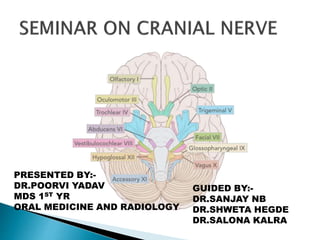
seminar on cranial nerve
- 1. PRESENTED BY:- DR.POORVI YADAV MDS 1ST YR ORAL MEDICINE AND RADIOLOGY GUIDED BY:- DR.SANJAY NB DR.SHWETA HEGDE DR.SALONA KALRA
- 2. INTRODUCTION DEVELOPMENT OF CRANIAL NERVES CRANIAL NERVE FUNCTIONAL COMPONENETS OLFACTORY NERVE[I] OPTIC NERVE[II] OCULOMOTOR NERVE[III] TROCLEAR NERVR[IV] TRIGEMINAL NERVE[V] ABDUCENT NERVE[VI] FACIAL NERVE[VII]
- 3. VESTIBULOCOCHLEAR NERVE[VIII] GLOSSPHYRYNGEAL NERVE[IX] VAGUS NERVE[X] ACCESORY NERVE[XI] HYPOGLOSSAL NERVE[XII] VASCULARIZATION OF CRANIAL NERVE EXAMINATION OF CRANIAL NERVE APPLIED ANATOMY
- 5. The 12 pairs of cranial nerves are part of the peripheral nervous system (PNS) and pass through foramina or fissures in the cranial cavity. All nerves except one, the accessory nerve[XI],originate from the brain. Having to similar somatic and visceral components as spinal nerves, some cranial nerve special sensory and motor components.
- 6. The special sensory components are associated with hearing, seeing , smelling , blanching , and tasting. Special motor components include those that innervate skeletal muscles derived embryologically from the pharyngeal arches and not from somites.
- 7. In human embryology , six pharyngeal arches are designated, but 5th pharyngeal arch never develops. Cranial nerves carry efferent fibers that innervate the musculature derived from the pharyngeal arch.
- 8. Innervation of the musculature derived from the five pharyngeal arches that do develop is as follows:- 1-first arch – trigeminal nerve 2-second arch - facial nerve 3-third arch – glossopharyngeal nerve 4-fourth arch – superior laryngeal branch of the vagus nerve 5- sixth arch – recurrent laryngeal branch of the vagus nerve
- 16. The Olfactory nerve [I] carries special afferent (SA) fibers for the sense of smell. Its sensory neurons have:- - peripheral processes that act as receptors in the nasal mucosa. - central processes that return information to the brain.
- 18. The receptors are in the roof and upper parts of nasal cavity and the central processes , after joining into small bundles , enter the cranial cavity by passing through the cribriform plate of the ethmoid bone. They terminate by synpasing with secondary neurons in the olfactory bulbs.
- 24. There are a number of disorder of the sense of smell, which can result:- hyposomia hypersomia anosomia parosmia
- 25. PERIPHERAL LESION:- LOCOREGIONAL:- Six can be mentioned:- nasal polyps Acute viral or bacterial rhinitis Nonallergic eosinophillic rhinitis Sinusitis Allergic rhinitis Tumor involvement
- 26. VIRAL:- Herpes Viral hepatitis TOXIC:- Tobacco Cement ammonia Cocaine
- 27. POST TRAUAMTIC Fracture of the anterior floor of the base of the skull ith involvement of the CRIBRIFORM PLATE. Usually caused by the occipital shock. in order of frequency :- olfactroy filaments ,nasal and sinus cavities,cerebral centers Immediate or delayed anosmia Recovery is rare.
- 28. POSTOPERATIVE , IATROGENIC Seen after surgical traction on the frontal lobe CENTRAL LESION:- Frontal or occipital trauma Neurotoxic medications
- 30. OTHER CAUSE:- ENDOCRINE:- Cushing syndrome Hypothyroidism Diabetes mellitus
- 31. NEUROLOGIC:- Alzheimer diseasse Parkinson disease Down syndrome Multiple sclerosis Epilepsy
- 32. KALLMANN DE MORSIER SYNDROME Hypogonadotropic hypogonadism Delayed puberty Often transmitted by X chromosome Congenital anosmia Atresia of choana
- 33. Various Paget Renal failure Hepatic failure Alcoholic cirrhosis AIDS IDOPATHIC Usually advanced age
- 34. The optic nerve carries SA fibers for vision. These fibers return information to the brain from photoreceptors in the retina. Neuronal processes leave the retinal receptors, join ,into small bundles, and are carried by the optic nerves to other components of the visual system in the brain. The optic nerves enter the cranial cavity through the optic canals.
