Overview of Colposcopy.pdf
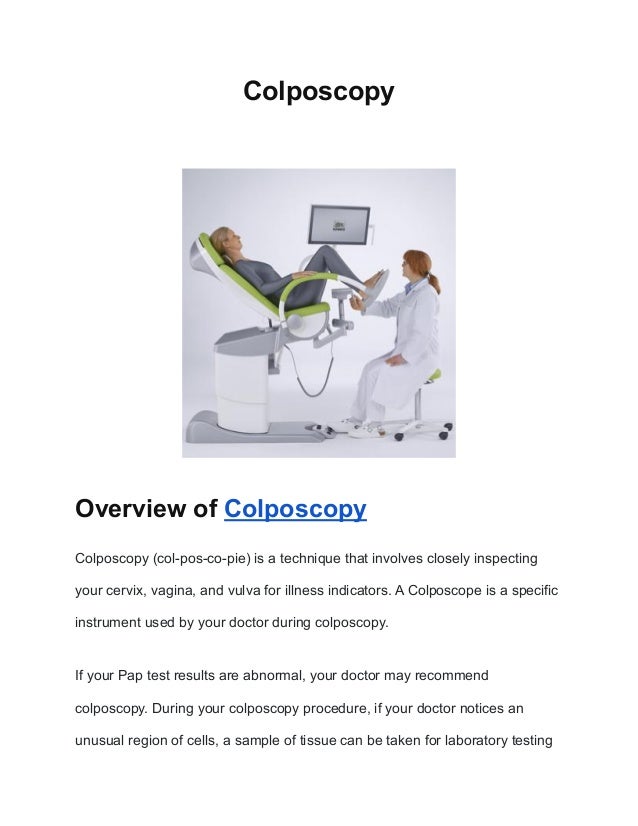
- 1. Colposcopy Overview of Colposcopy Colposcopy (col-pos-co-pie) is a technique that involves closely inspecting your cervix, vagina, and vulva for illness indicators. A Colposcope is a specific instrument used by your doctor during colposcopy. If your Pap test results are abnormal, your doctor may recommend colposcopy. During your colposcopy procedure, if your doctor notices an unusual region of cells, a sample of tissue can be taken for laboratory testing
- 2. (biopsy). You may experience anxiety before your colposcopy exam. Knowing what to expect during your colposcopy may help you feel more comfortable. What is a colposcopy? A colposcopy is a cervical cancer screening test. It allows your doctor or nurse to examine your cervix – the entryway to your uterus — up close. It’s used to look for cancerous cells in your cervix. History of colposcopy The first colposcopy was performed in March of 1924. Colposcopic examination was nearly impossible to undertake in the early studies due to the close proximity of the focus, which was only 80 mm. Hinselmann attempted to resolve the issue by removing the uterine cervix. This procedure anesthetizes the part being checked, which can affect the final outcome and cause a little amount of blood to bleed. Furthermore, if the portion is gripped by a thin
- 3. forceps, the patient may experience pain. Colposcopy, which had been established in Germany, has slowly spread throughout its homeland, owing to Hinselmann’s numerous errors technique that was proposed and is virtually solely used to detect cervical cancer early. Hinselmann, Hans (1884-1959) His stubbornness in considering leukoplakia as a precancerous lesion imposed on him a lot of opponents. His authoritative imposition of terms, especially histological, caused resistance by histopathologists, possibly due to fear of losing their prestige, who considered them too complex; his stubbornness in considering leukoplakia as a precancerous lesion imposed him a lot of opponents; There was no suitable instructional material available to several gynecologists until the 1950s; Hinselmann’s temperament, described by Wespi as a mix of innocence and missionary fervor, had not equipped him for conversation and compromise.
- 4. What is happening during a colposcopy and biopsy? You’ll lie down on an exam table, similar to how you’d lie down for a pelvic exam. A speculum will be inserted into your vaginal opening by the doctor or nurse. This splits the walls of your vaginal canal, allowing them to have a better look at your cervix. They’ll use a vinegar-like solution to clean your cervix. This makes aberrant cells more visible. They’ll then examine your cervix with a Colposcope, which looks like binoculars on a stand with a bright light. The Colposcope does not make contact with you or enter your body. A biopsy will be performed if your doctor or nurse notices something that doesn’t appear to be normal. This means a little sample of tissue will be taken and sent to a lab.
- 5. Types of Biopsy There are two types of biopsy. Type one: tissue from the exterior of your cervix. Type two: removes tissue from inside your cervix’s opening. More than one biopsy may be required in some cases. It only takes 5-10 minutes to perform a colposcopy and biopsy.
- 6. Is a Colposcopy painful? A Colposcopy is almost painless. When the speculum is inserted, you may feel pressure. When they cleanse your cervix with the vinegar-like fluid, it may sting or burn a little. You may experience some discomfort if you get a biopsy. The majority of people describe it as a strong pinch or a menstrual cramp. After a biopsy, you may experience some spotting, bleeding, or dark discharge from your vaginal area for a few days.
