Birth Trauma. Asphyxia.ppt
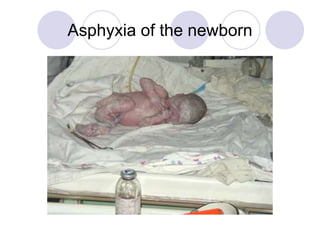
- 1. Asphyxia of the newborn
- 2. Hellou !
- 3. Definition WHO: Asphyxia is incapacity of newborn to begin or to support of spontaneous respiration after delivery due to breaching of oxygenation during labor and delivery India: Asphyxia is absent or ineffective respiration of newborn of 1 minute old with Apgar score less than 4
- 4. Definition Great Britain: Asphyxia is critical insufficiency of oxygen in fetus during delivery so severe that leads to development of metabolic acidosis and depression of spontaneous respiration
- 5. Definition Canada: Asphyxia is breach of gas exchange when hypoxia and hypercapnia, and considerable metabolic acidosis occur
- 6. Definition Australia: Asphyxia is a state with mother has complications in perinatal period that decrease provision with oxygen and leads to acidosis functional violation minimum 2 organs due to acts of acute hypoxia
- 7. Definition Ukraine: Asphyxia of newborn as a nosological form is conditioned by causes when fetus out and find (connect) with severe maternal-placental and (or) umbilical flow leads to increasing of oxygen approach to fetus tissue and hypoxia development
- 8. Definition
- 9. Asphyxia Asphyxia: means to be pulse less, but more useful is a definition of impaired or interrupted gas exchange. These situations can take place: a. Intrauterine: the gas exchange depends on the function of placenta, and the blood-flow in the umbilical vessels. b. Intrapartum c. Postnatal: after delivery the gas exchange takes place in the pulmonary vesicles or alveoli and depends on the function of the heart, lungs and brain.
- 10. Causes of Asphyxia Fetal hypoxia: Mother: hypoventilation during anesthesia, cyanotic heart disease, respiratory failure or carbon monoxide poisoning. Low maternal blood pressure as a result of the hypotension that may compression of the vena cava & aorta by the gravid uterus Inadequate relaxation of the uterus to permit placental filling as a result of uterine tetany caused by excessive administration of oxytocin Premature separation of the placenta; placenta previa Impedance to the circulation of blood through the umbilical cord as a result of compression or knotting of the cord Uterine vessel vasoconstriction by cocaine, smoking Placental insufficiency from numerous causes, including gestosis, eclampcia, toxemia, postmaturity Extremes in maternal age (< 20 years or >35 years) Preterm or postterm gestation.
- 11. Causes of Asphyxia Intrapartus asphyxia: More frequently inadequate obstetric aid Using focerps, vacuum extraction, cresteller, cesaring cection Trauma: narrow pelvis, presentation Extremely rapid or prolonged labor Multiple gestation Drags depression of CNS: anaesthesia, sedatics & analgetics Meconium –stained amniotic fluid
- 12. Causes of Asphyxia Postnatal hypoxia: Anemia severe enough to lower the oxygen content of the blood to a critical level due to severe hemorrhage or hemolytic disease Shock severe enough to interfere with the transport of oxygen to vital cells from adrenal hemorrhage, intraventricular hemorrhage severe enough to age, overwhelming infection or massive blood loss A deficit in arterial oxygen saturation resulting from failure to breathe adequately postnatally due to a cerebral defect, narcosis, or injury Failure of oxygenation of an adequate amount of blood resulting from of cyanotic congenital heart disease of deficient pulmonary function
- 13. Gas exchange.
