Food Protein-induced Allergic Proctocolitis to Multiple Foods
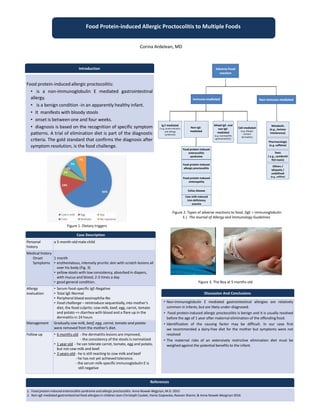
- 1. Food Protein-induced Allergic Proctocolitis to Multiple Foods Introduction Food protein-induced allergic proctocolitis: • is a non-immunoglobulin E mediated gastrointestinal allergy. • is a benign condition -in an apparently healthy infant. • It manifests with bloody stools • onset is between one and four weeks. • diagnosis is based on the recognition of specific symptom patterns. A trial of elimination diet is part of the diagnostic criteria. The gold standard that confirms the diagnosis after symptom resolution, is the food challenge. Case Description Discussion And Conclusions • Non-immunoglobulin E mediated gastrointestinal allergies are relatively common in infants, but are likely under-diagnosed. • Food protein-induced allergic proctocolitis is benign and it is usually resolved before the age of 1 year after maternal elimination of the offending food. • Identification of the causing factor may be difficult. In our case first we recommended a dairy-free diet for the mother but symptoms were not resolved • The maternal risks of an extensively restrictive elimination diet must be weighed against the potential benefits to the infant. References 1. Food protein-induced enterocolitis syndrome and allergic proctocolitis Anna Nowak-Węgrzyn, M.D. 2015 2. Non-IgE-mediated gastrointestinal food allergies in children Jean-Christoph Caubet, Hania Szajewska, Raanan Shamir, & Anna Nowak-Wezgrzyn 2016 Personal history a 5-month-old male child Medical history Onset Symptoms 1 month • erythematous, intensely pruritic skin with scratch lesions all over his body (Fig. 3) • yellow stools with low consistency, absorbed in diapers, with mucus and blood, 2-3 times a day • good general condition. Allergy evaluation • Serum food-specific IgE-Negative • Total IgE-Normal • Peripheral blood eosinophilia-No • Food challenge – reintroduce sequentially, into mother’s diet, the food culprits: cow milk, beef, egg, carrot, tomato and potato => diarrhea with blood and a flare up in the dermatitis in 24 hours Management Gradually cow milk, beef, egg, carrot, tomato and potato were removed from the mother's diet. Follow up • 6 months old - the dermatitis lesions are improved, - the consistency of the stools is normalized • 1 year old - he can tolerate carrot, tomato, egg and potato, but not cow milk and beef. • 2-years-old - he is still reacting to cow milk and beef - he has not yet achieved tolerance. - the serum milk-specific immunoglobulin E is still negative Figure 2. Types of adverse reactions to food. (IgE = immunoglobulin E.) The Journal of Allergy and Immunology Guidelines. CCMCorina Ardelean, M.D. Metabolic (e.g., lactose intolerance) Pharmacologic (e.g. caffeine) Toxic ( e.g., combroid fish toxin) Others / idiopatic / undefined (e.g., sulfites) Cell-mediated (e.g. allergic contact dermatitis) Mixed IgE- and non IgE- mediated (e.g. eosinophilic gastroenteritis) Non-IgE- mediated Food protein-induced enterocolitis syndrome Food protein-induced allergic proctocolitis Food protein-induced enteropathy Celiac disease Cow milk-induced iron deficiency anemia Immune-mediated Non-immune-mediated Adverse Food reaction Ig E mediated ( e.g.,acute urticaria, oral allergy syndrome) Figure 3. The Boy at 5 months old 65% 14% 5% 2% 7% 7% Cow's milk Egg Soy Corn Multiple No repsonse Figure 1. Dietary triggers