- 45. The occulomotor nerve carries two types of fibers :- - general soamtic efferent (GSE) fibers innervate most of the extra – ocular muscles. - general visceral efferent (GVE) fibers are part of the parasympathetic parts of the autonomic division of the PNS.
- 47. Motor: Innervates a number of the extraocular muscles. Parasympathetic: Supplies the sphincter pupillae and the ciliary muscles of the eye. Sympathetic: No direct function, but sympathetic fibres run with the oculomotor nerve to innervate the superior tarsal muscle (helps to raise the eyelid).
- 57. Paralysis of occulomotor nerve causes:- ptosis external strabismus inability to move the occular globe upward , downward ,or medially. Intrinsic lesion produces Mydriasis ,that does not react to light.
- 58. Paralysis of the Trochlear nerve results Diplopia. Paralysis of Abdunce nerve results CONVERGENT STRABISMUS in paralyzed eye. ABDUNCE NERVE PALSY
- 60. ETIOLOGY:- Deficiency of thiamine(B1) Characterized by clinical triad:- Mental status change Ataxia Eye sign( nystagmus , opthalmoplagia)
- 61. The trochlear nerve is a cranial nerve that carries GSE fibers to innervate the superior oblique muscle , an extra- ocular muscle in the orbit.
- 62. The trigeminal nerve is the largest cranial nerve. It carries general somatic afferent (GSA) and branchial efferent (BE) fibers. The trigeminal nerve is the major general sensory nerve of the head , and also innervates muscles that move the lower jaw.
- 64. Trigeminal nerve has to roots:- (a) sensory (b) motor . Sensory root has 3 division:- (a) V1 – Ophthalmic (b) V2 – Maxillary (c) V3 – Mandibular
- 65. both motor and sensory root are attached ventrally to junction of pons and middle ceberal peduncle with motor root lying ventromedially to the sensory root. Passes anteriorly in middle cranial fossa to lie below tentorium cerebelli in cavum trigeminale, here motor root lies to sensory root.
- 67. It has both efferent component for the muscle of mastication as well as some other cranial muscles, and an afferent component for teeth tongue and oral cavity , as well as most of the skin of face and head. Trigeminal nerve has no preganglionic parasympathetic fibers, postganglionic parasymapthetic fibers travel along with its branch.
- 69. The first division of the sensory root of the trigeminal nerve is the OPTHALMIC NERVE. This smallest branch serve as an afferent nerve for the conjunctiva , cornea , eyeball ,orbit , forehead , and ethmoid and frontal sinuses, plus a portion of the dura mater.
- 71. The FRONTAL NERVE is an afferent nerve located in the Orbit and is composed of merger of the SUPRAORBITAL NERVE from the forehead and anterior scalp and the SUPRATROCHLEAR NERVE from the bridge of the nose and medial portions of the upper eyelid and forehead. The nerve courses along the roof of the orbit toward the superior orbital fissure of the sphenoid bone , where it is joined by the lacrimal and nasociliary nerves to form V1.
- 73. The lacrimal nerve serve as a afferent nerve for the lateral portion of the eyelid, conjunctiva , and lacrimal gland. These nerves also responsible for the production of lacrimal fluid or tears. The nerve runs posteriorly along the lateral roof of the orbit and then joins the frontal and nasociliary nerves near superior orbital fissure of the sphenoid bone to form V1.
- 74. Several afferent nerve branches converge to form the NASOCILIARY NERVE. These branches include the INFRATROCHLEAR NERVE from the skin of the medial portion of the eyelid and the side of the nose, CILIARY NERVE to and from the eyeball and ANTERIOR ETHMOIDAL NERVE from nasal cavity and paranasal sinuses. The nasociliary nerve is an afferent nerve that runs within the orbit , superior to the second cranial nerve to join the frontal and lacrimal nerves near superior orbital fissure of the sphenoid bone to form V1.
- 77. The second division V2 from the sensory root of trigeminal nerve is the MAXILLARY NERVE. The afferent nerve branches of the maxillary nerve carry sensory information for the maxilla and overlying skin , maxillary sinuses , nasal cavity , palate ,and nasopharynx and a portion of the dura mater. The maxillary is a nerve trunk formed in the ptrygopalatine fossa by the convergence of many nerves.
- 78. The largest contributor is the infraorbital nerve. The tributaries of the maxillary nerve trunk include:- 1-zygomatic 2-anterior 3-middle 4-posterior 5-superior alveolar 6-greater and lesser palatine 7-nasopalatine nerves
- 80. The zygomatic is an afferent nerve composed of merger of the zygomaticofacial nerve and the zygomaticotemporal nerve in the orbit. The zygomatic nerve courses posteriorly along the lateral orbit floor , enters the pterygopalatine fossa through the inferior orbital fissure , between the sphenoid bone and maxilla, and finally joins V2.
