PTP&M011 PTM of Plantar Fasciitis Medical Journal
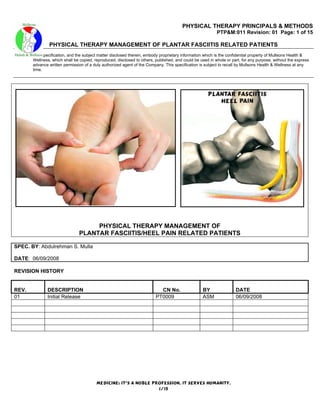
- 1. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 1 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN RELATED PATIENTS SPEC. BY: Abdulrehman S. Mulla DATE: 06/09/2008 REVISION HISTORY REV. DESCRIPTION CN No. BY DATE 01 Initial Release PT0009 ASM 06/09/2008 Medicine: It’s a noble profession, It serves humanity. 1/15
- 2. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 2 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. TABLE OF CONTENTS PAGE 1.0 PLANTAR FASCIITIS (PLAN-TUR FAS-E-I-TIS): 3 1.1 DIAGNOSIS: 3 1.2 HEEL PAIN/ AND NEURODYNAMICS: 4 1.2.1 SYMPTOMS: 5 1.3 CAUSES: 6 1.3.1 FACTORS THAT MAY INCREASE RISK OF DEVELOPING PLANTAR FASCIITIS: 6 A. AGE: 6 B. SEX: 6 C. CERTAIN TYPES OF EXERCISE: 6 D. FAULTY FOOT MECHANICS: 6 C. OBESITY: 6 D. OCCUPATIONS THAT KEEP YOU ON YOUR FEET: 7 E. IMPROPER SHOES. 7 1.4 TESTS AND DIAGNOSIS: 7 1.4.1 TRACK YOUR SYMPTOMS: 7 2.0 TREATMENTS AND DRUGS: 8 2.1 MEDICATIONS: 8 2.1.1 THERAPIES: 8 3.0 PHYSIOTHERAPY OF PLANTAR FASCIITIS/HEEL PAIN RELATED PATIENTS: 9 3.1 FURTHER INTERVENTION FOR PLANTAR FASCIITIS: 10 3.2 HEEL PAIN RELIEF EXERCISES: 11 3.2.1 CALF STRETCH: 11 3.2.2 ACHILLES TENDON STRETCH: 11 3.2.3 HAMSTRING STRETCH: 12 3.2.4 MARBLE LIFTS: 12 3.2.5 TOWEL STRETCH: 13 3.2.6 ALTERNATIVE EXERCISES & NEW INNOVATIONS: 14 A. DEEP TISSUE THERAPEUTIC WRAPS: 14 B. COLD PACK PRESSURE BRACES: 14 C. THERAPEUTIC ULTRASOUND: 15 D. NIGHT SPLINTS: 15 4.0 ALTERNATIVE MEDICINE: 15 5.0 PREVENTION: 15 Medicine: It’s a noble profession, It serves humanity. 2/15
- 3. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 3 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 1.0 PLANTAR FASCIITIS (PLAN-TUR FAS-E-I-TIS): Plantar fasciitis (PLAN-tur fas-e-I-tis) is one of the most common causes of heel pain. It involves pain and inflammation of a thick band of tissue, called the plantar fascia, which runs across the bottom of your foot — connecting your heel bone to your toes. Plantar fasciitis causes stabbing pain that usually occurs with your very first steps in the morning. Once your foot limbers up, the pain of plantar fasciitis normally decreases, but it may return after long periods of standing or after getting up from a seated position. Plantar fasciitis is particularly common in runners. People who are overweight, women who are pregnant and those who wear shoes with inadequate support are at a higher risk of plantar fasciitis. 1.1 DIAGNOSIS: Diagnosis of plantar fasciitis is based on the patient's history and on results of the physical examination. Patients typically present with inferior heel pain on weight bearing, and the pain often persists for months or even years. Pain associated with plantar fasciitis may be throbbing, searing, or piercing, especially with the first few steps in the morning or after periods of inactivity. The discomfort often improves after further ambulation but worsens with continued activity, often limiting daily activities. Walking barefoot, on toes, or up stairs may exacerbate the pain.3 The patient usually has tenderness around the medial calcaneal tuberosity at the plantar aponeurosis. A number of other conditions cause heel pain; most of these can be distinguished from plantar fasciitis by a history and physical examination. Differential Diagnosis of Heel Pain CONDITION CHARACTERISTICS Neurologic Abductor digiti quinti nerve entrapment Burning in heel pad Pain radiating down the leg to the heel, weakness, abnormal Lumbar spine disorders reflexes Medicine: It’s a noble profession, It serves humanity. 3/15
- 4. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 4 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. Problems with the medial calcaneal branch of the posterior tibial nerve Medial and plantar heel pain Neuropathies Common in patients who abuse alcohol and in patients with diabetes Tarsal tunnel syndrome Pain, burning sensation, and tingling on the sole of the foot Soft tissue Achilles tendonitis Pain is retrocalcaneal Fat pad atrophy Pain in area of atrophic heel pad Heel contusion History of trauma Plantar fascia rupture Intense tearing sensation on bottom of foot Posterior tibial tendonitis Pain on the inside of the foot and ankle Retrocalcaneal bursitis Pain is retrocalcaneal Skeletal Calcaneal epiphysitis (Sever's disease) Heel pain in adolescents Calcaneal stress fracture Calcaneal swelling, warmth, and tenderness Infections Osteomyelitis