Immediate loading
•Download as PPT, PDF•
66 likes•19,505 views
immediate loading applications in implant dentistry
Report
Share
Report
Share
Recommended
Recommended
This journal club deals with different loading protocols and comparative analysis among them. this basically deals with immediate and delayed loading protocols.Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...

Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...Partha Sarathi Adhya
More Related Content
What's hot
This journal club deals with different loading protocols and comparative analysis among them. this basically deals with immediate and delayed loading protocols.Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...

Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...Partha Sarathi Adhya
What's hot (20)
Sinus lift with dental implants Placement.(with Clinical Photographs) Dr. ...

Sinus lift with dental implants Placement.(with Clinical Photographs) Dr. ...
Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...

Implant Loading Protocols Journal Club-Comparative evaluation of the influenc...
Implant failure , complications and treatment, management- Partha Sarathi Adhya

Implant failure , complications and treatment, management- Partha Sarathi Adhya
Implant treatment plan for completely edentulous patient

Implant treatment plan for completely edentulous patient
Occulasl consideration for implant supported prostehsi/dental courses

Occulasl consideration for implant supported prostehsi/dental courses
Advanced soft tissue & hard tissue grafting Clinical Training

Advanced soft tissue & hard tissue grafting Clinical Training
Similar to Immediate loading
Description :
The Indian Dental Academy is the Leader in continuing dental education , training dentists in all aspects of dentistry and
offering a wide range of dental certified courses in different formats.for more details please visit
www.indiandentalacademy.com
loading of dental implants/certified fixed orthodontic courses by Indian dent...

loading of dental implants/certified fixed orthodontic courses by Indian dent...Indian dental academy
The Indian Dental Academy is the Leader in continuing dental education , training dentists in all aspects of dentistry and offering a wide range of dental certified courses in different formats.
Indian dental academy provides dental crown & Bridge,rotary endodontics,fixed orthodontics,
Dental implants courses.for details pls visit www.indiandentalacademy.com ,or call
0091-9248678078
Copy of osseointegration/certified fixed orthodontic courses by Indian dental...

Copy of osseointegration/certified fixed orthodontic courses by Indian dental...Indian dental academy
Indian Dental Academy: will be one of the most relevant and exciting training center with best faculty and flexible training programs for dental professionals who wish to advance in their dental practice,Offers certified courses in Dental implants,Orthodontics,Endodontics,Cosmetic Dentistry, Prosthetic Dentistry, Periodontics and General Dentistry.
Dental implant osseointegration/dental implant courses by Indian dental academy

Dental implant osseointegration/dental implant courses by Indian dental academyIndian dental academy
Similar to Immediate loading (20)
loading of dental implants / academy of fixed orthodontics

loading of dental implants / academy of fixed orthodontics
loading of dental implants/certified fixed orthodontic courses by Indian dent...

loading of dental implants/certified fixed orthodontic courses by Indian dent...
IMMEDIATE IMPLANT PLACEMENT WITH ONE YEAR FOLLOW-UP: A CASE REPORT

IMMEDIATE IMPLANT PLACEMENT WITH ONE YEAR FOLLOW-UP: A CASE REPORT
Stman et-al-2012-clinical_implant_dentistry_and_related_research

Stman et-al-2012-clinical_implant_dentistry_and_related_research
Parameters for a Success Implant Integration Revisited Part I by Oded Bahat

Parameters for a Success Implant Integration Revisited Part I by Oded Bahat
simplified drilling technique does not decrease dental implant osseointegration

simplified drilling technique does not decrease dental implant osseointegration
Copy of osseointegration/certified fixed orthodontic courses by Indian dental...

Copy of osseointegration/certified fixed orthodontic courses by Indian dental...
Dental implant osseointegration/dental implant courses by Indian dental academy

Dental implant osseointegration/dental implant courses by Indian dental academy
IMMEDIATE IMPLANT PLACEMENT WITH ONE YEAR FOLLOW-UP: A CASE REPORT

IMMEDIATE IMPLANT PLACEMENT WITH ONE YEAR FOLLOW-UP: A CASE REPORT
More from Mohammed Alshehri
More from Mohammed Alshehri (20)
How to apply for post graduate studies in dentistry

How to apply for post graduate studies in dentistry
How to apply for post graduate studies in dentistry

How to apply for post graduate studies in dentistry
How to apply for post graduate studies in dentistry

How to apply for post graduate studies in dentistry
Recently uploaded
Recently uploaded (20)
Basic Civil Engineering first year Notes- Chapter 4 Building.pptx

Basic Civil Engineering first year Notes- Chapter 4 Building.pptx
This PowerPoint helps students to consider the concept of infinity.

This PowerPoint helps students to consider the concept of infinity.
Salient Features of India constitution especially power and functions

Salient Features of India constitution especially power and functions
Micro-Scholarship, What it is, How can it help me.pdf

Micro-Scholarship, What it is, How can it help me.pdf
Python Notes for mca i year students osmania university.docx

Python Notes for mca i year students osmania university.docx
UGC NET Paper 1 Mathematical Reasoning & Aptitude.pdf

UGC NET Paper 1 Mathematical Reasoning & Aptitude.pdf
Fostering Friendships - Enhancing Social Bonds in the Classroom

Fostering Friendships - Enhancing Social Bonds in the Classroom
Unit 3 Emotional Intelligence and Spiritual Intelligence.pdf

Unit 3 Emotional Intelligence and Spiritual Intelligence.pdf
HMCS Vancouver Pre-Deployment Brief - May 2024 (Web Version).pptx

HMCS Vancouver Pre-Deployment Brief - May 2024 (Web Version).pptx
Immediate loading
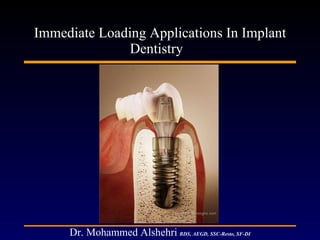
- 1. Immediate Loading Applications In Implant Dentistry Dr. Mohammed Alshehri BDS, AEGD, SSC-Resto, SF-DI
- 8. Introduction
