Report
Share
Recommended
Recommended
More Related Content
Similar to ivh.pptx
Similar to ivh.pptx (20)
MENINGITIS IN CHILDREN-1.pptx by John wambugu clinical officer paediatrics

MENINGITIS IN CHILDREN-1.pptx by John wambugu clinical officer paediatrics
More from 'محمد علي' لافي
More from 'محمد علي' لافي (6)
Recently uploaded
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Escort ServiceModels Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...GENUINE ESCORT AGENCY
Recently uploaded (20)
Andheri East ) Call Girls in Mumbai Phone No 9004268417 Elite Escort Service ...

Andheri East ) Call Girls in Mumbai Phone No 9004268417 Elite Escort Service ...
Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...

Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...
Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available
Call Girls Varanasi Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Varanasi Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available
Dehradun Call Girls Service {8854095900} ❤️VVIP ROCKY Call Girl in Dehradun U...

Dehradun Call Girls Service {8854095900} ❤️VVIP ROCKY Call Girl in Dehradun U...
Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...

Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...
Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...

Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...
Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...

Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...
Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time

Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time
Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...![Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...
Saket * Call Girls in Delhi - Phone 9711199012 Escorts Service at 6k to 50k a...

Saket * Call Girls in Delhi - Phone 9711199012 Escorts Service at 6k to 50k a...
Call Girls Mysore Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Mysore Just Call 8250077686 Top Class Call Girl Service Available
Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...

Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...
Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...

Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...
Call Girls in Delhi Triveni Complex Escort Service(🔝))/WhatsApp 97111⇛47426

Call Girls in Delhi Triveni Complex Escort Service(🔝))/WhatsApp 97111⇛47426
Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...

Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...
Call Girls Amritsar Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Amritsar Just Call 8250077686 Top Class Call Girl Service Available
Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...

Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...
ivh.pptx
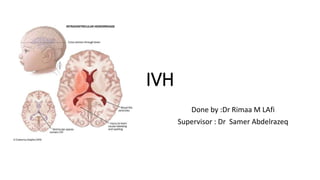
- 1. IVH Done by :Dr Rimaa M LAfi Supervisor : Dr Samer Abdelrazeq
- 2. Introduction: • IVH, the most common type of neonatal intracranial hemorrhage, occurs mainly in preterm infants ≤32 weeks of gestation. The incidence ranges from 13-65% in different centers, decreases with advancing gestational age and is influenced by certain perinatal risk factors (see below).
- 4. Pathogenesis is related to • (1) Intra-vascular factors: • Impaired cerebral autoregulation. • Fluctuating cerebral blood flow (related to fluctuating arterial blood pressure). • ↑ Cerebral blood flow (e.g., due to hypercarbia, excess volume expansion). • ↑ Cerebral venous pressure (e.g., with pneumothorax, asphyxial heart failure). • Hypotension and reperfusion. • Coagulation abnormalities. • (2) Vascular factors: • Germinal matrix, a highly vascular structure with poor capillary support, is present 50% of ventricular area or distends ventricle). • Intra-parenchymal echodensity (IPE) represents periventricular hemorrhagic infarction and is often referred to as Grade IV IVH.
- 5. severity and grading of IVH by head ultrasound: • The following grading system is used: • Grade I – Bleeding is confined to the germinal matrix*GM. • Grade II – GMH and IVH occupies between 10 to 50 percent of the lateral ventricle volume. • Grade III – GMH and IVH occupies more than 50 percent of the lateral ventricle volume and is associated with acute ventricular distension.
- 6. Management General measures include the following: • Maintenance of arterial perfusion to avoid hypotension or hypertension and preserve cerebral blood flow • Adequate oxygenation and ventilation with specific avoidance of hypocarbia, hypercarbia, and acidosis. • Provision of appropriate fluid, metabolic, and nutritional support. • Seizures should be treated • Detection of posthemorrhagic ventricular dilatation, which is the major complication of severe IVH.
- 7. • Other than early diagnosis and careful supportive care For progressive ventricular dilatation (post-hemorrhagic hydrocephalus), the essential point is early recognition. • do serial head U/S examinations in infants with IVH ≥grade II. Some cases of ventricular dilatation will respond to serial lumbar punctures and/or acetazolamide or other diuretics (to decrease CSF production). Persistent, progressive ventricular dilatation requires a ventricular reservoir or v-p shunt by a neurosurgeon.
- 8. Intraventricular Hemorrhage Prevention in preterm Guidelines (IVH PREVENTION BUNDLE) • Equipment • • Cardio-respiratory monitor • • Isolette and Isolette cover • “IVH Bundle” sign • • “Minimal Handling” sign
- 9. Implementation • • Place the infant into the isolette bed • • Confirm the infant weight and gestational age to determine eligibility for IVH Prevention Guidelines. ##An infant only needs to meet one of the two criteria for guideline implementation: less than 32 weeks gestation and/or less than 1500 grams. o Guideline interventions should be implemented soooon as possible!! .If it is known in advance that the infant will meet the criteria for IVH Guidelines, neutral head positioning should be implemented and maintained in the delivery room with Delayed Cord Clamping (DCC)
- 10. • A. Midline Positioning of the head • o Rationale: • Midline Positioning of the head Prevent cerebral blood flow fluctuations and maintaining jugular venous flow
- 11. • B. Elevate Hed of Bed • 1. Elevate the head of the bed 15-30° during the first 5-7 DAYS. • 2. May briefly to placed flat during X-rays or procedures as needed • 3. Avoid Trendelenburg position. and Avoid raising feet and legs above head
- 12. • C. Minimal Handling and stimulation • Rationale: Minimizing handling will prevent disturbances in cerebral blood flow; reducing stimulation and gentle care taking decrease incidence of IVH
- 13. • D. Minimize pain and stress • 1. Use swaddling and other non-pharmacologic interventions (boundaries; shield eyes from light) when performing mild painful procedures. • 2. Consider pain medication for painful procedures and intubated infant who are agitated and/or fighting the ventilator, continues infusion is preferred over bolus administration • 3. Suction (ETT, deep nasal/oral) only when clinically indicated • E. Maintain normothermia (36.5-37 °c)
- 14. • F. Slow increase intravascular volume • o Rationale rapid increase intravascular volume leading to impaired cerebral autoregulation • 1. Limit infusion rate of blood products 3 hours • 2. Limit infusion rate of bolus saline 30 minutes or more except in arrest situation • 3. DW10%, 2ml/kg for hypoglycemia boluses should be given over 5 minutes • 4. Avoid use of sodium bicarbonate. If needed give 1-2 mEq/kg over at least 30 minutes • 5. Avoid hypovolemia ,hypotension keep MAP within normal range
- 15. • G. Slow withdrawal/flushing of UAC • H. Respiratory intervention • I. Reduce fluctuations in blood pressure
- 16. • Patient Teaching • • Explain the procedure to the infant’s family and adverse reactions and discuss any other concerns. • Complications • • IVH causes brain injury in premature infants and is directly associated with negative neurodevelopmental outcomes. interventions are aimed at decreasing dramatic shifts in cerebral perfusion
- 17. References: • 1. Hansen AR, Cloherty and Stark's Manual of Neonatal Care, 8th edition, 2017. • 2. Gleason CA, Devaskar SU (Ed.), Avery’s Diseases of the Newborn, 9th edition, 2012. • 3. Gomella TL et al., Neonatology: Management, Procedures, On-Call Problems, Diseases and Drugs, 7th edition, 2013. • 4. Auckland District Health Board, Newborn Services Clinical Guideline, NZ, 2018 Update. • 5. Bedside Clinical Guidelines Partnership, Neonatal Guidelines 2017-19, Staffordshire, Shropshire and Black Country Neonatal Operational Delivery Network and Southern West Midlands Neonatal Operational Delivery Network. • 1- Implementing a Neuro-Bundle in a Level III Neonatal Intensive Care Unit, University of Maryland , • Baltimore , May 2019. http://hdl.handle.net/10713/9637 • 2- Chiriboga, N., Cortez, J., Pena-Ariet, A., Makker, K., Smotherman, C., Gautam, S.Hudak,M.L. (2019). • Successful implementation of an intracranial hemorrhage (ICH) bundle in reducing sever ICH: a quality • improvement project. Journal of Perinatology, 39, 143-151.2019 • 3- Romantsik, O., Calevo, M.G., & Bruschettini, M. (2017). Head midline position for preventing the • occurrence or extension of germinal matrix-intraventricular hemorrhage in preterm infants (review). • Cochrane Database of Systematic Reviews, 7CD012362.doi:10.1002/14651858.CD012362.pub2 • 4- Neonatal Neuro-protective Best Practice Guidelines NICU Brain Sensitive Care Committee Swedish Medical • Center-2015 • 5- REDUCING INTRAVENTRICULARHEMORRHAGE IN A LEVEL III NEONATAL INTENSIVE CARE UNIT, 1Hospital • of the University of Pennsylvania, United States 2015, 10.1136/bmjqs-2015-IHIabstracts.17