- 81. The infraorbital nerve is afferent nerve formed from the merger of cutaneous branches from the upper lip , medial portion of the cheek , lower eyelid and side of nose. The infraorbital nerve then passes into the infraorbital foramen of the maxilla and travels posteriorly through infraorbital canal along with the infraorbital blood vessels ,where it is joined by the anterior superior alveolar nerve.
- 82. From the infraorbital canal and groove the infraorbital nerve passes into the ptrygopatatine fossa through the inferior orbital fissure. After it leaves the infraorbital groove and within the pterygopalatine fossa , the infraorbital nerve receives the posterior superior alveolar nerve.
- 83. The ASA serves as an afferent nerve of sensation including pain for the maxillary central incisors , lateral incisors and canine as well as their associated tissues. The ASA nerve originates from dental branches in the pulp tissue of these teeth that exit through the apical foramina. The ASA nerve also innervates the overlying facial gingiva.
- 84. The ASA nerve then ascends along the anterior wall of the maxillary sinus to join the IO in the infraorbital canal.
- 85. The MIDDLE SUPERIOR ALVEOLAR NERVE serves as an afferent nerve of sensation (including pain), typically for the maxillary premolar teeth and the mesiobuccal root of the maxillary first molar and their associated periodontium and overlying buccal gingiva. The MSA originates from dental branches in the pulp tissue that exit the teeth through the apical foramina , as well as interdental and interradicular branches from periodontium.
- 86. MSA nerve like PSA and ASA forms the dental plexus or nerve network in the maxilla. The MSA nerve then ascends to join the IO nerve by running in the lateral wall of maxillary sinus.
- 87. The PSA joins the IO nerve in the pterygopalatine fossa. The PSA nerve serve as an afferent nerve of sensation (including pain)for most potions of the maxillary molar teeth and their periodontium and buccal gingiva as well as the maxillary sinus. Some branches of PSA nerve remain external to the posterior surface of the maxilla. These external branches provide afferent innervation for the buccal gingiva that overlies the maxillary molars.
- 88. Other afferent nerve branches of the PSA nerve originate from dental branches in the pulp tissue of the each of the maxillary molar teeth that exit the teeth by way of apical foramina. These dental branches are then joined by interdental branches and interradicular branches from the periodontium forming a dental plexus or a nerve network in the maxilla for the region.
- 89. All these internal branches of PSA nerve exit from several posterior superior alveolar foramina on the maxillary tuberosity of the maxilla. Both the external and internal branches of the PSA nerve then ascend together along the maxillary tuberosity , which forms the posterolateral wall of the maxillary sinus to join either the IO nerve or maxillary nerve.
- 90. The PSA typically provides afferent innervation for the maxillary second and third molars and the palatal and distal buccal root of the maxillary first molar , as well as the mucous membranes of the maxillary sinus.
- 91. The MSA nerve serves as an afferent nerve of sensation including pain typically for the maxillary premolar teeth and mesiobuccal root of the maxillary first molar and their associated periodontium and overlying bucaal gingiva.
- 92. MSA nerve originate from dental branches in pulp tissue that exit the teeth through apical foramina,as well as interdental and imterradicular branches from the periodontium. MSA also form dental plexus in maxilla. MSA nerve then ascends to join INFERIOR ALVEOLAR NERVE by running in the lateral wall of maxillary sinus.
- 93. Posterior superior alveolar nerve or PSA joins the INFERIOR ALVEOLAR NERVE in the pterygopalatine fossa. The nerve serve as an afferent nerve of sensation (including pain) for most portions of the maxillary molar teeth and their periodontium and buccal gingiva as well as the maxillary sinus.
- 94. Some branches of the PSA nerve remain external to the posterior surface of maxilla. These external branches provide afferent innervation for the buccal gingiva that overlies the maxillary molars. Other afferent nerve branches of PSA nerve originate from dental branches in the pulp tissue of each of maxillary teeth and exit from the apical foramina of the teeth.
- 95. These dental branch are then joined by the interdental branches and interradicular branches from the periodontium and form the nerve plexus in the maxilla for the region. All these internal branches of PSA nerve exit from several POSTERIOR SUPERIOR FORAMINA on the maxillary tuberosity.
- 96. Both the external and internal branches of PSA then ascend together along the maxillary sinus which form the posterolateral wall of the maxillary sinus. Then it join the either IO or Maxillary nerve. The PSA nerve typically provides afferent innervation for the maxillary 2nd & 3rd molars and palatal and distal buccal root of the 1st molar as well as mucous membranes of the maxillary sinus.
- 97. Both palatine nerves join the maxillary nerve from the palate. GREATER PALATINE NERVE It is also known as Anterior palatine nerve. It is located between the periosteum and bone of the anterior hard palate. Nerve serves as an afferent nerve for the posterior hard palate and posterior palatal gingiva.
