More Related Content
Similar to 10.0000@jamanetwork.com@jamainternalmedicine@article abstract@2774115
Similar to 10.0000@jamanetwork.com@jamainternalmedicine@article abstract@2774115 (20)
10.0000@jamanetwork.com@jamainternalmedicine@article abstract@2774115
- 1. Ventricular Preexcitation in a Patient Found to Have
Wolff-Parkinson-White Pattern
Anjali B. Thakkar, MD, MBA; Melvin Scheinman, MD; Nora Goldschlager, MD
A man in his 30s with a history of methamphetamine and heroin
usepresentedtotheemergencydepartmentcomplainingof30min-
utes of exertional, sharp, left-sided chest pain. He admitted to sub-
stance use on the day of presentation.
Onarrivalattheemergencydepartment,hisbloodpressurewas
152/85 mm Hg; all other vital signs were normal. Cardiac examina-
tion results revealed normal heart sounds and no murmurs or jugu-
lar venous distension. Neurologic and pulmonary examination re-
sultswerenormal.Chestradiographydemonstratedclearlungswith
no abnormalities. A 12-lead electrocardiogram (ECG) was obtained
(Figure, A).
Questions: What abnormalities are seen in this ECG, and how
would you treat this patient’s condition?
Interpretation
The ECG in Figure A shows sinus rhythm with ventricular preexci-
tation, demonstrated by a characteristic slurred upstroke, or delta
wave, seen at the onset of each QRS complex. There is also a short
PR interval, and the duration of the QRS complex is prolonged. The
preexcitation likely originates from a right anteroseptal or anterior
free wall accessory pathway (AP) based on early precordial transi-
tion and the positive vector of the delta wave in the inferior leads.1
Clinical Course
Laboratoryworkupresultsrevealedsubstantiallyelevatedlipaselev-
els;thepatient’schestpainwasconsideredtobeduetoalcohol-induced
pancreatitis.Telemetrymonitoringduringthehospitalcoursedidnot
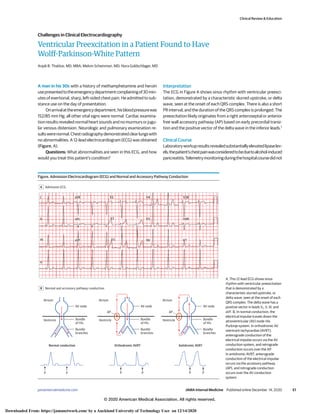
Figure. Admission Electrocardiogram (ECG) and Normal and Accessory Pathway Conduction
Admission ECG
A
aVR V1 V4 V3R
V2
V3
V5
V6
V4R
V7
I
II aVL
III
II
aVF
Normal and accessory pathway conduction
B
Atrium Atrium Atrium
Ventricle Ventricle Ventricle
Bundle
of His
Bundle
of His
AV node AV node
Bundle
branches
Bundle
of His
AV node
Bundle
branches
Bundle
branches
Orthodromic AVRT
Normal conduction Antidromic AVRT
P P
AP AP
P P P P
A, This 12-lead ECG shows sinus
rhythm with ventricular preexcitation
that is demonstrated by a
characteristic slurred upstroke, or
delta wave, seen at the onset of each
QRS complex. The delta wave has a
positive vector in leads V1, II, III, and
aVF. B, In normal conduction, the
electrical impulse travels down the
atrioventricular (AV) node-His
Purkinje system. In orthodromic AV
reentrant tachycardias (AVRT),
anterograde conduction of the
electrical impulse occurs via the AV
conduction system, and retrograde
conduction occurs over the AP.
In antidromic AVRT, anterograde
conduction of the electrical impulse
occurs via the accessory pathway
(AP), and retrograde conduction
occurs over the AV conduction
system.
Clinical Review & Education
Challenges in Clinical Electrocardiography
jamainternalmedicine.com (Reprinted) JAMA Internal Medicine Published online December 14, 2020 E1
© 2020 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by a Auckland University of Technology User on 12/14/2020
- 2. reveal evidence of arrhythmias. The patient left the hospital against
medical advice before additional workup could be performed.
