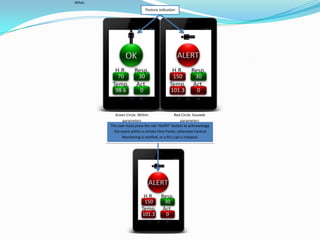
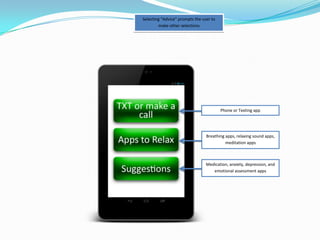
The document describes a proposed mobile application called the Emotion ALERT! System that utilizes wearable biometric sensors and physiological data to detect changes in a user's emotions and provide alerts. It is intended to help trauma brain injury survivors who have difficulties controlling emotional outbursts. The system monitors heart rate, respiration, skin temperature and other data to identify emotional arousal. It alerts users and allows them to get assistance, engage in regulation strategies, or contact emergency services if needed. Conversations with TBI survivors found emotional outbursts were challenging and this type of system could help provide more awareness and control.