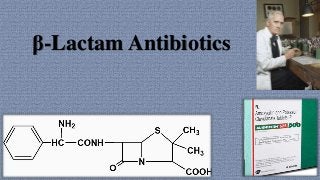
Beta lactam antibiotics
- 2. • BETA-LACTAM ANTIBIOTICS (inhibitors of cell wall synthesis) • Drugs includes- Penicillin, cephalosporin, Monobactam & Carbapenem • All of them have β -lactam ring in their chemical structure • Penicillin:- • First antibiotic developed & used clinically Discovered accidentally by Alexander Fleming(1928) High-yielding source→ Penicillium chrysogenum Low- yielding source→ Penicillium notatum • The side chain of natural penicillin can be split off by an amidase to produce 6-aminopenicillanic acid β-Lactam ring Thiazolidine ring
- 3. • β-Lactam ring is broken by – Penicillinase (β-Lactamase), and by gastric acid. • Resultant Product is Penicilloic acid with • No anti-bacterial activity but • Acts as antigenic determinant (Major determinant) • Bacterial Cell wall is composed of Peptidoglycans Cross linked by peptide chains. • NAM – NAG-(Aminosugar) • ( N-acetyl muramic acid and N- acetyl glucosamine) • Cross linked by a Pentaglycine cross bridge • Cross bridging is transpeptidation reaction. • Transpeptidase and related proteins (Penicillin Binding Proteins) are used for making cross linkage. • Cross linking provides stability, strength
- 5. • MOA:- All β-lactams antibiotics ↓↓ Bind to specific receptor called PBP(Penicillin binding protein) located on outer cell membrane of bacteria ↓↓ Inhibit cell wall synthesis of bacteria by inhibiting transpeptidation ↓↓ (Bactericidal Action) Result:- Damage of cross linking Weakening of cell wall Bacterial membrane bursts Bacterial lysis
- 6. Mechanism of bacterial resistance to penicillins:- 1. by producing β-lactamases, which destroy the β-lactam ring, e.g. S. aureus, E. coli, gonococci, H. influenzae, etc. 2. due to altered PBPs, which have less affinity for β-lactams, e.g. S. pneumoniae 3. due to decreased ability of the drug to penetrate to its site of action Pharmacokinetics:- Most of the orally administered penicillin G is destroyed by gastric acid (acid labile); hence penicillin-G is usually given by i.v. route. It can also be administered by i.m. route but is painful Distribution- throughout body tissues, but poorly crosses the BBB (except- meningitis) Metabolism- less bcoz of rapid excretion Excretion:-urine mainly by active tubular secretion Slow excretion in neonate & infants→renal function is not completely developed
- 7. The action of penicillins can be augmented and prolonged by giving probenecid simultaneously. Mechanism includes 1.Probenecid block the Tubular secretion of Penicillin –G 2.Probenecid also ↓ the Volume of distribution of penicillin Classification of Penicillin:- Penicillin Natural penicillins Penicillin-G Procaine penicillin G Benzathine penicillin G Semisynthetic penicillins Acid-resistant penicillin Penicillinase-resistant penicillins Extended-spectrum penicillins Phenoxymethyl penicillin (Penicillin V) Methicillin Oxacillin Cloxacillin Dicloxacillin Aminopenicillins Carboxypenicill ins Ureidopenicillin s
- 8. Extended-spectrum penicillins Aminopenicillins Ureidopenicillins Carboxypenicillins Ampicillin Amoxicillin Carbenicillin Carbenicillin indanyl Ticarcillin Mezlocillin Piperacillin Depot penicillins:- Penicillin-G + poorly water-soluble compounds such as procaine, benzathine Result- Aqueous suspension Penicillin-G Procaine penicillin G Benzathine penicillin G Fortified procaine penicillin G Duration-4–6 h 12–24 h 3–4 weeks 12–24 h Rapid onset of action Moderate plasma concentration Slow onset but has longest duration of action Rapid onset with high plasma concentration and longer duration of action severe infections— meningitis, endocarditis, pneumonia, etc used in mild to- moderate infections Used in syphilis, rheumatic fever prophylaxis, etc used in mild-to-moderate infections by sensitive organisms
