Al Razi Acute Pain Service Audit 2012 2013
•
1 like•521 views
This document summarizes pain service audits conducted in 2012 and 2013 at a hospital. The 2012 audit found issues like incomplete pain assessment documentation, high pain scores without timely intervention, and high catheter dislodgement rates. Solutions proposed included encouraging complete documentation, following up on high pain scores sooner, and improving catheter fixation. The 2013 audit found improvements in some areas like documentation but also an increase in missing patient records. Continuing to emphasize proper documentation follow up was recommended.
Report
Share
Report
Share
Download to read offline
Recommended
F. Benvenuti - Tele-rehabilitation service for stroke survivors with residual...

F. Benvenuti - Tele-rehabilitation service for stroke survivors with residual...Wydział ds. eZdrowia, Departament Polityki Zdrowotnej, Urząd Marszałkowski w Łodzi
Recommended
F. Benvenuti - Tele-rehabilitation service for stroke survivors with residual...

F. Benvenuti - Tele-rehabilitation service for stroke survivors with residual...Wydział ds. eZdrowia, Departament Polityki Zdrowotnej, Urząd Marszałkowski w Łodzi
More Related Content
What's hot
What's hot (18)
Importance of Evidence-Based Medicine on Research and Practice

Importance of Evidence-Based Medicine on Research and Practice
TACT: a trial of interventions to improve the use of malaria rd ts hreyburn

TACT: a trial of interventions to improve the use of malaria rd ts hreyburn
Non medical prescribing in multiple sclerosis: where does it fit into practice

Non medical prescribing in multiple sclerosis: where does it fit into practice
Improving compliance of applying fall risk precautions

Improving compliance of applying fall risk precautions
Making a difference: the benefits and challenges of non-medical prescribing

Making a difference: the benefits and challenges of non-medical prescribing
A PROSPECTIVE EVALUATION OF “KETOFOL”, KETAMINE & PROPOFOL COMBINATION FOR PR...

A PROSPECTIVE EVALUATION OF “KETOFOL”, KETAMINE & PROPOFOL COMBINATION FOR PR...
Similar to Al Razi Acute Pain Service Audit 2012 2013
promoting_comfort_and_pain_management_on_an_adult_acute_medicineuUnit_6b2015

promoting_comfort_and_pain_management_on_an_adult_acute_medicineuUnit_6b2015Susan Holmes-Walker, PhD, RN
Improving early acute pain management in an academic tertiary centre emergenc...

Improving early acute pain management in an academic tertiary centre emergenc...Canadian Patient Safety Institute
Similar to Al Razi Acute Pain Service Audit 2012 2013 (20)
Experience of a comprehensive pain care (cpc) clinic from a provincial gener...

Experience of a comprehensive pain care (cpc) clinic from a provincial gener...
surgical nurses in teaching hospitals in Ireland understanding pain

surgical nurses in teaching hospitals in Ireland understanding pain
ORIGINAL ARTICLE HIP - ANESTHESIAA randomized controlled.docx

ORIGINAL ARTICLE HIP - ANESTHESIAA randomized controlled.docx
Evaluating the Effectiveness of Current Pain Management Strategies

Evaluating the Effectiveness of Current Pain Management Strategies
For this assignment activity, I want you to answer the questions be

For this assignment activity, I want you to answer the questions be
promoting_comfort_and_pain_management_on_an_adult_acute_medicineuUnit_6b2015

promoting_comfort_and_pain_management_on_an_adult_acute_medicineuUnit_6b2015
Pain in the elderly. How to better understand and rate it.

Pain in the elderly. How to better understand and rate it.
Improving early acute pain management in an academic tertiary centre emergenc...

Improving early acute pain management in an academic tertiary centre emergenc...
EFFICACY OF TRANSDERMAL PATCHES IN THE MANAGEMENT OF POSTOPERATIVE PAIN: AN O...

EFFICACY OF TRANSDERMAL PATCHES IN THE MANAGEMENT OF POSTOPERATIVE PAIN: AN O...
2015: Pain Assessment, the Key to Treating Pain in the Inpatient Setting-Yi

2015: Pain Assessment, the Key to Treating Pain in the Inpatient Setting-Yi
More from Farah Jafri
More from Farah Jafri (7)
Total knee replacement post op pain control protocol for surgeons Al Razi Ort...

