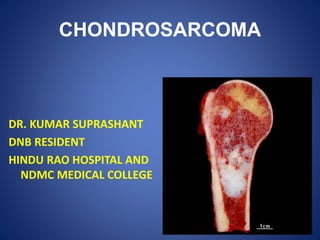
Chondrosarcoma
- 1. CHONDROSARCOMA DR. KUMAR SUPRASHANT DNB RESIDENT HINDU RAO HOSPITAL AND NDMC MEDICAL COLLEGE
- 2. CHONDROSARCOMA OVERVIEW 1.Defination 2.Frequency 3.Types Defination c/f Frequency radiology Epidemiology histology Etiology 4.Treatment
- 3. CHONDROSARCOMA DEFINATION Malignant tumour of cartilage producing cells
- 4. CHONDROSARCOMA FREQUENCY 9% of primary malignancies of bone 3rd most common primary malignancy of bone after multiple myeloma and osteosarcoma 2nd most common non hematological primary malignancy of bone
- 5. CHONDROSARCOMA TYPES • Primary chondrosarcoma • Secondary chondrosarcoma • Periosteal chondrosarcoma • Dedifferentiated chonrosarcoma • Clear cell chondrosarcoma • Mesnchymal chondrosarcoma
- 6. Primary chondrosarcoma • Malignant cartilage tumour arising in previously normal bone • a/k/a central or conventional chondrosarcoma • 90% of all chondrosarcoma • Age group- 40 to 60 yrs • Male: female = 3:2
- 7. • Sites –Pelvis most common site(ilium mc bone) –Proximal femur –Proximal humerus –Ribs (although rarely occour in hand but mc primary malignancy of bone in hand)
- 8. Clinical feature • Pain • Palpable mass • Asymptomatic incidental finding • Pathological fracture( in high grade chondrosarcoma)
- 9. Radiographic findings • Frequently diagnostic • Arising in medullary cavity with irregular matrix calcification- punctate , popcorn, comma shaped calcification( rings and arcs appearance) • Bone destruction, cortical erosions, periosteal reaction, soft tissue mass
- 10. Chondrosarcoma from iliac bone with soft tissue extention
- 11. Axial CT image showing mass arising from iliac bone with chondroid calcification which suggest chondrosarcoma
- 13. RING AND ARC CALCIFICATION
- 15. Differenciating encondroma from chondrosrcoma Enchondroma and low grade chondrosarcoma may appear radiologically similar Similarity- both located in metaphysis with stippled calcification and endosteal scalloping Histology– similar in enchondroma and low grade chondrosarcoma
- 16. Difference – Endosteal scalloping of more than 2/3rd of cortical thicness- chondrosarcoma Aggressive changes such as cortical erosion , bone destruction, periosteal reaction, soft tissue mass- chondrosarcoma size> 5 cm in axial skeleton- predictor of malignancy Apperance of lysis in previously calcified area- malignancy
- 17. Site- aggressive lesion in hand still considered benign whereas same amount of aggressive behaviour in pelvis or proximal femur is dignostic of chondrosarcoma
- 19. CT scan • Differentiate benign from malignant lesion • For characterizatiion of lesion in anatomically complex areas- sacrum, pelvis
- 20. MRI • Depict high water content of lesion with lobulation at margins • Best to see intramedullary extent • Cotical erosion, bone destruction, reactionary edema, soft tissue extention are well depicted
- 21. Intramedullary extention & soft tissue extention
- 22. Bone scan Radionucleotide uptake has been graded GRADE 1- uptake less than ASIS GRADE 2- uptake same as ASIS GRADE 3- uptake more than ASIS Grade 3 uptake is consistent with chondrosarcoma than enchondroma
- 23. PET scan • Standard uptake value (suv) may be helpful in diffrentiating benign from malignant catrilaginous lesion
