preventing long-term health effects.
- 33. Personal Protective Equipment (PPE) • NIOSH recommends employers take the following steps to protect workers from latex exposure and allergy in the workplace: • Provide workers with non-latex gloves to use when there is little potential for contact with infectious materials (for example, in the food service industry). • Appropriate barrier protection is necessary when handling infectious materials. • If latex gloves are chosen, provide reduced protein, powder-free gloves to protect workers from infectious materials.
- 34. Remember • No matter which control methods are used, it's important to evaluate current prevention strategies whenever a worker is diagnosed with latex allergy and provide the necessary controls to mitigate future risk.
- 35. Employer Responsibilities Latex allergy can be prevented only if employers adopt policies to protect workers from undue latex exposures. Detecting symptoms early and removing symptomatic workers from latex exposure are essential for preventing long-term health effects. NIOSH recommends employers take the following steps to protect workers from latex exposure and allergy in the workplace:
- 36. NIOSH recommends Ensure workers use good housekeeping practices to remove latex-containing dust from the workplace: • Identify areas contaminated with latex dust for frequent cleaning. • Make sure that workers change ventilation filters and vacuum bags frequently in latex-contaminated areas. Provide workers with education programs and training materials about latex allergy. Periodically screen high-risk workers for latex allergy symptoms. Evaluate current prevention strategies whenever a worker is diagnosed with latex allergy.
- 37. Employee Responsibilities Use non-latex gloves for activities that are not likely to involve contact with infectious materials. If you choose latex gloves, use only powder-free gloves with reduced protein content. "Hypoallergenic" latex gloves do not reduce the risk of latex allergy. However, they may reduce reactions to chemical additives in the latex (allergic contact dermatitis). When wearing latex gloves, do not use oil-based hand creams or lotions (which can cause glove deterioration) unless they have been shown to reduce latex related problems and maintain glove barrier protection. After removing latex gloves, wash hands with a mild soap and dry thoroughly. Use good housekeeping practices to remove latex-containing dust from the workplace. Frequently clean areas contaminated with latex dust (upholstery, carpets, and ventilation ducts).
