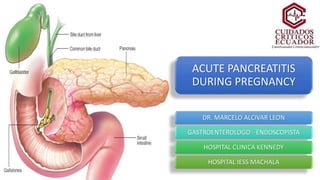
Pancreatitis en embarazo
- 1. ACUTE PANCREATITIS DURING PREGNANCY DR. MARCELO ALCIVAR LEON GASTROENTEROLOGO - ENDOSCOPISTA HOSPITAL CLINICA KENNEDY HOSPITAL IESS MACHALA
- 3. Acute pancreatitis is a relatively uncommon disease in pregnant women (1/1500–4500 pregnancies) Proposed numerous causes / unpredictable results Gallstone disease (70%) due to hormonal lithogenic effects Its progression can be fatal; fetal losses of up to 4.7% . Introduction Saldivar-Rodríguez D, Treviño-Montemayor OR, Guzman-López A, TreviñoMartinez G, Flores-Acosta .Ginecol Obstet Mex. 2016 feb;84(2):79-83.
- 4. VARIABLE 1 embarazo de cada 3.300 se complica con pancreatitis Swisher et al , 1 de cada 1.500 Legro y Laifer hallaron una incidencia de 1 de cada 4.000 Enfermedad litiásica de la vía biliar destaca como la causa más frecuente (67-100%) • Swisher SG, Hunt KK, Schmit PJ, Hiyama DT, Bennion RS, Thompson JE. Management of pancreatitis complicating pregnancy. Am Surg. 2016;60:759. 4. • Legro RS, Laifer SA. First trimester pancreatitis: Maternal and neonatal outcome. J Reprod Med. 2015;40:689. Epidemiology
- 5. 1990 0-37% 2000 11-37%, 2010 decrease Mortality Augustin G, Majerovic M. Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol 2007; 131: 4–12. 8. Hernandez A, Petrov MS, Brooks DC, Banks PA, Ashley SW, Tavakkolizadeh A. Acute pancreatitis and pregnancy: a 10-year single center experience. J Gastrointest Surg 2007; 11: 1623–1627 AP during pregnancy is a severe disease with a high maternal– fetal mortality rate (37% and 60%, respectively) according to old published series of cases, but this has recently decreased thanks to earlier diagnosis and some maternal and neonatal intensive care improvement
- 6. The most common etiological and risk factors of Acute Pancreatitis in Pregnancy Hacker FM, Whalen PS, Lee VR, Caughey AB. Maternal and fetal outcomes of pancreatitis in pregnancy. Am J Obstet Gynecol 2015;213:568.e1-5.
- 7. Sludge and stones in gallbladder during pregnancy Prevalence and risk factors A. MARINGHINI et al. Journal of Hepatology, 1987; 5:218-223
- 8. 19% • 1er Trim 26% • 2do Trim 53% • 3er Trim 60% • Parto pretérmino The most common etiological and risk factors of acute pancreatitis in pregnancy
- 9. The most common etiological and risk factors of acute pancreatitis in pregnancy Hacker FM, Whalen PS, Lee VR, Caughey AB. Maternal and fetal outcomes of pancreatitis in pregnancy. Am J Obstet Gynecol 2015;213:568.e1-5.
- 10. Definitions and Classification of AP Tang SJ, Rodriguez-Frias E, Singh S, Mayo MJ, Jazrawi SF, Sreenarasimhaiah J, et al. Acute pancreatitis during pregnancy. Clin Gastroenterol Hepatol 2016;8:85-90
- 11. • Abdominal ultrasound is safe and it has higher sensitivity than computerized tomography for detecting gallstones in cases of AP. • Magnetic resonance imaging (MRI) • AP • complications (edema, pseudocysts or hemorrhagic pancreatitis) • Main pancreatic duct is clear or not when persistent cholestasis occurs. • NO fetal toxicity even when gadolinium contrast media Imaging Roumieu F, Ponchon T, Audra P, Gaucherand P. Acute pancreatitis in pregnancy: place of the different explorations (magnetic resonance cholangiopancreatography, endoscopic ultrasonography) and their therapeutic consequences. Eur J Obstet Gynecol Reprod Biol 2008; 140: 141–142.
- 12. Definitions and Classification of AP Tang SJ, Rodriguez-Frias E, Singh S, Mayo MJ, Jazrawi SF, Sreenarasimhaiah J, et al. Acute pancreatitis during pregnancy. Clin Gastroenterol Hepatol 2016;8:85-90
- 13. Differential diagnosis of Acute Pancreatitis in Pregnancy Click B, Ketchum AM, Turner R, Whitcomb DC, Papachristou GI, Yadav D. The role of apheresis in hypertriglyceridemia induced acute pancreatitis: a systematic review. Pancreatology 2015;15:313-320.
