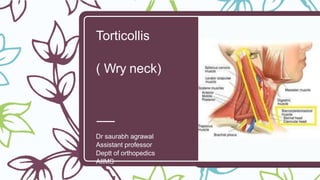
torticollis- cervical rib.pptx
- 1. Torticollis ( Wry neck) Dr saurabh agrawal Assistant professor Deptt of orthopedics AIIMS
- 3. So what is “Torticollis” ? – Torticollis, also known as wry neck, is a dystonic condition defined by an abnormal, asymmetrical head or neck position, which may be due to a variety of causes. – The term torticollis is derived from the Latin words tortus for twisted and collum for neck
- 4. Presentation of Torticollis :- – Torticollis is a fixed or dynamic tilt, rotation, with flexion or extension of the head and/or neck. The type of torticollis can be described depending on the positions of the head and neck:- – LATEROCOLLIS : the head is tipped toward the shoulder – ROTATIONAL TORTICOLLIS : the head rotates along the longitudinal axis – ANTEROCOLLIS : forward flexion of the head and neck – RETROCOLLIS : hyperextension of head
- 5. Signs and Symptoms – Torticollis can be a disorder in itself as well as a symptom in other conditions. – Other symptoms include: – Neck pain – Occasional formation of a mass – Thickened or tight sternocleidomastoid muscle – Tenderness on the cervical spine – Tremor in head – Unequal shoulder heights – Decreased neck movement
- 6. Types of Torticollis :- 1 Congenit al muscular torticolli s (CMT) 2 Postura l torticolli s 3 Ocular torticolli s (Trochle ar torticolli 4 Spasmo dic torticolli s (wryneck 5 Acute torticolli s
- 7. Congenital muscular torticollis The congenital muscular torticollis is the most common torticollis which is present at birth. The cause of congenital muscular torticollis is unclear. Supposed causes include :- Birth trauma •Intrauterine malposition •Repetitive microtrauma within the womb to the SCM • Sudden change in calcium concentration in body, causing prolonged period of muscle Congenital Torticollis is presented at 1–4 weeks of age and a hard mass usually develops. It is normally diagnosed using ultrasonography and a colour histogram or clinically through evaluating the infant's passive cervical range of motion.
- 8. Acquired torticollis Non-congenital muscular torticollis may result from :- • Scarring Or Disease Of Cervical Vertebrae • Adenitis • Tonsillitis, • Rheumatism • Enlarged Cervical Glands • Retropharyngeal Abscess • Cerebellar Tumors Type s Spasmod ic (Clonic) Permanent (Tonic)
- 9. Acquired T orticollis: Types Self- Limiting : One or more of the neck muscle is painful It resolves in 1-4 weeks SCM or upper Trapezius is usually the most involved Draughts or cold or abnormal posture is implicate Tumors of the Posterior Fossa These can compress the nerve supplying the neck muscle and have to be treated surgically Infection s Pharyn x Ear Adenectomy – cam cause Grisel’s syndrome which can cause subluxation of the upper cervical joints. Drug induced : Antipsychotics & Antiemetics Fibrodysplasia ossificans progressiva (FOP)
- 10. Other Types of Torticollis – Spasmodic Torticollis – Recurrent or transient contraction of the muscles of the neck muscles. – SCM is mostly involved – Cervical dystonia, idiopathic cervical dystonia, intermittent torticollis" – Trochlear torticollis (Congenital fourth nerve palsy) – This is unrelated to the SCM – Caused by damage to the Trochlear nerve (CN IV) that supplies the Superior Oblique muscle of the eye.
- 11. Torticollis may lead to additional problems :- – Flattening of the skull (plagiocephaly or brachycephaly) in infants. – Movement that favors one side of the body, affecting the arms, trunk, and hips. This can lead to strength imbalances, such as an elevated shoulder and side- bending of the trunk. This movement pattern can lead to delayed gross motor development. – Developmental hip dysplasia. – Scoliosis. – Limited ability to turn the head to see, hear, and interact with surroundings, which can lead to delayed cognitive development. – Delayed body awareness or lack of self- awareness and interaction. – Difficulty with balance. – Asymmetrical vision changes.
