Nursing case-study-musculoskeletal-philnursingstudent-philnursingstudent
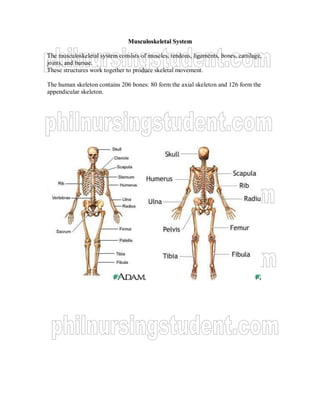
- 1. MMuussccuulloosskkeelleettaall SSyysstteemm The musculoskeletal system consists of muscles, tendons, ligaments, bones, cartilage, joints, and bursae. These structures work together to produce skeletal movement. The human skeleton contains 206 bones: 80 form the axial skeleton and 126 form the appendicular skeleton.
- 2. FFUUNNCCTTIIOONNSS MMoovveemmeenntt aanndd mmaaiinnttaaiinnss ppoossttuurree SSuuppppoorrtt PPrrootteeccttiioonn HHeemmaattooppooiieessiiss Mineral homeostasis ANATOMY AND PHYSIOLOGY Muscles: the body contains three major muscle types: visceral (involuntary, smooth), skeletal (voluntary, striated), and cardiac. Tendons: are bands of fibrous connective tissue that attach muscle to the periosteum (fibrous covering the bone). Enables the bone to move when skeletal muscles contract. Ligaments: dense, strong, flexible bands of fibrous connective tissue that tie bones to other bones. Bones: perform anatomic (mechanical) and physiologic functions. Protecting internal tissues and organs Stabilizing and supporting the body Providing a surface for muscle, ligament, and tendon attachment Moving through ―lever‖ action when contracted Producing red blood cells in the bone marrow (hematopoiesis) Storing mineral salts Bone formation Cartilage composes the fetal skeleton at 3 months in utero. By about 6 months, the fetal cartilage has been transformed into bony skeleton. Two types of osteocytes, osteoblasts and osteoclasts, are responsible for remodeling—the continuous process whereby bone is created and destroyed. Osteoblasts deposit new bone. Osteoclasts increase long-bone diameter through reabsorption of previously deposited bone. Cartilage: a dense connective tissue that consists of fibers embedded in a strong, gel-like substance. Avascular and lacks innervation Fibrous cartilage: forms the symphysis pubis and the intervertebral disks. Hyaline cartilage: covers the articular bone surfaces; connects the ribs to the sternum; and appears in the trachea, bronchi, and nasal septum. Elastic cartilage: located in the auditory canal, external ear, and epiglottis. It cushions and absorbs shock, preventing direct transmission to the bone.
- 3. Joints: two or more bones meet a joint. Synarthrodial joints, such as cranial sutures, permit no movement. This joint type separates bones with a thin layer of fibrous connective tissue. Amphiarthrodial joints, such as the symphysis pubis, allow slight movement. This joint type separates bones with hyaline cartilage. Diarthrodial joints, such as the ankle, wrist, knee, hip, and shoulder, permit free movement Bursae: located at friction points around joints between tendons, ligaments, and bones, bursae are small synovial fluid sacs that act as cushions, thereby decreasing stress to adjacent structures. AASSSSEESSSSMMEENNTT History o Reason for seeking care o Present illness o Medical history o Family history o Psychosocial history Physical Examination o Observe posture, gait and coordination o Inspect and palpate muscles: tone and mass; strength and joint ROM o Inspect and palpate joints and bones o Length of the extremities DIAGNOSTIC TESTS ASPIRATION Arthrocentesis: helps to assess infection and distinguish forms of arthritis, such as pseudogout and infectious arthritis. o In joint infection, for example, synovial fluid looks cloudy and contains more WBC and less glucose than normal. o When trauma causes bleeding into a joint, synovial fluid contains red blood cells. o In specific types of arthritis, crystals can confirm the diagnosis—for example, urate crystals indicate gout. o In symptomatic joint effusion, removing excess synovial fluid relieves pain. Nursing considerations o Describe this 10-minute procedure to the patient. o Patient will assume a position depending on the joint being aspirated, and then asked to remain still. o After withdrawing the fluid, he’ll apply a small bandage to the puncture site.
- 4. o After the test, ice or cold packs may be applied to the joint to reduce pain and swelling. o Advise patient not to use the joint excessively after the test to avoid joint pain, swelling, and stiffness. o Report any increased pain, tenderness, swelling, warmth, or redness as well as fever, these may signal infection. Bone marrow aspiration: help diagnose many abnormalities, including rheumatoid arthritis, tuberculosis, amyloidosis, syphilis, bacterial or viral infection, parasitic infestation, tumors and hematologic problems. o Aspiration usually involves the sternum or iliac crests. o The site is prepared and then infiltrated with a local anesthetic such as lidocaine. o The doctor inserts the marrow needle through the cortex; marrow cavity penetration causes a collapsing sensation. o Aspirates 0.2 to 0.5 ml of fluid. Nursing considerations o Inform patient that he’ll feel pressure as the doctor inserts the needle and that aspiration may hurt. o Procedure may last about 10 minutes that he’ll be sedated. o Watch for signs of infection after the procedure and make sure bleeding stops. ENDOSCOPY Arthroscopy: helps to assess joint problems, plan surgical approaches, and document pathology. o Used to evaluate the knee. Nursing considerations o Explain to the patient that this test allows direct examination of the inside of a joint and that it’s safe, convenient approach to surgery. o Done in the operating room under general or local anesthesia and takes 30 to 60 minutes. o Instruct NPO after midnight. o Check hypersensitivity to local anesthetics. o After the procedure patient can walk as soon as he’s fully awake and he’ll experience mild soreness and a slight grinding sensation in his knee for 1 to 2 days. o Instruct patient to notify doctor if he feels severe or persistent pain or develops a fever with signs of local inflammation. o Assess for signs of complications such as infection, hemarthrosis (blood accumulation in the joint), or a synovial cyst.
- 5. LABORATORY TESTS Blood tests: to rule out systemic infection, anemia, and white blood cell disorders as well as studies to measure blood levels of alkaline phosphatase, calcium, creatine kinase, and rheumatoid factor. o Check blood levels of antinuclear antibodies, phosphorus, and serum uric acid o Measure Erythrocyte Sedimentation Rate (ESR) — the rate at which red blood cells settles in uncoagulated blood during a 1-hour period. o Serial ESR measurements help monitor general or localized inflammation, which cause the rate to increase. Urine tests: 24-hour urine collection to check uric acid levels. o Check for urine for Bence Jones protein, which may indicate a bone tumor, hyperparathyroidism, or osteomalacia. RADIOGRAPHIC AND IMAGING STUDIESS Bone scan: detect bony metastasis, benign disease, fractures, avascualr necrosis, and infection. o IV introduction of a radioactive material, such as the radioisotope technetium polyphosphate, the isotope collects in areas of increased bone activity or active bone formation. Nursing considerations o Explain the procedure to the patient. o Fasting isn’t necessary. o Explain to the patient that there will be a 2- to 3- hour waiting period after the isotope is injected. o While waiting, the patient must drink four to six glasses of fluid. o Lie supine on a table within the scanner and lie as still as possible and to expect to assume various positions. Computed tomography: aids diagnosis of bone tumors and other abnormalities. o Helps to assess questionable cervical or spinal fractures, fracture fragments, bone lesions, and intra-articular loose bodies. Nursing considerations o Explain to the patient that CT helps detect bone abnormalities and that it takes 30 to 90 minutes. o If the patient is scheduled to receive a contrast medium, inform him that he must not eat for 4 hours before the test. o Instruct patient to remain still during the test. o If the patient received a contrast medium by mouth, encourage him to drink plenty of fluid after the test to help flush the contrast medium from his body.
- 6. Magnetic resonance imaging (MRI): show irregularities of the spinal cord and is especially useful for diagnosing disk herniation. Nursing considerations o Explain that the procedure may take up to 90 minutes and advise the patient to use the bathroom before the test. o Ask the patient to remove all metal objects, including bobby pins, jewelry, watches, eyeglasses, hearing aids, and dental appliances. o Remove clothes with metal zippers, buckles, or buttons as well as credit, bank, and parking cards because the scan could erase the magnetic codes. X-rays: help diagnose traumatic disorders, such as fractures and dislocations. o Reveal bone disease and joint disease Nursing considerations o Remove all jewelry. o Verify that the X-ray order includes pertinent recent history, such as trauma, and identifies the point tenderness site. BONE DISORDERS HALLUX VALGUS o Lateral deviation of the great toe at the metatarsophalangeal joint o Occurs with medial enlargement of the first metatarsal head and bunion formation. Causes: congenital or familial o More commonly acquired from degenerative arthritis or from prolonged pressure, especially form narrow-toed high-heeled shoes that compress the forefoot. Assessment findings: o May appear as a red tender bunion o Angulation of the great toe away from the midline of the body toward the other toes. o Advanced stages: may develop a flat, splayed forefoot, severely curled toes (hammertoes), and a small bunion on the fifth metatarsal. Diagnostic test: o X-rays confirm diagnosis by showing medial deviation of the first metatarsal and lateral deviation of the great toe. Treatment: o good foot care and proper shoes o felt pads to protect the bunion, foam pads or other devices to separate the first and second toes at night o supportive pad and exercises to strengthen the metatarsal arch.
- 7. o Early treatment is vital in patients predisposed to foot problems, such as those with rheumatoid arthritis or diabetes mellitus. o Severe deformity doctor may order bunionectomy MMUUSSCCUULLOOSSKKEELLEETTAALL IINNJJUURRIIEESS CCOONNTTUUSSIIOONNSS,, SSTTRRAAIINNSS,, AANNDD SSPPRRAAIINNSS CCoonnttuussiioonn-- ssoofftt ttiissssuuee iinnjjuurryy pprroodduucceedd bbyy bblluunntt ffoorrccee.. Many small blood vessels rupture and bleed into soft tissues (ecchymosis or bruising). A hematoma develops when the bleeding is sufficient to cause an appreciable collection of blood. SSttrraaiinn-- ――mmuussccllee ppuullll‖‖ ffrroomm oovveerruussee,, oovveerrssttrreettcchhiinngg,, oorr eexxcceessssiivvee ssttrreessss.. Strains are microscopic, incomplete muscle tears with some bleeding into the tissue. The patient experiences soreness or sudden pain, with local tenderness on muscle use and isometric contraction. SSpprraaiinn-- iinnjjuurryy ttoo tthhee lliiggaammeennttss ssuurrrroouunnddiinngg aa jjooiinntt,, ccaauusseedd bbyy aa wwrreenncchhiinngg oorr ttwwiissttiinngg mmoottiioonn.. The function of the ligament is to maintain stability while permitting mobility. A torn ligament loses its stabilizing ability. TTrreeaattmmeenntt:: ――RRIICCEE‖‖ RReesstt,, IIccee,, CCoommpprreessssiioonn,, EElleevvaattiioonn Nursing interventions o Immobilize the joint, using an elastic bandage or, if sprain is severe, a soft cast. o Control pain and swelling by giving analgesics as prescribed and immediate application of ice for up to 48 hours, followed by application of heat. o Complete muscle rupture may require surgical repair o Moist or dry cold applied intermittently for 20 to 30 minutes during the first 24 to 48 hours after injury produces vasoconstriction, which decreases bleeding, edema, and discomfort. o Care must be taken to avoid skin and tissue damage from excessive cold. o Elevate the joint for 48 to 72 hours after the injury and apply ice intermittently for 24 to 48 hours after the injury o After the acute inflammatory stage (eg, 24 to 40 hours after injury), heat may be applied intermittently (for 15 to 30 minutes, four times a day) to relieve muscle spasm and to promote vasodilation, absorption, and repair. o Depending on the severity of injury progressive passive and active exercise may begin in 2 to 5 days. o Severe sprains may require 1 to 3 weeks of immobilization before protected exercise are initiated.