Systemic symptoms (e.g., fever, night pain) Inflammatory arthropathies More likely with bilateral plantar fasciitis Multiple joints affected Subtalar arthritis Heel pain is supracalcaneal Miscellaneous Metabolic disorders Osteomalacia Diffuse skeletal pain, muscle weakness Paget's disease Bowed tibias, kyphosis, headaches Acute episodes of pain involving long bones, pelvis, sternum, ribs Sickle cell disease Dactylitis in young children Tumors (rare) Deep bone pain, night pain, constitutional symptoms Pain in muscle groups that is reproducible with exertion, Vascular insufficiency abnormal vascular examination 1.2 HEEL PAIN/ AND NEURODYNAMICS: Heel pain is a very common and sometimes difficult problem to treat. The most popular diagnosis for pain in the heel and under the foot is plantar fasciitis. This can naturally be caused by local tissue changes but another cause is nerve entrapment, specifically in the medial and lateral plantar, tibial and medial calcaneal nerves. Nerve conduction studies have shown abnormality in nerves in patients with foot pain, providing strong evidence of neural mechanism of symptoms in some cases. Many causes could exist for this problem, including abnormal foot biomechanics (eg. excessive pronation), anatomical variations, and neural pathologies. Magnetic resonance imaging can show Schwannomas, which are a tumour in the connective tissue of the nerve, and surgical removal has been shown to be effective in this Medicine: It’s a noble profession, It serves humanity. 4/15
- 5. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 5 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. type of case. However in relation to the more physical and benign causes, there are some key facts about neurodynamic problems at the ankle that are important when considering foot pain: Patient's left foot: Entrapment of the Tibial Nerve at the Ankle (Tarsal Tunnel Syndrome) Clearly not all foot/heel pain comes from nerves, but some does. Nerve abnormality is an underestimated cause of foot pain. Research shows that patients with foot pain can show reduced nerve conduction in various nerves in the ankle/foot region. Nerve problems can masquerade as plantar fasciitis and other local causes of heel pain. There should be a distinction between 'nerve entrapment' and 'neurodynamic disorders' around the ankle and foot. Nerve entrapment is frank trapping of the nerve that is mostly likely a compressive lesion (e.g. tarsal tunnel syndrome). But, whilst the term 'neurodynamic disorders' includes 'nerve entrapment', the term should be used to denote other types of mechanical and physiological problems in nerve function at this location, e.g. nerve irritation and inflammation due to excessive use of the ankle combined with excessive pronation. This may produce a neurodynamic disorder (probably neuritis) caused by mechanical irritation. Tissue changes in the foot/heel e.g. Swelling and tenderness DO NOT EXCLUDE a neurodynamic cause. This is because the nerves can produce inflammatory changes in the tissues they innervate by a mechanism called 'neurogenic inflammation'. 1.2.1 SYMPTOMS: In most cases, the pain associated with plantar fasciitis: Develops gradually Affects just one foot, although it can occur in both feet simultaneously Is worst with the first few steps after awakening, although it also can be triggered by long periods of standing or getting up from a seated position Feels like a sharp pain in the heel of your foot Medicine: It’s a noble profession, It serves humanity. 5/15
- 6. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 6 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 1.3 CAUSES: Under normal circumstances, your plantar fascia acts like a shock-absorbing bowstring, supporting the arch in your foot. But, if tension on that bowstring becomes too great, it can create small tears in the fascia. Repetitive stretching and tearing can cause the fascia to become irritated or inflamed. 1.3.1 FACTORS THAT MAY INCREASE YOUR RISK OF DEVELOPING PLANTAR FASCIITIS INCLUDE: A. AGE: Plantar fasciitis is most common between the ages of 40 and 60. B. SEX: Women are more likely than men to develop plantar fasciitis. C. CERTAIN TYPES OF EXERCISE: Activities that place a lot of stress on your heel and attached tissue — such as long-distance running, ballet dancing and dance aerobics — can contribute to an earlier onset of plantar fasciitis. Taking overly long strides when you walk or run can stretch the plantar fascia tissue further than it is meant to stretch and cause inflammation. D. FAULTY FOOT MECHANICS: Being flat-footed, having a high arch or even having an abnormal pattern of walking can adversely affect the way weight is distributed when you're standing, putting added stress on the plantar fascia. C. OBESITY: Excess pounds put extra stress on your plantar fascia. Medicine: It’s a noble profession, It serves humanity. 6/15