- 14. Cell pathology
- 15. Cell pathology
- 16. Cell pathology
- 17. Cell pathology
- 18. Cell pathology
- 19. Cell pathology
- 20. Heart rate, breath movements and blood pressure in fetus during primary and secondary apnea
- 21. Virginia Apgar
- 22. Apgar Score of the Newborn SIGNSCORE 0 1 2 Heart rate Absent <100 beats/min >100 Respiratory effort Absent Weak,irregular Strong cry Muscle tone Flaccid Some flexion Well Reflex irritability (response to catheter in nostril) No Grimace Cough or sneeze Skin colour Blue, pale extremities blue pink
- 23. CRITERIAS OF SEVERE ASPHYXIA: °Severe metabolic or mix acidosis pH ≤ 7.00 in arterial blood of umbilical vessels °Assessment by Apgar is 0-3 during more than 5 minutes ° Neurological symptoms such as general hypotonic, lethargy, coma, seizures °Damage of vital organs (lungs, heart and other) in fetus or newborn
- 27. Acute complications associated with Asphyxia hypotension hypoxic encephalopathy seizures persistent pulmonary hypertension hypoxic cardiomyopathy ileum and necrotizing enterocolitis acute tubular necrosis adrenal hemorrhage and necrosis hypoglycemia polycytemia disseminated intravascular coagulation
- 28. Brain Edema
- 30. Morphologic substrate of Cerebral palsy due to Asphyxia
- 31. DIAGNOSIS Clinical symptoms Metabolic derangement Renal and/or cardiac failure Assessment of the brain: a.. EEG EEG is useful particulary in the asphyxiated term newborn. Serial recordings are almost necessary. Low voltage. Burst-suppression patterns or electrical inactivity are associated with bad prognosis. Rapid resolution of EEG abnormalities and/or normal interictal EEG are associated with a good prognosis. b. Ultras onography: Ultrasound can be useful in premature newboms but is of more limited value in the term newborn. c. Computed tomography: CT is of major value both acutely during the neonatal period and later in childhood. The optimal timing of CT scanning is between 2 and 4 days.
- 32. DIAGNOSIS I. Intrauterine assessment A. Ultrasound and Doppler technique: Ultrasound: to measure the growth of the fetus. For this reason it is important have a reliable gestational age. Early during pregnancy an ultrasound will be done to date the fetus. This method safer than common clinical methods. The growth retarded fetus is in a great risk of developing asphyxia. Doppler techniques: to measure the blood flow in the umbilical vessels or aorta. A low flow or decreasing flow indicates a fetus in risk of asphyxia. B.Electrofysiological: Severe pathological fetus heart rate will lead to cessation of the delivery with Caesarean section. Fetal heart rate: Episodes of bradycardia can be dangerous and lead to brain damage. The problem is to do this type of measurement during long periods and on every pregnant woman. II. Extrauterine assessment C. Biochemical - C blood sample drawn from the umbilical artery is an ideal way to evaluate whether an intrapartum asphyxia exist or not. Low pH (< 7, 00) indicates the intrapartum asphyxia. PC02 and P02 will also be deranged as you have a diminished gas exchange. The low pH is the result of an increased level of H+ and lactate.
- 33. EEG
- 35. ABC resuscitation A- Airways (maintenance of passable ness of airway) B- breathing (stimulation of breathing) C- circulation (to support of circulation) D-drug
- 36. ABC resuscitation Step A- immediately after delivery the infant’s head should be placed in a neutral or slightly extended position Rolled towel under the shoulders
- 37. Step A- immediately after delivery the infant’s head should be placed in a neutral or slightly extended position
- 38. And airway established by clearing the mouth, then the nose by rubber bag
- 39. If meconium is present in amniotic fluid, after sucking of mouth and nose we must suck a pharynx by tube after laryngoscopes
- 40. If it is inadequate we must use step B. At first the tactile stimulation should be given to newborn, for example- gentle flicking of the feet or heel
- 41. ABC resuscitation or rubbing of the back
- 42. If these measures are inadequate, mechanical ventilation should be initiated, using mask and bag ventilation
- 43. If ventilation is adequate supplemental oxygen may be given to improve heart rate or skin colour
- 44. If mechanical ventilation does not improve the respiration, heart rate or colour skin, the following step is “C”-circulation. At first the assessment of heart rate is necessary
- 45. If heart rate is less than 60 beats/minute, or between 60 and 80 beats and is not improving, cardiac compression is a lower on/third of sternum Chest compressions with two fingers
- 46. ABC resuscitation Your big fingers must be lie on the sternum, other finder should lie under the back of newborn
- 47. ABC resuscitation If heart rate is less then 80 beats per minute the cardiac compression should be continued. If heart rate is 80 beats per minute or more the cardiac compression should be stop .
- 48. Brain death The clinical diagnosis of brain death is made on the basis of - coma manifested by lack of response to pain, light, or auditory stimulation; - apnea confirmed by documentation of failure to breathe when pCO2 is greater then 60 mm Hg tested by 3 minutes; - absent bulbar movements and brainstem reflexes (including midposition or fully dilated pupils with no response to light or pain and with absent oculocephalic, caloric, corneal, gag, cough, rooting and sucking reflexes, flaccid tone and absence of spontaneous or induced movements (excluding activity mediated at the spinal cord level)
- 49. Different painless is possible
- 50. PROGNOSIS. Prognosis is difficult because of the inability to establish the precise extent and duration of cerebral insult and injury. At the time of delivery low delayed Apgar scores between 0 and 3 at 10, 15 and 20 minutes' of age are associated with significantly increased mortality and morbidity, e.g. cerebral palsy. The single most useful prognostic factor is the severity of the neonatal neurological syndrome.
