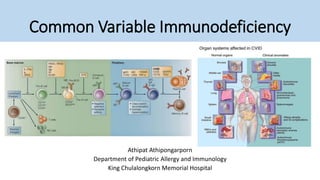
Common variable immunodeficiency
- 1. Common Variable Immunodeficiency Athipat Athipongarporn Department of Pediatric Allergy and Immunology King Chulalongkorn Memorial Hospital
- 2. Outline • Definition • Epidemiology • Diagnosis and Differential Diagnosis • Clinical Manifestation • Management
- 3. History 20161971 Definition CVID by WHO “less well-defined antibody deficiency syndromes” The International Union of Immunological Societies Expert Primary Immunodeficiency Committee 2009 : heterogeneous nature of these hypogammaglobulinemic states 2009 Francisco A. Bonilla et. al. JACI in practice. 2015 1999 Conley et al Ig G, IgA, IgM< -2SD Ameratunga et al Age > 4 Y Clinical and immunological criteria Histological markers 2013 2014 ESID Registry Age > 4 Y Clinical and immunological criteria ICON
- 4. R. Ameratunga. Clinical and Experimental Immunology, 174: 203–211
- 5. R. Ameratunga. Clinical and Experimental Immunology, 174: 203–211
- 7. Diagnosis • A male or female patient who has a marked decrease of IgG (at least 2 SD below the mean for age) and a marked decrease in at least one of the isotypes IgM or IgA and • Onset of immunodeficiency at greater than 2 years of age • Absent isohemagglutinins and/or poor response to vaccines • Defined causes of hypogammaglobulinemia have been excluded according to a list of differential diagnosis Francisco A. Bonilla et. al. JACI in practice. 2015
- 8. Consensus definition of CVID • Most patients will have • At least 1 of the clinical manifestations (infection, autoimmunity, lymphoproliferation) • A diagnosis of CVID may be conferred on asymptomatic individuals who fulfill criteria 2 to 5, especially in familial cases. • Hypogammaglobulinemia should be defined according to the age adjusted • The IgG level must be repeatedly low in at least 2 measurements more than 3 weeks apart in all patients. • Repeated measurement may be omitted if the level is very low (<100-300 mg/dL depending on age), other characteristic features are present, and it is considered in the best interest of the patient to initiate therapy with IgG as quickly as possible. • IgA or IgM level must also be low. • Note that some experts prefer a more narrow definition requiring low IgA level in all patients Francisco A. Bonilla et. al. JACI in practice. 2015
- 9. Consensus definition of CVID • All patients with an IgG level of more than 100 mg/dL should be studied for responses to T-dependent (TD) and T-independent (TI) antigens • In all patients undergoing such testing, there must be a demonstrable impairment of response to at least 1 type of antigen (TD or TI). • At the discretion of the practitioner, specific antibody measurement may be dispensed with if all other criteria are satisfied and if the delay incurred by prevaccination and postvaccination antibody measurement is thought to be deleterious to the patient’s health. • Other causes of hypogammaglobulinemia must be excluded (Table I). • Genetic studies to investigate monogenic forms of CVID or for disease-modifying polymorphisms are not generally required for diagnosis and management in most of the patients, • Especially those who present with infections only without immune dysregulation, autoimmunity, malignancy, or other complications. • In these latter groups of patients, however, single gene defects may be amenable to specific therapies (eg, stem cell therapy) and molecular genetic diagnosis should be considered when possible. Francisco A. Bonilla et. al. JACI in practice. 2015
- 10. Francisco A. Bonilla et. al. JACI in practice. 2015
- 11. Francisco A. Bonilla et. al. JACI in practice. 2015
- 12. Epidemiology • Almost every primary immunodeficiency registry available for consultation reports a predominance of antibody defects (generally >50%) • CVID is the most frequent symptomatic antibody deficiency diagnosed in adulthood • IgA deficiency and CVID reported as the most frequent types • The United States Immunodeficiency Network registry contains 3,459 subjects, with 1,049 subjects with CVID (30%). Francisco A. Bonilla et. al. JACI in practice. 2015