- 7. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 7 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. D. OCCUPATIONS THAT KEEP YOU ON YOUR FEET: People with occupations that require a lot of walking or standing on hard surfaces — such as factory workers, teachers and waitresses — can damage their plantar fascia. if your job requires you to stand or walk for long periods of time. Staying on your feet for hours can cause the plantar fascia to swell and cause plantar fasciitis. Plantar fasciitis is very common among the restaurant waiters as they stand and walk for long periods of time. Waiters, waitresses, convenience food and department store cashiers frequently get a foot plantar fasciitis, which leads to a heel spur and is very painful according to interviews with waiters and waitresses in the area, 75% of them complain of some sort of foot pain by the end of the workday E. IMPROPER SHOES. Shoes that are thin soled, loose, or lack arch support or the ability to absorb shock doesn’t protect your feet. If you regularly wear shoes with high heels, your Achilles tendon — which is attached to your heel — can contract and shorten, causing strain on the tissue around your heel. Get your weight checked. Write down your current weight as well as what your weights has been in the past. Gaining weight can cause or aggravate plantar fasciitis, so it can help your doctor diagnose plantar fasciitis. Take a close look at your favorite pair of shoes. Your favorite pair of comfortable shoes may have lost the ability to properly support your feet. You may need new shoes or ones more suitable to your foot structure. 1.4 TESTS AND DIAGNOSIS: Your doctor may suggest an X-ray or magnetic resonance imaging (MRI) to make sure your pain isn't being caused by another problem, such as a stress fracture or pinched nerve. Sometimes, an X-ray shows a spur of bone projecting forward from the heel bone. In the past, these bone spurs were often blamed for heel pain and removed surgically. But many people who have bone spurs on their heels have no heel pain. 1.4.1 TRACK YOUR SYMPTOMS: Keep a foot pain journal to help your doctor diagnose the cause of your pain. Write down the times when your feet hurt the most. Plantar fasciitis often causes the most pain upon rising in the morning. Note whether or not your feet hurt more when you climb stairs. Pain when climbing is another sign of plantar fasciitis. Keep track of pain in your heels when you stand on your toes. Standing on your toes stretches the plantar fascia and can be a symptom of plantar fasciitis. Medicine: It’s a noble profession, It serves humanity. 7/15
- 8. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 8 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. Pay attention to tingling or numbness that accompanies your foot pain. Numbness and tingling may indicate tarsal tunnel syndrome, which is a pinching of the tibial nerve in the leg. 2.0 TREATMENTS AND DRUGS: About 90 percent of the people who have plantar fasciitis recover with conservative treatments in just a few months. 2.1 MEDICATIONS: Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs, such as ibuprofen (Advil, Motrin, others) and naproxen (Aleve), may ease pain and inflammation, although they won't treat the underlying problem. Corticosteroids. This type of medication may be delivered through a process called iontophoresis, in which a corticosteroid solution is applied to the skin over the painful area and the medication is absorbed with the aid of a nonpainful electric current. Another delivery method is injection. Multiple injections aren't recommended because they can weaken your plantar fascia and possibly cause it to rupture, as well as shrink the fat pad covering your heel bone. Ultrasound guidance is sometimes used for more accurate placement of the corticosteroid injection. 