- 8. o If an elastic bandage is applied, tell the patient to remove the bandage before going to sleep and to loosen it if it causes the leg to become pale, numb or painful. o Consult doctor if pain worsens or persists (X-ray may detect a fracture that was missed originally) FFRRAACCTTUURREE BBrreeaakk iinn tthhee ccoonnttiinnuuiittyy ooff bboonnee Arm and leg fractures can cause substantial muscle, nerve, and other soft-tissue damage. Prognosis varies with the extent of disability or deformity, amount of tissue and vascular damage, adequacy of reduction and immobilization, and the patient’s age, health, and nutrition. Children’s bones usually heal rapidly and without deformity. Bones of adults in poor health and who have impaired circulation may never heal properly. A history of trauma and suggestive findings on physical examination (including gentle palpation and failure of a cautious attempt by the patient to move parts distal to the injury) indicate a likely diagnosis of an arm or leg fracture. Causes o major trauma (fall on an outstretched arm, a skiing accident, or child abuse) o pathologic bone weakening conditions (osteoporosis, bone tumors or metabolic disease) o prolonged standing, walking or running can cause stress fractures of the foot and ankle, usually seen in nurses, postal workers, soldiers and joggers Signs and symptoms o pain and point tenderness o pallor o pulse loss distal to fracture site o paresthesia or paralysis distal to fracture site o deformity
- 9. o swelling o discoloration o crepitus o loss of limb function o substantial blood loss o life threatening hypovolemic shock Diagnostic test o anteroposterior and lateral X-rays o angiography OOBBJJEECCTTIIVVEESS OOFF TTRREEAATTMMEENNTT OOppttiimmaall rreeaalliiggnnmmeenntt RRiiggiidd iimmmmoobbiilliizzaattiioonn RReessttoorraattiioonn ooff ffuunnccttiioonn Treatment o splinting the limb above and below the suspected fracture o applying a cold pack o elevating the limb to reduce edema and pain o severe fractures that cause blood loss: direct pressure should be applied to control bleeding and fluid replacement o reduction, followed by immobilization by splint, cast or traction o Closed reduction: manual manipulation, a local anesthetic and an analgesic are used to minimize pain and a muscle relaxant is used to facilitate muscle stretching to realign the bone. o Open reduction: reduces and immobilizes the fracture by means of rods, plates, or screws. o Skeletal traction: immobilization by the use of weights and pulleys; pin or wire is inserted through the bone distal to the fracture and attached to a weight. o Skin traction: elastic bandages and moleskin coverings are used to attach traction devices to the patient’s skin. o Treatment for open fractures also requires wound cleaning, tetanus prophylaxis, antibiotics, and possibly surgery to repair soft tissue damage Nursing interventions o Monitor for signs of shock o Analgesics as prescribed oo DDiieett:: hhiigghh pprrootteeiinn,, iirroonn,, vviittaammiinnss ((ttiissssuuee rreeppaaiirr)),, mmooddeerraattee ccaarrbboohhyyddrraatteess ((pprreevveenntt wweeiigghhtt ggaaiinn)) o For long-term immobilization with traction, reposition the patient frequently to increase comfort and prevent pressure ulcers o Assist with active range of motion exercises to prevent muscle atrophy o Encourage deep breathing and coughing to avoid hypostatic pneumonia o Monitor the patient for fat embolism, a complication that may occur as bone marrow releases fat into the veins
- 10. o Increase fluid intake to prevent urine stasis and constipations o Provide cast care: While cast is wet, support it with pillows. o Watch for skin irritation near cast edges, and check for foul odors or discharge o Monitor patient for compartment syndrome, watch for increasing pain in the limb; skin color changes, absent pulse, or edema distal to the injury site; decreased active and passive muscle stretching; and sensory changes, such as numbness or tingling (late sign) o Remove any obvious constriction, such as a dressing or wrap, and have the cast cut to relieve pressure if necessary. o If these measures don’t relieve the signs and symptoms in 4 to 6 hours, the doctor may relieve the compression surgically. TTYYPPEESS CCoommpplleettee-- ffrraaccttuurree eexxtteennddss tthhrroouugghh eennttiirree bboonnee,, pprroodduucciinngg 22 oorr mmoorree ffrraaggmmeennttss SSiimmppllee oorr CClloosseedd-- ffrraaccttuurreedd bboonnee ddooeess nnoott pprroottrruuddee tthhrroouugghh sskkiinn CCoommppoouunndd oorr OOppeenn-- ffrraaccttuurreedd bboonnee eexxtteennddss tthhrroouugghh sskkiinn aanndd mmuuccoouuss mmeemmbbrraanneess Open fractures are graded according to the following criteria: Grade I is a clean wound less than 1 cm long Grade II is a larger wound without extensive soft tissue damage. Grade III is highly contaminated, has extensive soft tissue damage, and is the most severe. CCoommmmiinnuutteedd ffrraaccttuurree-- mmuullttiippllee bboonnee ffrraaggmmeennttss OObblliiqquuee ffrraaccttuurree-- ffrraaccttuurree lliinnee aatt 4455--ddeeggrreeee aannggllee ttoo lloonngg aaxxiiss ooff bboonnee SSppiirraall ffrraaccttuurree-- ffrraaccttuurree lliinnee eenncciirrcclliinngg tthhee bboonnee TTrraannssvveerrssee ffrraaccttuurree-- ffrraaccttuurree lliinnee ppeerrppeennddiiccuullaarr ttoo lloonngg aaxxiiss ooff bboonnee EExxttrraaccaappssuullaarr-- ffrraaccttuurree iiss cclloossee ttoo tthhee jjooiinntt bbuutt rreemmaaiinnss oouuttssiiddee tthhee jjooiinntt ccaappssuullee.. IInnttrraaccaappssuullaarr-- ffrraaccttuurree wwiitthhiinn tthhee jjooiinntt ccaappssuullee..
- 11. IInnccoommpplleettee-- wwhheenn oonnllyy ppaarrtt ooff tthhee bboonnee iiss bbrrookkeenn.. GGrreeeennssttiicckk ffrraaccttuurree-- ffrraaccttuurree ooff oonnee ssiiddee ooff bboonnee;; ootthheerr ssiiddee mmeerreellyy bbeennddss;; uussuuaallllyy sseeeenn oonnllyy iinn cchhiillddrreenn BBoowwiinngg ffrraaccttuurree-- bbeennddiinngg ooff bboonnee.. SSttrreessss ffrraaccttuurree-- mmiiccrrooffrraaccttuurree..
- 12. CCOOMMPPLLIICCAATTIIOONN OOFF FFRRAACCTTUURREE SSHHOOCCKK ((EEAARRLLYY)) HHyyppoovvoolleemmiicc oorr ttrraauummaattiicc sshhoocckk rreessuullttiinngg ffrroomm hheemmoorrrrhhaaggee aanndd ffrroomm lloossss ooff eexxttrraacceelllluullaarr fflluuiidd iinnttoo ddaammaaggeedd ttiissssuueess mmaayy ooccccuurr iinn ffrraaccttuurreess ooff tthhee eexxttrreemmiittiieess,, tthhoorraaxx,, ppeellvviiss,, oorr ssppiinnee.. TTrreeaattmmeenntt ooff sshhoocckk ccoonnssiissttss ooff rreessttoorriinngg bblloooodd vvoolluummee aanndd cciirrccuullaattiioonn,, rreelliieevviinngg tthhee ppaattiieenntt’’ss ppaaiinn,, pprroovviiddiinngg aaddeeqquuaattee sspplliinnttiinngg,, aanndd pprrootteeccttiioonn tthhee ppaattiieenntt ffrroomm ffuurrtthheerr iinnjjuurryy aanndd ootthheerr ccoommpplliiccaattiioonnss.. FFAATT EEMMBBOOLLII ((EEAARRLLYY)) After fracture of long bones or pelvis, multiple fractures, or crush injuries, fat emboli may develop. Fat embolism syndrome occurs most frequently in young adults and elderly adults who experience fractures of the proximal femur. At the time of fracture, fat globules may move into the blood because the marrow pressure is greater than the capillary pressure or because catecholamines elevated by the patient’s stress reaction mobilize fatty acids and promote the development of fat globule sin the bloodstream. The fat globules (emboli) occlude the small blood vessels that supply the lungs, brain, kidneys, and other organs. The onset of symptoms is rapid, usually occurring within 24 hours to 72 hours, but may occur up to a week after injury. Clinical Manifestations: hypoxia, tachypnea, tachycardia, and pyrexia. The respiratory distress response includes tachypnea, Dyspnea, crackles, wheezes, precordial chest pain, cough, large amounts of thick white sputum, and tachycardia. The chest x-ray shows a typical ―snowstorm‖ infiltrate. Eventually, acute pulmonary edema, acute respiratory distress syndrome, and heart failure develop. Cerebral disturbances (due to hypoxia and the lodging of fat emboli in the brain) are manifested by mental status changes varying from headache, mild agitation, and confusion t delirium and coma.
- 13. Prevention and Management Immediate immobilization of fractures, minimal fracture manipulation, adequate support for fractured bones during turning and positioning, and maintenance of fluid and electrolyte balance are measures that may reduce the incidence of emboli. Support the respiratory system, to prevent respiratory and metabolic acidosis, and to correct homeostatic disturbances. Respiratory failure is the most common cause of death. Respiratory support is provided with oxygen given in high concentration. Controlled-volume ventilation with positive end-expiratory pressure may be used to prevent or treat pulmonary edema. Corticosteroids may be administered to treat the inflammatory lung reaction and to control cerebral edema. Vasoactive medications to support cardiovascular function are administered to prevent hypotension, shock, and interstitial pulmonary edema. Accurate fluid intake and output records facilitate adequate fluid replacement therapy. Morphine may be prescribed for pain and anxiety for the patient who is on a ventilator. CCOOMMPPAARRTTMMEENNTT SSYYNNDDRROOMMEE ((EEAARRLLYY)) A complication that develops when tissue perfusion on the muscles is less than that required for tissue viability. The patient complains of deep, throbbing, unrelenting pain, which is not controlled by opioids. This pain can be caused by (1) reduction in the size of the muscle compartment because the enclosing muscle fascia is too tight or a cast or dressing is constrictive, or (2) an increase in muscle compartment contents because of edema or hemorrhage associated with a variety or problems. The forearm and leg muscle compartments are involved most frequently.
