Dr. Treacy's Dermatology Casebook No 1
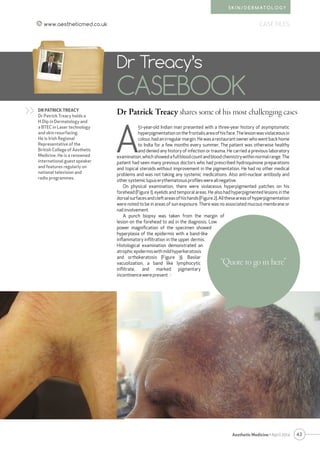
- 1. 43 CASE FILESwww.aestheticmed.co.uk Aesthetic Medicine • April 2014 S K I N / D E R M AT O L O G Y A 51-year-old Indian man presented with a three-year history of asymptomatic hyperpigmentationonthefrontalisareaofhisface.Thelesionwasviolaceousin colour,hadanirregularmargin.Hewasarestaurantownerwhowentbackhome to India for a few months every summer. The patient was otherwise healthy and denied any history of infection or trauma. He carried a previous laboratory examination,whichshowedafullbloodcountandbloodchemistrywithinnormalrange.The patient had seen many previous doctors who had prescribed hydroquinone preparations and topical steroids without improvement in the pigmentation. He had no other medical problems and was not taking any systemic medications. Also anti-nuclear antibody and othersystemiclupuserythematosusprofileswereallnegative. On physical examination, there were violaceous hyperpigmented patches on his forehead (Figure 1), eyelids and temporal areas. He also had hyperpigmented lesions in the dorsalsurfacesandcleftareasofhishands(Figure2).Alltheseareasofhyperpigmentation were noted to be in areas of sun exposure. There was no associated mucous membrane or nailinvolvement. A punch biopsy was taken from the margin of lesion on the forehead to aid in the diagnosis. Low power magnification of the specimen showed hyperplasia of the epidermis with a band-like inflammatory infiltration in the upper dermis. Histological examination demonstrated an atrophicepidermiswithmildhyperkeratosis and orthokeratosis (Figure 3). Basilar vacuolization, a band like lymphocytic infiltrate, and marked pigmentary incontinencewerepresent.> Dr Patrick Treacy shares some of his most challenging cases Dr Treacy’s CASEBOOK DR PATRICK TREACY Dr Patrick Treacy holds a H.Dip in Dermatology and a BTEC in Laser technology and skin resurfacing. He is Irish Regional Representative of the British College of Aesthetic Medicine. He is a renowned international guest speaker and features regularly on national television and radio programmes. >> “Quote to go in here”
- 2. 44 CASE FILES www.aestheticmed.co.uk Aesthetic Medicine • April 2014 S K I N / D E R M AT O L O G Y COMMENT Based on the clinical findings in his fingers a provisional diagnosis of Lichen Planus was made. Additionally, because the violaceous lesions developed on his forehead, which is a sun exposed area, andwasatrophicinappearance the suspicion of LPA (lichen planus actinicus) existed. This is a photodistributed variant of lichen planus that most often occurs in dark- complexioned young adults of Middle Eastern descent. (1) Four morphologic patterns have been clinically described in the literature including: summertime actinic lichenoid eruption, lichen planus atrophicus annularis, lichen planus tropicus, and lichenoid melanodermatitis (2). Although the etiology of this disease has not been determined, the lesions often are exacerbated by sun exposure and may improve spontaneously in the winter months (3).The lesions of lichen planus actinicus usually occur on the forehead,face,neck,andtheextensorsurfacesofthearmsandhands.(3-4). Thelateralaspectoftheforeheadisthemostcommonsiteofpresentation. (5).Clinically, lichen planus actinicus resembles the lesions found in discoid lupus erythematosus (DLE), granuloma annulare, melasma, morphea, secondarysyphilis,lichenoiddrugeruptionandpolymorphouslighteruption and should be differentiated by histopathologic and immunofluorescence (IF) findings (5). In DLE, the liquefaction, degeneration or thickening of the basal layer is more prominent and IF finding or autoantibody in a blood test may be the conclusive factor. In melasma, melanin synthesis in epidermal layerandthenumberofmelanocytesareincreased. The histologic features of lichen planus actinicus are consistent with findingsinclassiclichenplanus.