2.1.1 THERAPIES: Physical therapy. A physical therapist can instruct you in a series of exercises to stretch the plantar fascia and Achilles tendon and to strengthen lower leg muscles, which stabilize your ankle and heel. A therapist may also teach you to apply athletic taping to support the bottom of your foot. Night splints. Your doctor may recommend wearing a splint fitted to your calf and foot while you sleep. This holds the plantar fascia and Achilles tendon in a lengthened position overnight so that they can be stretched more effectively. Orthotics. Your doctor may prescribe off-the-shelf or custom-fitted arch supports (orthotics) to help distribute pressure to your feet more evenly. Surgical or other procedures Extracorporeal shock wave therapy. In this procedure, sound waves are directed at the area of heel pain to stimulate healing. It's usually used for chronic plantar fasciitis that hasn't responded to more-conservative treatments. This procedure may cause bruises, swelling, pain, numbness or tingling, and has not been shown to be consistently effective. Surgery. Only a small percentage of people need surgery to detach the plantar fascia from the heel bone. It's generally an option only when the pain is severe and all else fails. Side effects include a weakening of the arch in your foot. Medicine: It’s a noble profession, It serves humanity. 8/15
- 9. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 9 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.0 PHYSIOTHERAPY OF PLANTAR FASCIITIS/HEEL PAIN RELATED PATIENTS: Initially treatment is aimed at decreasing inflammation. Later the therapist will strengthen the small muscles of your feet and improve the flexibility of your fascia and Achilles tendon. The aim is to support and put less stress on the weak and inflamed plantar fascia. Stretching is an important treatment. If the pain is bad in the morning putting a towel under the forefoot and pulling up with the hands can stretch the foot up. Standing calf stretches and a night splint to hold the foot up in a partly stretched position can also be useful. Deep massage along the plantar fascia may be useful and can be done by the sufferer once shown how by a therapist. Ice can reduce both pain and inflammation, used from 10 to 20 minutes as an ice pack. Use care with ice and ensure your skin is protected. Do not put a freezing pack directly on your skin as this can cause frostbite like damage. A therapist or trainer to attempt to route some of the forces through the sole along a different line can use taping. Advice on activity modification is important, as the condition may not completely resolve. Patients may need to consider alternative methods of keeping up their aerobic fitness and strength if weight-bearing activity is too painful. Shock absorbing heel pads can be useful and should be tried as soon as the condition presents. Silicone gel pads are commonly used and are relatively cheap. Arch supports may also be useful to restore more normal foot mechanics in cases where this has been disturbed. Medicine: It’s a noble profession, It serves humanity. 9/15
- 10. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 10 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.1 FURTHER INTERVENTION FOR PLANTAR FASCIITIS: Despite appropriate physiotherapy management, some patients with plantar fasciitis do not improve. When this occurs the treating physiotherapist or doctor will advise on the best course of management. This may include further investigations (such as X-rays, Ultrasound, MRI scan), pharmaceutical intervention, corticosteroid injection, autologous blood injection or referral to appropriate medical authorities who can advise on any intervention that may be appropriate to improve the condition. A review with a podiatrist may also be required for prescription of orthotics to improve foot posture and function. In very rare chronic cases surgical intervention may be considered. Referral pathway for plantar fasciitis Medicine: It’s a noble profession, It serves humanity. 10/15
- 11. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 11 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.2 HEEL PAIN RELIEF EXERCISES: 3.2.1 CALF STRETCH: Stand facing a wall with your hands on the wall at about eye level. Put the leg you want to stretch about a step behind your other leg. Keeping your back heel on the floor, bend your front knee until you feel a stretch in the back leg. Hold the stretch for 15 to 20 seconds. Repeat 4 times. 3.2.2 ACHILLES TENDON STRETCH: Stand on a step as shown. Slowly let your heels down over the edge of the step as you relax your calf muscles. Hold the stretch for about 15 to 20 seconds, then tighten your calf muscle a little to bring your heel back up to the level of the step. Repeat 4 times. Medicine: It’s a noble profession, It serves humanity. 11/15