- 98. Posteriorly,the GP nerve enters the greater palatine foramen in the palatine bone near the maxillary 2nd or 3rd molar to travel in the pterygopalatine canal along with greater palatine blood vessels. Lesser Palatine Nerve It is also called Posterior Palatine nerve. Serve as an afferent nerve for the soft palate and tonsillar tissues.
- 99. The lesser palatine nerve enters the lesser palatine foramen in the palatine bone near its junction with pterygoid process of sphenoid bone,along ith lesser palatine blood vessels. The lesser palatine nerve join the greater palatine nerve in the pterygopalatine canal.
- 100. Both palatine nerves ascend through the pterygopalatine canal ,towards the maxillary nerve in the pterygopalatine fossa. On the way , palatine nerves are joined by the lateral nasal branches, which are afferent nerves from the posterior nasal cavity.
- 101. The Nasopalatine nerve or NP originate from the mucosa of the anterior hard palate, palatal to the anterior maxillary teeth. The right and left NP nerves enter the incisive canal by way of the incisive foramen , beneath the incisive papilla , thus exiting the oral cavity. The NP serve as an afferent nerve for the anterior hard palate , and the palatal gingiva of the maxillary anterior teeth as well as the nasal septal tissues.
- 102. The third division (V3) of the trigeminal nerve is the mandibular nerve. Which is a short main trunk formed by the merger of a smaller anterior trunk and a larger posterior trunk in the infraorbital fossa,before the nerve passes through the foramen ovale of the sphenoid bone.
- 103. The mandibular nerve then joins with the opthalmic and maxillary nerve to form the TRIGEMINAL GANGLION of the TRIGEMINAL NERVE.
- 105. Few branches arises from the V3 trunk before its separation to Anterior and Posterior trunks. These branches from the undivided mandibular nerve include the MENINGEAL BRANCHES, which are afferent nerves for portions of the Dura matter.
- 106. also from the undivided branch from the mandibular nerve are MASCULAR NERVE. They are efferent nerves for the medial pterygoid tensor tympani tensor veli palatine
- 107. Anterior trunk formed by the merger of the:- Buccal nerve additional muscular nerve branches Posterior trunk formed by the merger of the :- auriculotemporal nerve lingual nerve inferior alveolar nerve
- 109. The buccal nerve also known as long buccal nerve serve as an afferent nerve for skin of cheek , buccal mucous membranes and buccal gingiva of the mandibular posterior teeth. The nerve is located on the surface of the buccinator muscle. The buccal nerve then travels posteriorly in the cheek, deep to the masseter muscle.
- 110. at the level of the occlusal plane of the last manibular molar , the nerve crosses in front the anterior border of the ramus of the mandible then goes between the two heads of the lateral pterygoid muscle to join the anterior trunk of the V3.
- 111. They arises from the motor root of the trigeminal nerve. Muscular branches are:- 1- deep temporal nerve 2- masseteric nerve 3- lateral pterygoid muscle 1- DEEP TEMPORAL NERVE Usually 2 in number Anterior and posterior,efferent nerves They passes between the sphenoid bone and superior border of the lateral ptrygoid muscle then turn around the infratemporal crest of the sphenoid bone to end in the deep surface of the temporal muscle that they innervate.
- 112. 2- MASSETRIC NERVE It is also an efferent nerve. It is passes between sphenoid bone and superior border of the lateral pterygoid muscle. The nerve then accompanies the masseteric blood vessels through the mandibular notch to innervate the massetric muscle.
- 113. 3- LATERAL PTERYGOID MUSCLE A small sensory branch goes to the temporalmandibular joint,after the short course it enters the deep surface of the lateral pterygoid muscle. Between the muscle’s two heads of origin and serve as an efferent nerve for the muscle.
- 115. It travels with superficial temporal artery and vein serve as an afferent nerve for the scalp and external ear. It also carries the postganglionic parasympathetic fibers to the parotid salivary gland. The parasympathetic fibers arises from the lesser petrosal branch of the IXth cranial nerve.
- 116. The nerve runs deep to the lateral pterygoid muscle and the neck of the mandible ,then splits to encircle the middle meningeal artery and finally join the posterior trunk of the V3.
- 117. It is formed by the afferent branches of the body of the tongue that travels along the lateral surface of the tongue. Then it passes posteriorly, passing from the medial to the lateral surface of the duct of the sub mandibular galnd by going under the duct.
- 118. The lingual nerve communicate with the submandibualr ganglion located superior to the deep lobe of the submandibular gland. At the base of the tongue, the lingual nerve ascends and runs between the medial pterygoid muscle and the mandible, anterior and slightly medial to the inferior alveolar nerve. The lingual nerve then continues to travel upward to join the posterior trunk of V3.