- 13. Diagnosis –General History taking –Birth History –History of Trauma –Neurological examination –X-ray of cervical spine –MRI –USG – Muscular tissue, Color Histogram –Optometrist evaluation
- 14. Assessment : – Observation of any asymmetries including facial, cranial, neck and positional preference and presence of plagiocephaly. – Observation of skin creases. – Observation of infant in developmentally appropriate positions to detect asymmetry and screen developmental milestones. – Cervical active and passive range of movement testing. – Upper and lower limb ROM screen, checking for hip dysplasia, which can be associated with CMT, and spine asymmetry. – Pain at rest and during movements. – Palpation of sternocleidomastoid for size and elasticity and presence of mass. – Screen of visual tracking. – Screen muscle tone. – Identification of Red flags and appropriate onward referral: – poor tracking – abnormal muscle tone – other features inconsistent with CMT – poor progress with treatment
- 15. Management : Physical Therapy (Goals) To correct the deformity by release of the contracted soft tissues and To maintain the correction by suitable exercise regime; avoiding recurrence.
- 16. Physiotherapy Management – Early mild cases – Children with a mild degree of deformity reporting early for the treatment can be managed with physiotherapy. – The physiotherapy procedures employed are: – I. Evaluation: Careful evaluation of ROM and the degree of deformity. – II. Massage: Massage can relax the muscle preceding the stretching maneuvers. – III. Thermo Therapy Modality: Carefully administered thermo-therapy modality induces relaxation. – IV. Passive movements: The child is placed in supine position with head beyond the edge of the table with the neck in extension by positioning a pillow under the thoracic region; Shoulders are stabilized by an assistant.
- 17. Physiotherapy Management – To attain relaxation, all the movements of the cervical spine are done in a form of slow relaxed passive movements. – This should be followed by sustained passive stretching to the affected sternomastoid. E.g. when the right sternomastoid is involved the head should be gradually bent inside flexion to the left, held there for a while and then rotated gradually to the right. Try to gain as much overcorrection as possible by applying gradual traction to gain further stretching.
- 18. Physiotherapy Management – Maintenance of Correction: Once the correction is achieved. It has to be maintained by passively holding or keeping a sandbag. – E.g: Kineso taping, Cervical Brace, Cervical collars – The same maneuver can be repeated during the subsequent visits. – Active correction: Active correction is best achieved by assisting the child head to follow an object moved in the proper arc of correction. The bright-colored sound producing object is ideal to attract the child attention. – PNF: patients with neck extension can be used to an advantage with emphasis on stretch and traction.
- 20. Surgical Management – Subcutaneous tenotomy, open tenotomy, bipolar tenotomy, and radical resection of a sternomastoid tumor or the SCM. – The sterna and the clavicular heads of sternomastoid are divided close to the origin along with the release of the tight fascia. The head is then immobilized in a plaster cast in over-corrected position for 2 to 4 weeks. Mobilization is begun as soon as the cast is removed.
- 21. Post surgical PT management – Hot packs for pain relief. – Active movements of sternocleidomastoid to prevent post surgery weakness. – Free active movements in the direction of correction followed by resistive exercises. – Self correction in front of mirror. – Specially molded cervical collar and maintenance of correction during sleep.
- 22. Cervicalrib
- 24. • Definition:It is basically a congenital condition in which supernumerary (Extra rib)usually arising from 7th cervical vertebrae. • Usually bilateral
- 25. Patholog y • Persistent ossification of C7 lateral costal element which gets reabsorbed.
- 26. Clinicalpresentation • Asymptomatic • Pain(Dull aching) and parasthesia in ulnar aspect of hand and little fingers. • Tingling Of forearm and Hand-”Falling asleep” due to circulatory insufficiency. • Diminished sensations in medial 11/2 digits • Symptoms are accentuated in downward displacement of shoulder girdle(heavy weight lifting)
- 27. Sign s • 1)Thoracic outlet syndrome • 2)Pallor • 3)Cyanosis • 4)Trophic changes-Glossy skin,brittle nails,ulcer • 5)Gangrene • 6)Adsons test positive •
- 28. Differentialdiagnosis • 1) Herniated cervical disc • 2) Hyperabduction syndrome • 3) Costoclavicular compression syndrome
- 29. Investigations • 1)Plain x-ray cervical spine • 2)Chest x-ray •
- 31. Treatment • Conservative • 1)Pain medications-NSAIDS • • 2)Avoid heavy weight lifting • 3)Physio-Self resisted elevation and adduction of scapula.Endurance trailing for sports.
- 32. Surger y • If symptoms persist • Remove surgical rib .