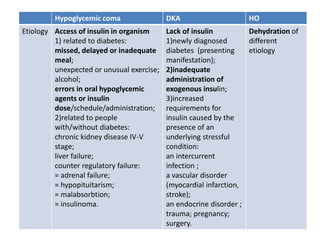
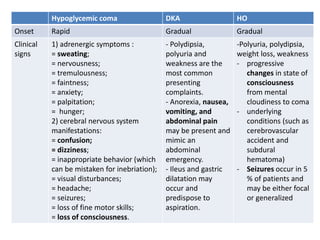
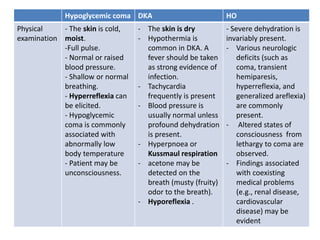
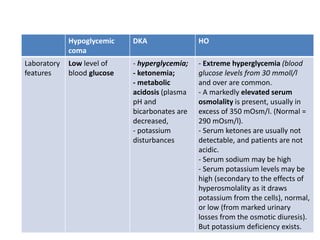
Based on the information provided, the patient is presenting with symptoms consistent with hypoglycemia that improve with glucose administration. Her symptoms also occur in the context of increased stress and alcohol use. The next appropriate step in diagnosis would be to measure serum insulin and insulin antibodies (option B) to determine if she has developed insulinoma or autoimmune hyperinsulinemia. Liver tests, cortisol/ACTH, and growth hormone measurements are not the direct next steps given the presentation of hypoglycemia.