- 14. Clinical Manifestation: sensory deficits include paresthesia, unrelenting pain, and hypoesthesia. Paresthesia and numbness along the involved nerve are early signs of nerve involvement. Peripheral circulation is evaluated by assessing color, temperature, capillary refill time, swelling, and pulses. Swelling (edema) reduces tissue perfusion. Cyanotic (blue-tinged) nail beds suggest venous congestion. Pale or dusky and cold finger or toes and prolonged capillary refill time suggest diminished arterial perfusion. Edema may obscure the present of arterial pulsation and Doppler ultraonography may be used to verify a pulse. Deep, throbbing, unrelenting pain, which is greater than expected and not controlled by opioids. Medical Management Elevation of the extremity to the heart level, release of restrictive devices (dressing or cast), or both. If conservative measures do not restore tissue perfusion and relieve pain within 1 hour, a fasciotomy (surgical decompression with excision of the fibrous membrane that covers and separates muscles) may be needed to relieve the constrictive muscle fascia. After fasciotomy, the wound is not sutured but instead is left open to permit the muscle tissues to expand; it is covered with moist, sterile saline dressing. The limb is splinted in a functional position and elevated, and prescribed passive ROM exercises are usually performed every 4 to 6 hours. In 3 to 5 days, when the swelling has resolved and tissue perfusion has been restored, the wound is debrided and closed (possibly with skin graft). Fasciotomy
- 15. OOTTHHEERR EEAARRLLYY CCOOMMPPLLIICCAATTIIOONNSS Deep vein thrombosis (DVT), thromboembolism, and pulmonary embolus (PE) are associated with reduced skeletal muscle contractions and bed rest. Patient with fractures of the lower extremities and pelvis are at high risk for thromboembolism. Pulmonary emboli may cause death several days to weeks after injury. DIC includes a group of bleeding disorders with diverse causes, including massive tissue trauma. Manifestations of DIC include ecchymosis, unexpected bleeding after surgery, and bleeding from the mucous membranes, venipuncture sites, and gastrointestinal and urinary tracts. All open fractures are considered contaminated. Surgical internal fixation of fractures carries a risk for infection. The nurse must monitory for and teach the patient to monitor for signs of infections, including tenderness, pain, redness, swelling, local warmth, elevated temperature, and purulent drainage. Infections must be treated promptly. Antibiotic therapy must be appropriate and adequate for prevention and treatment of infection. AAVVAASSCCUULLAARR NNEECCRROOSSIISS ((DDEELLAAYYEEDD)) Avascular necrosis occurs when the bone loses its blood supply and dies. It may occur after a fracture with disruption of the blood supply (especially of the femoral neck). It is also seen with dislocations, bone transplantation, prolonged high-dosage corticosteroid therapy, chronic renal disease, sickle cell anemia, and other diseases. The devitalized bone may collapse or reabsorb. The patient develops pain and experiences limited movement. X-rays reveal calcium loss and structural collapse. Treatment generally consists of attempts to revitalize the bone with bone grafts, prosthetic replacement, or arthrodesis (joint fusion). REDUCTION Reduction of a fracture (―setting‖ the bone) refers to restoration of the fracture fragments to anatomic alignment and rotation. Closed Reduction Accomplished by bringing the bone fragments into apposition (ie, placing the ends in contact) through manipulation and manual traction.
- 16. The extremity is held in the desired position while the physician applies a cast, splint, or other device. The immobilizing device maintains the reduction and stabilizes the extremity for bone healing. X-rays are obtained to verify that the bone fragments are correctly aligned. Open Reduction Through a surgical approach, the fracture fragments are reduced. Internal fixation devices (metallic pins, wires, screws, plates, nails, or rods) may be used to hold the bone fragments in position until solid bone healing occurs. These devices may be attached to the sides of bone, or they may be inserted through the bony fragments or directly into the medullary cavity of the bone. Internal fixation devices ensure firm approximation and fixation of the bony fragments. Internal and External Fixation Devices
- 17. TRACTION oo MMeecchhaanniissmm bbyy wwhhiicchh aa sstteeaaddyy ppuullll iiss ppllaacceedd oonn aa ppaarrtt oorr ppaarrttss ooff tthhee bbooddyy PRINCIPLES FOR EFFECTIVE TRACTION o Whenever traction is applied, countertraction must be used to achieve effective traction. Countertraction is the force acting in the opposite direction. Usually the patient’s body weight and bed position adjustments supply the needed countertraction. o Traction must be continuous to be effective in reducing and immobilizing fractures. o Skeletal traction is never interrupted. o Weights are not removed unless intermittent traction is prescribed. o Any factor that might reduce the effective pull or alter the resultant line of pull must be eliminated: - The patient must be in good body alignment in the center of the bed when traction is applied. - Ropes must be unobstructed. - Weights must hang free and not rest on the bed or floor. - Knots in the rope or the footplate must not touch the pulley or the foot of the bed. SKIN TRACTION -- AApppplliiccaattiioonn ooff wwiiddee bbaanndd ooff mmoolleesskkiinn,, aaddhheessiivvee,, oorr ccoommmmeerrcciiaallllyy aavvaaiillaabbllee ddeevviicceess ddiirreeccttllyy ttoo tthhee sskkiinn aanndd aattttaacchhiinngg wweeiigghhttss ttoo tthheemm.. - Used to control muscle spasms and to immobilize an area before surgery. - It is accomplished by using a weight to pull on traction tape or on a foam boot attached to the skin. The amount of weight applied must not exceed the tolerance of the skin. - No more than 2 to 3.5 kg (4.5 to 8 lb) of traction can be used on an extremity. Pelvic traction is usually 4.5 to 9 kg (10 to 20 lb), depending on the weight of the patient. BBuucckk’’ss eexxtteennssiioonn A skin traction to the lower leg. The pull is exerted in one plane when partial or temporary immobilization if desired. It is used to provide immobility after fractures of the proximal femur before surgical fixation. RReelliieevvee mmuussccllee ssppaassmm
- 18. HHeeeell iiss ssuuppppoorrtteedd ooffff bbeedd ttoo pprreevveenntt pprreessssuurree oonn hheeeell,, wweeiigghhtt hhaannggss ffrreeee ooff tthhee bbeedd,, aanndd ffoooott iiss wweellll aawwaayy ffrroomm ffoooottbbooaarrdd ooff bbeedd,, aanndd ppaarraalllleell ttoo tthhee bbeedd.. RRuusssseell ttrraaccttiioonn UUsseedd iinn tthhee ttrreeaattmmeenntt ooff iinntteerrttrroocchhaanntteerriicc ffrraaccttuurree ooff tthhee ffeemmuurr wwhheenn ssuurrggeerryy iiss ccoonnttrraaiinnddiiccaatteedd HHiipp iiss sslliigghhttllyy fflleexxeedd.. PPiilllloowwss mmaayy bbee uusseedd uunnddeerr lloowweerr lleegg ttoo pprroovviiddee ssuuppppoorrtt aanndd kkeeeepp tthhee hheeeell ffrreeee ooff tthhee bbeedd.. BBrryyaanntt’’ss ttrraaccttiioonn-- uusseedd ttoo rreedduuccee ffeemmoorraall ffrraaccttuurree iinn cchhiillddrreenn.. BBuuttttoocckkss aarree sslliigghhttllyy eelleevvaatteedd aanndd cclleeaarr ooffff tthhee bbeedd..
- 19. Nursing considerations Check periodically to ensure that weights, ropes, and pulleys are in proper alignment and functional. Don’t manipulate the weights yourself; consult the doctor if you suspect the need for any adjustment. Avoid wrinkling and slipping of the traction bandage and to maintain countertraction. POTENTIAL COMPLICATIONS Skin breakdown Remove the foam boots to inspect the skin, th ankle, and the Achilles tendon three times a day. A second nurse is needed to support the extremity during the inspection and skin care. Palpate the area of the traction tapes daily to detect underlying tenderness. Provide back care at least every 2 hours to prevent pressure ulcers. Use special mattress overlays (eg, air-filled, high-density foam) to minimize the development of skin ulcers. Nerve pressure Regularly assess sensation and motion. Immediately investigate any complaint of burning sensation under the traction bandage or boot. Promptly report altered sensation or motor function. Circulatory impairment Peripheral pulses, color, capillary refill, and temperature of the fingers of toes. Indicators of DVT, including calf tenderness, swelling, and positive Homans’sign. SSKKEELLEETTAALL TTRRAACCTTIIOONN - Placement of a pin through the bone, to which the traction apparatus is attached - Common types include: Gardner-Wells and Crutchfield tongs; halo vest; pin placement through the femur, lower tibia, calcaneus, ulna, radius, or wrists; Kirschner wire; and Steinmann pin Purpose: to immobilize bones and allow healing of fractures, correction of congenital abnormalities, or stabilization of spinal degeneration. TTrraaccttiioonn aapppplliieedd ddiirreeccttllyy ttoo bboonnee..
- 20. NNuurrssiinngg ccoonnssiiddeerraattiioonnss o Perform pin care daily with water and normal saline solution or hydrogen peroxide o Observe the pin insertion site for signs of infection o Check the pin for proper fit, making sure that it doesn’t move in the bone o Teach the patient how to use the trapeze to lift himself off the bed, if permitted o If cervical traction is being used, check the occipital area of the head for skin breakdown. o When caring for a patient in a halo vest, bathe under the vest daily. CCRRUUTTCCHH WWAALLKKIINNGG TThhee ddiissttaannccee bbeettwweeeenn tthhee aaxxiillllaa aanndd tthhee aarrmm ppiieeccee oonn tthhee ccrruuttcchheess sshhoouulldd bbee aatt lleeaasstt 33 ffiinnggeerrwwiiddtthhss bbeellooww tthhee aaxxiillllaa TThhee eellbboowwss sshhoouulldd bbee sslliigghhttllyy fflleexxeedd,, 3300 ddeeggrreeeess WWhheenn aammbbuullaattiinngg wwiitthh tthhee cclliieenntt,, ssttaanndd oonn tthhee aaffffeecctteedd ssiiddee.. CCrruuttcchh ssttaannccee:: ttrriippoodd ((ttrriiaannggllee)) ppoossiittiioonn.. IInnssttrruucctt tthhee cclliieenntt nneevveerr ttoo rreesstt tthhee aaxxiillllaa oonn tthhee aaxxiillllaarryy bbaarrss.. IInnssttrruucctt tthhee cclliieenntt ttoo llooookk uupp aanndd oouuttwwaarrdd wwhheenn aammbbuullaattiinngg.. IInnssttrruucctt tthhee cclliieenntt ttoo ssttoopp aammbbuullaattiioonn iiff nnuummbbnneessss oorr ttiinngglliinngg iinn tthhee hhaannddss oorr aarrmmss ooccccuurrss..
- 21. CCrruuttcchh ggaaiittss FFoouurr--ppooiinntt ggaaiitt SSeeqquueennccee:: AAddvvaannccee lleefftt ccrruuttcchh 44--66 iinncchheess AAddvvaannccee rriigghhtt ffoooott AAddvvaannccee rriigghhtt ccrruuttcchh AAddvvaannccee lleefftt ffoooott AAddvvaannttaaggeess:: mmoosstt ssttaabbllee ccrruuttcchh ggaaiitt RReeqquuiirreemmeennttss:: WWeeiigghhtt bbeeaarriinngg iiss ppeerrmmiitttteedd oonn bbootthh lleeggss TThhrreeee--ppooiinntt ggaaiitt SSeeqquueennccee:: AAddvvaannccee bbootthh ccrruuttcchheess ffoorrwwaarrdd wwiitthh tthhee aaffffeecctteedd lleegg aanndd sshhiifftt wweeiigghhtt ttoo ccrruuttcchheess.. AAddvvaannccee uunnaaffffeecctteedd lleegg aanndd sshhiifftt wweeiigghhtt oonnttoo iitt.. AAddvvaannttaaggeess:: aalllloowwss tthhee aaffffeecctteedd lleegg ttoo bbee ppaarrttiiaallllyy oorr ccoommpplleetteellyy ffrreeee ooff wweeiigghhtt bbeeaarriinngg RReeqquuiirreemmeennttss:: FFuullll wweeiigghhtt bbeeaarriinngg oonn oonnee lleegg.. TThhee ootthheerr ffoooott ccaannnnoott ssuuppppoorrtt bbuutt mmaayy aacctt aass aa bbaallaannccee.. TTwwoo--ppooiinntt ggaaiitt SSeeqquueennccee:: AAddvvaannccee lleefftt ccrruuttcchh aanndd rriigghhtt ffoooott AAddvvaannccee rriigghhtt ccrruuttcchh aanndd lleefftt ffoooott AAddvvaannttaaggeess:: FFaasstteerr vveerrssiioonn ooff tthhee ffoouurr--ppooiinntt,, mmoorree nnoorrmmaall wwaallkkiinngg ppaatttteerrnn.. RReeqquuiirreemmeennttss:: PPaarrttiiaall wweeiigghhtt bbeeaarriinngg oonn bbootthh lleeggss SSwwiinngg--tthhrroouugghh ggaaiitt SSeeqquueennccee:: UUnnaaffffeecctteedd ffoooott bbeeaarrss wweeiigghhtt MMoovvee bbootthh ccrruuttcchheess ffoorrwwaarrdd.. MMoovvee bbootthh lleeggss ffaarrtthheerr aahheeaadd tthhaann ccrruuttcchheess.. WWeeiigghhtt bbeeaarriinngg rreettuurrnnss ttoo tthhee uunnaaffffeecctteedd lleegg RReeqquuiirreemmeennttss:: wweeiigghhtt--bbeeaarriinngg iiss ppeerrmmiitttteedd oonn oonnllyy oonnee ffoooott AAMMPPUUTTAATTIIOONN OOFF TTHHEE LLOOWWEERR EEXXTTRREEMMIITTYY RReemmoovvaall ooff aa bbooddyy ppaarrtt,, uussuuaallllyy aann eexxttrreemmiittyy Amputation is performed at the most distal point that will heal successfully. The site of amputation is determined by two factors: circulation in the part, and functional usefulness. Amputee may experience phantom limb pain soon after surgery or 2 to 3 months after amputation. It occurs more frequently in above-knee amputations.