- 51. HI brain injure is the most impotent consequence of perinatan Asphyxia Leads to increase lactate, fall in pH, ↓ATP, ↑ glucose utilization, loss of cerebrovascular autoregulation Impairs ion pumps with accumulation Na,Cl,H2O, Ca intracellularly ↑ amino acid neurotransmitters (glutamate, aspartate) Generation of free radicals & leukotriens wich they overwhelm endogeneous scavenger mechanism Damage nucleic acids, lipids & proteins
- 52. HIE
- 53. Birth Trauma
- 54. Development of the CNS
- 55. Development of the CNS
- 56. Development of the CNS
- 57. Development of the CNS
- 58. Birth trauma The term “Birth trauma” is used to denote mechanical and anoxic trauma incurred by the infant during labor and delivery.
- 59. Birth trauma The incidence of B.T. has been estimated at 2 – 7 per 1000 live births. Overall 5 - 8 per 100000 infants die of B.T. and 25 per 100000 die of anoxic injuries. Some injuries may be latent initially but later result in severe illness or squealed
- 60. Birth trauma The process of birth is blend of compressions, contractions, and tractions.
- 61. Birth trauma When fetal size, presentation, or neurological immaturity complicate this event, such intrapartum forces may lead to tissue damage, edema, hemorrhage or fracture in the neonate.
- 62. Birth trauma The use of obstetrical instruments may further amplify the effect of such forces or may induce injury by itself. Although breech presentation carries the greatest risk of injury, delivery by cesarean section does not guaranteed an injury – free infant.
- 63. The risk of birth injury Primiparity Small maternal stature Maternal pelvic anomalies Extremely rapid Prolonged labor Deep transverse arrest of descent of presenting part of fetus Oligohydramnions Abnormal presentation (i.e. breech)
- 64. The risk of birth injury Use of mid-forceps or vacuum extraction Cesarean section Versions and extraction Very low birth weight infant or extreme premature Postmature infant (> 42 week of gestation) Fetal macrosomia Large fetal head Fetal anomalies (see teratoma)
- 65. Teratoma
- 66. Classification of birth injuries I. Soft-tissue injuries - caput succedaneum - subcutaneous and retinal hemorrhage, petechia - ecchymoses and subcutaneous fat necrosis
- 67. Classification of birth injuries II. Cranial injuries cephalohematoma fractures of the skull
- 68. Classification of birth injuries III. Intracranial hemorrhage subdural hemorrhage subarachnoid hemorrhage intra- and peryventricular hemorrhage parenchyma hemorrhage
- 69. Classification of birth injuries IV. Spine and spinal cord fractures of vertebra Erb-Duchenne paralysis Klumpke paralyses Phrenic nerve paralyses Facial nerves palsy
- 70. Classification of birth injuries V. Peripheral nerve injuries VI. Viscera (rupture of liver, spleen and adrenal hemorrhage) VII. Fractures of bones.
- 71. Birth trauma
- 72. Birth trauma Petechiae and ecchymosis are common manifestation of birth trauma in the newborn. If the etiology is uncertain, studies to rule out coagulation disorders or infections etiology are indicated. This lesions resolve spontaneously within 1 week. Petechiae of the skin of the heard and neck are common. All are probably secondary to a sudden increase in intrathoracic pressure during passage of the chest through the birth canal. Parents should be assured that they are temporary and result of normal hazards of delivery.
- 73. Birth trauma Subcutaneous fat necrosis. Although not detectable et birth this irregularly shaped, hard no pitting, subcutaneous plagues with overlying dusky, red – purple discoloration may by caused by pressure during delivery. They appear during the first 2 weeks of life usually in large babies on the cheeks, arms, back, buttocks end thinks.
- 74. Birth trauma Caput succedaneum is a subcutaneous extraperiosteal fluid collection with poorly defined margins it may extend across the midline over suture lines end is usually associated with heat molding the soft tissue edema will usually resolve over the few days post partum.