(2-5)Hyperkeratosisofthestratumcorneum, hypergranulosis, basal cell vacuolization, and Civatte bodies usually are present. Although clinically similar to cutaneous lupus and polymorphous light eruption, lichen planus actinicus can be distinguished histologically from these photodermatoses. Lichen planus actinicus lacks follicular plugging, thickening of the basement membrane, and the periadnexal inflammatory infiltrate seen in cutaneous lupus erythematosus. (3-4). Clinical manifestations such as the site of lesion, age or the history of sun exposure should be examined for final diagnosis. Finally, the patient with lichenoiddrugeruptionshouldhaveahistoryofmedication. TREATMENT The cause of actinic LP is still unknown but sunlight might be the major precipitating factor. Several modalities such as topical corticosteroid, 4,6 hydroxychloroquine , intralesional corticosteroid injection, grenz ray, arsenic compounds or antimalarial agent have been applied for the treatment of actinic LP. (5-8). Acitretin, used in combination with topical steroids and sun avoidance, also has resulted in complete resolution of lesions without recurrence. (9) Van der Shroeff et all, induced actinic LP by using repeated doses of UVB radiation on the back. So sunscreen is considered necessary for treatment. (10). Although psoralen-UVA, isotretinoin,systemiccorticosteroids,cyclosporine,anddapsonehavebeen usedtotreatclassiclichenplanus,therearecurrentlynoreportsoftheiruse in lichen planus actinicus. (11-12).Recently topical 0.1% pimecrolimus cream have been reported to be successful in a case of actinic LP (12). This patient wassuccessfullytreatedwithPIGMANORM®CrèmeWIDMERwithactive ingredientsHydroquinone5.0g.Tretinoin0.1g.Hydrocortisone1.0g. AM REFERENCES 1. ZancaA,ZancaA.Lichenplanusactinicus.IntJDermatol. 1978;17:506-508. 2. SalmanSM,KibbiAG,ZaynounS.Actiniclichenplanus.JAm AcadDermatol.1989;20:226-231. 3 ShannaB.Meads,MD;JoyKunishige,BS;FranciscoA.Ramos- Caro,MD;AshrafM.Hassanein,MD,PhDCutis.2003;72:377- 381. 4. KatzenellenbogenI.Lichenplanusactinicus(lichenplanusin subtropicalcountries).Dermatologica.1962;124:10-20. 5. DilaimyM.Lichenplanussubtropicus.ArchDermatol. 1976;112:1251-1253. 6. BediTR.Summertimeactiniclichenoideruption. Dermatologica.1978;157:115-125. 7. VerhagenAR,KotenJW.Lichenoidmelanodermatitis.a clinicopathologicalstudyoffifty-oneKenyanpatientswithso- calledtropicallichenplanus.BritJDermatol.1979;101:651-658. 8. BoydA,NeldnerK.Lichenplanus.JAmAcadDermatol. 1991;25:593-619. 9. JansenT,GambichlerT,vonKobyletzkiL,etal.Lichenplanus actinicustreatedwithacitretinandtopicalcorticosteroids.J EurAcadDermatolVenereol.2002;16:174-175. 10 VanderShroeffJG,SchothorstAA,KanaarP.Inductionof actiniclichenplanuswithartificialUVsources.ArchDermatol 1983;119:498-500. 11. BakerH,AlmeydaJ.Lichenplanusactinicus.BritJDermatol. 1970;82:426-427. 12 EzzedineK,SimonartT,VereeckenP,HeenenM.Facialactinic lichenplanusfollowingtheBlaschko’slines:successful treatmentwithtopical0.1%pimecrolimuscream.JEurAcad DermatolVenereol2009;23:458-459. HISTOLOGY REPORT Skin with a prominent lichenoid superficial dermal infiltrate, composed predominantly of lymphocytes. Vacuolar interface change with associated basal apoptotic keratinocytes and focal lymphocyte exocytosis are present. The most striking feature is marked pigment incontinence in the dermis. The features are those of lichen planus actinus – a variant of lichen planus in which lesions are limited to sun exposedareas. Prof.KieranSheahan,Consultant Histopathologist,St.Vincent’sUniversity Hospital,ElmPark,Dublin4. DrLindaMulligan,PathologyRegistrar,St. Vincent’sUniversityHospital,ElmPark, Dublin4. “Quote to go in here”