- 119. It is serve as an afferent nerve for the general sensation for the body of the tongue, floor of the mouth and lingual gingiva of the mandibular teeth.
- 120. It is a main branch of the lower jaw. It is an afferent nerve formed by the merger of the MENTAL NERVE & INCISIVE NERVE. After forming inferior alveolar nerve travel posterior through the mandibular canal along with the inferior alveolar artery and vein. Join by the interdental and interradicualr branches of the peridontium and form the nerve plexus in the region.
- 121. then it exit the mandible through mandibular foramen , where it is joined by the mylohyoid nerve. Then travels lateral to the pterygoid muscle and between the ramus of the mandible and sphenomandibular ligamentwwithin the pterygomandibualr space. Then it join the posterior trunk of the V3.
- 122. It is composed of the external branches that serve as an afferent nerve for the chin ,lower lip ,labial mucosa of premolars and anterior teeth. The nerve then enters the mental foramen on the anterolateral surface of the mandible, usually between the apices of the mandibular premoalrs. Then it merge with the incisive nerve to form the inferior alveolar nerve in the mandibular canal.
- 123. It is an afferent nerve composed of dental branches from the mandibular premolars and anterior teeth that originate in the pulp tissue exit the teeth through the apical foramina , and then join with interdental branches from the surrounding periodontium forming the dental plexus in the region. It is merge to the mental nerve just posterior to the mental foramen to form the inferior alveolar nerve in the mandibular canal.
- 124. It is serve as an afferent nerve for the mandibular premolars and anterior teeth. MYLOHYOID NERVE After the inferior alveolar nerve exits the mandibular foramen, small branches occur called mylohyoid nerve. It pierces the sphenomandibular ligament and runs inferiorly and anteriorly in the mylohyoid groove then onto the inferior surface of the mylohyoid muscle.
- 125. It serves as an efferent nerve to the mylohyoid muscle and anterior belly of digestric muscle.
- 133. It is distinct neurological syndrome of deficits that can arise due to the closeness of the cerebellopalatine angle to specific cranial nerve. ETIOLOGIES:- Schwannoma Meningioma Tumor of the petrous bone
- 134. CLINICAL FEATURES:- Unilateral sensorineural hearing loss Unilateral tinnitus Disequilibrium (vertigo) rare NERVE AFFECTED:- cranial nerve V,VII,VIII,sometimes IX
- 135. Gradenigo syndrome first describe by GUISEPPE GRADENIGO in 1904. ETIOLOGIES:- petrositis tumor of the apex of the petrous bone CLINICAL FEATURES Periorbital unilateral pain related to trigeminal nerveinvolvement Diplopia due to VI nerve paralysis Persistent otorrhea
- 136. LOCALIZATION:- Apex of petrosal NERVE INVOLVED:- V VI
- 137. It is rare disorder. CLINICAL FEATURE:- Unilateral headache Orbital pain Weakness ¶lysis of extraocular muscle LOCALZIATION :- Lateral wall of cavernous sinus ETIOLOGIES:- Aneurysm /thrombosis of cavernous sinus NERVED INVOLVED:- III,IV, VI, V1 ,V2
- 138. ETIOLOGIES:- Aneurysm /thrombosis of cavernous sinus NERVED INVOLVED:- III,IV, VI, V1 ,V2
- 139. LOCALIZATION :- Superior orbital fissure ETIOLOGIES:- Invasive tumor of the sphenoid sinus Aneruysm Inflammatory granuloma Invasive sellar tumor
- 140. NERVES INVOLVED:- III IV VI V1
- 141. It is very rare pathological condition. Resulting from neuralgia of nasocilliary nerve. It is also known as nasal nerve syndrome. CLINICAL FEATURE:- Severe unilateral pain , generated by irritation of the ciliary ganglion. Affected areas:- Above and outside of nose Above the inner canthus Inferior angle of medial tarsal ligament
- 142. ASSOCIATED SYMPTOMS:- Unilateral vasomotor obstruction of the nasal fossa Sneezing Hydrorrhoea Cutaneous hyperasthesia Conjectival hypermia Keratitis Corneal ulcer
- 143. There might be:- slight inflammatory swelling of upper eyelid Photophobia Ciliary & conjectival infection
- 144. DIFFERENTIAL DIAGNOSIS cluster headache Trigeminal neuralgia Demyelinating disease
- 145. It is also known as shingles. It is secondary manifestation of varicella zoster infection. CLINICAL PRESENTATION:- Form of multiple vesicles along the course of one of the three division. Prodrome fever Headache Rash Malaise nausea
- 146. Rash Malaise Nausea Hutchinson’s sign
- 147. ORAL MANIFESTATION Vesicles affecting the palate , uvula ,tonsils , tongue Buccal mucosa floor of the mouth -devitalized teeth - internal resorption - Pulpal necrosis - Severe periodontitis
- 154. It also known as STYLOHYOD SYNDROME,STYLOID SYNDROME , STYLOID –STYLOHYOID SYNDROME ,STYLOID CAROTID ARTERY SYNDROME. It is first described by Watt Weems eagle in 1937. It is characterized by elongated styloid process , or calcification of stylohyoid ligament. Classical eagle syndrome is ipsilateral.