- 22. The patient describes pain or unusual sensation, such as numbness, tingling, or muscle cramps, as well as a feeling that the extremity is present, crushed, cramped or twisted in an abnormal position. When a patient describes phantom pains or sensations, the nurse acknowledges these feelings and helps the patient modify these perceptions. Phantom limb sensation diminish over time RRiisskk FFaaccttoorrss AAtthheerroosscclleerroossiiss oobblliitteerraannss UUnnccoonnttrroolllleedd DDMM MMaalliiggnnaannccyy EExxtteennssiivvee aanndd iinnttrraaccttaabbllee iinnffeeccttiioonn SSeevveerree ttrraauummaa CCoommpplliiccaattiioonnss ooff AAmmppuuttaattiioonn IInnffeeccttiioonn WWoouunndd nneeccrroossiiss PPhhaannttoomm lliimmbb ppaaiinn CCoonnttrraaccttuurreess SSkkiinn bbrreeaakkddoowwnn
- 23. NNuurrssiinngg IInntteerrvveennttiioonn AAsssseessss ssttuummpp aanndd mmoonniittoorr ccaatthheetteerr ddrraaiinnaaggee ffoorr ccoolloorr aanndd aammoouunntt;; rreeppoorrtt ssiiggnnss ooff iinnccrreeaasseedd ddrraaiinnaaggee BKA: keep knee extended to avoid hamstring contracture IIff pprreessccrriibbeedd,, dduurriinngg tthhee ffiirrsstt 2244 hhoouurrss,, eelleevvaattee tthhee ffoooott ooff tthhee bbeedd ttoo rreedduuccee eeddeemmaa;; tthheenn kkeeeepp tthhee bbeedd ffllaatt ttoo pprreevveenntt hhiipp fflleexxiioonn ccoonnttrraaccttuurreess DDoo nnoott eelleevvaattee tthhee ssttuummpp iittsseellff——eelleevvaattiioonn ccaann ccaauussee fflleexxiioonn ccoonnttrraaccttuurree ooff tthhee hhiipp jjooiinntt.. AAfftteerr 2244 aanndd 4488 hhoouurrss ppoossttooppeerraattiivveellyy,, ppoossiittiioonn tthhee cclliieenntt pprroonnee iiff pprreessccrriibbeedd,, ttoo ssttrreettcchh tthhee mmuusscclleess aanndd pprreevveenntt fflleexxiioonn ccoonnttrraaccttuurreess ooff hhiipp TToo pprreevveenntt lleegg aabbdduuccttiioonn,, kkeeeepp lleeggss cclloossee ttooggeetthheerr EEnnccoouurraaggee eexxeerrcciisseess ttoo pprreevveenntt tthhrroommbbooeemmbboolliissmm EEnnccoouurraaggee ppaattiieenntt ttoo aammbbuullaattee uussiinngg ccoorrrreecctt ccrruuttcchh--wwaallkkiinngg tteecchhnniiqquueess Teach patient triceps strengthening exercises for crutch walking, such as pushups and flexion and extension of the arms using traction weights. Instruct the patient to rub the stump with alcohol daily to toughen the skin Avoid applying powder or lotion Massage the stump toward the suture line to mobilize the scar and prevent its adherence to bone To prepare the stump for prosthesis, teach progressive resistance maneuvers. Stress the importance of performing prescribed exercises to help minimize complications, maintain muscle strength and tone, prevent contractures, and promote independence. IINNFFLLAAMMMMAATTOORRYY DDIISSOORRDDEERRSS OOFF TTHHEE MMUUSSCCUULLOOSSKKEELLEETTAALL SSYYSSTTEEMM RRHHEEUUMMAATTOOIIDD AARRTTHHRRIITTIISS CChhrroonniicc ssyysstteemmiicc iinnffllaammmmaattoorryy ddiisseeaassee DDeessttrruuccttiioonn ooff ccoonnnneeccttiivvee ttiissssuuee aanndd ssyynnoovviiaall mmeemmbbrraannee wwiitthhiinn tthhee jjooiinnttss WWeeaakkeennss aanndd lleeaaddss ttoo ddiissllooccaattiioonn ooff tthhee jjooiinntt aanndd ppeerrmmaanneenntt ddeeffoorrmmiittyy Spontaneous remissions and exacerbations mark the course of RA.
- 24. RRiisskk FFaaccttoorrss:: EExxppoossuurree ttoo iinnffeeccttiioouuss aaggeennttss FFaattiigguuee SSttrreessss SSiiggnnss aanndd SSyymmppttoommss IInniittiiaall ssyymmppttoommss:: ffaattiigguuee,, mmaallaaiissee,, aannoorreexxiiaa,, ppeerrssiisstteenntt llooww ggrraaddee ffeevveerr,, wweeiigghhtt lloossss,, aanndd llyymmppaaddeennooppaatthhyy joint pain, tenderness, warmth, and swelling joint symptoms occur bilaterally and symmetrically MMoorrnniinngg ssttiiffffnneessss SSwwaann nneecckk ddeeffoorrmmiittyy--llaattee DDiiaaggnnoossttiicc SSttuuddiieess XX--rraayy,, sshhooww bboonnee ddeemmiinneerraalliizzaattiioonn aanndd ssoofftt ttiissssuuee sswweelllliinngg EElleevvaatteedd EESSRR,, aanndd ppoossiittiivvee RRFF TTrreeaattmmeenntt Salicylates, to decrease inflammation and relieve joint pain. NNSSAAIIDDss ((iinnddoommeetthhaacciinn,, kkeettoorroollaacc,, iibbuupprrooffeenn,, CCooxx--22 IInnhhiibbiittoorrss ((CCeelleeccooxxiibb,, RRooffeeccooxxiibb)) oo IInnhhiibbiittss oonnllyy ccyyccllooooxxyyggeennaassee--22 eennzzyymmeess Antimalarials (chloroquine and hydroxychloroquine) Gold sodium thiomalate penicilamine Corticosteroids Immunosuppressives (methotrexate, cyclophosphamide, azathioprine) HHoott aanndd CCoolldd ppaacckkss ttoo aaffffeecctteedd jjooiinnttss SSuurrggiiccaall PPrroocceedduurreess:: ssyynnoovveeccttoommyy,, aarrtthhrroottoommyy,, aarrtthhrrooddeessiiss,, aarrtthhrrooppllaassttyy SSuuppppoorrttiivvee mmeeaassuurreess iinncclluuddee:: 88 ttoo 1100 hhoouurrss ooff sslleeeepp eevveerryy nniigghhtt,, aaddeeqquuaattee nnuuttrriittiioonn,, ffrreeqquueenntt rreesstt ppeerriiooddss bbeettwweeeenn ddaaiillyy aaccttiivviittiieess,, aanndd sspplliinnttiinngg ttoo rreesstt iinnffllaammeedd jjooiinnttss.. Swan neck deformity
- 25. NNuurrssiinngg MMaannaaggeemmeenntt Assess all joints carefully Monitor vital signs and note weight changes, sensory disturbances, and level of pain. Give meticulous skin care. Use lotion or cleansing oil, not soap, for dry skin Apply splints carefully Encourage a balanced diet. Urge the patient to perform activities of daily living BBeedd rreesstt DDaaiillyy RROOMM eexxeerrcciisseess RReelliieevviinngg ppaaiinn aanndd ddiissccoommffoorrtt AAddmmiinniisstteerr ddrruuggss aass pprreessccrriibbeedd aanndd mmoonniittoorr eeffffeeccttss NNuurrssiinngg DDiiaaggnnoossiiss PPaaiinn rreellaatteedd ttoo jjooiinntt ddeessttrruuccttiioonn IImmppaaiirreedd pphhyyssiiccaall mmoobbiilliittyy rreellaatteedd ttoo jjooiinntt ccoonnttrraaccttuurreess RRiisskk ffoorr iinnjjuurryy rreellaatteedd ttoo tthhee iinnffllaammmmaattoorryy pprroocceessss BBooddyy iimmaaggee ddiissttuurrbbaannccee rreellaatteedd ttoo jjooiinntt ddeeffoorrmmiittyy SSeellff--ccaarree ddeeffiicciitt rreellaatteedd ttoo mmuussccuulloosskkeelleettaall iimmppaaiirrmmeenntt OOSSTTEEOOAARRTTHHRRIITTIISS ((DDEEGGEENNEERRAATTIIVVEE JJOOIINNTT DDIISSEEAASSEE)) PPrrooggrreessssiivvee ddeeggeenneerraattiioonn ooff tthhee jjooiinnttss aass aa rreessuulltt ooff wweeaarr aanndd tteeaarr AAffffeeccttss wweeiigghhtt--bbeeaarriinngg jjooiinnttss aanndd jjooiinnttss tthhaatt rreecceeiivvee tthhee ggrreeaatteesstt ssttrreessss,, ssuucchh aass tthhee hhiippss aanndd kknneeeess
- 26. RRiisskk FFaaccttoorrss AAggiinngg ((>>5500 yyrr)) RRhheeuummaattooiidd aarrtthhrriittiiss AArrtteerriioosscclleerroossiiss OObbeessiittyy TTrraauummaa FFaammiillyy hhiissttoorryy SSiiggnnss aanndd SSyymmppttoommss ppaaiinn,, tteennddeerr jjooiinnttss,, ppaarrttiiccuullaarrllyy aafftteerr eexxeerrcciissee oorr wweeiigghhtt bbeeaarriinngg aanndd iiss uussuuaallllyy rreelliieevveedd bbyy rreesstt stiffness in the morning and after exercise that is usually relieved by rest achiness during changes in weather, cold intolerance ffaattiiggaabbiilliittyy,, mmaallaaiissee ccrreeppiittuuss pprreesseennccee ooff HHeebbeerrddeenn’’ss nnooddeess oorr BBoouucchhaarrdd’’ss nnooddeess lliimmiitteedd mmoovveemmeenntt Diagnostic tests X-rays of the affected joint help confirm diagnosis Treatment Palliative treatment Medications include: aspirin (or other nonnarcotic analgesics), phenylbutazone, indomethacin, ketorolac, ibuprofen, propoxyphene hydrochloride, rofecoxib, and in some cases, intra-articular injections of corticosteroid AAssppiirriinn IInnhhiibbiittss ccyyccllooooxxyyggeennaassee eennzzyymmee,, ddiimmiinniisshheess tthhee ffoorrmmaattiioonn ooff pprroossttaaggllaannddiinnss AAnnttii--iinnffllaammmmaattoorryy,, aannaallggeessiicc,, aannttiippyyrreettiicc aaccttiioonn IInnhhiibbiitt ppllaatteelleett aaggggrreeggaattiioonn iinn ccaarrddiiaacc ddiissoorrddeerrss
- 27. AAddvveerrssee eeffffeeccttss:: EEppiiggaassttrriicc ddiissttrreessss,, nnaauusseeaa,, aanndd vvoommiittiinngg IInn ttooxxiicc ddoosseess,, ccaann ccaauussee rreessppiirraattoorryy ddeepprreessssiioonn HHyyppeerrsseennssiittiivviittyy RReeyyee’’ss ssyynnddrroommee IIbbuupprrooffeenn UUssee ffoorr cchhrroonniicc ttrreeaattmmeenntt ooff rrhheeuummaattooiidd aanndd oosstteeooaarrtthhrriittiiss LLeessss GGII eeffffeeccttss tthhaann aassppiirriinn AAddvveerrssee eeffffeeccttss:: DDyyssppeeppssiiaa ttoo bblleeeeddiinngg HHeeaaddaacchhee,, ttiinnnniittuuss aanndd ddiizzzziinneessss IInnddoommeetthhaacciinn IInnhhiibbiittss ccyyccllooooxxyyggeennaassee eennzzyymmee MMoorree ppootteenntt tthhaann aassppiirriinn aass aann aannttii--iinnffllaammmmaattoorryy aaggeenntt AAddvveerrssee eeffffeeccttss:: TThhee aaddvveerrssee eeffffeeccttss aarree ddoossee--rreellaatteedd.. NNaauusseeaa,, vvoommiittiinngg,, aannoorreexxiiaa,, ddiiaarrrrhheeaa HHeeaaddaacchhee,, ddiizzzziinneessss,, vveerrttiiggoo,, lliigghhtt--hheeaaddeeddnneessss,, aanndd mmeennttaall ccoonnffuussiioonn HHyyppeerrsseennssiittiivviittyy rreeaaccttiioonn Effective treatment also reduces joint stress by supporting or stabilizing the joint with crutches, braces, a cane, a walker, a cervical collar, or traction. Other supportive measures include massage, moist heat, paraffin dips for hands, protective techniques for preventing undue stress on the joints Those with severe osteoarthritis with disability or uncontrollable pain may undergo: arthroplasty- replacement of a deteriorated joint with a prosthetic appliance arthrodesis- surgical fusion of bones, which is used primarily in the spine (laminectomy) osteoplasty- scraping of deteriorated bone from a joint osteotomy- excision of bone to change alignment and relieve stress NNuurrssiinngg IInntteerrvveennttiioonn PPrroommoottee ccoommffoorrtt:: rreedduuccee ppaaiinn,, ssppaassmmss,, iinnffllaammmmaattiioonn,, sswweelllliinngg MMeeddiiccaattiioonnss aass pprreessccrriibbeedd.. HHeeaatt ttoo rreedduuccee mmuussccllee ssppaassmm CCoolldd ttoo rreedduuccee sswweelllliinngg aanndd ppaaiinn
