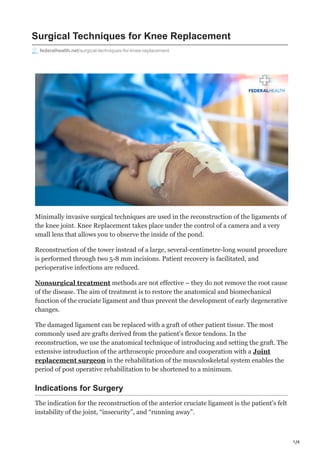
Surgical Techniques for Knee Replacement
- 1. 1/4 Surgical Techniques for Knee Replacement federalhealth.net/surgical-techniques-for-knee-replacement Minimally invasive surgical techniques are used in the reconstruction of the ligaments of the knee joint. Knee Replacement takes place under the control of a camera and a very small lens that allows you to observe the inside of the pond. Reconstruction of the tower instead of a large, several-centimetre-long wound procedure is performed through two 5-8 mm incisions. Patient recovery is facilitated, and perioperative infections are reduced. Nonsurgical treatment methods are not effective – they do not remove the root cause of the disease. The aim of treatment is to restore the anatomical and biomechanical function of the cruciate ligament and thus prevent the development of early degenerative changes. The damaged ligament can be replaced with a graft of other patient tissue. The most commonly used are grafts derived from the patient’s flexor tendons. In the reconstruction, we use the anatomical technique of introducing and setting the graft. The extensive introduction of the arthroscopic procedure and cooperation with a Joint replacement surgeon in the rehabilitation of the musculoskeletal system enables the period of post operative rehabilitation to be shortened to a minimum. Indications for Surgery The indication for the reconstruction of the anterior cruciate ligament is the patient’s felt instability of the joint, “insecurity”, and “running away”.
- 2. 2/4 Reconstruction is one of the main factors in preventing secondary damage to the cartilage surfaces and menisci of the knee. It should be performed no later than 4-6 months after the original injury. Description of the Knee Ligament Reconstruction Anesthesia is required for the operation. The anesthetist examines the patient before anesthesia and explains the proposed type of anesthesia. Most patients undergo knee or ankle surgery under local or lumbar anesthesia. This anesthesia is chosen because of fewer complications that can occur and the absence of unpleasant side effects of general anesthesia, such as nausea, vomiting, sore throat and larynx, and a feeling of available breakdown. In some cases, general anesthesia is used for arthroscopy. After the surgery, the knee is fitted with a sterile dressing, stabilizer, and a thin tube (drain) is left in the joint to drain excess blood. It will be deleted the next or next morning. Immediately after returning to bed, the patient’s knee is cooled with a cooling dressing. The final price of the procedure depends on the type and number of implants/staples necessary for the successful performance of the process. How to Prepare? Basic additional examinations should be performed 10-14 days before admission to the ortho hospital. Belong to them: Blood group Morphology Electrolytes Sugar level
- 3. 3/4 Liver tests Coagulation system EKG Chest photo with description Urine analysis. A valid vaccination against hepatitis B is absolutely necessary. If the patient has another disease, such as heart, lung, liver, kidney or nervous system disease, it is required to contact your family doctor beforehand to rule out contraindications for surgery. Admission to the hospital takes place in the morning on surgery; the patient must be on an empty stomach. Pre-procedure Diagnostics Recommended A knee replacement doctor who will perform this procedure qualifies the patient for the reconstruction procedure. In addition to the clinical examination, the attending physician requires a diagnostic ultrasound of the joint or MRI exam. Sometimes it is necessary to perform an X-ray of the joint. The date for the operation is determined when the type and indications of surgery have been discussed with the patient. Expected hospitalization time Length of stay in hospital: 1-2 days. The procedure is performed as a one-day surgery. The patient is admitted to the ward in the morning and discharged the next morning. If necessary, the stay may be extended up to several days. Recommendations after Surgery – Convalescence
- 4. 4/4 After the procedure, the patient receives painkillers and anticoagulants (heparins) for several days. Physical activity should be restricted to a minimum for at least a week. As you can easily expect, the body reacts to the surgery performed. The response is greater if the postoperative hematoma is large. Within 24 hours of the surgery, it is possible to sit, stand and walk. A physiotherapist helps you to master walking. Shows the first exercises, teaches how to walk with 2 walking sticks. The patient will use them for about 3-4 weeks after the surgery. The doctor or physiotherapist informs you about the amount of force you can stand on the operated leg. Usually, full leg loading is possible after approx. 7 days. After ligament reconstruction, it is necessary to use a joint stabilizer. Please take your own brace to the hospital – you will need it immediately after the procedure. If the patient does not have a stabilizer, it is possible to buy it in the hospital (PLN 800). It is not possible to obtain a refund for a stabilizer purchased in our hospital. After the procedure, special attention should be paid to typical postoperative symptoms: Feverish conditions and moderate pain, mainly in the evening (up to 38 ° C) Swelling and fluid in the joint Slight oozing of blood from the postoperative wound Difficulties in keeping the joint fully extended Moderate to severe, bloody bruising of the shin and below the knee Swelling in the ankles and shins. But if: Body temperature is constantly elevated (over 38.5 ° C) The wound area has changed and is becoming more and more swollen and red The pain in the joint, instead of gradually decreasing, is constantly getting worse A large amount of bloody discharge comes out of the wound Ankle swelling is painful and gets bigger Nausea and vomiting appear and persist A severe headache appeared In such cases, you should immediately contact your GP or the surgery of the doctor who performed the operation or the nearest hospital.