- 24. Histology Composed of malignant cells with abundant cartilaginous matrix, cartilage permeates the host bony trabeculae Histologically three grades Grade 1- less cellular and less nuclear atypia (vis-à-vis enchondroma) Grade 2 - ↑ cellularity and nuclear atypia Grade 3- ↑ ↑ cellularity and pleomorphic anaplastic cells
- 25. Factors which favour malignancy Hypercellularity, plump nuclei, binucleate cells, permeative pattern, entrapment of bony trabeculae Overall anatomical location, clinical behavior, radiologic finding must be considered along with histology to diffrentiate enchondroma from low grade chondrosarcoma
- 26. Intramedullary ,soft tiisue extention of tumour with calcification
- 30. SECONDARY CHONDROSARCOMA Arise at the site of preexisting benign cartilage lesion • Ollier disease(multiple enchondroma) • Maffucci disease( multiple enchodroma+ soft tissue hemagioma) • Solitary osteochondroma(1%) • Multiple heriditary exostosis(5%) • Synovial chondromatosis • Chondromyxoid fibroma
- 31. • Periosteal chondroma • Chondroblastoma • Fibrous dysplasia • Previous irradiation Chondrosarcoma developing on the surface of bone as a result of malignant transformation of cartilage cap of preexisting osteochondroma is k/a peripheral chondrosarcoma
- 32. Age- 25- 45 yrs( earlier than primary chondrosarcoma) Site- pelvis & shoulder girdle mc affected C/F Change in clinical symptom of a patient with precursor lesion Sudden onset of pain Increase in size of swelling
- 33. Radiology Osteochondroma- irregular mineralization, increased thickness of cartilage cap( size of cap > 2 cm in skeletally mature patient on CT/MRI) Enchondroma- destructive permeation of bone and development of soft tissue mass
- 34. Periosteal chondrosarcoma a/k/a juxtacortical chondrosarcoma Arise from outer surface of bone possibly of periostel origin
- 36. Dedifferentiated chondrosarcoma High grade sarcoma(osteosarcoma, fibrosarcoma, malignant fibrous histiocytoma) adjacent to a low grade chondrosarcoma Radiological- aggressive radiolucent area juxtaposed to typical chondrosarcoma
- 37. Low grade chondrosarcma High grade spindle cells
- 38. Clear cell chondrosarcoma • Round cells with abundant clear cytoplasm and distinct cytoplasmic border with abundant background of cartilaginous matrix • Multinucleate giant cells are apparent • Strong tendency to arise in epiphysis • May have benign radiological feature and confused with chondroblastoma or GCT
- 39. Epiphyseal Gaint Cell Tumor Chondroblastoma Clear cell chondrosarcoma
- 40. Mesenchymal chondrosarcoma • High grade • Small round blue cells with islands of benign appearing cartilage • Hemangiopericytomatous growth with staghorn like vessels • Aggressive radiographic findings
- 42. Treatment Summary Chondrosarcomas represent a diverse spectrum of diseases. They are tumors that should be treated with definitive and complete surgical resection if local control is to be achieved. Although grade 1 lesions in the extremity can be managed with curettage, incomplete surgical resection of intermediate and high- grade lesions puts the patient at risk for local failure, metastases, and eventual death.