- 28. PPrreevveenntt ccoonnttrraaccttuurreess:: eexxeerrcciissee,, bbeedd rreesstt oonn ffiirrmm mmaattttrreessss,, sspplliinnttss ttoo mmaaiinnttaaiinn pprrooppeerr aalliiggnnmmeenntt WWeeiigghhtt rreedduuccttiioonn IIssoommeettrriicc aanndd ppoossttuurraall eexxeerrcciisseess Firm mattress or bed board to decrease morning pain Assist with ROM and strengthening exercises Instruct patients to wear well-fitting supportive shoes, install safety devices at home, maintain proper body weight to lessen joint stress, avoid overexertion. NNuurrssiinngg DDiiaaggnnoossiiss PPaaiinn rreellaatteedd ttoo ffrriiccttiioonn ooff bboonneess iinn jjooiinnttss RRiisskk ffoorr iinnjjuurryy rreellaatteedd ttoo ffaattiigguuee IImmppaaiirreedd pphhyyssiiccaall mmoobbiilliittyy rreellaatteedd ttoo ssttiiffff,, lliimmiitteedd mmoovveemmeenntt GGOOUUTTYY AARRTTHHRRIITTIISS MMeettaabboolliicc ddiissoorrddeerr tthhaatt ddeevveellooppss aass aa rreessuulltt ooff pprroolloonnggeedd hhyyppeerruurriicceemmiiaa ccaauusseedd bbyy pprroobblleemmss iinn ssyynntthheessiizziinngg ppuurriinneess oorr bbyy ppoooorr rreennaall eexxccrreettiioonn ooff uurriicc aacciidd.. aaccuuttee oonnsseett,, ttyyppiiccaallllyy nnooccttuurrnnaall aanndd uussuuaallllyy mmoonnaarrttiiccuullaarr,, oofftteenn iinnvvoollvviinngg tthhee ffiirrsstt mmeettaattaarrssoopphhaallaannggeeaall jjooiinntt RRiisskk FFaaccttoorrss MMeenn AAggee 3300 oorr oollddeerr aanndd iinn ppoossttmmeennooppaauussaall wwoommeenn GGeenneettiicc//ffaammiilliiaall tteennddeennccyy Causes Unknown Linked to a genetic defect in purine metabolism, which causes overproduction of uric acid, retention of uric acid, or both. Secondary gout, which develops during the course of another disease (such as obesity, DM, HPN, sickle cell anemia, renal disease, myeloma, leukemia)
- 29. Following drug therapy, hydrochlorothiazide or pyrazinamide, which interferes with urate excretion SSiiggnnss aanndd SSyymmppttoommss AAffffeecctteedd jjooiinnttss aappppeeaarr hhoott,, tteennddeerr,, iinnffllaammeedd,, dduusskkyy rreedd,, oorr ccyyaannoottiicc Metatarsophalangeal joint of the great toe usually becomes inflamed first (podagra), then the instep, ankle, heel, knee or wrist joints EExxttrreemmeellyy ppaaiinnffuull FFeevveerr IInnccrreeaasseedd ccoonncceennttrraattiioonn ooff uurriicc aacciidd lleeaaddss ttoo uurraattee ddeeppoossiittss,, ccaalllleedd TToopphhii Diagnostic tests ((++)) uurraattee mmoonnoohhyyddrraattee ccrryyssttaallss iinn ssyynnoovviiaall fflluuiidd ttaakkeenn ffrroomm aann iinnffllaammeedd jjooiinntt oorr ttoopphhuuss aassppiirraattiioonn ooff ssyynnoovviiaall fflluuiidd ((aarrtthhrroocceenntteessiiss)) oorr ooff ttoopphhaacceeoouuss mmaatteerriiaall rreevveeaallss nneeeeddlleelliikkee iinnttrraacceelllluullaarr ccrryyssttaallss ooff ssooddiiuumm uurraattee EElleevvaatteedd sseerruumm uurriicc aacciidd EElleevvaatteedd uurriinnaarryy uurriicc aacciidd eessppeecciiaallllyy iinn sseeccoonnddaarryy uurriicc aacciidd lleevveellss IInn cchhrroonniicc ggoouutt,, XX--rraayyss sshhooww aa ppuunncchheedd--oouutt llooookk wwhheenn uurraattee aacciiddss rreeppllaaccee bboonnyy ssttrruuccttuurreess TTrreeaattmmeenntt AAllllooppuurriinnooll oo AA ppuurriinnee aannaalloogg oo RReedduucceess tthhee pprroodduuccttiioonn ooff uurriicc aacciidd bbyy ccoommppeettiittiivveellyy iinnhhiibbiittiinngg uurriicc aacciidd bbiioossyynntthheessiiss wwhhiicchh iiss ccaattaallyyzzeedd bbyy xxaanntthhiinnee ooxxiiddaassee.. EEffffeeccttiivvee iinn tthhee ttrreeaattmmeenntt ooff pprriimmaarryy hhyyppeerruurriicceemmiiaa ooff ggoouutt aanndd hhyyppeerruurriicceemmiiaa sseeccoonnddaarryy ttoo ootthheerr ccoonnddiittiioonnss ((mmaalliiggnnaanncciieess)).. AAddvveerrssee eeffffeeccttss:: hhyyppeerrsseennssiittiivviittyy rreeaaccttiioonnss,, nnaauusseeaa aanndd ddiiaarrrrhheeaa CCoollcchhiicciinnee EEffffeeccttiivvee ffoorr aaccuuttee aattttaacckkss Taken every hour for 8 hours, until pain subsides or until signs of overdose such as nausea, vomiting, cramping or diarrhea develop AAnnttii--iinnffllaammmmaattoorryy aaccttiivviittyy aalllleevviiaattiinngg ppaaiinn wwiitthhiinn 1122 hhoouurrss AAddvveerrssee eeffffeeccttss:: nnaauusseeaa,, vvoommiittiinngg,, aabbddoommiinnaall ppaaiinn,, ddiiaarrrrhheeaa,, aaggrraannuullooccyyttoossiiss,, aappllaassttiicc aanneemmiiaa,, aallooppeecciiaa PPrroobbeenneecciidd//SSuullffiinnppyyrraazzoonnee UUrriiccoossuurriicc aaggeennttss IInnccrreeaasseess tthhee rreennaall eexxccrreettiioonn ooff uurriicc aacciidd aanndd iinnhhiibbiitt aaccccuummuullaattiioonn ooff uurriicc aacciidd SSuullffiinnppyyrraazzoonnee uusseedd aass aa pprreevveennttiivvee aaggeenntt.. AAddvveerrssee eeffffeeccttss:: nnaauusseeaa,, rraasshh && ccoonnssttiippaattiioonn Don’t administer these drugs to patient with calculi
- 30. Corticosteroids or joint aspiration and an intra-articular corticosteroid injection For resistant inflammation Analgesics, such as acetaminophen or ibuprofen Relieve pain associated with mild attacks NNuurrssiinngg IInntteerrvveennttiioonnss BBeedd rreesstt,, iimmmmoobbiilliizzaattiioonn,, aanndd pprrootteeccttiioonn ooff iinnffllaammeedd,, ppaaiinnffuull jjooiinnttss;; llooccaall aapppplliiccaattiioonn ooff hheeaatt oorr ccoolldd.. MMaaiinnttaaiinn aa fflluuiidd iinnttaakkee ooff aatt lleeaasstt 22000000 ttoo 33000000 mmLL aa ddaayy ttoo aavvooiidd kkiiddnneeyy ssttoonnee.. AAvvooiidd ffooooddss hhiigghh iinn ppuurriinnee ssuucchh aass wwiinnee,, aallccoohhooll,, oorrggaann mmeeaattss,, ssaarrddiinneess,, ssaallmmoonn,, aanncchhoovviieess,, sshheellllffiisshh aanndd ggrraavvyy.. TTaakkee mmeeddiiccaattiioonn wwiitthh ffoooodd.. HHaavvee aa yyeeaarrllyy eeyyee eexxaammiinnaattiioonn bbeeccaauussee vviissuuaall cchhaannggeess ccaann ooccccuurr ffrroomm pprroolloonnggeedd uussee ooff aallllooppuurriinnooll CCaauuttiioonn cclliieenntt nnoott ttoo ttaakkee aassppiirriinn wwiitthh tthheessee mmeeddiiccaattiioonn bbeeccaauussee iitt mmaayy ttrriiggggeerr aa ggoouutt aattttaacckk aanndd mmaayy ccaauussee aann eelleevvaatteedd uurriicc aacciidd lleevveellss.. EEnnccoouurraaggee rreesstt aanndd iimmmmoobbiilliizzee tthhee iinnffllaammeedd jjooiinnttss dduurriinngg aaccuuttee aattttaacckkss AAvvooiidd eexxcceessssiivvee aallccoohhooll iinnttaakkee NNoottiiffyy pphhyyssiicciiaann iiff rraasshh,, ssoorree tthhrrooaatt,, ffeevveerr oorr bblleeeeddiinngg ddeevveellooppss.. Nursing Diagnosis Chronic pain Impaired physical mobility Risk for injury OOSSTTEEOOMMYYEELLIITTIISS PPyyooggeenniicc iinnffeeccttiioonn ooff tthhee bboonnee.. TThhee bboonnee bbeeccoommeess iinnffeecctteedd bbyy oonnee ooff tthhrreeee mmooddeess:: Extension of soft tissue infection (eg, infected pressure or vascular ulcer, incisional infection) Direct bone contamination from bone surgery, open fracture, or traumatic injury (eg, gun shot wound Hematogenous (bloodborne) spread from other sites of infection (eg, infected tonsils, boils, infected teeth, upper respiratory infections). Infection causes tissue necrosis, breakdown of bone structure, and decalcification SSttaapphhyyllooccooccccuuss aauurreeuuss iiss tthhee mmoosstt ccoommmmoonn ppaatthhooggeenn.. OOtthheerr oorrggaanniissmmss iinncclluuddee PPrrootteeuuss,, PPsseeuuddoommoonnaass aanndd EE.. ccoollii
