Hereditary breast and ovarian cancer clinic visit visual aids (Mayo Clinic Florida)
•Download as PPT, PDF•
1 like•1,098 views
Report
Share
Report
Share
Recommended
More Related Content
What's hot
What's hot (20)
Beyond BRCA Mutations: What's New in the World of Genetic Testing?

Beyond BRCA Mutations: What's New in the World of Genetic Testing?
BRCA – IMPORTANCE IN HEREDITARY BREAST & OVARIAN CANCER by Dr Sharda Jain 

BRCA – IMPORTANCE IN HEREDITARY BREAST & OVARIAN CANCER by Dr Sharda Jain
Aviad Zick. Role of BRCA status in treatment planning

Aviad Zick. Role of BRCA status in treatment planning
Breast cancer genetic testing: Is it right for you?

Breast cancer genetic testing: Is it right for you?
HEREDITARY BREAST and OVARY CANCER [HBOC] SYNDROME, Dr BUI DAC CHI.![HEREDITARY BREAST and OVARY CANCER [HBOC] SYNDROME, Dr BUI DAC CHI.](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![HEREDITARY BREAST and OVARY CANCER [HBOC] SYNDROME, Dr BUI DAC CHI.](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
HEREDITARY BREAST and OVARY CANCER [HBOC] SYNDROME, Dr BUI DAC CHI.
Similar to Hereditary breast and ovarian cancer clinic visit visual aids (Mayo Clinic Florida)
All in the Family: Using Family Health History to Identify and Support Women ...

All in the Family: Using Family Health History to Identify and Support Women ...Chicago Center for Jewish Genetic Disorders
Similar to Hereditary breast and ovarian cancer clinic visit visual aids (Mayo Clinic Florida) (20)
All in the Family: Hereditary Risk for Gynecologic Cancer

All in the Family: Hereditary Risk for Gynecologic Cancer
Testing, genetic counselling and its implications in Gynaecological Cancers

Testing, genetic counselling and its implications in Gynaecological Cancers
Genetic Connections to Breast Cancer - February 14, 2023

Genetic Connections to Breast Cancer - February 14, 2023
All in the Family: Using Family Health History to Identify and Support Women ...

All in the Family: Using Family Health History to Identify and Support Women ...
Etiopathogenesis and Risk factors of Ca Breast.pptx

Etiopathogenesis and Risk factors of Ca Breast.pptx
More from Douglas Riegert-Johnson
More from Douglas Riegert-Johnson (14)
Version i. riegert johnson. colorectal neoplasms and hereditary syndromes

Version i. riegert johnson. colorectal neoplasms and hereditary syndromes
Lynch Syndrome and Serrated Polyposis Syndrome in 20 minutes.

Lynch Syndrome and Serrated Polyposis Syndrome in 20 minutes.
2016 may. version c. pearls in the management of pjs

2016 may. version c. pearls in the management of pjs
Companion slideshow for polyppolyp.com (Familial adenomatous polyposis)

Companion slideshow for polyppolyp.com (Familial adenomatous polyposis)
Familial Polyposis and Lynch syndrome review March 2014

Familial Polyposis and Lynch syndrome review March 2014
Recently uploaded
Recently uploaded (20)
Call Girls Service in Bommanahalli - 7001305949 with real photos and phone nu...

Call Girls Service in Bommanahalli - 7001305949 with real photos and phone nu...
Sonagachi Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now

Sonagachi Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now
Call Girls Jp Nagar Just Call 7001305949 Top Class Call Girl Service Available

Call Girls Jp Nagar Just Call 7001305949 Top Class Call Girl Service Available
Call Girls Service Nandiambakkam | 7001305949 At Low Cost Cash Payment Booking

Call Girls Service Nandiambakkam | 7001305949 At Low Cost Cash Payment Booking
Call Girls In Andheri East Call 9920874524 Book Hot And Sexy Girls

Call Girls In Andheri East Call 9920874524 Book Hot And Sexy Girls
Call Girls Hebbal Just Call 7001305949 Top Class Call Girl Service Available

Call Girls Hebbal Just Call 7001305949 Top Class Call Girl Service Available
Call Girls Whitefield Just Call 7001305949 Top Class Call Girl Service Available

Call Girls Whitefield Just Call 7001305949 Top Class Call Girl Service Available
Kolkata Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now

Kolkata Call Girls Services 9907093804 @24x7 High Class Babes Here Call Now
Glomerular Filtration and determinants of glomerular filtration .pptx

Glomerular Filtration and determinants of glomerular filtration .pptx
Bangalore Call Girls Marathahalli 📞 9907093804 High Profile Service 100% Safe

Bangalore Call Girls Marathahalli 📞 9907093804 High Profile Service 100% Safe
High Profile Call Girls Jaipur Vani 8445551418 Independent Escort Service Jaipur

High Profile Call Girls Jaipur Vani 8445551418 Independent Escort Service Jaipur
Call Girls Service Chennai Jiya 7001305949 Independent Escort Service Chennai

Call Girls Service Chennai Jiya 7001305949 Independent Escort Service Chennai
College Call Girls Pune Mira 9907093804 Short 1500 Night 6000 Best call girls...