- 7. What should I be aware of prior to my appointment for Colposcopy? To prepare for a colposcopy, you don’t need to do anything. Here are two things you can do to help things go more smoothly: One is: Schedule your colposcopy for when you won’t be bleeding much or when you won’t be on your period. It’ll be easier to see your cervix this way. Two is: The day before your session, avoid having vaginal sex or inserting anything into your vagina (such as fingers or sex toys). Where can I get a Colposcopy? A colposcopy can be done at your doctor’s or nurse’s office, some community health clinics, or a Planned Parenthood health facility near you. What happens if I have a Colposcopy? After your colposcopy and biopsy, you should have no difficulties. If your results reveal any issues, your doctor may recommend more tests or treatment.
- 8. What should I do following my Colposcopy Procedure? Your vagina may be a bit sore for a number of days after a colposcopy. Spotting or dark-colored vaginal discharge are possible side effects of a biopsy. Unless your doctor or nurse tells you not to, use a pad, panty liner, or tampon. Following your colposcopy and biopsy, there are a few more things to keep in mind: You are free to shower or bathe whenever you like. You can have vaginal sex whenever you want if you didn’t have a biopsy. If you have a biopsy, you should wait 3 days before having vaginal sex. Your cervix will be able to recover as a result of this. Continue to take any drugs you’re taking, including birth control, as usual.
- 9. What are the possible side effects of a colposcopy and biopsy? https://web.facebook.com/BLXMedical/photos/a.1027761811355497/1027761 778022167/ It is uncommon to experience complications following a colposcopy and biopsy. Bleeding or an infection that requires treatment are rare hazards. If you have any concerns, contact your doctor or nurse: Unless you assume it’s your period, bleeding that’s heavier than spotting. Chills or a fever. Vaginal discharge that is thick, yellow-colored, or smells terrible. Terrible discomfort in the lower belly button. If You’re Pregnant. A Colposcopy technique is safe to have while you’re pregnant. While having a biopsy while pregnant is quite low-risk, your doctor may advise you to wait until after your baby is born. Pregnant women may experience greater
- 10. bleeding following a biopsy than non-pregnant women. This is due to the increased blood flow to the cervix during pregnancy. Don’t worry: a colposcopy and biopsy will not prevent you from having children in the future. What if the results of my Colposcopy aren’t Normal? You may not need to take any action right away if your doctor or nurse discovers abnormal cells. You may require additional tests or treatments at times. It depends on the degree to which your cervical cells are aberrant. Your doctor or nurse may advise you to wait and see if the cells heal on their own. You’ll undergo another Pap test and possibly other tests to monitor the cells in this scenario.
- 11. Your biopsy may also serve as a treatment. This is because during the biopsy, your doctor may be able to remove all of your problematic cells. You won’t need any more treatment if this is the case. You’ll resume undergoing pelvic exams, Pap tests, and/or HPV tests on a regular basis. Your doctor or nurse will advise you on how frequently you should get these tests. You may possibly require additional treatment. There are four treatments for eliminating aberrant cells and avoiding cervical cancer that are very effective.
- 12. Advantages of Colposcopy Women between the ages of 21 and 65 who have cytology every 2 to 3 years had a lower risk of dying from cervical cancer. Cervical cancer could kill ten out of every 1,000 women who do not get checked. Cervical cancer might kill two out of every 1,000 women who are checked. As a result, for every 1,000 women who get checked, there are 8 fewer cervical cancer-related deaths. This is as a result of the fact that: Screening aids in the detection of abnormal cells in the cervix that can lead to cancer. Before cancer starts, a doctor can remove the portions of the cervix
- 13. that contain these cells. Screening lessens the risk of cervical cancer in this way. If a cancer has already developed, early detection through screening increases the odds of a successful recovery. Disadvantages of Colposcopy Despite their benefits, cytology is not without flaws. An abnormal cytology indicates that the cells that line the cervix have changed. As a result, the lady must have a procedure known as a colposcopy. Anxiety can arise from receiving an abnormal cytology test and waiting for colposcopy results. Colposcopy results are usually normal. A colposcopy can be unpleasant and even painful. The presence of abnormal cells can be detected with a colposcopy. These cells can, but do not always, turn cancerous. Because it is hard to predict the presence of abnormal cells in the cervix, the area of the cervix containing these cells must be removed as a precaution. As a result, some women may have a portion of their cervix removed “for no reason.” As indicated in the statistics below, such cases disproportionately affect younger women:
- 14. As a result of screening, the number of women who have a colposcopy has increased. Colposcopy Units The colposcopy facility is a suitable location for triaging patients with lower genital tract diseases, particularly those who have been recognised as having a high risk of acquiring cancer by screening testing. The colposcopic process, related instrumentation, and internationally accepted colposcopic terminology have all been discussed in this article.