- 31. Pathophysiology Staphylococcus aureus causes 70% to 80% of bone infections. Other pathogenic organisms frequently found in osteomyelitis include Proteus and Pseudomonas species and Escherichia coli. The incidence of penicillin-resistant, nosocomial, gram- negative, and anaerobic infections is increasing. Initial response to infection is inflammation, increased vascularity, and edema. After 2 or 3 days, thrombosis of the blood vessels occurs in the area, resulting in ischemia with bone necrosis. The infection extends into the medullary cavity and under the periosteum and may spread into adjacent soft tissues and joints. Unless the infective process is treated promptly, a bone abscess forms. The resulting abscess cavity contains dead bone tissue (the sequestrum), which does not easily liquefy and drain. SSiiggnnss aanndd ssyymmppttoommss SSuuddddeenn ppaaiinn iinn tthhee aaffffeecctteedd bboonnee;; tteennddeerrnneessss,, hheeaatt aanndd sswweelllliinngg oovveerr tthhee aaffffeecctteedd aarreeaa,, aanndd rreessttrriicctteedd mmoovveemmeenntt.. CClliinniiccaall mmaanniiffeessttaattiioonnss ooff sseeppttiicceemmiiaa ((ffeevveerr,, cchhiillllss,, ttaacchhyyccaarrddiiaa,, ggeenneerraall mmaallaaiissee)) DDiiaaggnnoossttiicc SSttuuddiieess XX--rraayy:: ddeemmoonnssttrraattee ssoofftt ttiissssuuee sswweelllliinngg BBoonnee SSccaann aanndd MMRRII:: hheellpp wwiitthh eeaarrllyy ddeeffiinniittiivvee ddiiaaggnnoossiiss BBlloooodd aanndd wwoouunndd ccuullttuurree:: iiddeennttiiffyy aapppprroopprriiaattee aannttiibbiioottiicc tthheerraappyy Elevated WBC and ESR Treatment o Administration of large doses of antibiotics I.V. after blood cultures are taken o Early surgical drainage to relieve pressure buildup and sequestrum formation o Immobilization of the affected bone by plaster cast, traction, or bed rest o Supportive measures: analgesics and I.V. fluids o If an abscess forms, incision and drainage, followed by a culture of the drainage matter
- 32. o Antibiotic therapy to control infection o Local application of packed, wet, antibiotic-soaked dressings o Surgery to remove dead bone and to promote drainage NNuurrssiinngg iinntteerrvveennttiioonnss oo PPrroommoottee ccoommffoorrtt IImmmmoobbiilliizzeedd aaffffeecctteedd bboonnee bbyy mmaaiinnttaaiinniinngg sspplliinnttiinngg.. EElleevvaattee aaffffeecctteedd lleegg ttoo rreedduuccee sswweelllliinngg AAddmmiinniisstteerr aannaallggeessiiccss aass nneeeeddeedd.. oo CCoonnttrrooll iinnffeeccttiioouuss pprroocceessss MMoonniittoorr ssiiggnnss ooff ssuuppeerriinnffeeccttiioonn ((eegg,, oorraall oorr vvaaggiinnaall ccaannddiiddiiaassiiss,, lloooossee oorr ffoouull-- ssmmeelllliinngg ssttoooollss)) AAddmmiinniisstteerr aannttiibbiioottiiccss aass pprreessccrriibbeedd.. UUssee aasseeppttiicc tteecchhnniiqquuee wwhheenn ddrreessssiinngg tthhee wwoouunndd ttoo pprroommoottee hheeaalliinngg aanndd ttoo pprreevveenntt ccrroossss ccoonnttaammiinnaattiioonn.. oo EEnnccoouurraaggee ppaarrttiicciippaattiioonn iinn AADDLL wwiitthhiinn tthhee pphhyyssiiccaall lliimmiittaattiioonnss ooff tthhee ppaattiieenntt ttoo pprroommoottee ggeenneerraall wweellll bbeeiinngg.. o Administer I.V. fluids to maintain adequate hydration as needed o Provide a high protein and vitamin C
- 33. o Support the affected limb with firm pillows. o Provide good cast care. Support the cast with firm pillows and ―petal‖ the edges with pieces of adhesive tape or moleskin to smooth rough edges o Check circulation and drainage every 4 hours for the first 24 hours postoperatively. OOSSTTEEOOPPOORROOSSIISS TThhee rraattee ooff bboonnee rreessoorrppttiioonn aacccceelleerraatteess wwhhiillee tthhee rraattee ooff bboonnee ffoorrmmaattiioonn sslloowwss ddoowwnn,, ccaauussiinngg aa lloossss ooff bboonnee mmaassss BBoonneess lloossee ccaallcciiuumm aanndd pphhoosspphhaattee ssaallttss aanndd bbeeccoommee ppoorroouuss,, bbrriittttllee,, aanndd aabbnnoorrmmaallllyy vvuullnneerraabbllee ttoo ffrraaccttuurree Affects weight bearing vertebrae, ribs, femurs, and wrist bones. Vertebral and wrist fractures are common. RRiisskk FFaaccttoorrss PPoossttmmeennooppaauussaall wwoommeenn SSmmaallll--ffrraammeedd,, nnoonn--oobbeessee AAggeess 5500--7700 LLoonngg tteerrmm ccoorrttiiccoosstteerrooiidd tthheerraappyy HHiigghh ccaaffffeeiinnee iinnttaakkee SSmmookkiinngg HHiigghh aallccoohhooll iinnttaakkee SSeeddeennttaarryy lliiffeessttyyllee oorr iimmmmoobbiilliittyy IInnssuuffffiicciieenntt ccaallcciiuumm iinnttaakkee oorr aabbssoorrppttiioonn SSmmaallll tthhiinn ffrraammee HHeerreeddiittaarryy pprreeddiissppoossiittiioonn CCooeexxiissttiinngg mmeeddiiccaall ccoonnddiittiioonnss ((hhyyppeerrppaarraatthhyyrrooiiddiissmm,, hhyyppeerrtthhyyrrooiiddiissmm))
- 34. Causes: o Primary osteoporosis- unknown o Secondary osteoporosis- prolonged therapy with steroids, heparin, anticonvulsants, or thyroid preparations; from aluminum-containing antacids; or total immobility or disuse of a bone. o Linked also to alcoholism, malnutrition, malabsorption, scurvy, lactose intolerance, hyperthyroidism, and osteogenesis imperfecta AAsssseessssmmeenntt FFiinnddiinnggss Develops insidiously, an elderly person bends to lift something, hears a snapping sound, then feels a sudden pain in the lower back. LLoossss ooff hheeiigghhtt FFrraaccttuurreess ooff tthhee wwrriisstt,, vveerrtteebbrraall ccoolluummnn aanndd hhiipp LLoowweerr bbaacckk ppaaiinn KKyypphhoossiiss RReessppiirraattoorryy iimmppaaiirrmmeenntt DDiiaaggnnoossttiicc tteessttss XX--rraayyss:: ddeeggeenneerraattiioonn iinn tthhee lloowweerr tthhoorraacciicc aanndd lluummbbaarr vveerrtteebbrraaee;; vveerrtteebbrraall bbooddiieess mmaayy aappppeeaarr ffllaatttteenneedd,, wwiitthh vvaarryyiinngg ddeeggrreeeess ooff ccoollllaappssee aanndd wweeddggiinngg.. DDuuaall--eenneerrggyy xx--rraayy aabbssoorrppttiioommeettrryy ((DDEEXXAA)) SSeerruumm ccaallcciiuumm-- nnoorrmmaall SSeerruumm aallkkaalliinnee pphhoosspphhaattaassee-- nnoorrmmaall Serum phosphorus- normal
- 35. Treatment Physical therapy program Doctor may order estrogen to decrease the rate of bone resorption and calcium and vitamin D to support normal bone metabolism Surgery: correct pathologic fractures of the femur be open reduction and internal fixation Adequate intake of dietary calcium and regular weight bearing exercise may reduce a person’s chances of developing senile osteoporosis Hormone treatments Decreased alcohol consumption Prompt treatment of hyperthyroidism NNuurrssiinngg iinntteerrvveennttiioonnss PPrreevveennttiioonn AAddeeqquuaattee ddiieettaarryy oorr ssuupppplleemmeennttaall ccaallcciiuumm RReegguullaarr wweeiigghhtt bbeeaarriinngg eexxeerrcciissee MMooddiiffiiccaattiioonn ooff lliiffeessttyyllee CCaallcciiuumm wwiitthh vviittaammiinn DD ssuupppplleemmeennttss AAddmmiinniisstteerr HHRRTT,, aass pprreessccrriibbeedd RReelliieevviinngg ppaaiinn IImmpprroovviinngg bboowweell eelliimmiinnaattiioonn PPrreevveennttiinngg iinnjjuurryy NNuurrssiinngg AAccttiivviittiieess EEnnccoouurraaggee uussee ooff aassssiissttiivvee ddeevviicceess wwhheenn ggaaiitt iiss uunnssttaabbllee PPrrootteecctt ffrroomm iinnjjuurryy ((ssiiddee rraaiillss,, wwaallkkeerr)) EEnnccoouurraaggee aaccttiivvee//ppaassssiivvee RROOMM PPrroommoottee ppaaiinn rreelliieeff EEnnccoouurraaggee ggoooodd ppoossttuurree aanndd bbooddyy mmeecchhaanniiccss DEXA scan
- 36. PPAAGGEETT’’SS DDIISSEEAASSEE PPrrooggrreessssiivvee sskkeelleettaall ddiisseeaassee wwiitthh ddeeffoorrmmiittyy EExxcceessssiivvee bboonnee rreessoorrppttiioonn ((oosstteeooccllaassttiicc pphhaassee)),, ffoolllloowweedd bbyy aa rreeaaccttiivvee pphhaassee ooff eexxcceessssiivvee aabbnnoorrmmaall bboonnee ffoorrmmaattiioonn ((oosstteeoobbllaassttiicc pphhaassee)) Chaotic, fragile, and weak, the new bone structure causes painful deformities of external contour and internal structure IItt ccaann bbee ffaattaall,, ppaarrttiiccuullaarrllyy iiff aassssoocciiaatteedd wwiitthh hheeaarrtt ffaaiilluurree,, bboonnee ssaarrccoommaa,, oorr ggiiaanntt cceellll ttuummoorrss Causes Unknown One theory holds that early viral infection (possibly with mumps virus) causes a dormant skeletal infection that erupts many years later as Paget’s disease. CClliinniiccaall MMaanniiffeessttaattiioonn EEaarrllyy ssttaaggeess:: sseevveerree,, ppeerrssiisstteenntt ppaaiinn iinntteennssiiffiieess wwiitthh wweeiigghhtt bbeeaarriinngg aanndd mmaayy iimmppaaiirr mmoovveemmeenntt AAssyymmmmeettrriiccaall bboowwiinngg ooff ffeemmuurr aanndd ttiibbiiaa EEnnllaarrggeemmeenntt ooff tthhee sskkuullll ((ffrroonnttaall aanndd oocccciippiittaall aarreeaa)),, hhaatt ssiizzee iinnccrreeaasseess CCrraanniiaall nneerrvvee ccoommpprreessssiioonn Kyphosis Barrel shaped chest RReessppiirraattoorryy ddiissttrreessss PPaaiinn DDiiaaggnnoossttiicc FFiinnddiinnggss XX--rraayyss EElleevvaatteedd sseerruumm aallkkaalliinnee pphhoosspphhaattaassee Elevated serum calcium BBoonnee ssccaann Treatment Drug therapy: calcitonin and etidronate or plicamycin Calcitonin and etidronate: retard bone resorption and reduce serum alkaline phosphatase levels and urinary hydroxyproline secretion Plicamycin: decreases calcium, urinary hydroxyproline and serum alkaline phosphatase levels. Surgery: to reduce or prevent pathologic fractures, correct secondary deformities, and relieve neurologic impairment Aspirin, indomethacin, or ibuprofen usually controls pain
