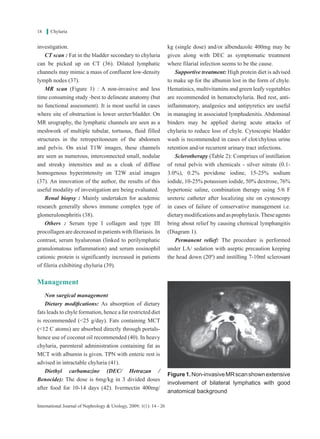
The document provides an overview of chyluria, which is the passage of milky white urine due to the presence of chyle. It discusses the history and theories around the causes of chyluria. It is most commonly caused by parasitic infections like Wuchereria bancrofti but can also have non-parasitic causes. The clinical features, grading, investigations and management options for chyluria are described in detail. Recent diagnostic techniques like MR scan and treatment advances including robotics are also reviewed.






![23
The prognosis of non-parasitic chyluria is usually
very good and the treatment is mostly conservative
(19). A long-term remission rate of 62% in the
conservatively managed group (DEC + fat restricted
diet), and a cure rate of 90% of patients in the operated
group has been reported. Postoperative recurrence rate
was 10%. There was more weight gain and dietary
freedom along with a longer chyluria free period
in the operated group relative to the conservatively
managed group (27).
Though pure dextrose treatment has been
discontinued due to poor success, povidone iodine
0.2% has been found to be as effective as 1% silver
nitrate [82% (silver nitrate) and 83% (povidone;
P=1.0)] (45). Definitive surgical ablation of lymphatic
urinary fistula is better than conservative medical
management because it has a higher success rate,
more dietary freedom and better patient acceptability
(27). Over 95% success rate has been described
with a follow up of 1 to 9 years following a single
microsurgical operation (54).
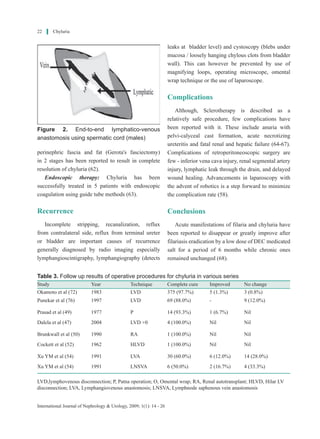
Reno-lymphatic disconnection is the reference
procedure, with long-term success rates of 99% (69).
The follow up results of various series are depicted
(Table 3).
References
1. Hemal AK, Gupta NP. Retroperitoneoscopic
lymphatic management of intractable chyluria. J
Urol. 2002 Jun;167(6):2473-6.
2. Hemal AK, Kumar M, Wadhwa SN.
Retroperitoneoscopic nephrolympholysis and
ureterolysis for management of intractable filarial
chyluria. J Endourol. 1999 Sep;13(7):507-11.
3. HemalAK, RS KMP, Gupta NP. The laparoscopic
management of chyluria by retroperitoneal access.
BJU Int. 2000;86(3):402.
4. Kumar M, Kumar R, Hemal AK, Gupta NP.
Complications of retroperitoneoscopic surgery at
one centre. BJU Int. 2001 May;87(7):607-12.
5. Prout W. On the nature and treatment of stomach
and urinary diseases. third ed: Churchill, London
120; 1841.
6. Maget A. Renal chyluria. Br J Urol.
1967;39:555.
7. Choi JK, Wiedemer HS. Chyluria:
Lymphangiographic study and review of
literature. J Urol. 1964 Dec;92:723-7.
8. Lazarus JA, Marks MS. Non-parasitic chyluria
with special reference to traumatic chyluria. J
Urol. 1946;56:246.
9. MansonBahr PH. Tropical diseases sixteen ed.
London Balliere Tindall and Cassel; 1954.
10. Sen SB, Ellappan S. Chylous manifestations
of filariasis: a clinical and lymphographic
study: Part I: Filarial chyluria. Ind J Med Res.
1968;56(10):1535 - 45.
11. Aye UT, Aung STT. Chyluria. Clin Rad.
1975;26:237.
12. Ngan H, Leong CH. A lymphographic study of
chyluria. Br J Radiol. 1977 Dec;50(600):863-70.
13. Gluck Z, Ruegger S, Sulser T. A rare cause of
nephrotic syndrome in a young woman with flank
pain, milky urine and leukocyturia. Ther Umsch.
2002 Mar;59(3):144-7.
14. Gupta NP. Retroperitoneoscopic management of
intractable chyluria. Indian Journal of Urology
2005;21(1):63-5.
15. Lin TP, Hsu YS, Chen KK, Lin AT, Chang YH,
Wu HH, et al. Chyluria--experience of Taipei
Veterans General Hospital. J Chin Med Assoc.
2003 Feb;66(2):109-12.
16. Peng HW, Chou CF, Shiao MS, Lin E, Zheng
HJ, Chen CC, et al. Urine lipids in patients with
a history of filariasis. Urol Res. 1997;25(3):217-
21.
17. Muguruma K, Matsuda T, Koyama Y, Komatz Y.
Chyluria treated with inguinal lymphangiovenous
and lymph node-venous anastomosis: a case
report. Nippon Hinyokika Gakkai Zasshi. 1994
Oct;85(10):1571-4.
18. Cao W, Van der Ploeg CP, Ren Z, Habbema JD.
Success against lymphatic filariasis. World Health
Forum. 1997;18(1):17-20.
19. Stalens JP, Falk M, Howmann-Giles R, Roy
Ashok Kumar Hemal et al
International Journal of Nephrology & Urology, 2009; 1(1): 14 - 26](https://image.slidesharecdn.com/chyluria-anoverview-190529154505/85/Chyluria-an_overview-10-320.jpg)
![24
LP. «Milky» urine--a child with chyluria. Eur J
Pediatr. 1992 Jan;151(1):61-2.