- 155. CLINICAL FEATURE:- Sharp , shooting pain in the jaw ,back of the throat , base of tongue , ears ,neck or face. Difficulty swallowing Pain from chweing , swallowing , turning the neck or touching the back of the throat. tinnitus
- 157. NERVE INVOLVED:- Glossophyrangeal Facial nerve Hypoglossal nerve Vegus nerve V3
- 158. DIIFERENTIAL DIAGNOSIS Pulpitis Idiopathic trigeminal neuralgia TMJ disorder
- 159. The abducent nerve carries GSE fibers to innervate the lateral rectus muscle in the orbit.
- 160. Nerve exits the skull through the superior orbital fissure of sphenoid bone on its way to the orbit. Runs through the sinus , close to the internal carotid artery.
- 162. It contains both afferent and efferent components. Nerve carries the Efferent component for the:- muscle of facial expression preganglionic parasympathetic fiber of the lacrimal gland , submandibular gland and sublingual gland. Afferent component serves:- tiny patch skin behind the ear taste sensation body of the tongue
- 164. Nerve leaves the cranial cavity by passing through the internal acoustic meatus in the petrous region of the temporal bone. Within the bone the nerve gives off small efferent branch to the muscle in the middle ear and two large branches GREATER PETROSAL AND CHORDA TYMAPNI. Both of which carry parasympathetic fibers.
- 166. The main trunk emerges from the skull through the stylomastoid foramen of the temporal bone and gives off two branches POSTERIOR AURICULAR NERVE and NERVE TO POSTERIOR BELLY OF DIGESTRIC MUSCLE &STYLOID MUSCLE. Then passes into the parotid salivary gland divides into several branches &innervate muscles of facial expression.
- 167. It carries the efferent fibers preganglionic parasymapthrtic fibers to ptrygopalatine ganglion in pterygopalatine fossa. Also carries the afferent fibers for taste sensation in the palate.
- 169. It arises before the facial nerve exit from the skull, join with the branches of the maxillary nerve of the trigeminal nerve,to be carried to the lacrimal gland , nasal cavity minor salivary gland of the hard and soft palate. It also carries afferent nerve fibers for taste sensation in the palate.
- 170. It is the small branch of the facial nerve. Parasympathetic efferent nerve for the submandibular and sublingual galnd. Afferent nerve for the taste sensation. It is branching off the facial nerve within the petrous portion of the temporal bone.
- 172. Crosses the medial surface of the tympanic membrane. Exit the skull by petrotymapni fissure,travel with the lingual nerve along the floor of the mouth.
- 174. It is arises opposite the pyramid of the middle ear , and supplies the stapedius muscle. The muscle dampens excessive vibrations of the stapes caused by high - pitched sounds. Paralysis of stapedius muscle caused Hyperacusis.
- 175. It arises just below the stylomastoid foramen. It ascends between the mastoid process and the external acoustic meatus. It supplies :- auricularis posterior occipitalis intrinsic muscles on the back of the auricle.
- 177. It arises close to the stylomastoid foramen. It is short and supplies to posterior belly of digestric muscle.
- 178. It arises with the digestric branch. It is long and supplies the stylohyoid muscle. THE TEMPORAL BRANCH It crosses the zygomatic arch and supply:- auricularis anterior Auricularis superior Intrinsic muscles on the lateral side of the ear Frontalis Orbicularis oris Corrugator supercilii
- 179. It runs across the zygomatic bone and supplies the orbicularis oculi. THE BUCCAL BRANCHES It is two in number. Upper buccal nerve:- it runs above the parotid duct. Lower buccal branch:-it runs below the parotid duct. Innervates :- They supply muscles in that vicinity especially the buccinator.
- 180. It runs below the angle of the mandible deep to platysma. It crosses the body of the mandible and supplies muscle of lower lip and chin. THE CERVICAL BRANCH It emerges from the apex of the parotid gland and runs downwards and forwards in the neck. It supply the platysma.
- 181. For effective coordination between the movements of the muscles of the first , second , and the third branchial arches , the motor nerves of the three arches communicate with each other. The facial nerve also communicates with sensory nerves distributed over its motor territory.