- 14. Algorithm of treatment in acute biliary pancreatitis in pregnant women Acute pancreatitis during pregnancy G Ducarme et al. Journal of Perinatology (2014), 87 – 94
- 16. Cirugia Española 2014, 92 (7): 468 - 471
- 17. Revista Facultad de Salud - RFS - Julio - Diciembre.
- 18. International Journal of Applied and Basic Medical Research, Jul-Dec 2013, Vol 3, Issue 2 Conservative medical management of acute pancreatitis was the main stay of treatment. Surgical management (laparoscopic cholecystectomy) was carried out for the underlying cause (cholelithiasis) in three patients. One patient underwent ERCP for CBD stone
- 19. SUMMARY
- 20. A multidisciplinary approach, including gastroenterology and obstetric care, seems to be a key in making the best choice for management of AP during pregnancy Traditionally conservative, the treatment of biliary lithiasis depends on the symptoms. There is no consensus in the literature regarding the management of AP during pregnancy. AP during pregnancy is a rare but severe disease. CONCLUSIONS
Editor's Notes
- La pancreatitis aguda es una enfermedad inflamatoria que afecta al tejido pancreático, de la que se han propuesto numerosas causas.1 Los casos de pancreatitis durante el embarazo son realmente excepcionales, por lo que la información de sus complicaciones maternas y fetales es limitada.2 Su etiología ha sido largamente estudiada; en el siglo XIX Claude Bernard propuso como posible causa el reflujo biliar en el conducto pancreático. Opie asoció la litiasis vesicular con la pancreatitis, a estas causas se agregó, posteriormente, el consumo de alcohol como predisponente.1 Su incidencia varía en diferentes estudios publicados,3 se reporta desde 1 caso por cada 1000 embarazos, hasta 1 en 3000,4 40002 e incluso hay reportes de caso por cada 12,000 nacidos vivos, según la población estudiada. Reportes en los decenios de 1970 y 1980 estiman tasas de mortalidad materna y perinatal entre 0-37% y 11-37%, respectivamente.5,6 Sin embargo, reportes del 2000 señalan una disminución de las complicaciones para la madre y el recién nacido debido a los avances en el tratamiento de las complicaciones y al desarrollo de las técnicas quirúrgicas. Las causas más comunes relacionadas con la pancreatitis aguda durante el embarazo son: litos vesiculares (66%), abuso de alcohol (12%), idiopática (17%), hiperlipidemia (4%) y menos comúnmente hiperparatiroidismo, traumatismo, debida a medicamentos o hígado graso del embarazo.7 Durante el embarazo el incremento en los lípidos es fisiológico y casi siempre se debe a variaciones en las concentraciones hormonales. Este aumento aporta a la madre una fuente energética valiosa, tanto para el mantenimiento de su metabolismo basal, como para favorecer el desarrollo Hospital Universitario Dr. José Eleuterio Gonzalez, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León. Correspondence Dr. Oscar Rubén Treviño Montemayor dr_ortm@hotmail.com tions is limited.
- Reportes en los decenios de 1970 y 1980 estiman tasas de mortalidad materna y perinatal entre 0-37% y 11-37%, respectivamente.5,6 Sin embargo, reportes del 2000 señalan una disminución de las complicaciones para la madre y el recién nacido debido a los avances en el tratamiento de las complicaciones y al desarrollo de las técnicas quirúrgicas
- Brigham and Women’s Hospital (Boston, MA) from January 1, 1996 through January 1, 2006 . 93,440, which estimates the incidence of 34 pctes AP in pregnancy at 0.02%, or 1 in 4,449 pregnancies. y. The disease usually appears during the third trimester or in the early postpartum period with the association of symptoms like upper abdominal pain, nausea or vomiting, anorexia, fever and elevated serum amylase or lipase activities.
- HCC incidence rates have increased in each successive birth cohort born between 1900 and 1959 3 (Fig. 2). In addition, the age distribution of HCC patients has shifted to younger ages, with the greatest proportional increases among individuals 45–60 years old
- HCC incidence rates have increased in each successive birth cohort born between 1900 and 1959 3 (Fig. 2). In addition, the age distribution of HCC patients has shifted to younger ages, with the greatest proportional increases among individuals 45–60 years old