- 12. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 12 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.2.3 HAMSTRING STRETCH: Extend one leg in front of you with the foot flexed. Bend your other knee and lean back slightly. Your pelvis should be tilted forward. Keep your upper body upright as you hold the stretch for 10-20 seconds, then switch sides. You should feel the stretch up the back of your extended leg (all the way up your calf and thigh). To perform an assisted version of this stretch, place a stretching strap around the ball of the extended foot and use your arms to pull on the strap to draw in your leg closer to your body, as in step 2 above. 3.2.4 MARBLE LIFTS: Place marbles on the floor next to a cup, as shown. Using your toes, try to lift the marbles up from the floor and deposit them in the cup. Repeat exercise 15 times. Medicine: It’s a noble profession, It serves humanity. 12/15
- 13. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 13 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.2.5 TOWEL STRETCH: Grab a rolled towel at both ends, holding it under the ball of your foot. Gently pull the towel toward you while keeping your knee straight. Hold this position for 15 to 20 seconds. Repeat 4 times. Medicine: It’s a noble profession, It serves humanity. 13/15
- 14. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 14 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. 3.2.6 ALTERNATIVE EXERCISES & NEW INNOVATIONS: Swimming, treading water, cycling. Avoid weight-bearing exercise that places strain on the plantar fascia e.g. running and football. Put your feet up. Stay off your feet for several days when the pain is severe. Apply ice. Hold a cloth-covered ice pack over the area of pain for 15 to 20 minutes three or four times a day or after activity. Or try ice massage. Freeze a water-filled paper cup and roll it over the site of discomfort for about five to seven minutes. Regular ice massage can help reduce pain and inflammation. Decrease your miles. You probably won't have to permanently retire your running or walking shoes, but it's a good idea to cover shorter distances until pain subsides. Take up a no- or low-impact exercise. Swap swimming or bicycling in place of walking or jogging. You'll likely be able to return to your regular activities as heel pain gradually improves or disappears. However, some people find that the only way to avoid a recurring problem is to permanently modify their aerobic activities. Add arch supports to your shoes. Inexpensive over-the-counter arch supports take the tension off the plantar fascia and help absorb shock. Stretch your arches. Simple exercises using household objects can stretch your plantar fascia, Achilles tendon and calf muscles. A. DEEP TISSUE THERAPEUTIC WRAPS: During normal use, activity promotes blood flow through our body. Our body responds to the activity by sending oxygen and nutrient-rich blood to the muscles, tendons, ligaments and surrounding tissue. When we are at rest, the blood flow to that area is greatly reduced. But, when your body is injured, it really needs the blood flow to promote the healing process. Since you can't work the area without danger of further injury, you need to stimulate the blood flow another way. These innovative wraps give you the best Blood Flow Stimulation Therapy available. The wrap creates special energy waves that stimulate blood flow by penetrating through the outer layers of your skin. The energy waves reach deep into your muscles, ligaments, tendons and cartilage, reducing your pain as they heal the inner tissue. The wrap for Plantar Fasciitis is revolutionary. Its soft flexible design molds itself to the contours of your body, providing you with a perfectly fitted, easy-to-use Blood Flow Stimulation Therapy tool. You have to try one to appreciate the ease and comfort. The wrap is made of durable, medical-grade neoprene. It stays in place, is flexible and contours to the shape of your foot. The strategically placed pocket holds the Energy Web component across the bottom of your foot and up the back of the heel while focusing the soothing and healing energy waves where you need them, at your damaged tissue. A wrap gives you unparalleled blood flow stimulation energy. You simply won’t find a comparable product on the market. You