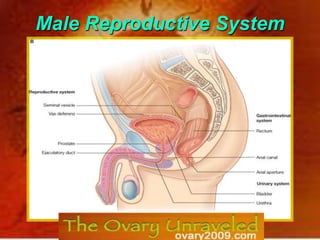
Human System System Of Male Reproductive
- 2. Primary Sex Organ Testis Accessory Sex Organs
- 7. Genital Ducts: store sperm &transport sperms
- 8. Accessory glands: secrete substances that nourish the sperms
- 10. Penis: organ of copulation
- 12. spermatozoa (exocrine function)
- 13. & testosterone hormone (endocrine function).
- 14. Location:
- 16. 3 capsules:
- 17. tunica vasculosa
- 18. tunica albuginia:fibrous layer, which thickened posteriorly to form mediastinum testis
- 20. Internal spermatic fascia: derived from the fascia transversalis
- 21. Cremasteric muscle and fascia: derived from the internal oblique muscle
- 23. The Covering Of The Testis (From Outside To Inside)
- 24. Internal Structure Of The Testis From the medistinum testis septa arise and dividing the testis into 250 lobules each lobule contains 1-4 convoluted seminiferous tubules(60 cm in length)
- 25. Connective tissue between the tubules contains interstitial cells of Leydig which secrete testosterone Spermatogenic cells: produce sperms Sertoli cells: supporting The seminiferous tubules join to form straight tubules called tubuli recti Which break into a network of canaliculi called rete testis.
- 27. left testicular vein drains into the left renal veinBlood Supply
- 28. Lymph Drainage of the Testis & Scrotum The lymph drainage of the testis and epididymis is into the lumbar or paraaortic lymph nodes at the level of the first lumbar vertebra. The lymph drainage of the scrotal wall is into the superficial inguinal lymph nodes.
- 30. It is a common disorder in young adults, with most occurring on the left side.
- 32. Imperfect descent (Cryptorchidism) Incomplete descent: in which the testis, although traveling down its normal path, fails to reach the floor of the scrotum. It may be found within The abdomen, within the inguinal canal, at the superficial inguinal ring, or high up in the scrotum. It is necessary for the testes to leave the abdominal cavity because the temperature there retards the normal process of spermatogenesis. If an incompletely descended testis is brought down into the scrotum by surgery before puberty, it will develop and function normally. A maldescended testis, although often developing normally, is susceptible to traumatic injury and, for this reason, should be placed in the scrotum. The incidence of tumor formation is greater in testes that have not descended into the scrotum.
- 33. Hydrocele: This is an accumulation of fluid within the tunica vaginalis. The indirect inguinal hernia: the protrusion of part of the abdominal contents into the inguinal canal &scrotum It is congenital in origin (the remains of the processus vaginalis). The hernial sac enters the inguinal canal through the deep inguinal ring and lateral to the inferior epigastric vessels. The hernial sac may extend down into the scrotum Scrotal swelling: Varicocele, Inguinal hernia, Hydrocele or testicular tumor
- 34. The Scrotum It is a sac of dark & wrinkled skin It is divided by a septum into right & left compartments, each of which enclose: a testis The epididymis The lower end of the spermatic cord
- 35. The wall of the scrotum has the following layers: Skin; dartos muscle; Colles’ fascia; external spermatic fascia; cremastric muscle &fascia; internal spermatic fascia& tunica vaginalis the dartos muscle is innervated by sympathetic nerve &contraction ofdartosmuscle wrinkles the scrotum & reducing heat loss. The external location of the testis in the scrotum brings the tests in an environment with a temperature less than the body by 1.5-2 degree, a condition necessary for thedevelopment & storage of the sperms.
- 38. testicular vein (Pampiniform plexus)
- 42. Cremasteric muscle & fascia: derived from the internal oblique muscle
- 45. Rete testis.
- 48. Vas deferens
- 51. 3-Then, it passes on the side wall of pelvis crossing the following from above down: External iliac vessels Umbilical artery Obturator nerve & vessels Then, it passes medially crossing over the ureter and descends behind the base of urinary bladder medial to seminal vesicle where it forms the ampulla of vas. It join the duct of seminal vesicle to form ejaculatory duct. Vasectomy:male sterilization is done by vasectomy, where a short segment of vas is cut through an incision in the upper part of the scrotum .
- 53. It opens in the prostatic urethra.
- 54. Urethra:
- 57. lying behind the urinary bladder, lateral to the ampulla of vas& anterior to the rectum.
- 58. Formed of highly coiled tube
- 59. Its duct joins the vas deferens to form ejaculatory duct
- 61. Site: lies below the neck of urinary bladder
- 62. behind the lower border of symphysis pubis
- 63. surrounding the upper part of the urethra (prostatic urethra).Shape: inverted cone which has: Apex. Base. 4 surfaces.
- 64. Apex: directed downwards Base: directed upwards. It is directly with the bladder neck. It is pierced by the urethra Posterior surface:related to ampulla of rectum It is pierced by 2 ejaculatory ducts Anterior surface: lies behind the lower border of Symphysis pubis
- 66. It produces an acidic secretion, which is add to the (25%) semen during ejaculation
- 67. The urethra & 2 ejaculatory ducts traverse the prostate; dividing it into 5 lobes: Lobes:1. Median:It lies between the urethra and the 2 ejaculatory ducts. It projects inside the urinary bladder forming “uvula vesicae” just behind the internal urethral meatus. It contains much glandular tissue (common site of adenoma). 2.Anterior, 3.Posterior 4.Right & 5. left lateral lobes
- 69. Per rectal examination of the prostateBulbourethral (Cowper’s) glands: They are small gland that lie on either side of membranous urethra. They open into penile urethra. They produce alkaline secretion that protecting the sperms & lubricate the tip of the penis
- 71. Ejaculation: is by sympathetic nerves.Corpora cavernosa Corpusspongiosum Bulb of penis Crus of penis
- 72. It consists of a : Root: that attach penis to perineum A body (shaft): Glans penis: enlarged end of the body. Prepuce (foreskin): partially covers glans and surrounds external urethral meatus (may be removed in circumcision)
- 73. Internal Structure Of The Penis It consists of 3 masses of erectile tissue: 2 corpora cavernosa Corpus spongiosum: is traversed by the urethra & its posterior end expand to form the bulb of the penis.