- 9. Precautions for using Penicillin-G therapy:- 1. Before giving penicillin, history of previous administration and allergic manifestations, if any, must be noted. 2. In patients with history of asthma, allergic rhinitis, hay fever, etc. there is an increased risk of penicillin allergy; hence it should be avoided in such cases. 3. Sensitivity test should be performed by an intradermal test on the ventral aspect of forearm. Itching, erythema and wheal formation are watched for. A negative skin test does not ensure absolute safety. 4. Inj. adrenaline and hydrocortisone should be kept ready before injecting penicillin to treat the anaphylactic reaction
- 10. Adverse reactions of penicillin G:- 1. Hypersensitivity reactions(type-I), such as skin rashes, urticaria, fever, dermatitis, bronchospasm, angioedema, joint pain, serum sickness or anaphylactic reaction. • It is not a dose-related adverse drug reaction and can occur with any dosage form of penicillin. • Rx of Anaphylactic shock- • 1. Inj. adrenaline 0.3–0.5 mL of 1:1000 solution intramuscularly. • 2. Inj. hydrocortisone 200 mg intravenously. • 3. Inj. diphenhydramine 50–100 mg intramuscularly or intravenously • Jarisch–Herxheimer reaction:-It is an acute exacerbation of signs and symptoms of syphilis during penicillin therapy due to release of endotoxins from the dead organisms. • The manifestations are fever, chills, myalgia, hypotension, circulatory collapse, etc. • Rx-with aspirin and corticosteroids.
- 11. Therapeutic uses of penicillin G:- In dentistry:- necrotizing gingivitis, periodontal infections, etc. either alone or with metronidazole Pneumococcal infections: In pneumonia, meningitis or other serious infections, 3rd -generation cephalosporins (DOC). However, i.v. penicillin G can be used as an alternative if the organism is sensitive Streptococcal infections:- streptococcal pharyngitis, otitis media, rheumatic fever(Procaine penicillin G or benzathine penicillin G ), etc Meningococcal meningitis- I.V. penicillin G but DOC- 3rd generation cephalosporine Syphilis:- Penicillin G DOC. The alternative drugs-ceftriaxone and azithromycin and doxycycline Diphtheria: It is an acute infection of upper respiratory tract caused by C. diphtheriae. Pt. allergic to penicillin- erythromycin preferred
- 12. • Clostridial infections (tetanus and gas gangrene):- The main treatment is the neutralisation of the toxin by using human tetanus immunoglobulin. For gas gangrene, penicillin G is used as an adjunct to antitoxin. • Other infections: Anthrax, listeria infections, leptospirosis, actinomycosis, rat- bite fever, etc. are effectively treated with penicillin G. • Anaerobic infections: Penicillin G is effective for the treatment of anaerobic infections (periodontal) • Prophylactic uses of penicillins:- 1. Rheumatic fever: The causative organism β-haemolytic streptococcus. prophylaxis, inj. benzathine penicillin G(i.m. once a month) • Pt. allergic to penicillin →erythromycin or sulphadiazine. 2. Bacterial endocarditis: Patients with valvular lesions are at high risk of developing infective endocarditis hence they should receive chemoprophylactic agents before dental or surgical procedures to prevent bacteraemia.
