Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement
The Health Innovation Network Polypharmacy Programme is working with healthcare professionals to address problematic polypharmacy by supporting easier identification of patients at potential risk from harm from multiple medications. Our evidence-based polypharmacy Action Learning Sets (ALS) are being rolled out across England to support GPs, pharmacists and other healthcare professionals who undertake prescribing or medication reviews to understand the complex issues around stopping inappropriate medicines safely. To drive and accelerate changes in practice, delegates complete a quality improvement project to address problematic polypharmacy in their workplace. This poster summary, Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement, can be viewed here. For more information about the polypharmacy programme, please visit https://thehealthinnovationnetwork.co.uk/programmes/medicines/polypharmacy/
Recommended
Recommended
More Related Content
Similar to Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement
Similar to Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement (20)
More from Health Innovation Wessex
More from Health Innovation Wessex (20)
Recently uploaded
Recently uploaded (20)
Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement
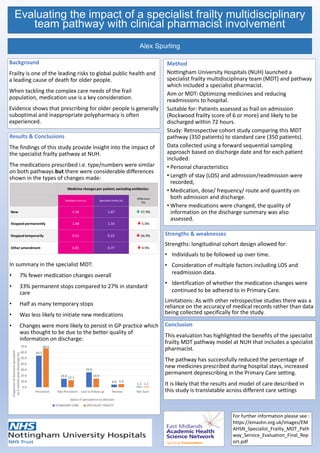
- 1. Evaluating the impact of a specialist frailty multidisciplinary team pathway with clinical pharmacist involvement Alex Spurling Background Frailty is one of the leading risks to global public health and a leading cause of death for older people. When tackling the complex care needs of the frail population, medication use is a key consideration. Evidence shows that prescribing for older people is generally suboptimal and inappropriate polypharmacy is often experienced. Method Nottingham University Hospitals (NUH) launched a specialist frailty multidisciplinary team (MDT) and pathway which included a specialist pharmacist. Aim or MDT: Optimizing medicines and reducing readmissions to hospital. Suitable for: Patients assessed as frail on admission (Rockwood frailty score of 6 or more) and likely to be discharged within 72 hours. Study: Retrospective cohort study comparing this MDT pathway (350 patients) to standard care (350 patients). Data collected using a forward sequential sampling approach based on discharge date and for each patient included: • Personal characteristics • Length of stay (LOS) and admission/readmission were recorded, • Medication, dose/ frequency/ route and quantity on both admission and discharge. • Where medications were changed, the quality of information on the discharge summary was also assessed. Strengths & weaknesses Strengths: longitudinal cohort design allowed for: • Individuals to be followed up over time. • Consideration of multiple factors including LOS and readmission data. • Identification of whether the medication changes were continued to be adhered to in Primary Care. Limitations: As with other retrospective studies there was a reliance on the accuracy of medical records rather than data being collected specifically for the study. Conclusion This evaluation has highlighted the benefits of the specialist frailty MDT pathway model at NUH that includes a specialist pharmacist. The pathway has successfully reduced the percentage of new medicines prescribed during hospital stays, increased permanent deprescribing in the Primary Care setting. It is likely that the results and model of care described in this study is translatable across different care settings Results & Conclusions The findings of this study provide insight into the impact of the specialist frailty pathway at NUH. The medications prescribed i.e. type/numbers were similar on both pathways but there were considerable differences shown in the types of changes made: In summary in the specialist MDT: • 7% fewer medication changes overall • 33% permanent stops compared to 27% in standard care • Half as many temporary stops • Was less likely to initiate new medications • Changes were more likely to persist in GP practice which was thought to be due to the better quality of information on discharge: 54.2 14.6 25.6 4.6 1.1 66.6 12.1 14.9 5.3 1.1 0.0 10.0 20.0 30.0 40.0 50.0 60.0 70.0 Persistent Not Persistent Lost to follow up Review Not Sure Proportion of decisions persistent at 3 months post discharge (%) status of persistence to decision STANDARD CARE SPECIALIST FRAILTY For further information please see : https://emashn.org.uk/images/EM AHSN_Specialist_Frailty_MDT_Path way_Service_Evaluation_Final_Rep ort.pdf