- 188. PERIPHERAL FACIAL PARALYSIS CLINICAL PRESENTATION:- Unilateral facial weakness Loss of taste Hyperacusis Decreased salivation Decreased tear secretion
- 191. It is also known as BOGOARD’S SYNDROME. It is rare complication. ETIOLOGY:- Aberent regeneration after Trauma CLINICAL PRESENTATION Lacrimation during eating
- 192. Involvement of geniculate ganglia by HERPES ZOSTER. CLINICAL PRESENTATION:- Hyperacusis Loss of lacrimation Loss of sensation of taste in anterior two third of tongue Bell’s palsy Lack of salivation Vesicle on auricle
- 194. It is rare condition. It is serious autoimmune disorder in which the immune system attacks healthy nerve cells in peripheral nervous syndrome. CLINCAL PRESENTATION:- Tingling sensation in toes , feet , and legs . Muscle weakness Difficulty moving eyes face chewing or swallowing Severe lower back ache
- 195. Rapid heart rate Difficulty in breathing paralysis
- 196. It is rare neurological disorder Characterized by paralysis of multiple cranial nerve , most often the VI and VII cranial nerve. CLINICAL PRESENTATION:- Micrognathia Microstomia Cleft palate Dental abnoramalties Strabismus
- 197. Ptosis Hypotonia Hypoacusis Mask like face Incompetent lips Ulceration
- 199. It is also known as BAILLARGER’S SYNDROME , DUPUY’S SYNDROME , AURICULOTEMPORAL SYNDROME , FREY-BAILLARGER SYNDROME. It is rare postoperative phenomenon following salivary gland surgery , facelift procedures, trauma. It is characterized by gustatory sweating and flushing in the preauricular area in response to mastication or salivary stimulation. It was first described by Lucie Frey in 1923 and was termed auriculotemporal syndrome.
- 201. CLINICAL PRESENTATION:- flushing Sweating Burning Itching
- 202. It is serve as an afferent nerve for hearing and balance. Nerve enters the cranial nerve through the internal acoustic meatus of the temporal bone.
- 203. LARGE VESTIBULAR AQUEDUCT SYNDROME:- It is congenital malformation of cochlea and semicircular canal. Hypoacusis
- 204. It is an illusion rotatory movement due to disturbed orientation of the body in space. It is due to disease of vestibular nerve. ETIOLOGIES:- Meniere’s disease Vestibular neuritis Head or neck injury Tumor or stroke Migraine headache
- 205. CLINICAL PRESENTATION:- Dizziness Nausea Nystagmus Sweating Hearing loss in one ear tinnitus
- 206. It is very frequent disorder. It consist of perception of a sensation of sound localized in one or both ear. TYPE OF TINNITUS Subejctive objective
- 215. Carries the effernt component for the phyryngeal muscle, stylopharygeus muscle and preganglionic parasympathetic innervation for the parotid galnd. Afferent component for the:- pharynx taste general sensation of the base of the tongue
- 217. Pharyngeal branch – combines with fibres of the vagus nerve to form the pharyngeal plexus. It innervates the mucosa of the oropharynx. Lingual branch – provides the posterior 1/3 of the tongue with general and taste sensation
- 218. Tonsillar branch – forms a network of nerves, known as the tonsillar plexus, which innervates the palatine tonsils.
- 219. Lesion of glossophyrangeal nerve causes:- Absence of taste from posterior one third of tongue Absence of secretion of parotid gland Loss of pain sensations from tongue , tonsil , pharynx , and soft palate Gag reflex is absent
- 220. It is sharp ,shooting severe attack of pain affecting posterior part of pharynx. JUGULAR FORAMEN SYNDROME It is also known as VERNET’S SYNDROME. It involved usually IX , X , XI cranial nerve CLINICAL PRESENTATION:- Dysphonia Soft palate dropping Deviation of uvula towards the normal side
- 221. Dysphagia Loss of sensory function from the posterior 1/3rd of tongue Sternocleidomastoid and trapezius muscle paralysis ETIOLOGIES:- 1-Tumors:- Glommus jugulare tumors Meningioma
- 222. 2-Inflammation:- Meningitis Malignant otitis externa Sarcoidosis 3- Trauma 4- narrowing of jugular foramen
- 223. It is rare disease. It involved the IX X XI XII cranial nerve. Characterized by:- Constricted pupil(miosis) Drooping of upper eyelid(ptosis) Absence of sweating (anhidrosis) enopthalmous
- 230. NERVE INVOLVED:- Facial nerve Occulomotor nerve
- 231. It is also known as Pnumogastric nerve. Large efferent component for the muscles of the:- soft palate larynx Parasympathetic fibers for the:- thorax heart stomach thymus gland
- 232. Carries small afferent fibers for :- small amount of skin around ear taste sensation epiglottis
- 234. In the Head :- Within the cranium, the auricular branch arises. This supplies sensation to the posterior part of the external auditory canal and external ear. In the Neck In the neck, the vagus nerve passes into the carotid sheath, travelling inferiorly with the internal jugular vein and common carotid artery. At the base of the neck, the right and left nerves have differing pathways:
- 235. The right vagus nerve passes anterior to the subclavian artery and posterior to the sternoclavicular joint, entering the thorax. The left vagus nerve passes inferiorly between the left common carotid and left subclavian arteries, posterior to the sternoclavicular joint, entering the thorax.