Discussion
Wolff-Parkinson-White (WPW) is an uncommon syndrome result-
ing from myocardial remnant tissue connecting atria and ven-
tricles, allowing for anomalous ventricular activation (preexcita-
tion)fromtheatriumtotheventricle,bypassingtheatrioventricular
(AV) node-His axis. The degree of conduction via the AP can vary
from entirely over the AV node-His-Purkinje system (no preexcita-
tion) to entirely over the AP (maximal preexcitation). Wolff-
Parkinson-White is most commonly diagnosed on routine ECG in
asymptomaticindividualsforwhom3characteristicfeaturesarepre-
sent:aslurredupstroke(deltawave)oftheQRScomplex(whichcan
bepositiveornegative),widenedQRScomplex,andshortPRinter-
val. When the WPW ECG pattern is seen in the absence of sympto-
matic arrhythmias, it is known as WPW pattern; in the presence of
symptomatic arrhythmias, it is known as WPW syndrome.
The prevalence of WPW in multiple community-based popula-
tionstudiesisestimatedtobebetween1to3per1000individuals.2
Autosomal dominant familial forms of WPW syndrome have been
identified; the prevalence is 5.5 in 1000 first-degree relatives of in-
dividuals with WPW.2,3
Electrophysiologicstudieshaveelucidatedthemechanismsun-
derlying symptoms in patients with WPW. Symptomatic arrhyth-
mias are due either to tachycardias that use the AP to initiate and
sustain a reentrant circuit, or tachycardias in which the AP serves
as a bystander route of arrhythmia conduction. Tachycardias that
use the AP as a critical component of the tachycardia circuit are
AV reentrant tachycardias (AVRT); tachycardias in which the AP is
a bystander to other atrial arrhythmias include atrial tachycardia,
AV nodal reentrant tachycardia, and atrial flutter or fibrillation. The
presenceofanterogradeconductionresultsintheclassicdeltawave
finding on ECG; pathways with retrograde-only properties, known
as concealed pathways, will not manifest a delta wave.4
In AVRT, the circuit consists of the normal AV conduction sys-
tem and an AP, both of which link the atria and ventricles (Figure, B).
The electrical impulse can conduct either via the AV conduction sys-
tem or the AP. When anterograde conduction occurs via the AV con-
duction system and retrograde conduction occurs over the AP, the
tachycardia is known as orthodromic AVRT and is associated with
anarrowQRScomplex,orbundlebranchblockmorphologyintheset-
ting of aberrant ventricular conduction. In orthodromic AVRT, the
tachycardia can be initiated with an atrial premature depolarization
thatblocksintheAP,conductsoverthenode,andthenreturnstothe
atrium via the AP. Orthodromic AVRT is the most common arrhyth-
mia observed in WPW syndrome because the AV nodal refractory
period is shorter than that of the AP. In contrast, in up to 8% of
cases, anterograde conduction occurs over the AP with retrograde
nodal conduction, which is associated with a broad QRS because of
maximalpreexcitation;thistachycardiaisknownasantidromicAVRT.5
AsymptomaticindividualswhoarefoundtohaveWPWpattern,as
inthispatient,shouldbeevaluatedfortheriskofsuddencardiacarrest.
While electrophysiologic study is the criterion standard for risk strati-
fication,ECGduringrestandexercisestresscanbehelpful.Whenstress
testresultsshowalossofpreexcitationatlowheartrates,thissuggests
amorebenignpathway.Thisisbecausepreexcitedatrialtachyarrhyth-
mias,likeatrialfibrillation,wouldbeunabletoconductrapidlyenough
viatheaccessorypathwaytoprecipitatelife-threateningarrhythmias.
Ifpreexcitationpersistsduringastresstest,invasiveelectrophysiologic
studyiswarrantedtoidentifythelocationandelectrophysiologicprop-
ertiesoftheAPandtheneedforcatheterablation.
Take-Home Points
• Wolff-Parkinson-Whiteisanuncommonsyndromeresultingfrommyo-
cardialremnanttissueconnectingatriaandventricles,allowingforven-
tricularactivationseparatefromtheAVnode-HisPurkinjesyndrome.
