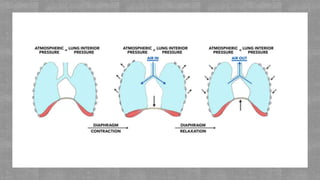
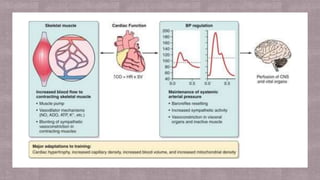
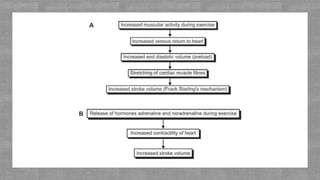
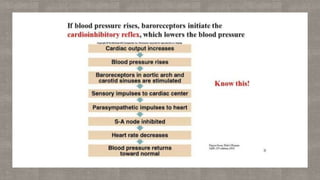
Lung function plays a crucial role in exercise performance by supplying oxygen to the body and removing carbon dioxide. Adequate lung function is necessary to take in sufficient oxygen and deliver it to working muscles. It also influences ventilation and gas exchange in the lungs, maximizing oxygen uptake and carbon dioxide removal during exercise. Optimizing lung function through exercise and respiratory health can enhance exercise performance.