- 13. Pathogenesis
- 14. Pathogenesis • B cell defect • T cell defect • DC defect • Chronic immune activation
- 15. B cell defect • Decrease isotype-switched B cells in a majority (not all) and a loss of plasma cells in both bone marrow and mucosal tissues. • B cells of some subjects produce normal amounts of immunoglobulin in culture, others produce only IgM, and others are unable to produce any immunoglobulin at all • These defects are variably present in patients with CVID, underlying the significant heterogeneity of this disease population Francisco A. Bonilla et. al. JACI in practice. 2015
- 16. Francisco A. Bonilla et. al. JACI in practice. 2015
- 17. T cell defect • Relative loss of T-cell function in many subjects • Defects in thymic maturation, monocyte/dendritic cell defects and impaired innate immune responses48 including loss of natural killer cells • Several studies have identified • Decreases in the number of naive CD4 cells in the peripheral blood • Defective generation of T-cell precursors in the bone marrow • Decreased numbers of Treg in the peripheral blood Francisco A. Bonilla et. al. JACI in practice. 2015
- 18. DC defect • Both plasmacytoid and myeloid DCs are present in decreased number in the peripheral blood of patients with CVID • The reason for the decrease in DC number is not known • No quantitative abnormality of DC precursors in bone marrow and tissue Jordan K. Abbott. Immunol Allergy Clin N Am 35 (2015) 637–658
- 19. Chronic immune activation • T cells, invariable natural killer T cells (iNKT) and monocytes • Elevated sCD14 levels • Exhausted bacteria-specific T cells and detectable lipopolysaccharide levels in the plasma who inadequate immunoglobulin replacement suggests that bacterial translocation from the GI tract • Adequate IVIg • transiently decrease numbers of inflammatory monocytes • Infection prevention • Antiinflammatory effects Jordan K. Abbott. Immunol Allergy Clin N Am 35 (2015) 637–658
- 20. Genetics
- 21. Genetics • Most cases of CVID are sporadic. • 5% to 25% are familial, with an AD pattern • CVID/IgAD families : several putative susceptibility loci identified within the HLA region on chromosome 6p • Most of the patients inherited HLA *DQ2, *DR7, *DR3, *B8, and/or *B44 • Monogenic causes of biallelic deleterious mutations in ICOS, TNFRSF13C CD19, CD20, CD21, CD81, and TNFRSF13B • Mutations in various nonredundant genes have been shown to be disease causing in some patients who fulfill criteria for CVID Francisco A. Bonilla et. al. JACI in practice. 2015 Jordan K. Abbott. Immunol Allergy Clin N Am 35 (2015) 637–658
- 22. Genetics • Particular polymorphisms in the TACI (TNFRSF13B) and MSH5 genes may affect the phenotype of about 5% to 8% of the patients with CVID • Impair T-cell independent class-switch recombination because interactions between TACI and its ligands • APRIL [a proliferation-inducing ligand] • BAFF [B cell activating factor] Francisco A. Bonilla et. al. JACI in practice. 2015
- 23. Delfien J A Bogaert et. al. J Med Genet 2016;53:575–590
- 24. Delfien J A Bogaert et. al. J Med Genet 2016;53:575–590 Genes encoding receptors ligands
- 25. Delfien J A Bogaert et. al. J Med Genet 2016;53:575–590 Genes encoding intracellular signal molecules
- 26. Group Gene Inherit ance Onset Clinical spectrum Gene encoding receptor and ligands ICOS deficiency (3.74%) AR Infant and childhood RTI, GI infections, bacterialskin infections, localised herpes simplex infections,bronchiectasis, AI (incl. AI cytopenia, rheumatic disease, IBD), organomegaly, granulomata, malignancy. TACI Monoall elic/ biallelic Early childhood to adulthood BAFF-R Monoall elic/ biallelic Infancy to late adulthood LRBA (26.4%) AR Infancy to childhood Severe AI (incl. AI cytopenia, severe IBD, type 1 diabetes mellitus), severe (EBV-induced) lymphoproliferation with generalised BLH and lymphocytic infiltration of organs (eg, kidney, brain), LIP, GLILD, granulomata Gene encoding intracellular signal molecules Protein kinase C delta (2.14%) AR Infancy to early childhood Severe systemic AI with features reminiscent of SLE , severe (EBV/ CMV-induced) lymphoproliferation with generalized BLH, splenomegaly, hepatomegaly, RTI, GI infections, UTI, failure to thrive PIK3 CD (26.7%) AD Infancy to early childhood RTI, GI infections, bacterial skin infections, deep abscesses, warts, persistent CMV/EBV viraemia, failure to thrive, bronchiectasis, AI (AI cytopenia, IBD, AI primary sclerosing cholangitis) Delfien J A Bogaert et. al. J Med Genet 2016;53:575–590