20. Guillonneau B, Bouchot O, Buzelin F, Dupas B,
Barrier JH, Buzelin JM. Lymphangiomyomatosis:
an exceptional cause of chyluria. Report of a case.
Prog Urol. 1993 Jun;3(3):484-9.
21. Kekre NS,Arun N, DateA. Retroperitoneal cystic
lymphangioma causing intractable chyluria. Br J
Urol. 1998 Feb;81(2):327-8.
22. Lewsuwan S, Kanjanabuch T, Avihingsanon Y,
Praditpornsilpa K, Eiam-Ong S. A rare case of
chylous ascites and chyluria in an adult nephrotic
syndromewithfocalsegmentalglomerulosclerosis.
J Med Assoc Thai. 2006 Aug;89 Suppl 2:S253-6.
23. KanoK,ArisakaO.Chyluriaduetoretroperitoneal
lymphangioma producing nephrotic syndrome. J
Pediatr. 2003 Nov;143(5):685.
24. Nandy PR, Dwivedi US, Vyas N, Prasad M,
Dutta B, Singh PB. Povidone iodine and dextrose
solution combination sclerotherapy in chyluria.
Urology. 2004 Dec;64(6):1107-9; discussion 10.
25. Mehta VK, Lohar H, Banerjee GK, Reddy MV,
HarinathBC.Surgicalfilariasis:immunoscreening
for filarial IgG antibodies using Wuchereria
bancrofti microfilarial excretory-secretory
antigen. J Commun Dis. 1999 Mar;31(1):35-40.
26. Zhang X, Ye ZQ, Chen Z, Chen ZQ, Zhu QG,
Xin M, et al. Comparison of open surgery versus
retroperitoneoscopic approach to chyluria. J Urol.
2003 Mar;169(3):991-3.
27. Tandon V, Singh H, Dwivedi US, Mahmood M,
Singh PB. Filarial chyluria: long-term experience
of a university hospital in India. Int J Urol. 2004
Apr;11(4):193-8; discussion 9.
28. Grunert JH, Hendrickx P, Wagner HH. The
diagnosis of lymphatic vascular dysplasia
and lymphatic fistula formation. Rofo. 1992
Mar;156(3):282-5.
29. Koga S, Nagata Y, Arakaki Y, Matsuoka M,
Ohyama C. Unilateral pedal lymphography in
patients with filarial chyluria. BJU Int. 2000
Feb;85(3):222-3.
30. Koga S, Nagata Y, Arakaki Y, Matsuoka M,
OhyamaC.Lymphangiographyoffilarialchyluria:
injections via right and left feet at different times.
Br J Urol. 1992 Mar;69(3):318.
31. Pui MH, Yueh TC. Lymphoscintigraphy in
chyluria, chyloperitoneum and chylothorax. J
Nucl Med. 1998 Jul;39(7):1292-6.
32. Thet Thet L, Takeda T, Kuramochi M, Sato M,
Wu J, Myo M, et al. Tc-99m diethylenetriamine
pentaacetic acid (DTPA)-human serum albumin
(HSA) radionuclide lymphography for detecting
the location of chyluria. Ann Nucl Med. 1998
Aug;12(4):205-7.
33. Nishiyama Y, Yamamoto Y, Mori Y, Satoh K,
Takashima H, Ohkawa M, et al. Usefulness
of Technetium-99m human serum albumin
lymphoscintigraphy in chyluria. Clin Nucl Med.
1998 Jul;23(7):429-31.
34. Gu XT, Gao ZG, Shen BR, Hu GZ, Tang XL, Ma
Q.[ChangesinT-lymphocytesubsetsofperipheral
blood in patients with filarial chyluria]. Zhongguo
Ji Sheng Chong Xue Yu Ji Sheng Chong Bing Za
Zhi. 2000;18(2):103-5.
35. Xing C, Xing XM, Xing L. Immunological
observation on chyluric patients with heat-
clearing and hemostatic drugs. Zhongguo Zhong
Xi Yi Jie He Za Zhi. 1994 Oct;14(10):601-3.
36. Miller FH, Keppke AL, Yaghmai V, Gabriel
H, Hoff F, Chowdhry A, et al. CT diagnosis of
chyluria after partial nephrectomy. AJR Am J
Roentgenol. 2007 Jan;188(1):W25-8.
37. Govil S, Justus A, Lakshminarayanan R, Nayak
S, Devasia A, Gopalakrishnan G. Retroperitoneal
lymphatics on CT and MR.Abdom Imaging. 2007
Jan-Feb;32(1):53-5.
38. Date A, Shastry JC, Johny KV. Ultrastructural
glomerular changes in filarial chyluria. J Trop
Med Hyg. 1979 Jul;82(7):150-4.
39. Esterre P, Plichart C, Huin-Blondey MO, Nguyen
LN, Hartmann D, Guerret S, et al. Circulating
fibrosis markers, eosinophil cationic protein and
eosinophil protein X in patients with Wuchereria
bancrofti infection: association with clinical
status. Parasite. 2006 Jun;13(2):165-70.
40. Geliebter A, Torbay N, Bracco EF, Hashim SA,
Van Itallie TB. Overfeeding with medium-chain
triglyceride diet results in diminished deposition
of fat. Am J clin Nutr. 1983; 37(1):1-4.
41. Buttiker V, Fanconi S, Burger R. Chylothorax
in children: guidelines for diagnosis and
Chyluria
International Journal of Nephrology & Urology, 2009; 1(1): 14 - 26](https://image.slidesharecdn.com/chyluria-anoverview-190529154505/85/Chyluria-an_overview-11-320.jpg)