• The WPW pattern is manifest by 3 characteristic ECG features:
a delta wave, widened QRS complex, and short PR interval.
• InpatientswithWPWsyndrome,symptomaticarrhythmiasaredue
either to tachycardias that use the AP as a critical part of the reen-
trant circuit, or tachycardias in which the AP acts as a bystander.
• AsymptomaticindividualsfoundtohaveWPWpatternshouldundergo
riskstratificationwithECGduringrestandexercisestresstoassessfor
lossofpreexcitation;ifpreexcitationpersists,electrophysiologicstudy
iswarrantedtodeterminetheneedforcatheterablation.
ARTICLE INFORMATION
Author Affiliations: Department of Medicine,
University of California, San Francisco,
San Francisco (Thakkar); Division of Cardiology,
Department of Medicine, University of California
San Francisco, San Francisco (Scheinman,
Goldschlager); Division of Cardiology, Department
of Medicine, Zuckerberg San Francisco General
Hospital and Trauma Center, San Francisco,
California (Goldschlager); Section Editor,
JAMA Internal Medicine (Goldschlager).
Corresponding Author: Anjali B. Thakkar, MD,
MBA, Department of Medicine, University of
California, San Francisco, 505 Parnassus Ave,
Room M-1483, San Francisco, CA 94143-0119
(anjali.thakkar@ucsf.edu).
Published Online: December 14, 2020.
doi:10.1001/jamainternmed.2020.6847
Conflict of Interest Disclosures: None reported.
Disclaimer: Dr Goldschlager is a Section Editor of
the Challenges in Electrocardiography section of
JAMA Internal Medicine, but she was not involved in
any of the decisions regarding review of the
manuscript or its acceptance.
REFERENCES
1. Fitzpatrick AP, Gonzales RP, Lesh MD, Modin GW,
Lee RJ, Scheinman MM. New algorithm for the
localization of accessory atrioventricular
connections using a baseline electrocardiogram.
J Am Coll Cardiol. 1994;23(1):107-116. doi:10.1016/
0735-1097(94)90508-8
2. Cohen MI, Triedman JK, Cannon BC, et al;
Pediatric and Congenital Electrophysiology Society
(PACES); Heart Rhythm Society (HRS); American
College of Cardiology Foundation (ACCF); American
Heart Association (AHA); American Academy of
Pediatrics (AAP); Canadian Heart Rhythm Society
(CHRS). PACES/HRS expert consensus statement
on the management of the asymptomatic young
patient with a Wolff-Parkinson-White (WPW,
ventricular preexcitation) electrocardiographic
pattern: developed in partnership between the
Pediatric and Congenital Electrophysiology Society
(PACES) and the Heart Rhythm Society (HRS).
endorsed by the governing bodies of PACES, HRS,
the American College of Cardiology Foundation
(ACCF), the American Heart Association (AHA),
the American Academy of Pediatrics (AAP), and
the Canadian Heart Rhythm Society (CHRS). Heart
Rhythm. 2012;9(6):1006-1024. doi:10.1016/j.
hrthm.2012.03.050
3. Vidaillet HJJ Jr, Pressley JC, Henke E, Harrell FEJ
Jr, German LD. Familial occurrence of accessory
atrioventricular pathways (preexcitation
syndrome). N Engl J Med. 1987;317(2):65-69.
doi:10.1056/NEJM198707093170201
4. Narula OS. Wolff-Parkinson-White syndrome.
a review. Circulation. 1973;47(4):872-887. doi:10.
1161/01.CIR.47.4.872
5. Brembilla-Perrot B, Pauriah M, Sellal J-M, et al.
Incidence and prognostic significance of
spontaneous and inducible antidromic tachycardia.
Europace. 2013;15(6):871-876. doi:10.1093/europace/
eus354
Clinical Review & Education Challenges in Clinical Electrocardiography
E2 JAMA Internal Medicine Published online December 14, 2020 (Reprinted) jamainternalmedicine.com
© 2020 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by a Auckland University of Technology User on 12/14/2020