- 27. Genetics • Molecular genetic analysis of patients is not a requirement for conferring the diagnosis • In light of the possible definitive or supportive therapies (HSCT, cytokine therapy) that may be afforded to patients with specific genetic defects Francisco A. Bonilla et. al. JACI in practice. 2015
- 29. Unusual infections • Recurrent urinary tract or uterine cervical infections due to Ureaplasma urealyticum • Arthritides and lung infections may also be caused by Ureaplasma or Mycoplasma organisms • Enteroviral infections may cause meningoencephalitis or a dermatomyositis- like syndrome • Opportunistic infections should raise suspicion for a combined immunodeficiency or diagnosis other than CVID Francisco A. Bonilla et. al. JACI in practice. 2015
- 30. Chronic lung disease • Sequelae of recurrent acute infections • Lymphoid interstitial pneumonia or follicular bronchitis/bronchiolitis • Airway inflammation: Obstructive or restrictive disease and bronchiectatic changes • Immune-mediated pathology • Granulomatous lymphocytic interstitial lung disease • Although not necrotizing, are not perilymphatic as in sarcoidosis • Mediastinal lymphadenopthy • Investigation: chest CT scan → gas transfer obtained at the time of diagnosis , baseline for comparison in the future • Mortality in CVID was linked to both structural and functional lung impairment Francisco A. Bonilla et. al. JACI in practice. 2015
- 31. Nisha Verma. Lancet Respir Med 2015; 3: 651–60
- 32. Bronchiectasis • Definition : permanent abnormal dilatation of the airways in conjunction with persistent or recurrent bronchial sepsis • Chronic productive cough, susceptibility to recurrent exacerbations, and breathlessness • The prevalence of bronchiectasis in CVID (23% across a European cohort of 902 patients) Nisha Verma. Lancet Respir Med 2015; 3: 651–60
- 33. Bronchiectasis • Management • Correction of the underlying defect (IVIg replacement) • Sputum clearance training from a respiratory physiotherapist, • prevention of further infection • influenza and Pneumococcal vaccines Nisha Verma. Lancet Respir Med 2015; 3: 651–60 Radiologic findings - Increased bronchoarterial ratio (> 1.5) - Bronchial wall thickening: normally wall of bronchus should be less than half the width of the accompanying pulmonary artery branch - mucoid impaction - Signs described on CT include: : tram-track sign, signet ring sign, string of pearls sign , cluster of grapes sign https://radiopaedia.org/articles/bronchiectasis
- 34. Granulomatous lymphocytic interstitial lung diseases : GLILD • Associated with autoimmune cytopenia, splenomegaly, enteritis, and adenopathy • Cough and breathlessness. Impairment in gas transfer seems to be the most frequent abnormality on lung function testing • DDx : infection, other interstitial lung diseases, and lymphoma • Investigations : bronchoalveolar lavage (BAL) before the biopsy to exclude infection • A higher CD4:CD8 ratio was associated with a more favourable outcome in terms of lung function decline Nisha Verma. Lancet Respir Med 2015; 3: 651–60
- 35. Granulomatous lymphocytic interstitial lung diseases : GLILD • First-line therapy : High-dose corticosteroids • Prednisone 1 mg/kg per day until a maximum improvement in lung function and radiology • Combine IVIg + steroid for patient who not response steroid alone Nisha Verma. Lancet Respir Med 2015; 3: 651–60 Radiologic findings -Irregular ground-glass nodules in a peribronchovascular distribution - bulky mediastinal and hilar Lymphadenopathy - fluffy tree-in- bud “cotton-in-bud” distribution Basheer et. al.Clin Respir J. 2018;12:337–343