- 13. • Penicillin-G & V are natural penicillin both are β-lactamase sensitive • But Penicillin-V→ acid stable (can be given orally) • Procaine Penicillin-G & benzathine Penicillin-G→ longest half life due to delayed intramuscular absorption • Cloxacillin & dicloxacillin→ Acid stable (good absorption so can be given orally) • Methicillin→ high Nephrotoxic (withdrawn from market) • Limitations/drawbacks of penicillin G:- 1. Acid labile – orally not very effective. 2. Short duration of action (to overcome this, repository penicillins have been developed). 3. Narrow spectrum of antibacterial activity (mainly against gram-positive organisms). 4. Destroyed by penicillinase enzyme. 5. Possibility of anaphylaxis. To overcome Limitation of Penicillin-G →semisynthetic penicillins have been developed
- 14. Extended spectrum Penicillins • Aminopenicillin:- All are β-lactamase sensitive but acid stable All are semisynthetic derivatives of penicillin Antimicrobial spectrum:- Strept. pneumoniae & Pyogenes Additional action-(gram-ve) E.coli,salmonella,shilgella,H influenza, H.pylori,proteus mirabilis,listeria Not effective against-MRSA & pseudomonas Drugs includes- Amoxycillin & Ampicillin
- 15. Ampicillin Amoxycillin Food ↓Absorption of ampicillin(incomplete absorption from gut) No effect of Food Effective in meningitis Not effective in meningitis More damage to intestinal flora so more chance of superinfection Less damage to intestinal flora so less chances of superinfection Effective against Shigella and Haemophilus influenzae Less effective against Shigella and H. influenzae Ampicillin reduces the effectiveness of oral contraceptives Does not reduce the effectiveness of oral Contraceptives Preferred by i.m. or i.v. route except GIT infection Preferred by oral route Duration is shorter Duration is longer Concentrated in bile(suitable for cholecystitis) Concentrated in respiratory secretion & sputum Dose:- Ampicillin 250–500 mg QID Dose:- Amoxicillin 250–500 mg TID
- 16. • Therapeutic uses:- • In dentistry:- (most commonly use Antibiotics) • Acute necrotizing ulcerative gingivitis, • dentoalveolar abscess, • Osteomyelitis of mandible, etc. • Ludwig’s angina in immunocompetent individuals- Ampicillin–sulbactam • URTI(upper respiratory tract infection)- Ampicillin and amoxicillin • pharyngitis, sinusitis, otitis media, bronchitis, etc. caused by S. pyogenes, S. pneumoniae and H. influenzae • Cholecystitis –Ampicillin but less effective then FQS • H.Pylori-both effective but Amoxicillin preferred • UTI-due to E.coli (safe in pregnancy) • Gonorrhoea- Ampicillin/Amoxicillin + probenecid • Typhoid-Ampicillin-12gm per day (DOC-fluoroquinolone or ceftriaxone) Amoxicillin is used alone or with metronidazole
- 17. • Meningitis:-listeria meningitis DOC-Ampicillin • Bacillary dysentery-(shigella)-Ampicillin • Bacterial endocarditis- Ampicillin + gentamicin & Prophylaxis-Amoxicillin • Side effect:- Skin rash(more with ampicillin), Nausea, vomiting, diarrhoea • Antipseudomonal penicillins:- • They are carbenicillin, carbenicillin indanyl, ticarcillin, mezlocillin and piperacillin. • Uses:- • Serious infections—bacteremias, pneumonias, UTIs, burns, etc. by P. aeruginosa and Proteus→ piperacillin than carbenicillin. • UTI caused by P. aeruginosa and Proteus spp-Carbenicillin indanyl(orally) • Mixed nosocomial infection- Ticarcillin + β-lactamase inhibitor +aminoglycoside