- 37. NNuurrssiinngg iinntteerrvveennttiioonnss Monitor serum calcium and alkaline phosphatase levels Monitor intake and output Change position to prevent pressure ulcers Provide high topped sneakers to prevent foot drop. Demonstrate to patient how to inject calcitonin and rotate injection sites Warn the patient that adverse effects (nausea, vomiting, local inflammation at injection site, facial flushing, itching of hands, and fever) may occur. Tell the patient receiving etidronate to take this medication with fruit juice 2 hours before or after meals (milk or other high-calcium fluids impair absorption) Tell patient receiving plicamycin to watch for signs of infection, easy bruising, and bleeding and temperature elevation and to report for regular follow-up laboratory tests. Suggests firm mattress or a bed board to minimize spinal deformities Prevent injury PPrreevveenntt ppaatthhoollooggiiccaall ffrraaccttuurreess CCoonnttrrooll ppaaiinn AAddmmiinniisstteerr ddrruuggss aass pprreessccrriibbeedd BBOONNEE TTUUMMOORRSS OOSSTTEEOOSSAARRCCOOMMAA MMoosstt ccoommmmoonn pprriimmaarryy bboonnee ttuummoorr OOccccuurrss bbeettwweeeenn 1100--2255 yyeeaarrss ooff aaggee,, wwiitthh PPaaggeett''ss ddiisseeaassee aanndd eexxppoossuurree ttoo rraaddiiaattiioonn EExxhhiibbiittss aa mmootthh--eeaatteenn ppaatttteerrnn ooff bboonnee ddeessttrruuccttiioonn.. MMoosstt ccoommmmoonn ssiitteess:: mmeettaapphhyyssiiss ooff lloonngg bboonneess eessppeecciiaallllyy tthhee ddiissttaall ffeemmuurr,, pprrooxxiimmaall ttiibbiiaa aanndd pprrooxxiimmaall hhuummeerruuss CClliinniiccaall MMaanniiffeessttaattiioonn llooccaall ssiiggnnss –– ppaaiinn ((dduullll,, aacchhiinngg aanndd iinntteerrmmiitttteenntt iinn nnaattuurree)),, sswweelllliinngg,, lliimmiittaattiioonn ooff mmoottiioonn PPaallppaabbllee mmaassss nneeaarr tthhee eenndd ooff aa lloonngg bboonnee ssyysstteemmiicc ssyymmppttoommss:: mmaallaaiissee,, aannoorreexxiiaa,, aanndd wweeiigghhtt lloossss
- 38. DDiiaaggnnoossttiicc FFiinnddiinnggss BBiiooppssyy-- ccoonnffiirrmmss tthhee ddiiaaggnnoossiiss XX--rraayy MMRRII BBoonnee SSccaann IInnccrreeaassee aallkkaalliinnee pphhoosspphhaattaassee Treatment RRaaddiiaattiioonn CChheemmootthheerraappyy SSuurrggiiccaall mmaannaaggeemmeenntt:: AAmmppuuttaattiioonn LLiimmbb ssaallvvaaggee pprroocceedduurreess PPrrooggnnoossiiss:: ppoooorr pprrooggnnoossiiss ((rraappiidd ggrroowwtthh rraattee)) NNuurrssiinngg iinntteerrvveennttiioonnss PPrroommoottee uunnddeerrssttaannddiinngg ooff tthhee ddiisseeaassee pprroocceessss aanndd ttrreeaattmmeenntt rreeggiimmeenn PPrroommoottee ppaaiinn rreelliieeff PPrreevveenntt ppaatthhoollooggiicc ffrraaccttuurree.. PPrroommoottee ccooppiinngg sskkiillllss aanndd sseellff eesstteeeemm AAsssseessss ffoorr ppootteennttiiaall ccoommpplliiccaattiioonnss ((iinnffeeccttiioonn,, ccoommpplliiccaattiioonnss ooff iimmmmoobbiilliittyy)).. EEnnccoouurraaggee eexxeerrcciissee aass ssoooonn aass ppoossssiibbllee ((11sstt oorr 22nndd ppoosstt--oopp ddaayy)) DDaannggllee aanndd ttrraannssffeerr ppaattiieenntt ttoo wwhheeeellcchhaaiirr aanndd bbaacckk wwiitthhiinn 11sstt oorr 22nndd ddaayy ppoosstt--oopp;; ccrruuttcchh wwaallkkiinngg ssttaarrtteedd aass ssoooonn aass ppaattiieenntt ffeeeellss ssuuffffiicciieennttllyy ssttrroonngg TTOOTTAALL HHIIPP RREEPPLLAACCEEMMEENNTT aa ppllaassttiicc ssuurrggeerryy tthhaatt iinnvvoollvveess rreemmoovvaall ooff tthhee hheeaadd ooff tthhee ffeemmuurr ffoolllloowweedd bbyy ppllaacceemmeenntt ooff aa pprroosstthheettiicc iimmppllaanntt
- 39. NNuurrssiinngg iinntteerrvveennttiioonnss TTeeaacchh cclliieenntt hhooww ttoo uussee ccrruuttcchheess TTeeaacchh cclliieenntt mmeecchhaanniiccss ooff ttrraannssffeerrrriinngg.. DDiissccuussss iimmppoorrttaannccee ooff ttuurrnniinngg aanndd ppoossiittiioonniinngg ppoosstt--oopp.. PPllaaccee aaffffeecctteedd lleegg iinn aann aabbdduucctteedd ppoossiittiioonn aanndd ssttrraaiigghhtt aalliiggnnmmeenntt ffoolllloowwiinngg ssuurrggeerryy PPrreevveenntt hhiipp fflleexxiioonn ooff mmoorree tthhaann 9900 ddeeggrreeeess.. AAppppllyy ssuuppppoorrtt ssttoocckkiinnggss AAddvviissee cclliieenntt ttoo aavvooiidd eexxtteerrnnaall//iinntteerrnnaall rroottaattiioonn ooff aaffffeecctteedd eexxttrreemmiittyy ffoorr 66 mmoonntthhss ttoo 11 yyeeaarr aafftteerr ssuurrggeerryy IInnssttrruucctt cclliieenntt ttoo aavvooiidd eexxcceessssiivvee bbeennddiinngg,, hheeaavvyy lliiffttiinngg,, jjooggggiinngg,, jjuummppiinngg EEnnccoouurraaggee iinnttaakkee ooff ffooooddss rriicchh iinn VViittaammiinn CC,, pprrootteeiinn,, aanndd iirroonn.. AAddmmiinniisstteerr pprreessccrriibbeedd mmeeddiiccaattiioonnss.. CCoommpplliiccaattiioonnss IInnffeeccttiioonn HHeemmoorrrrhhaaggee TThhrroommbboopphhlleebbiittiiss PPuullmmoonnaarryy eemmbboolliissmm PPrroosstthheessiiss ddiissllooccaattiioonn PPrroosstthheessiiss lloooosseenniinngg DDEEVVEELLOOPPMMEENNTTAALL DDYYSSPPLLAASSIIAA OOFF TTHHEE HHIIPP ((DDDDHH)) ccoonnddiittiioonn iinn wwhhiicchh tthhee hheeaadd ooff tthhee ffeemmuurr iiss iimmpprrooppeerrllyy sseeaatteedd iinn tthhee aacceettaabbuulluumm,, oorr hhiipp ssoocckkeett,, ooff tthhee ppeellvviiss.. Most common disorder that affects the hip joints of children under age 3. The abnormality may be unilateral or bilateral. It occurs in 3 forms of varying severity: o Unstable hip dysplasia- the hip is positioned normally but can be dislocated by manipulation o Subluxation or incomplete dislocation- the femoral head rides on the edge of the acetabulum. o Complete dislocation- the femoral heads is totally outside the acetabulum.
- 40. CCaauusseess:: o Unknown o One theory: hormones that relax maternal ligaments in preparation for labor may also cause laxity of infant ligaments around the capsule of the hip joint. o Dislocation occurs 10 times more often after breech delivery (malpositioning in utero) than after cephalic delivery. o Occurs 3x more often to the left hip than the right hip AAsssseessssmmeenntt NNeeoonnaatteess:: Experience no gross deformity of pain In complete dysplasia, the hip rides above the acetabulum, causing the leg on the affected side to appear shorter or the affected hip more prominent To test for Ortolani’s sign, place the infant on his back, with his hip flexed and in a neutral position. Grasp the legs just below the knees, then gently abduct the hip form a neutral position. If you exert slight pressure upward and inward beneath the greater trochanter, the dislocated head of the femur may slip into the acetabulum with a palpable click. IImmpplleemmeennttaattiioonn:: iinnffaannttss yyoouunnggeerr tthhaann 33 mmoonntthhss SSpplliinnttiinngg ooff tthhee hhiippss wwiitthh PPaavvlliikk hhaarrnneessss ttoo mmaaiinnttaaiinn fflleexxiioonn aanndd aabbdduuccttiioonn aanndd eexxtteerrnnaall rroottaattiioonn ((nneeoonnaattaall ppeerriioodd)) tthhee iinnffaannttss mmuusstt wweeaarr tthhiiss aappppaarraattuuss ccoonnttiinnuuoouussllyy ffoorr 22 ttoo 33 mmoonntthh aanndd tthheenn wweeaarr aa nniigghhtt sspplliinntt ffoorr aannootthheerr mmoonntthh ssoo tthhee jjooiinntt ccaappssuullee ccaann ttiigghhtteenn aanndd ssttaabbiilliizzee iinn ccoorrrreecctt aalliiggnnmmeenntt.. Gentle manipulation to reduce the dislocation
- 41. IInnffaannttss bbeeyyoonndd tthhee nneewwbboorrnn ppeerriioodd aanndd cchhiilldd AAsssseessssmmeenntt TThhee wwaallkkiinngg cchhiilldd:: mmiinniimmaall ttoo pprroonnoouunncceedd vvaarriiaattiioonn iinn ggaaiitt,, mmaayy ccaauussee tthhee cchhiilldd ttoo sswwaayy ffoorrmm ssiiddee ttoo ssiiddee ((――dduucckk wwaaddddllee‖‖)) ffoorr uunnccoorrrreecctteedd bbiillaatteerraall ddyyssppllaassiiaa;; uunniillaatteerraall ddyyssppllaassiiaa mmaayy pprroodduuccee aa lliimmpp AAssyymmmmeettrryy ooff tthhee gglluutteeaall aanndd tthhiigghh sskkiinn ffoollddss wwhheenn tthhee cchhiilldd iiss ppllaacceedd pprroonnee aanndd tthhee lleeggss aarree eexxtteennddeedd aaggaaiinnsstt tthhee eexxaammiinniinngg ttaabbllee ssuuggggeessttiinngg ssuubblluuxxaattiioonn oorr ddiissllooccaattiioonn LLiimmiitteedd rraannggee ooff mmoottiioonn iinn tthhee aaffffeecctteedd hhiipp.. AAssyymmmmeettrriicc aabbdduuccttiioonn ooff tthhee aaffffeecctteedd hhiipp wwhheenn tthhee cchhiilldd iiss ppllaacceedd ssuuppiinnee wwiitthh tthhee kknneeeess aanndd hhiippss fflleexxeedd.. AAppppaarreenntt sshhoorrtt ffeemmuurr oonn tthhee aaffffeecctteedd ssiiddee To test for Trendelenburg’s sign, have the child rest his weight on the side of the dislocation and lift his other knee. His pelvis drops on the normal side because of weak abductor muscles in the affected hip. When the child stands with his weight on the normal side and lifts the other knee, the pelvis remains horizontal or is elevated; these phenomena make up a positive Trendelenburg’s sign. IImmpplleemmeennttaattiioonn TTrraaccttiioonn aanndd//oorr ssuurrggeerryy ttoo rreelleeaassee mmuusscclleess aanndd tteennddoonnss Bilateral skin traction (in infants) or skeletal traction (in children who have started walking) in an attempt to reduce the dislocation by gradually abducting the hips. Closed reduction, if traction fails. FFoolllloowwiinngg ssuurrggeerryy,, ppoossiittiioonniinngg aanndd iimmmmoobbiilliizzaattiioonn iinn aa ssppiiccaa ccaasstt uunnttiill hheeaalliinngg iiss aacchhiieevveedd,, ffoorr 44 ttoo 66 mmoonntthhss If closed treatment fails, open reduction, followed by immobilization in a hip-spica cast for an average of 6 months. The earlier the infant receives treatment, the better the chances for normal development Treatment varies with the patient’s age.
