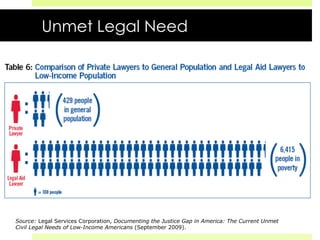
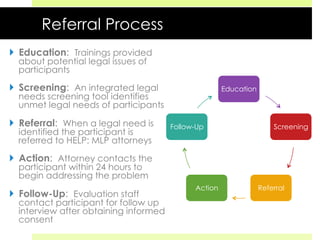
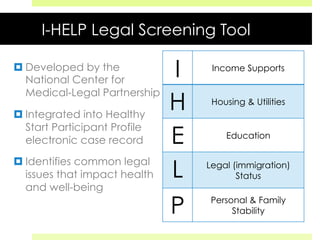
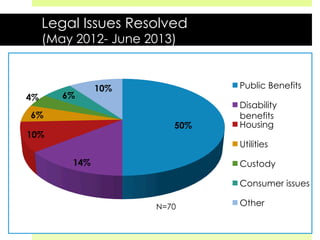
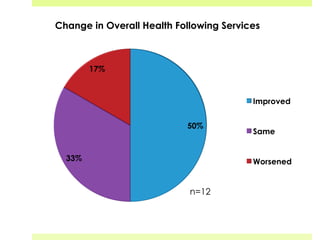
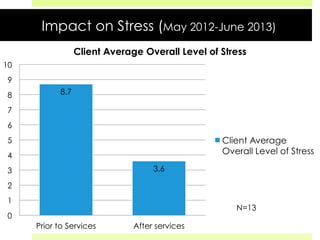
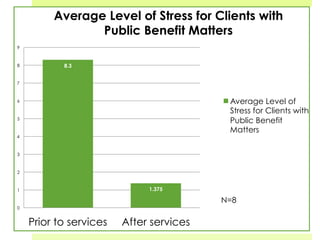
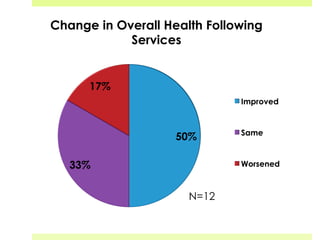
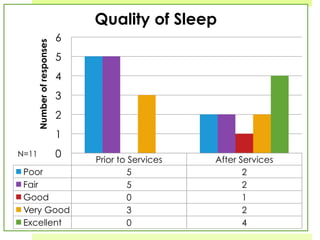
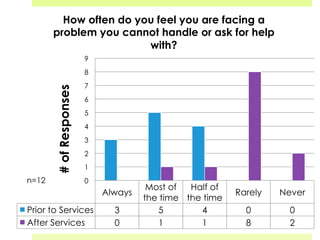
This document discusses medical-legal partnerships (MLPs), which integrate legal assistance into patient care to address social determinants of health. It provides examples of how MLPs have helped patients experiencing issues like difficulties accessing public benefits, housing problems, and education barriers. The Health, Education and Legal Assistance Project MLP improved patients' health, reduced stress, and resolved issues like gaining disability benefits or public housing for over 100 individuals. MLPs help healthcare providers identify legal needs and improve health outcomes, but challenges include sustainability, evaluation, and gaining long-term health data.