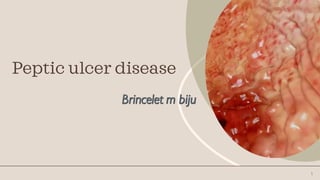
PEPTIC ULCER DISEASE,SLIDESHARE PRESENTATION
Peptic ulcer disease (PUD) is the presence of one or more ulcerative lesions in the stomach or duodenum. Etiologies include infection with Helicobacter pylori (most common), prolonged NSAID use (NSAID-induced ulcer), conditions associated with an overproduction of stomach acid (hypersecretory states), and stress. Epigastric pain is a typical symptom of PUD; however, many patients remain asymptomatic. Usually, patients younger than 60 years of age can be managed with a test-and-treat strategy for H. pylori infection or with empirical acid suppression therapy. Older patients and those with high-risk clinical features benefit from an esophagogastroduodenoscopy (EGD) and biopsies to confirm the diagnosis or rule out differential diagnoses (especially gastric cancer). First-line treatment for most peptic ulcers involves symptom control (e.g., acid-lowering medication), H. pylori eradication therapy, and withdrawal of causative agents. Antisecretory drugs (e.g., proton-pump inhibitors), which reduce stomach acid production, are continued for 4–8 weeks after eradication therapy and may be considered for maintenance therapy if symptoms recur. Surgical intervention may be considered in rare cases. Some patients benefit from endoscopic surveillance, especially if symptoms persist or there is clinical suspicion for malignancy. Peptic ulcer: a defect in the gastric or duodenal mucosa with a diameter of at least 0.5 cm and a depth that penetrates through the muscularis mucosae [1] Gastric ulcer: a peptic ulcer of the gastric mucosa, typically located along the lesser curvature in the transitional portion between the corpus and antrum Duodenal ulcer: a peptic ulcer of the duodenal mucosa, usually located on the anterior or posterior wall of the duodenal bulb
Recommended
More Related Content
What's hot
What's hot (20)
Similar to PEPTIC ULCER DISEASE,SLIDESHARE PRESENTATION
Similar to PEPTIC ULCER DISEASE,SLIDESHARE PRESENTATION (20)
More from BRINCELET M BIJU
More from BRINCELET M BIJU (17)
Recently uploaded
Recently uploaded (20)
PEPTIC ULCER DISEASE,SLIDESHARE PRESENTATION
- 2. Definition 2 ❑Peptic ulcer are the open sores that occurs in the lining of the stomach or small intestine. It is the erosion of mucosal layer and break in the lining of the stomach . ❑Peptic ulcer results from imbalance of protective factors like bicarbonate ,mucus and damaging factors like acid and pepsin. ❑Incidence of duodenal ulcer is more common than gastric ulcer.
- 3. There are three types of peptic ulcers; ❑Gastric ulcers : ulcers that develop inside the stomach ❑Esophageal ulcers : ulcers that develop inside the esophagus ❑Duodenal ulcers : ulcers that develop in the upper section of the small intestines, called the duodenum 3
- 4. Risk factors: ❑Smoking ❑Alcohol intake ❑Spicy food ❑Prolong use of NSAIDS(eg; paracetamol, ibuprofen) ❑H.pylori ❑Stress like major injuries,illness,tumour. ❑Gender: duodenal ulcer are increasing in older women. ❑Age duodenal:30-40 ,,Gastric over 50
- 5. Difference between gastric and duodenal ulcer 5 Gastric. 1. They occur in stomatch. 2. They cause by injury like Substances,alcohol,aspirin,NSAIDs,drugs. 3. Pain in left epigastric region in gastric ulcer 4. Nausea is common, vomiting with blood occurs in this case. 5. Weight loss, pain starts just after taking food 6. Pain is present while hungry. 7.Malignancy is not common Duodenal 1. They occur in duodenum 2. these are cause by HCl secretion by vagus nerve 3. Pain in the right epigastric region 4. Stool with blood. 5. No weight loss,onset of pain after 2-4hrs of taking food 6. Absent 7. Malignancy is common
- 6. Etiology 6 ❑Epigastric pain ❑Nausea ❑Vomiting ❑Dyspepsia ❑Bloating ❑Belching ❑Pain after food intake ❑Radiation therapy ❑Stomach cancer
- 7. Clinical manifestations ❑The most common symptom of a peptic ulcer is burning abdominal pain that extends from the navel to the chest, which can range from mild to severe. In some cases, the pain may wake you up at night. Small peptic ulcers may not produce any symptoms in early phases. ❑Other common signs of a peptic ulcer include; ❑Changes in appetite ❑Nausea ❑Bloody or dark stools ❑Unexplained weight loss ❑Indigestion ❑Vomiting ❑Chest pain 7
- 8. Complications ❑Perforation leading to peritonitis ❑Haemorrhage by erosion of vessel in base. ❑Penetration of surrounding organ (liver/pancreas) ❑Obstruction (by scarring) - pyloric stenosis ( cancer – rare event in true peptic ulcer ) 8
- 9. Diagnostic tests 9 ❑Medical history ❑Physical exam ❑Lab tests • Stool examination for fecal occult blood • Complete blood count for decrease in blood cells. ❑Upper gastrointestinal endoscopy and biopsy ❑Upper GI series ❑Computerised tomography scan
- 10. Lifestylemodification ❑Discontinue NSAIDs ❑Smoking cessation ❑Alcohol cessation ❑Stress reduction 10
- 11. Drug management ❑Antibiotic medications to H. Pylori. If H.pylori is found in your digestive tract, the doctor may recommend a combination of antibiotics to kill the bacterium. These include amoxicillin,clarithromycin,methronidazole. ❑Proton pump inhibitors Also called PPIs reduce stomach acid by blocking the action of the parts of cells that produce acid. These drugs include the prescription and over the counter medications like omeorazole,lansoprazole. ❑ Acid blockers Also called histamine blockers,reduce the amount of stomach acid released into your digestive tract, which relieves ulcer pain and encourages healing eg; ranitidine ❑Antacids Neutralize existing stomach acid and can provide rapid pain relief.side effects can include constipation or diarrhoea, depending on the main ingredients. 11
- 13. ❑H. Pylori is the most common cause of PUD and is a risk factor for gastric cancer. ❑H.pylori eradication reduces the risk of the disease reoccurrence ❑Test and test strategy is recommended for patients with undifferentiated dyspepsia ❑Initial evaluation with endoscopy is recommended for those with alarm symptoms or those failing treating ❑Optimum treatment regimens are 14d multidrug with antibiotics and acid suppressants (triple therapy) 13 Summary
- 14. Thank you Brincelet m biju