- 36. • Optional treatment • Rituximab plus azathioprine (targeting T cells) in a small series : improved spirometry values and fewer imaging abnormalities • Ciclosporin and abatacept Nisha Verma. Lancet Respir Med 2015; 3: 651–60
- 37. Pulmonary assessment in CVID • Asymptomatic patients and absence of other biological markers • CT assessment at diagnosis • Repeat CT assessments (in our practice every 5 years to limit lifetime radiation exposure with repeated scanning) • Annual lung function screening) • Symptomatic patients • Serial lung function testing every 6–12 months, depending on severity • Repeat CT imaging, since lung involvement • Patients whose genetic defect affects DNA recombination and DNA repair, leading to radio-sensitivity → Prefer MRI than CT Nisha Verma. Lancet Respir Med 2015; 3: 651–60
- 38. Diffuse granulomatous disease • Granulomatous disease or atypical sarcoid like lesions occur in 8% to 22% • Lungs, lymph nodes, and spleen are commonly affected • Noncaseating, and microbial associations have not been described • DDx sarcoidosis : Hypergammaglobulinemia, monocytosis Francisco A. Bonilla et. al. JACI in practice. 2015
- 39. • Methods • French DEFI cohort, a prospective study on adults with hypogammaglobulinemia. • The medical charts of. • Population • 436 subjects with CVID • 59 patients (13.5 %) were diagnosed with GD • 55 patients (93 %) of the GD cohort were reviewed • Results • Corticosteroids were the most frequently used drug. • Other drugs : cyclophosphamide, hydroxychloroquine, rituximab and methotrexate. Azathioprine, cyclosporine, mycophenolate mofetil Jean-Nicolas Boursiquot et. al. J Clin Immunol (2013) 33:84–95
- 40. Jean-Nicolas Boursiquot et. al. J Clin Immunol (2013) 33:84–95 GD+ group - Lower IgG, lower ALC, lower T cell, lower B cell - 59 patients (13.5 %) were diagnosed with GD in one or more organs - Patients from the GD+ group had a more severe immune deficiency with lower CD4+CD45RA+naive T cell (13.9 % vs 31.5 %) and lower CD19+CD27+ memory B cells (9 % vs 18 %)
- 41. Jean-Nicolas Boursiquot et. al. J Clin Immunol (2013) 33:84–95
- 42. - Systemic oral steroids were the most frequently used drug (54 TR in 31 patients) and most of the complete responses were achieved with this medication - Cyclophosphamide, hydroxychloroquine, rituximab and methotrexate have also led to complete responses in a few cases - Complete response was most commonly seen in lymph nodes
- 43. Autoimmunity • 25% to 30% of the patients • The most common : ITP, AIHA, Evans syndrome • Other autoimmune diseases : enteropathy, granulomatous disease, splenomegaly and splenectomy, low IgA level, and later age of onset Francisco A. Bonilla et. al. JACI in practice. 2015
- 44. Gastrointestinal disease • Some form of enteropathy was found in 9% of the patients • High rate of nonmalignant mortality, possibly due to malabsorption • Unexplained persistent chronic diarrhea, weight loss, steatorrhea, and malabsorption with loss of both minerals and fat soluble vitamins • Bacterial overgrowth is common and can lead to bloating and worsening diarrhea Francisco A. Bonilla et. al. JACI in practice. 2015
- 45. Lymphoid hyperplasia • Cervical, mediastinal, and abdominal lymphoid hyperplasia and/or splenomegaly are found in at least 20% • splenomegaly was reported in 26% • Lymph nodes biopsy : atypical lymphoid hyperplasia, reactive lymphoid hyperplasia, or granulomatous inflammation • Clonal lymphocytes is not diagnostic of lymphoma because these can be found in CVID lymphoid tissue showing reactive hyperplasia • Splenomegaly can be massive and yet not cause clinical symptoms Francisco A. Bonilla et. al. JACI in practice. 2015
- 46. Malignancy • Possibly 6% to 9% of the patients • Lymphomas are the most common • Ratio for lymphoma in CVID : normal population was 12:1 and for stomach cancer was 10:3 Francisco A. Bonilla et. al. JACI in practice. 2015
- 47. Jordan K. Abbott. Immunol Allergy Clin N Am 35 (2015) 637–658
- 48. Investigations