College Call Girls Pune Mira 9907093804 Short 1500 Night 6000 Best call girls...
call girls in Connaught Place DELHI 🔝 >༒9540349809 🔝 genuine Escort Service ...

call girls in Connaught Place DELHI 🔝 >༒9540349809 🔝 genuine Escort Service ...
Russian Call Girls in Pune Riya 9907093804 Short 1500 Night 6000 Best call gi...

Russian Call Girls in Pune Riya 9907093804 Short 1500 Night 6000 Best call gi...
Mumbai Call Girls Service 9910780858 Real Russian Girls Looking Models

Mumbai Call Girls Service 9910780858 Real Russian Girls Looking Models
See the 2,456 pharmacies on the National E-Pharmacy Platform

See the 2,456 pharmacies on the National E-Pharmacy Platform
Russian Call Girls Chickpet - 7001305949 Booking and charges genuine rate for...

Russian Call Girls Chickpet - 7001305949 Booking and charges genuine rate for...
Call Girls ITPL Just Call 7001305949 Top Class Call Girl Service Available

Call Girls ITPL Just Call 7001305949 Top Class Call Girl Service Available
Call Girls Electronic City Just Call 7001305949 Top Class Call Girl Service A...

Call Girls Electronic City Just Call 7001305949 Top Class Call Girl Service A...
Hereditary breast and ovarian cancer clinic visit visual aids (Mayo Clinic Florida)
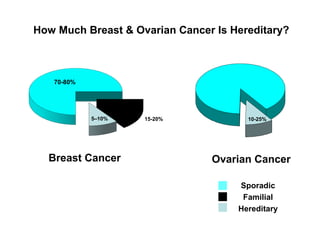
- 1. How Much Breast & Ovarian Cancer Is Hereditary? Ovarian CancerBreast Cancer 10-25% 70-80% 5–10% 15-20% Sporadic Familial Hereditary
- 2. Features of Hereditary and Sporadic Cancer in Hereditary Breast and Ovarian Cancer Syndrome (HBOC) Hereditary Sporadic • Multiple affected blood relatives in more than one generation • Typically, earlier age of onset (<50) • Individuals with bilateral or more than one cancer diagnosis (breast/ovarian) •Males with breast cancer • One or only a few affected blood relatives • Typically, later age of onset Br, 42 Br, 47 Ov, 58 Br, 35Ov, 50 Br, 72
- 3. Chromosomes BRCA1BRCA2 ***~84% of HBOC is caused by BRCA1 & BRCA2
- 4. 50% 50% BRCA1 -chromosome 17 BRCA2 - chromosome 13
- 5. BRCA1 & BRCA2 Lifetime Cancer Risks Type of Cancer General Population BRCA1 BRCA2 Female Breast Cancer 12% 56-87% 56-87% 2nd Breast Cancer 0.8-1.5% (per year – 5y) 5 year: 20% Lifetime: 64% 5 year: 12% Lifetime: 50% Ovarian Cancer 1.8% 44% 27% Male Breast Cancer 0.1% ~1-2% 6-10% Pancreatic Cancer <1% - - ~1.5-5% Melanoma 1-2% - - Increased Prostate Cancer 12% ~15-20% ~15-20%
- 6. Cancer Screening and Risk-Reduction Options Increased Screening Risk-Reduction Surgery Medications Breast • Monthly breast-self exam • Clinical breast exam every 6 months • Yearly mammogram • Yearly MRI Bilateral Mastectomy can reduce the risk of breast cancer by 96% Tamoxifen/ Raloxifene can reduce the risk of breast cancer by approximately 50% Ovarian • Transvaginal Ultrasound • CA-125 blood tests every 6 months * Limitations: Screening is not effective at picking up early stage cancer * Bilateral Salpingo- Oophorectomy (removing both the ovaries and fallopian tubes) can reduce the risk of ovarian cancer by 96% Oral Contraceptives (birth control pills) can reduce the risk of ovarian cancer by approximately 50%
- 7. Genetic Testing for Breast Cancer BRCA1 BRCA2 ATGCCGTATAGCTAGTCGATGTACG • Blood Test • Misspellings, Deleted, or Added DNA [i.e., mutation] • Tests offered: -Analysis of BRCA1 & BRCA2 genes [3-4 weeks] -Breast/Ovarian Panels [12 weeks] -Targeted mutation analysis (when family mutation is known) [3 weeks]
- 8. Possible Test Results Positive Result Increased chance of certain cancers; (implications for other family members ) (Known mutation detected) Mutation has been identified in Negative Result family (True Negative) (No mutation detected) - No increase in risk above the general population Mutation has not been identified in family and patient has cancer - Cancer most likely not due to BRCA1/2 Mutation has not been identified in family and patient does not have cancer - Doesn’t rule out BRCA1/2 Variant of Uncertain Significance Cancer risk not yet known (Mutation, but implications/management are not known)
- 10. Breast/Ovarian Panels **Includes BRCA1/2 & 19 additional genes that can increase the risk for breast cancer **High risk gene panel-BRCA1/2, CDH1, PTEN, STK11, TP53
