Axillary Hidradenitis Reconstruction Using a Dermal Regeneration Template.pptx
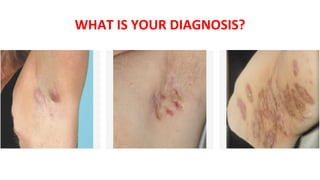
- 1. WHAT IS YOUR DIAGNOSIS?
- 3. Axillary Hidradenitis Reconstruction Using a Dermal Regeneration Template Casey Kraft, MD1 and Gregory Pearson, MD1,2 1Ohio State University Wexner Medical Center, Columbus, OH; 2Nationwide Children's Hospital, Columbus, OH Correspondence Gregory Pearson, MD, Nationwide Children's Hospital, 700 Children's Dr, Columbus, OH 43205; gregory.pearson@nationwidechildrens.org February 2022 ISSN 1044-7946 Index Wounds 2022;34(2):43–46 PRESENTER: Gerelmaa J, MD AGAPE CHRISTIAN HOSPITAL, JOURNAL CLUB 2022.04.29
- 4. Introduction Hidradenitis suppurativa can be a debilitating condition, particularly in the pediatric population. Axillary hidradenitis can be particularly challenging because of the risk of scar contracture and limited range of motion after definitive resection and reconstruction.
- 5. TREATMENT OPTION • A dermal regeneration template (DRT) • Skin grafting
- 6. Dermal Regeneration Template (DRT)
- 7. This case series retrospectively reviewed and evaluated outcomes using DRT and skin grafting for axillary hidradenitis reconstruction.
- 8. Materials and Methods • Patient selection Single surgeon, patients between 2015 -2018 Inclusion criteria: DRT was used for the reconstruction. Exclusion criteria: - reconstruction using any other method - absence of plastic surgery involvement in reconstruction - hidradenitis location other than the axilla.
- 9. Materials and Methods Treatment data: - several negative pressure wound therapy (NPWT) changes - time to skin grafting - age at treatment - pain medication consumption - axillary range of motion. Surgical complications: - infection - DRT loss - graft loss - hidradenitis recurrence
- 10. Surgical technique Representative example of hidradenitis suppurativa preoperatively with areas of drainage and induration.
- 11. Surgical technique • Complete axillary excision was performed to encompass all hair follicles of the axilla. • Excision: - dermis to the subcutaneous tissue - all affected dermis
- 12. Surgical technique - The DRT was then trimmed to the shape of the excised area and stapled into place.
- 13. Surgical technique - The NPWT device - Airplane splint that had been customized preoperatively by an occupational therapist
- 14. Surgical technique - This splint remained - The patient was then admitted to the hospital - Weekly or biweekly NPWT changes - Complete take of the DRT - in the OR
- 15. Surgical technique - The NPWT device - Gentle use of the arm as tolerated was allowed, and standard wound care for skin grafting
- 16. Results
- 17. Discussion - Axillary reconstruction- NPWT, skin grafting, local flaps, extended latissimus dorsi flaps, and thoracodorsal artery perforator flaps.[9–12] - bilayer DRT - good results.[13,14] - These studies are limited, with Ribeiro and Guerra[13] describing a single case report and Gonzaga et al[14] reporting a cohort of 4 patients with a 25% skin substitute loss rate and 50% reoperation rate.
- 18. Discussion - there were no unplanned operations - there was no DRT loss or recurrence of hidradenitis. - Cost concerns have been raised in the literature. - Reduced risk of axillary contracture from using DRT and the elimination of additional donor sites is worth consideration until higher-level studies are performed.
- 19. Limitations - This study is a limited case series of a single surgeon's experience at 1 academic center - Additional prospective, large-scale, multi- surgeon studies are warranted for further analysis
- 20. Conclusions 1. Management of axillary hidradenitis with complete excision and reconstruction using a DRT with skin grafting appears to be safe and effective in the pediatric population.
- 21. Conclusions 2. Patients in the current cohort tolerated the procedure well and had no complications, including loss of DRT or skin graft, infection, loss of axillary range of motion, or recurrence of hidradenitis.
- 22. Conclusions 3. Surgeons should consider using this method of reconstruction for axillary hidradenitis, although more extensive studies are needed to confirm its safety and efficacy.
- 23. 1.ACH case 2.Recommendation for other doctors
- 24. DIAGNOSIS
- 25. TREATMENT RECOMMENDATIONS The Hurley staging system: • mild and moderate cases (stages I and II) - topical antibiotics, oral antibiotics, biologics, laser therapy, and botulinum toxin.[2–5] • severe cases (stage III)- wide excision and reconstruction.[6,7]