Total knee replacement post op pain control protocol for surgeons Al Razi Ort...
Pediatric pain protocol Al Razi Anesthesia department Kuwait

Pediatric pain protocol Al Razi Anesthesia department Kuwait
Patient control epidural analgesia Al Razi hospital Kuwait

Patient control epidural analgesia Al Razi hospital Kuwait
Epidural dislodgements Audit Al Razi hospital Kuwait

Epidural dislodgements Audit Al Razi hospital Kuwait
Recently uploaded
☑️░ 9630942363 ░ CALL GIRLS ░ VIP ░ ESCORT ░ SERVICES ░ AGENCY ░
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...

Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...GENUINE ESCORT AGENCY
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service AvailableGENUINE ESCORT AGENCY
☑️░ 9630942363 ░ CALL GIRLS ░ VIP ░ ESCORT ░ SERVICES ░ AGENCY ░
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Trichy Call Girls Book Now 9630942363 Top Class Trichy Escort Service Available

Trichy Call Girls Book Now 9630942363 Top Class Trichy Escort Service AvailableGENUINE ESCORT AGENCY
☑️░ 9630942363 ░ CALL GIRLS ░ VIP ░ ESCORT ░ SERVICES ░ AGENCY ░
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...

Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...GENUINE ESCORT AGENCY
Model Call Girl Services in Delhi reach out to us at 🔝 9953056974 🔝✔️✔️
Our agency presents a selection of young, charming call girls available for bookings at Oyo Hotels. Experience high-class escort services at pocket-friendly rates, with our female escorts exuding both beauty and a delightful personality, ready to meet your desires. Whether it's Housewives, College girls, Russian girls, Muslim girls, or any other preference, we offer a diverse range of options to cater to your tastes.
We provide both in-call and out-call services for your convenience. Our in-call location in Delhi ensures cleanliness, hygiene, and 100% safety, while our out-call services offer doorstep delivery for added ease.
We value your time and money, hence we kindly request pic collectors, time-passers, and bargain hunters to refrain from contacting us.
Our services feature various packages at competitive rates:
One shot: ₹2000/in-call, ₹5000/out-call
Two shots with one girl: ₹3500/in-call, ₹6000/out-call
Body to body massage with sex: ₹3000/in-call
Full night for one person: ₹7000/in-call, ₹10000/out-call
Full night for more than 1 person: Contact us at 🔝 9953056974 🔝. for details
Operating 24/7, we serve various locations in Delhi, including Green Park, Lajpat Nagar, Saket, and Hauz Khas near metro stations.
For premium call girl services in Delhi 🔝 9953056974 🔝. Thank you for considering us!Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X79953056974 Low Rate Call Girls In Saket, Delhi NCR
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In Hyderabad Escorts Service
Escorts Service Available
Whatsapp Chaya ☎️ : [+91-9352852248 ]
Escorts Service Hyderabad are always ready to make their clients happy. Their exotic looks and sexy personalities are sure to turn heads. You can enjoy with them, including massages and erotic encounters.#P12Our area Escorts are young and sexy, so you can expect to have an exotic time with them. They are trained to satiate your naughty nerves and they can handle anything that you want. They are also intelligent, so they know how to make you feel comfortable and relaxed
SERVICE ✅ ❣️
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS HOUSE WIFE RUSSIAN , AIR HOSTES ,VIP MODELS .
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★
SATISFACTION,UNLIMITED ENJOYMENT.
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL Star Hotel Service .In Call & Out call
SeRvIcEs :
★ A-Level (star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
★ANAL SERVICES.
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...

🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...Call Girls In Delhi Whatsup 9873940964 Enjoy Unlimited Pleasure
Recently uploaded (20)
Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time

Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time
Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...

Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...
VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋

VIP Hyderabad Call Girls Bahadurpally 7877925207 ₹5000 To 25K With AC Room 💚😋
Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...

Call Girls Vasai Virar Just Call 9630942363 Top Class Call Girl Service Avail...
Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available
Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...

Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...
Trichy Call Girls Book Now 9630942363 Top Class Trichy Escort Service Available

Trichy Call Girls Book Now 9630942363 Top Class Trichy Escort Service Available
Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...

Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...
Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...

Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...
Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...

Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...
Call Girls Hosur Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Hosur Just Call 9630942363 Top Class Call Girl Service Available
Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...

Pondicherry Call Girls Book Now 9630942363 Top Class Pondicherry Escort Servi...
Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...