- 49. Laboratory manifestations • United States and in Europe have suggested that IgG levels of less than 4.5 g/L are found in most patients with CVID (85%-94%) • IgM levels are variable • IgA levels are low or undetectable in CVID, with 70% • There are several reported cases of patients with selective IgA deficiency with normal IgG level at initial evaluation in whom IgG levels slowly decline until they fulfill laboratory criteria for CVID • 21% of the patients with CVID may have very low levels or absence of all immunoglobulin isotypes at presentation Francisco A. Bonilla et. al. JACI in practice. 2015
- 50. Specific antibody production • Antigen-specific IgG levels or vaccine responses : within normal limits at initial presentation, but may decrease over time • Large proportion of children (73%) retained normal isohemagglutinin titers and specific antibody responses to protein antigens • Absent responses to pneumococcal polysaccharide antigens was noted in 71% of children Francisco A. Bonilla et. al. JACI in practice. 2015
- 51. Flow cytometry • Most patients with CVID will have normal levels of total circulating T cells and natural killer cells in peripheral blood • B-cell numbers are variable • 54% of the patients had normal levels (6%-16%) • 19% had increased levels (>17%) • 12% had reduced levels (1%-6%) • 12% had undetectable levels Francisco A. Bonilla et. al. JACI in practice. 2015
- 52. Flow cytometry • CD27+IgM-IgD- associated with splenomegaly, granulomatous disease, possibly chronic lung disease, and autoimmunity • Transitional B cells (CD38hi IgM hi ) and CD21low B cells associated with lymphadenopathy and splenomegaly Francisco A. Bonilla et. al. JACI in practice. 2015
- 53. Late-onset combined immune deficiency (LOCID) • 9% of CVID patients • Decrease in the naive CD4 population (CD45RA+CCR7+CD4+) • CD4 T-cell count of less than 200 cells/mL • Opportunistic infection • Intestinal disease, splenomegaly, lymphomas, and granulomas • Similar to Good syndrome (without thymoma) Francisco A. Bonilla et. al. JACI in practice. 2015
- 54. Serum immunoglobulins • Low IgG and low IgA or low IgM • Diagnosis merits demonstration of persistently low serum immunoglobulin levels (as discussed previously) before starting IgG therapy • IVIg therapy should not be unduly delayed if harmful condition • Quantitation of IgG subclasses is not relevant to the diagnosis • Elevate IgE is unusual in this setting : immune dysregulation Francisco A. Bonilla et. al. JACI in practice. 2015
- 55. Assessment of vaccine responses • Vaccine responses should be determined in all patients except those who present with very low or undetectable IgG levels • Tetanus and diphtheria toxoids, Haemophilus influenza type B, and pneumococcal vaccine • Meningococcus (both protein-conjugate and polysaccharide preparations) and pure polysaccharide salmonella vaccine • Other routine childhood vaccines such as measles, mumps, rubella, polio, hepatitis B, and varicella may sometimes be helpful Francisco A. Bonilla et. al. JACI in practice. 2015
- 56. Assessment of vaccine responses • If antigen-specific antibody levels are low on initial measurement, immunization followed by repeat measurement of specific antibody levels 3 to 6 weeks later (4 weeks is often considered standard) • Evaluation of functional antibody responses to T-independent antigens • Postimmunization specific IgG level • May be used reliably in adults and in children older than 12 months Francisco A. Bonilla et. al. JACI in practice. 2015
- 57. Francisco A. Bonilla et. al. JACI in practice. 2015
- 58. Pneumococcal vaccine Serotype 1 3 4 5 6B 7F 9V 14 18 C 19 F 19 A 23 F 1 2 3 4 5 6B 7F 8 9N 9V 10 A 11 A 12 F 14 15 B 17 F 18 C 19 F 19 A 20 22 F 23 F 33 F 1 4 6B 14 15 B 18 C 23 F 33 F PCV13 PCV23 LAB https://www.merckvaccines.com/products/pneumovax23 https://www.prevnar13.com/ 6A
- 59. Management
- 60. Immunoglobulin replacement therapy • The required IgG dose for an individual patient is unknown • Dose • 0.4 to 0.5 g/kg/month for IVIG, Interval every 3-4 weeks • 0.4 to 0.6 g/kg/month for SCIG • SCIG in adult 100 to 200 mg/kg/week and dosing intervals from daily to twice weekly (Vary dose) • If there is preexisting bronchiectasis, there is evidence for using 0.6 g/kg/month • Higher doses (0.6-0.8 g/kg/month) for patients with enteropathy or splenomegaly Francisco A. Bonilla et. al. JACI in practice. 2015