will feel the soothing, deep penetrating warmth as it works to stimulate your blood flow, B. COLD PACK PRESSURE BRACES: Cold compression wraps interrupt and slow nerve and cell function in the damaged area. Once blood vessels are damaged they can no longer carry oxygenated blood to the damaged tissue and therefore cells begin to breakdown. The deep cold provided by cold compression wraps slow cell function thereby reducing cellular breakdown. Furthermore, because the cold wraps serve to numb the nerves the wraps also reduce pain! In the early days or weeks of your injury the inflammation is partly your body's reaction to try to immobilize the injured area. Unfortunately this inflammation also strains the surrounding tissue and causes pain. Cold compression braces provide the support and reduce the inflammation giving your body the support it needs without the usual pain. Medicine: It’s a noble profession, It serves humanity. 14/15
- 15. PHYSICAL THERAPY PRINCIPALS & METHODS PTP&M:011 Revision: 01 Page: 15 of 15 PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS RELATED PATIENTS NOTICE: This specification, and the subject matter disclosed therein, embody proprietary information which is the confidential property of Mullsons Health & Wellness, which shall be copied, reproduced, disclosed to others, published, and could be used in whole or part, for any purpose, without the express advance written permission of a duly authorized agent of the Company. This specification is subject to recall by Mullsons Health & Wellness at any time. C. THERAPEUTIC ULTRASOUND: Ultrasonic massage treatments these days are a primary treatment for all forms of soft tissue inflammation. It is also a supplementary treatment for plantar fasciitis. One can get maximum benefit from getting ultrasound treatments 3 times each day and every day. Ultrasound treatments can reduce the amount of scarring around the injured area. In fact, doctors and physical therapists to break down existing scar tissue regularly use ultrasound treatments. With ultrasound, you heal more quickly and more completely. D. NIGHT SPLINTS: Using night splints regularly will allow you to awaken each morning in less pain and discomfort and help you recover from Plantar Fasciitis faster. Treating your inflamed fascia with radiant energy, cold compression and ultrasound throughout the day will relieve your pain and get you on the right track to a healthy fascia ligament. However, when you sleep some of your hard work is undone as your foot relaxes and your fascia becomes taut. By wearing a night splint, you ensure continuous healing while you sleep. Night splints are proven effective devices that are designed to maintain a passive stretch in the fascia ligament by stabilizing your ankle and preventing your foot from falling into a relaxed position. By gently stretching the fascia ligament throughout the night you not only stop the retearing every morning, you also add 8 hours of effortless healing time to your therapy program while you sleep. 4.0 ALTERNATIVE MEDICINE: Although some over-the-counter arch supports contain magnets, no reliable evidence indicates that arch supports with magnets relieve heel pain any better than arch supports without magnets. 5.0 PREVENTION: You can take some simple steps now to prevent painful steps later: Maintain a healthy weight. This minimizes the stress on your plantar fascia. Choose supportive shoes. Avoid high heels. Buy shoes with a low to moderate heel, good arch support and shock absorbency. Don't go barefoot, especially on hard surfaces. Don't wear worn-out athletic shoes. Replace your old athletic shoes before they stop supporting and cushioning your feet. If you're a runner, buy new shoes after about 500 miles of use. Medicine: It’s a noble profession, It serves humanity. 15/15
- 16. Filename: PTP&M011 PTM of Plantar Fasciitis Medical Journal Directory: C:UsersAnjumDocumentsShadab MullaMullsons Medical Journals Template: C:UsersAnjumAppDataRoamingMicrosoftTemplates Normal.dot Title: PHYSICAL THERAPY MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN RELATED PATIENTS Subject: Physiotherapy Author: Abdulrehman Keywords: Comments: Creation Date: 4/13/2009 3:45 AM Change Number: 25 Last Saved On: 6/6/2009 2:19 AM Last Saved By: Abdulrehman S. Mulla Total Editing Time: 877 Minutes Last Printed On: 6/6/2009 2:19 AM As of Last Complete Printing Number of Pages: 15 Number of Words: 3,743 (approx.) Number of Characters: 21,339 (approx.)
