Cervicitis.pptx
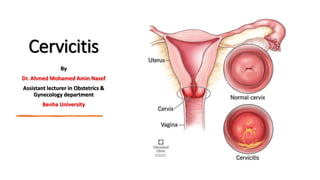
- 1. Cervicitis By Dr. Ahmed Mohamed Amin Nasef Assistant lecturer in Obstetrics & Gynecology department Benha University
- 2. Definition An inflammatory process in the cervical epithelium and stroma can be associated with trauma, inflammatory systemic disease, neoplasia and infection There are 2 types: Ectocervicitis HSV or result from severe vaginitis by T vaginalis or candida albicans Endocervicitis (mucopurulent cervicitis) Nonspecific organism as staph, strept, E-coli ….. Specific infection C. trachomatis, N. gonorrhea, mycoplasma genitalie
- 4. Definition • Clinically Gross visualization of yellow purulent material on a white cotton swab • Histologically Presence of 10 or more PMN leukocytes per HPF on gram- stained smears obtained from ectocervix
- 5. Clinical presentation • Asymptomatic in about 60% • Postcoital bleeding • Purulent or mucopurulent vaginal discharge • Hypertrophied edematous cervix • Dyspareunia, dysuria, deep pelvic pain, backache • Perinatal infections of membranes, AF and neonatal infections • The physical sign of cervical infection grossly appearance of yellow mucopurulent material on a white cotton swab
- 7. Investigations WET MOUNT GRAM STAIN PRESENCE OF 10 OR MORE PMN LEUKOCYTES PER HPF ON GRAM-STAINED SMEARS OBTAINED FROM ENDOCERVIX CULTURE & SENSITIVITY NAAT TEST DIRECT PROBE ANALYSIS
- 9. Microbiology • Gram negative coccobacilli • Invade columnar & transitional epithelial cells to be intracellular so squamous vaginal epithelium didn’t be affected
- 10. Transmission Sexual contact Nonsexual from mother to neonate during childbirth (ophthalmia neonatorum) Infection of: 1ry sites urethra, skene's gland, Bartholin gland, endocervix, rectum, pharynx, conjunctiva Spread PID, perihepatitis (Fitz-Hugh-Curtis syndrome) Systemic spread arthritis, endocarditis, meningitis, septicemia
- 11. Clinical presentation • Asymptomatic • Postcoital bleeding • Purulent or mucopurulent vaginal discharge • Dysuria, dyspareunia • Bartholin abscess • During pregnancy Perinatal transmission, PPROM, PTL, chorioamnionitis, Newborn ophthalmia neonatorum, pneumonia, otitis media Male urethritis, epididymitis, prostatitis, proctitis
- 12. Detection • Endocervical smear • Gram stain Gram negative coccobacilli • Culture On chocolate agar or Thayer martin agar • NAAT Gold standard for diagnosis
- 14. Treatment • Abstinence until therapy is completed • Investigate for other STDs • Treat patient & sexual partner • Drugs used for treatment Ceftriaxone 250 mg IM + Azithromycin 500 mg 1gm single dose Or Cefixime (Suprax) 400 mg orally once + Azithromycin 500 mg 1gm single dose
- 16. Microbiology Immotile Didn’t stain with gram (resist gram staining) replicate only within a host cell Present in 2 forms Elementary bodies (spore like & infectious) Reticulate bodies (replicative stage % only within host cells)
- 17. Classification Types A,B,C causes trachoma Types from D to K infect genital tract, non gonococcal urethritis, cervicitis, salpingitis, PID Types L1,L2,L3 infection of lymph nodes near genitals (LGV) lymphogranuloma venereum
- 18. Transmission • Sexual contact • Nonsexual from mother to neonate during childbirth (ophthalmia neonatorum, pneumonia It is the most common sexually transmitted bacteria The most common infectious cause of blindness
- 19. Clinical presentation • Asymptomatic • Postcoital bleeding • Purulent or mucopurulent vaginal discharge • Dysuria, dyspareunia • Bartholin abscess • During pregnancy Perinatal transmission, PPROM, PTL, chorioamnionitis, Newborn ophthalmia neonatorum, pneumonia, otitis media Male urethritis, epididymitis, prostatitis, proctitis
- 20. Investigations • Microscopic inspection Reveals 20 or more leukocytes per HPF • Gram stain Resist stain with gram stain • Culture Not cultured except on tissue culture • Molecular testing NAAT • Enzyme linked immunosorbent assay (ELISA)
- 21. Treatment • Abstinence until therapy is completed • Investigate for other STDs • Treat patient & sexual partner • Drugs used for treatment Doxycycline 100 mg orally 2 times per day for 7 days Or Azithromycin 500 mg 1gm single dose
- 23. Definition Chronic condition in which cervical glands act as a reservoir for pyogenic organisms and associated with macroscopic changes in cervical architecture, shape or secretions
- 24. Etiology Sequalae of acute cervicitis Chronic nonspecific cervicitis Chronic specific cervicitis
- 25. Pathological types of chronic cervicitis Chronic endocervicitis (chronic mucopurulent discharge) Mucus polyps (hyperplasia of cervical epithelium) Nabothian follicles (multiple cysts due to obstruction of Nabothian glands) Hypertrophic cervicitis (hyperplasia of cervical stroma) Atrophic cervicitis (wooden small cervix) Cervical ulcer (true ulceration) Cervical ectopy (eversion of ectocervix following bilateral cervical tears
- 26. Nabothian cysts
- 27. Cervical erosion
- 28. Cervical polyp
- 29. Microscopically • Infiltration by lymphocytes and macrophages
- 30. Clinical presentation • Asymptomatic • Contact bleeding • Infertility (cervical cause) • Mucopurulent vaginal discharge • Cervical hypertrophy • Pain, dyspareunia, deep pelvic pain • Pregnancy complications PPROM, chorioamnionitis • By examination pathological form seen
- 31. Investigations No pathogen detected Pap smear (suspicious cervix) Ultrasound finding Polyp, cysts, barrel shaped cervix, hypertrophy
- 32. Treatment • Prophylaxis Early proper treatment of acute cervicitis • Medical Antiseptics Hygiene Antibiotics are not effective (as no pathogen) • Drainage of pus Electrocautery Cryotherapy Laser
- 33. Cervical ectopy Presence of endocervical epithelium in the ectocervix Etiology Chronic cervicitis Congenital Hormonal effect (COC users, pregnancy, lactation) Presentation Asymptomatic Mucopurulent discharge Contact bleeding Examination Simple (red flat), papillary (velvet like), follicular Investigations Pap smear, culture and sensitivity Treatment Follow up and no treatment is required or treat as chronic cervicitis if present as chronic cervicitis
- 34. Cervical ectopy Presence of endocervical epithelium in the ectocervix