- 236. Several branches arise in the neck: Pharyngeal branches – Provides motor innervation to the majority of the muscles of the pharynx and soft palate. Superior laryngeal nerve – Splits into internal and external branches. The external laryngeal nerve innervates the cricothyroid muscle of the larynx. The internal laryngeal provides sensory innervation to the laryngopharynx and superior part of the larynx.
- 237. Recurrent laryngeal nerve (right side only) – Hooks underneath the right subclavian artery, then ascends towards to the larynx. It innervates the majority of the intrinsic muscles of the larynx
- 238. In the Thorax In the thorax, the right vagus nerve forms the posterior vagal trunk, and the left forms the anterior vagal trunk. Branches from the vagal trunks contribute to the formation of the oesophageal plexus, which innervates the smooth muscle of the oesophagus.
- 239. Two other branches arise in the thorax: Left recurrent laryngeal nerve – it hooks under the arch of the aorta, ascending to innervate the majority of the intrinsic muscles of the larynx. Cardiac branches – these innervate regulate heart rate and provide visceral sensation to the organ. The vagal trunks enter the abdomen via the oesophageal hiatus, an opening in the diaphragm.
- 240. In the Abdomen In the abdomen, the vagal trunks terminate by dividing into branches that supply the oesophagus, stomach and the small and large bowel (up to the splenic flexure)
- 243. It carries the efferent component for the TRAPEZIUS AND STERNOCLEIDOMASTOID muscle as well as for muscle of soft palate and pharynx. It passes through the skull by the way of jugular foramen between occipital and temporal bone.
- 247. It function as efferent nerve for:- intrinsic muscle extrinsic muscle of the tongue It exit the skull through the hypoglossal canal In the occipital bone.
- 251. TAPIA’S SYNDROME: -it invoved the X , XII cranial nerve. CLINICAL PRESENTATION:- Dysphonia Deviation of tongue Dysphagia
- 252. A bulbar palsy refers to disease affecting the glossopharyngeal, vagus, accessory and hypoglossal nerves and is due to lower motor neuron pathology. CLINICAL PRESENTATION:- dysphagia, dysarthria, flaccid pareses, atrophy and fasciculation of muscles supplied by those cranial nerves and fibrilliation of the tongue
- 253. weakness of the palate reduced or absent gag reflex, dribbling of saliva and nasal speech.
- 254. The inferolateral trunk of carotid siphon vascualrize the:- V1 III IV VI
- 255. The ascending pharyngeal artery vacularize :- IX X XI XII The middle meningeal and accessory arteries ,the inferolateral trunk of the carotid siphon and ascending pharyngeal artery have abundant anastomoses.
- 256. Textbook of anatomy ;gray’s 39th edition Textbook of antomy of the head and neck- margaret j. fehrenbach, susan . Herring Textbook of cranial nerve- Dominique doyon ,Kathlyn marsot – dupuch ,Jean –paul Francke Textbook of human antomy-B D Chaurasia vol 3 6th edition Textbookof oral medicine – Burket’s 10th edition Journal of medical case reports ISSN :1752-147 Erol FS,Kaplan M, Ozveren MF.Jugular foramen syndrome caused by choleastatoma.Clin Neurol Neurosurg.2005jun;107(4):342-6. PMID:15885397
- 257. Chandrashekhar S , PeterfreundRA.Horner’s syndrome following very low concentration Bupivacaine infusion for labor epidural analgesia .J Clin Anesth. 2003;15:217-19 Malik U,Sunil MK ,Gupta C , Kumari M.Trigeminal HerpesZoster:Early Recognition and Treatment-A Case Report.J Indian Acad Oral Radiol 2017;2;350-3.
- 258. Singh MP,Mukherji A , Vats Ak. Arare case of Charlin’s syndrome.J Indian Acad Oral Med Radiol 2017;29;129-31 Raina D , Gothi R, Rajan S .J Radiol Imaginig.2009 May;19(2):107-108 Motz M K , Kim J Y,Otolaryngeal Clin North Am.2016 Apr;49(2):501-501 Adams et al., Principles of Neurology, 6th ed, p1091; Brain 1992 Dec;115(Pt 6):1889-1900)