- 61. Immunoglobulin replacement therapy • It is possible to use SCIG in patients who previously had severe adverse effects with IVIG and in those with high titers of IgG anti-IgA antibodies • Complication • Hepatitis B or hepatitis C, are now extremely rare → check AST, ALT annully • AKI : associated with sucrose-containing products and in patients with preexisting kidney disease • Hemolysis and thromboembolic phenomena Francisco A. Bonilla et. al. JACI in practice. 2015
- 62. Immunization • Routine boosters of tetanus or diphtheria toxoids or pneumococcus are probably not necessary for individuals receiving IgG replacement therapy • Therapeutic IgG contains significant amounts of neutralizing antibodies : measles, mumps, rubella, polio, and varicella • Live attenuated polio, may cause disease in patients with CVID if they have not yet been diagnosed or if IgG therapy has not been initiated Francisco A. Bonilla et. al. JACI in practice. 2015
- 64. Treatment of complications • Rhinosinusitis • Adequate replacement immunoglobulin therapy • Adequate antibiotics and/or surgery • antibiotic prophylaxis CRS, AOM : no controlled trials, expert opinion • Bronchiectasis • Baseline chest CT and lung function tests are essential • Physiotherapy and sometimes prophylactic antibiotics : Azithomycin • 7% hypertonic saline in conjunction with pulmonary hygiene has been found to be useful Francisco A. Bonilla et. al. JACI in practice. 2015
- 65. Treatment of complications • Unusual infections (Ureaplasma or Mycoplasma infections) • Macrolide antibiotic to which the organism is sensitive • High-dose IVIG with measurable titer antibody to the infecting serotype may be helpful • Granulomatous disease • Corticosteroids, in low doses for long periods • Steroid sparing drugs: azathioprine, cyclosporine, Infliximab Francisco A. Bonilla et. al. JACI in practice. 2015
- 66. Treatment of complications • Enteropathy • Biopsies of the intestinal mucosa for diagnosis • CVID is not responsive to gluten withdrawal • azathioprine or 6-mercaptopurine, can be used safely • Infliximab : severe enteropathy • Interstitial lung disease → High mortality • All patients should have at least 1 high-resolution CT scan at diagnosis • at least annually with spirometry Francisco A. Bonilla et. al. JACI in practice. 2015
- 67. HSCT • HSCT have not been considered to have an important role in the treatment of CVID • Significant procedure-related mortality in those receiving HSCT • The indication for HSCT • Hematologic malignancy → Survivial rate 83% • Other conditions : refractory to conventional therapies: autoimmune cytopenias, respiratory or gastrointestinal infections, interstitial/granulomatous lung → Survival rate 33 % Francisco A. Bonilla et. al. JACI in practice. 2015
- 68. • Objective: • We sought to define the outcomes of HSCT for patients with CVID • Methods: • Retrospective data were collected from 14 centers worldwide on patients with CVID receiving HSCT between 1993 and 2012 Claudia Wehr et. al. JACI. 2015
- 69. Claudia Wehr et. al. JACI. 2015
- 70. Claudia Wehr et. al. JACI. 2015
- 71. Summary Claudia Wehr et. al. JACI. 2015 • HSCT in patients with CVID might improve PID-related complications and cure hypogammaglobulinemia • but is associated with high mortality and high GvHD incidence. • Cure of this chronic disease is possible, but patient selection and transplant refinement are critical.
- 73. Children • The main goal of treatment: decrease the morbidity and mortality associated with recurrent infections • Higher doses of IgG replacement therapy (800 mg/kg IVIG every 4 weeks) result in fewer infections • Complications in children are common • Recurrent infection effect growth • Bronchial hyperreactivity Francisco A. Bonilla et. al. JACI in practice. 2015
- 74. Pregnancy • Plasma dilution in the third trimester of pregnancy results in a modest reduction in serum IgG trough levels • It is advisable to increase the replacement IgG dose during this time and for delivery Francisco A. Bonilla et. al. JACI in practice. 2015