Premium Bangalore Call Girls Jigani Dail 6378878445 Escort Service For Hot Ma...
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Call Girls in Gagan Vihar (delhi) call me [🔝 9953056974 🔝] escort service 24X7
Call Girls Service Jaipur {9521753030} ❤️VVIP RIDDHI Call Girl in Jaipur Raja...

Call Girls Service Jaipur {9521753030} ❤️VVIP RIDDHI Call Girl in Jaipur Raja...
Call Girls Jaipur Just Call 9521753030 Top Class Call Girl Service Available

Call Girls Jaipur Just Call 9521753030 Top Class Call Girl Service Available
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...

🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...
The Most Attractive Hyderabad Call Girls Kothapet 𖠋 9332606886 𖠋 Will You Mis...

The Most Attractive Hyderabad Call Girls Kothapet 𖠋 9332606886 𖠋 Will You Mis...
All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...

All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...
Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available
Al Razi Acute Pain Service Audit 2012 2013
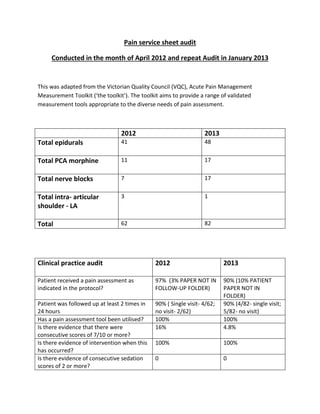
- 1. Pain service sheet audit Conducted in the month of April 2012 and repeat Audit in January 2013 This was adapted from the Victorian Quality Council (VQC), Acute Pain Management Measurement Toolkit (‘the toolkit’). The toolkit aims to provide a range of validated measurement tools appropriate to the diverse needs of pain assessment. 2012 2013 Total epidurals 41 48 Total PCA morphine 11 17 Total nerve blocks 7 17 Total intra- articular shoulder - LA 3 1 Total 62 82 Clinical practice audit 2012 2013 Patient received a pain assessment as indicated in the protocol? 97% (3% PAPER NOT IN FOLLOW-UP FOLDER) 90% (10% PATIENT PAPER NOT IN FOLDER) Patient was followed up at least 2 times in 24 hours 90% ( Single visit- 4/62; no visit- 2/62) 90% (4/82- single visit; 5/82- no visit) Has a pain assessment tool been utilised? 100% 100% Is there evidence that there were consecutive scores of 7/10 or more? 16% 4.8% Is there evidence of intervention when this has occurred? 100% 100% Is there evidence of consecutive sedation scores of 2 or more? 0 0
- 2. Is there evidence of intervention when this has occurred? N.A N.A Is there evidence of any other reportable observation? Nausea, vomiting, hypotension etc Yes, YES Is there evidence of interventions in response to the other reportable observations? 100% 100% Data entry in pain service sheet Patient name 100% 100% Age 100% 100% Medical problem 95% 100% Name of block 70% 100% File number 92% 100% Premature catheter dislodgement 13%; 7% -epidural;40%- nv.blk, 3.6%; 1.2% epidural;2.4% nv blk Problem area identified in 2012 1. Pain service follow up sheet, not filled and put in the collection box in the recovery 2. High percentage of “2 consecutively high pain scores”. Immediate rescue analgesics are given for high pain score but follow up not done after 30 min, fixed time for rounds, and reliance on ward staff for feedback. Missed cases of analgesia failure. 3. High dislodgement rate 4. Deficient data in the follow up sheets related to name of nerve block and medical problems Solution suggested in 2012 1. Encourage colleagues to fill the chart and put in the collection box, the doctor posted in the recovery, during the morning hours confirms the chart is written. 2. Follow up of patients with high initial pain scores after 30 min to 1 hour. 3. Better fixation, tunneling of catheters 4. Information sessions for colleagues on the importance of filling the charts properly, for example a chart with information about allergies or co morbid conditions will help the pain service in adding co analgesics or rescue medications. Repeat Audit 2013 1. Marked improvement in certain parameters like chart filling up by anesthetists, was observed
- 3. 2. Dislodgement rate decreased due to better fixation 3. Lower pain scores and no cases with high (7/10) pain scores 4. Increase in papers not found in the follow up box. Solution suggested in 2013 Create awareness amongst anesthetist and technician about keeping the paper in the box (better follow up of patients, patient safety and early detection of complication if case followed up). Conducted by Dr Farah Jafri