- 18. β-Lactamase Inhibitors • Contains β-lactams ring but negligible Antibiotic effect • Drugs includes-clavulanic acid, sulbactam and tazobactam. • They structurally resemble β-lactam molecules. • Beta-lactamase inhibitors bind to lactamases and inactivate them. • Coadministration:-(β-lactams+ β-lactamase inhibitors)→ ↑ the activity of β- lactams by preventing them from enzymatic destruction(↑spectrum) • Clavulanic acid:- • Derived from streptomyces clavigerus • MOA:- It competitively and irreversibly inhibits -lactamases produced by a wide range of gram-positive and gram-negative bacteria. • After binding to the enzyme, clavulanic acid itself gets inactivated hence it is called a ‘suicide’ inhibitor • Combination therapy required dose reduction in renal insufficiency
- 19. Preparation (Brand Name) Route(s) of Administration Uses Clavulanic acid + amoxicillin (Augmentin) Oral, i.m., i.v. Skin, soft tissue, otitis media, respiratory and urinary tract infections caused by -lactamase-producing strains of S. aureus, E. coli, H. inuenzae and gonococci Clavulanic acid + ticarcillin i.m., i.v. Mixed nosocomial infections due to aerobic gram- negative bacilli,S. aureus and Bacteroides spp Sulbactam + ampicillin Oral, i.m., i.v. Intra-abdominal and pelvic infections (mixed aerobic and anaerobic infections) due to -lactamase-producing strains of S. aureus, gram negative aerobes and anaerobes Tazobactam + piperacillin i.v. Severe infections caused by -lactamase-producing strains of gram-negative bacilli
- 20. Question paper discussion 1.Write short note on: -Amoxycillin 2. Discuss the pharmacological basis for the use of : A. Amoxycillin with clavulanic acid B.Probenecid with Penicillin 3. Classification of β-lactam antibiotics. Discuss mechanism of action uses and adverse effect of amoxycillin 4. Classify Penicillins. Discuss their mechanism of action, uses, drug interactions & adverse effects 5.Discuss mechanism of action, side effects and therapeutic uses of Penicillin. 6. Enumerate penicillin antimicrobials. Discuss the Antibacterial spectrum, uses precaution & adverse effects of extended spectrum penicillin
- 21. CEPHALOSPORINS • The first cephalosporins were obtained from a fungus, Cephalosporium acremonium. • Later, semisynthetic cephalosporins were developed. • Cephalosporins are β-lactam antibiotics. • MOA:- Similar to penicillin (Bactericidal action)but they bind with different binding protein. • All resistant to β-lactamases (Except-1st Generation) • Classification:- Based on Spectrum of activity (Divided into 4-generations) 1St generation 2nd Generation 3rd Generation 4th Generation Cephalexin (O) Cefadroxil (O) Cefazolin (P) Cephradine(i.m./O) Cephalothin(i.m.) Cefaclor Cefuroxime Cefoxitin Cefotetan Cefixime (O) Ceftriaxone (i.m., i.v.) Cefotaxime (i.m., i.v.) Cefoperazone (i.m., i.v.) Ceftazidime (i.m., i.v.) Ceftizoxime(i.v.,i.m.) Cefepime (i.v.) Cefpirome(i.v./i.m.)
- 22. 1St generation 2nd Generation 3rd Generation 4th Generation AMS:- Effective-Mainly gram(+ve) cocci Not effective against- MRSA, Pseudomonas, Salmonella AMS:- Effective- activity ↑ against (Gm-Ve) & Anaerobes Not effective against- Pseudomonas, Salmonella AMS:- Effective- Active against (Gm-Ve) & Anaerobes, Pseudomonas, Salmonella less effective against-(Gm + ve) AMS:- Effective- active against (Gm-Ve) & Anaerobes, Pseudomonas Sensitive to β-lactamase Cefoxitin, cefuroxime- resistant to β-lactamases All are resistant to β- lactamases All are resistant to β- lactamases Cross BBB Excretion-kidney Cefuroxime-cross BBB Excretion-Kidney Cross BBB, reach high concentration in CSF Excretion-kidney, bile Cross BBB Uses:- In dentistry:- Odontogenic infections- Cephalexin and cefadroxil Prophylaxis of bacterial endocarditis before dental procedures Uses:- In dentistry:- Orodental Infections-Cefaclor or Cefuroxime axetil Uses:- In dentistry:- Cefixime & cefotaxime- dentoalveolar infection Limited use