- 42. NNuurrssiinngg IInntteerrvveennttiioonnss When transferring the child after casting, use your palms to avoid making dents in the cast. Such dents predispose the patient to pressure ulcers. (the casts needs 24 to 48 hours to dry naturally) Immediately after the cast is applied, use a plastic sheet to protect it from moisture around the perineum and buttocks. Turn the child every 2 hours during the day and every 4 hours at night. Check color, sensation, and motion of the infant’s legs and feet. Check the cast daily for odors which may signify infection. If the child complains of itching, she may benefit from diphenhydramine. You may aim a blow-dyer set on cool at the cat edges to relieve itching. Provide adequate nutrition, and maintain adequate fluid intake to avoid complication of immobility, such as renal calculi and constipation. SSCCOOLLIIOOSSIISS LLaatteerraall ccuurrvvaattuurree ooff tthhee ssppiinnee May occur in the thoracic, lumbar, or thoracolumbar spinal segment There are 2 types of scoliosis: functional (postural) and structural. Both types are commonly associated with kyphosis (humpback) and lordosis (swayback)
- 43. Causes Functional scoliosis: results from poor posture or a discrepancy in leg lengths Structural scoliosis: involves deformity of the vertebral bodies. It may be congenital, paralytic, or idiopathic. SSuurrggiiccaall aanndd nnoonnssuurrggiiccaall iinntteerrvveennttiioonnss aarree eemmppllooyyeedd,, aanndd tthhee ttyyppee ooff ttrreeaattmmeenntt ddeeppeennddss oonn tthhee ddeeggrreeee ooff ccuurrvvaattuurree,, tthhee aaggee ooff tthhee cchhiilldd,, aanndd tthhee aammoouunntt ooff ggrroowwtthh tthhaatt iiss aannttiicciippaatteedd.. AAsssseessssmmeenntt VViissiibbllee ccuurrvvee ffaaiillss ttoo ssttrraaiigghhtteenn wwhheenn tthhee cchhiilldd bbeennddss ffoorrwwaarrdd aanndd hhaannggss aarrmmss ddoowwnn ttoowwaarrdd ffeeeett.. AAssyymmmmeettrryy ooff hhiipp hheeiigghhtt PPeellvviicc oobblliiqquuiittyy IInneeqquuaalliittiieess ooff sshhoouullddeerr hheeiigghhtt SSccaappuullaarr pprroommiinneennccee RRiibb pprroommiinneennccee RRiibb hhuummppss SSeevveerree ccaasseess,, ccaarrddiiooppuullmmoonnaarryy aanndd ddiiggeessttiivvee ffuunnccttiioonn mmaayy bbee aaffffeecctteedd bbeeccaauussee ooff ccoommpprreessssiioonn oorr ddiissppllaacceemmeenntt ooff iinntteerrnnaall oorrggaannss.. Diagnostic tests Anterior, posterior, and lateral spinal X-rays, taken with the patient standing upright and bending, confirm scoliosis and determine the degree of curvature and flexibility of the spine.
- 44. Treatment close observation exercise- to strengthen torso muscles and prevent curve progression Brace, Milwaukee brace- a curve of 25 to 40 degrees requires spinal exercises and a brace halts progression in most patients but doesn’t reverse established curvature. Surgery- a curve of 40 degrees or more requires surgery (spinal fusion) NNuurrssiinngg IInntteerrvveennttiioonnss MMoonniittoorr pprrooggrreessssiioonn ooff tthhee ccuurrvvaattuurree PPrreeppaarree tthhee cchhiilldd aanndd ppaarreennttss ffoorr tthhee uussee ooff aa bbrraaccee iiff pprreessccrriibbeedd UUssuuaallllyy wwoorrnn 2233 hhoouurrss aa ddaayy aanndd ttoo rreemmoovvee oonnllyy ffoorr bbaatthhiinngg aanndd eexxeerrcciissee.. IInnssppeecctt tthhee sskkiinn ffoorr ssiiggnnss ooff rreeddnneessss oorr bbrreeaakkddoowwnn KKeeeepp tthhee sskkiinn cclleeaann aanndd ddrryy,, aavvooiiddiinngg lloottiioonnss aanndd ppoowwddeerrss Instead, suggest use of rubbing alcohol or tincture of benzoin to toughen the skin.
- 45. Increase activities gradually and avoid vigorous sports aaddvviissee tthhee cchhiilldd ttoo wweeaarr ssoofftt nnoonniirrrriittaattiinngg ccllootthhiinngg uunnddeerr tthhee bbrraaccee PPrreeppaarree tthhee cchhiilldd aanndd ppaarreennttss ffoorr ssuurrggeerryy iiff pprreessccrriibbeedd.. PPoossttooppeerraattiivvee:: MMaaiinnttaaiinn pprrooppeerr aalliiggnnmmeenntt;; aavvooiidd ttwwiissttiinngg mmoovveemmeennttss LLooggrroollll tthhee cchhiilldd wwhheenn ttuurrnniinngg,, ttoo mmaaiinnttaaiinn aalliiggnnmmeenntt IInnssttrruucctt iinn aaccttiivviittyy rreessttrriiccttiioonnss IInnssttrruucctt tthhee cchhiilldd ttoo rroollll ffrroomm aa ssiiddee--llyyiinngg ppoossiittiioonn ttoo aa ssiittttiinngg ppoossiittiioonn,, aanndd aassssiisstt wwiitthh aammbbuullaattiioonn KYPHOSIS an anteroposterior curving of the spine causes a bowing of the back, usually at the thoracic level. Occurs in children and adults Causes Congenital kyphosis leads to cosmetic deformity and reduced pulmonary function. Appear in adolescence or adulthood Adult kyphosis may result from aging and associated degeneration of intervertebral disks, atrophy, and osteoporotic collapse of the vertebrae; from endocrine disorders, such as hyperparathyroidism and Cushing’s disease; and from prolonged steroid therapy Assessment findings Mild pain at the apex of the curve Fatigue Tenderness or stiffness in the involved area or along the entire spine Prominent vertebral spinous processes at the lower dorsal and upper lumbar levels Round back appearance associated with weakness of the back and generalized fatigue Disk lesions called Schmorl’s nodes develops in the anteroposterior curving of the spine Diagnostic tests On PE: curvature of the spine in varying degrees of severity. X-ray: show vertebral wedging, Schmorl’s nodes, irregular end plates Mild scoliosis of 10 to 20 degrees Treatment Therapeutic exercises Bed rest on firm mattress (with or without traction) Brace to straighten the kyphotic curve until spinal growth is complete Pelvic tilt to decrease lumbar lordosis Hamstring stretch to overcome muscle contractures Thoracic hyperextension to flatten the kyphotic curve
- 46. Lateral X-rays taken every 4 months to evaluate correction Gradual weaning from the brace Surgery for spinal curve greater than 60 degrees or intractable and disabling back pain in a patient with full skeletal maturity. ANKYLOSING SPONDYLITIS chronic, progressive inflammatory disease affects the sacroiliac, apophyseal, and costovertebral joints and adjacent soft tissue disease progresses unpredictably and can go into remission, exacerbation, or arrest at any stage Causes unknown more than 90% of patient with this disease exhibit the histocompatibility antigen HLA-B27 Immunity activity by the presence of circulating immune complexes Familial tendency Assessment findings Intermittent lower back pain, most severe in the morning or after a period of inactivity Stiffness and limited motion of the lumbar spine Pain and limited expansion of the chest Peripheral arthritis involving the shoulders, hips and knees Kyphosis, in advanced stages, caused by chronic stooping to relieve symptoms Hip deformity and limited range of motion Tenderness over sites of inflammation Tenderness over the sacroiliac joint Mild fatigue, fever, anorexia, or weight loss Occasional iritis Aortic regurgitation and cardiomegaly Diagnostic tests X-ray findings: blurring of the bony margins of joints in the early stage, bilateral sacroiliac involvement, patchy sclerosis with superficial bony erosions, eventual squaring of the vertebral bodies, and ―bamboo‖ spine with complete ankylosis confirms the diagnosis Slightly elevated ESR and alkaline phosphatase and creatine kinase levels Treatment Management aims to delay further deformity by good posture, stretching and deep- breathing exercises Braces and lightweight supports
- 47. Anti-inflammatory analgesics, such as aspirin, indomethacin, and sulindac, control pain and inflammation Surgery Nursing interventions Promote patient comfort Administer medications as ordered Apply local heat and provide massage to relieve pain Assess mobility and degree of discomfort frequently. CARPAL TUNNEL SYNDROME Most common nerve entrapment syndrome, results form compression of the median nerve at the wrist, within the carpal tunnel. The median nerve, along with blood vessels and flexor tendons, passes through this tunnel to the fingers and thumb. Occurs in women between ages 30 and 60 and poses a serious occupational health problem Causes Some conditions can cause the contents or structure of the carpal tunnel to swell and press the median nerve against the transverse carpal ligament Conditions like: rheumatoid arthritis, flexor tenosynovitis, nerve compression, pregnancy, renal failure, menopause, diabetes mellitus, acromegaly, edema following Colle’s fracture, hypothyroidism, myxedema, benign tumors, and tuberculosis. Dislocation or acute sprain of the wrist Assessment findings Weakness, pain, burning, numbness, or tingling in one or both hands This paresthesia affects the thumb, forefinger, middle finger, and half of the fourth finger Decreased sensation to light touch or pinpricks in the affected fingers Inability to clench the hand into a fist Nail atrophy Dry, shiny skin and pain Diagnostic test (+) Tinel’s sign: tingling over the median nerve on light percussion (+) Phalen’s wrist-flexion test: holding the forearms vertically and allowing both hand to drop into complete flexion at the wrists for 1 minute Compression test: blood pressure cuff inflated above systolic pressure on the forearm for 1 to 2 minutes provokes pain and paresthesia along the distribution of the median nerve Electromyography: detects a median nerve motor conduction delay of more than 5 milliseconds
- 48. Treatment Resting the hands by splinting the wrist in neutral extension for 1 to 2 weeks Correction of underlying disorder Surgical decompression of the nerve by sectioning the entire transverse carpal tunnel ligament Nursing interventions Mild analgesics Apply splint. Perform range of motion exercises After surgery, monitor vital signs, and regularly check the color, sensation, and motion of the affected hand ptf 2005
