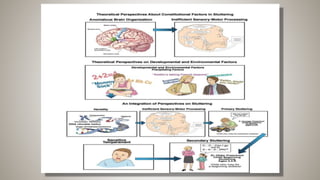
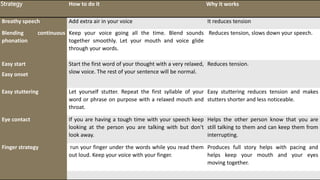
The document provides an extensive overview of stuttering, covering its types, causes, prevalence, classification, and treatment approaches. It discusses developmental and environmental factors contributing to stuttering, as well as assessment and management strategies. Theories regarding the etiology of stuttering and practical therapeutic techniques are also addressed in detail.