- 23. Uses:- • Surgical prophylaxis & septic arthritis-1st generation (DOC-cefazolin) • Safe in pregnancy (UTI, respiratory tract infection)-cephalexin, cefadroxil • Respiratory tract infections:- otitis media and sinusitis, oral cefuroxime axetil can be used • Intra-abdominal and pelvic infections:- 2nd generation (Cefoxitin & cefotetan) • Community-acquired pneumonia : Ceftriaxone, cefotaxime (3rd gen) • Gonorrhoea:- Ceftriaxone (DOC) (3rd gen) • Typhoid fever: Ceftriaxone & cefoperazone (3rd gen) • Meningitis- caused by Haemophilus influenzae: Inj. Cefotaxime & ceftriaxone • Mixed aerobic and anaerobic infections-3rd gen • Septicaemia:- caused by gram-negative infections-3rd gen • Nosocomial infection- 3rd gen
- 24. • Pharmacokinetics:- • Administered either orally or parenterally • Excretion- mainly via kidney either by glomerular filtration or by tubular secretion.(Except-Cefoperazone-bile) • Active tubular secretion- of cephalosporins is blocked by probenecid, resulting in higher blood levels and longer duration of action. • Metabolism:-the body before their excretion. • Cefotaxime is deacetylated in the body before its excretion. • Side effects:- • Hypersensitivity:-They are skin rashes, urticaria and rarely anaphylaxis. • GI disturbances—mainly diarrhoea, vomiting and anorexia • Pain at the site of i.m. injection (cephalothin) • Thrombophlebitis- I.V. cephalosporins • Nephrotoxicity may occur. Co-administration of cephalothin and gentamicin increases the nephrotoxicity.
- 25. • Disulfiram-like reaction:-has been reported with cefotetan and cefoperazone • Severe bleeding:- can occur either due to hypoprothrombinaemia (which responds to vitamin K therapy) or thrombocytopaenia and/or platelet dysfunction • Semisynthetic β-lactam antibiotic • Containg Carbon atom in place of sulfur atom so called “Carbapenams” • Drugs includes-Imipenem, meropenem, doripenem, faropenem • Considered as “ Drugs of last resort” • MOA:- similar like penicillin i.e. inhibit cell wall systhesis after binding with penicillin binding protein(PBP) exert Bactericidal action • Broader spectrum than other β-lactam antibiotic(Post antibiotic effect) & resistant to β-lactamase CARBAPENEMS
- 26. • Spectrum of activity:- • Gm +ve organisms like streptococci, staphylococci, enterococci, Listeria and C. difficile (anaerobe) • Gm -ve organisms like P. aeruginosa, enterobacteriaceae and B. fragilis (anaerobes) • I.M. is painful so I.V. route is preferred • Only imipenem hydrolysed by →renal dehydropeptidase present in renal brush border(↓urinary conc) • Cilastatin-Inhibitors of renal dehydropeptidase (should be combined) USES:- Mixed bacterial infections:- urinary, respiratory, intra-abdominal, gynaecologic, skin, soft tissue, bone and joint infections (Imipenem+ cilastatin) ↑Conc. Imipenem in urine leading to ↑spectrum SE:- Nausea, vomiting and skin rashes & rare side effect-Seizures
- 27. • Meropenem:- (I.V.) • Resistant to →dehydropeptidase (combination not required) • Seizures less likely & effective against imipenem resistant P. aeruginosa. • Faropenem:- (orally) Used for respiratory and genitourinary infections. • MONOBACTAMS:- (i.v./i.m.) • Drugs:-Aztreonam • β-lactam antibiotic with only one ring(β-lactam) in its structure (absence of sulfur containing thiazolidine ring)→so called “Monobactam” • Resistant → β-lactamase • Effective against →only gm-ve bacteria • Lack of cross sensitivity with other β-lactam antibiotics (due to Lack of ‘S’ ring) (except ceftazidime) hence use in pt. allergic to penicillin or cephalosporine • USES:- Genitourinary, intra-abdominal infection (hospital aquired Gm-ve infection)
- 28. Thank You
Editor's Notes
- Ludwig's angina is a rare skin infection that occurs on the floor of the mouth, underneath the tongue