- 43. Low grade chondrosarcoma • controversial treatment • Extended curettage with use of intraoperative adjuvant- only for low grade chondrosarcoma confined to medullary canal. • With soft tissue extention- treated similar to high grade
- 44. High grade chondrosarcoma • Wide or radical resection or amputation • Primary wide resection without a biopsy(to avoid chance of tumour contamination) is indicated for any lesion in pelvis or expendable location. Local recurrence rate after tumour contamination is high After wide resection recurrence is < 10%
- 45. Chemotherapy • No role • Currently evaluated for treatment of mesenchymal and dediffrentiated chondrosarcoma Radiotherapy • Limited role • For palliative purpose Proton beam therapy(recent advance) Used for skull base chondrosarcoma
- 46. Metastasis • Most local recurrence & pulmonary metastasis occour within 1st 5 years of initial presentation • Compared to other sarcomas chondrosarcoma has high prevalance of local recurrence or metastasis after 5 years hence survival of patient be determined at 10 years rather than 5 years • Pulmonary metastasis- wide surgical resection
- 47. • Prognosis mostly depends on size, grade & location of tumour • More size – poor prognosis • Higher grade- poor prognosis • Pelvic lesion- poor prognosis
- 48. • Low grade chondrosarcoma- 10 year survival rate> 90% • High grade chondrosarcoma- 10 year survival rate 20-40% • Recurrence generally have higher grade than primary malignancy bcoz slow growing tumour and recurrence or mets cant be detected years after primary procedure Long term follow up with regular imaging of operative site and chest
- 49. Work up for a case of chondrosarcoma • Diagnosis often on clinical & radiological findings • Biopsy- controversial role • Laboraty investigations- nonspecific • Staging- CT chest • Treatment based on combined clinical, radiological , histological grade findings
- 50. Biopsy • Performed only to confirm what in clinically and radiologically obvious • Decision taken by an experienced orthopaedic oncologist • Closed or open • Closed- taken from area of uncalcified matrix disadvantage- chondrosarcoma highly heterogeneous( high grade can have areas of low grade)
- 51. Open biopsy – sometimes advocated to minimise potential sampling error Pelvic lesion – biopsy is generally not recommended
- 52. Extended curettage Simple curettage+ use of adjuvants Adjuvants-phenol, nitrogen,polymethyl methacrylate,argon beam coagulator • Cortical window-larger than lesion • Tumour scooped out • Cavity enlarged in each direction with burr hole • Copious irrigation of cavity • Use of adjuvant • Filling cavity-autogenous bone graft, allograft, artificial bone graft substitute,demineralized bone matrix, bone cement
- 54. Wide/negative margins are the goal of surgical resection
- 55. Limb salvage vs amputation Every patient with tumor of the extremity should be considered for limb salvage if the tumor can be removed with an adequate margin and the resulting limb is worth saving. No justification for limiting the limb salvage process based only on the prognosis
- 56. contraindication Neurovascular involvement Large size tumour Displaced pathologic fracture(relative contraindication) Fungating and infected tumors Recurrence of malignant tumors Skeletal immaturity Pulmonary metastasis is not a contraindication of surgery Contraindications of limb salvage are the indications for amputation
- 57. RESECTION & RECONSTRUCTION Resection-Wide margin Reconstruction Arthrodesis Mobile joint reconstruction • Osteoatricular allograft reconstruction • Endoprosthetic reconstruction • Allograft prosthesis composite reconstruction • Rotationplasty • Autoclaved bone tumour
- 58. Arthrodesis • Bone allografts, Vascularised autografts or both. • Provides a stable, durable reconstruction which requires limited postoperative follow-up • Inherent disadvantages: - Loss of joint function - Increased energy expenditure - Additional abnormal mechanical stress to other joints
- 63. Osteoarticular allografts • Adv: – Ability to replace ligaments, tendons & intraarticular structures. – As a temporary measure to preserve adjacent physis till skeletal maturity e.g. Prox tibia • Disadv: – nonunion at graft host jxn. – fatigue #, articular collapse, dislocation, degenerative jt. dis. & failure of ligament & tendon attachments.
- 65. Endoprosthetic Reconstruction • Adv: –Predictable immediate stability –Quicker rehab –Increased durability – better implants. –Incremental limb lengthening • Disadv: –Long term compl. if pt. is cured of disease. –polyetheylene wear – inserts replaced. –Fatigue # at base of stem – difficult to remove
- 67. Allograft prosthesis composite reconstruction
- 69. Amputation Specific technical difficulty for resection as well as reconstruction of pelvic chondrosarcoma • Interilio-abdominal disarticulations • Conservative surgeries
- 70. Pelvic resection • I- iliac • II-periacetabular • III-obturator • IV-sacral
- 71. • Eg- acetabulum+ iliac wing ka I,II pelvic resection • H- added as suffix if femoral head is resected
- 72. • Type I- no recontruction required ,limb length discrepancy(1-2 cm) adjusted with shoe raise • Type II- reconstruction with iliofemoral, ischiofemoral arthrodesis or prosthesis • Type III- no reconstruction required (pubis does not bear weight)
- 73. Type II resection reconstructed with saddle prosthesis
- 74. Thank you