- 75. Birth trauma Cephalohematoma is a subperiosteal collection of blood secondary to rupture of the blood vessels between the scull and pereostium, its extent will be delineated by suture lines over days. The extent of hemorrhage may be severe enough to present as anemia and hypotension with secondary hyperbilirubinemia. It may be a focus of infection leading to meningitis, particularly when there is a concominant skull fracture. Skull X-rays should be obtained if there are CNS symptoms, if the hematoma is very large or if the delivery was very difficult. Resolution occurs over 1 to 2 month, occasionally with residual calcification as a thrombus.
- 76. Birth trauma INTRACRANIAL HEMORRHAGE occur in 20% to more than 40% of infants with birth weight under 1500 gm but is less common among more mature infants. Intracranial hemorrhage may occur in the subdural, subarachnoid, intraventricular or intracerebral regions. Subdural and subarachnoid hemorrhage follow head trauma e.g., in breech, difficult and prolonged labor and after forceps delivery. Other forms of intracranial bleeding are associated with immaturity and hypoxia. With better obstetric care intracranial bleeding has become rare.
- 77. Predisposing factors of IVH premature respiratory distress syndrome hypoxic ischemic or hypotensive injuries reperfusion of damaged vessels increased venous pressure pneumothorax hypervolemia, hypertensia
- 78. The etiologic factors with IVH in low- birth-weight infants (Intravascular inflow factors) impaired autoregulation seizers manipulation with infant infusion of hyperosmotic solutions rapid colloid infusion apnea presents of patent ductus arteriosus hypertension and use of ECMO
- 79. The etiologic factors with IVH in low- birth-weight infants (Intravascular outflow factors) respiratory distress pneumothorax congestive heart failure continuous positive airway pressure labor/delivery acute angle of the internal cerebral vein
- 80. The etiologic factors with IVH in low-birth- weight infants (Vascular and extra vascular structural factors) normal regression of germinal matrix relatively large blood flow to deep cerebral structures hypoxic-ischemic injury to germinal matrix or its vessels present of fibrinolitic enzymes poor structural support of germinal matrix vessels abrupt termination of media in arteries proximal to germinal matrix
- 81. Clinical manifestation IVH Absent Moro reflex Poor muscle tone Lethargy excessive somnolence Pallor or cyanosis Respiratory distress DIC Jaundice
- 82. Clinical manifestation IVH Bulging anterior fontanel Hypotonia Weakness, seizures, muscular twitching Temperature instability Brain stem signs (apnea, lost extraocular movements, facial weakness, abnormal eye sing)
- 83. Laboratory correlates of blood loss Metabolic acidosis Low hematocrit Hypoxemia, hypercarbia Respiratory acidosis Thrombocytopenia and prolongation of protrombin time (PT) and partial thromboplastin time (PTT)
- 84. Diagnosis IVH History Clinical manifestation Transfontanel cranial ultrasonography Computed tomography Glucose level Coagulogramma, hematocrit Lumbal punction
- 85. Outcomes and prognosis Patients with massive bleeding have a poor prognosis. About 10-15% infants may develop post hemorrhagic hydrocephalus and chronic neurological pathology
- 86. Spinal cord Strong traction exerted when the spine is hyper extended or when the direction of pull is lateral, or forceful longitudinal traction on the trunk while the head is still firmly, engaged in the pelvic, especially when combined with flections and torsion of vertical axis, may produce fracture and separation of the vertebra. Tran section of the cord may occurs with or without vertebral fractures
- 87. Clinical data Areflexia Loss of sensation Complete paralysis of voluntary motion below the level of injury Epidural hemorrhage Apnea
- 88. Delivery room If cord injury is suspected, effort in the delivery room should immediately focus on resuscitation and prevention of further insult. The head should be made immobile relative to the spine and secured on a flat, firm surface with padding of pressure points.
- 89. Duchenne-Erb paralysis Injury to the 5th and 6th cervical nerves Affected arm is adducted, internally rotated Forearm is in pronation Wrist is flexed Arm falls limply to the side of the body when passively adducted Moro, biceps and radial reflexes absent
- 90. Cervix injury
- 91. Klumpke’s paralysis injury to the 7th and 8th cervical and 1st thoracic spinal nerves Horner syndrom (ipsilateral ptosis and miosis) if the thoraxic spinal nerve is involved Absent of movements of the wrist
- 92. Phrenic nerve palsy Injury to the C3,C4 or C5 Brachial plexur injury RDS Paradox (upward) movement during inspiration
- 93. Clavicular fracture Most common Crepitus, palpable bony irregularity sternoclaidomastoid muscle spasm Cry during movement of upper extremities
- 94. Long bone injures Loss of spontaneous arm or leg movement is usually the first sing of humeral or femoral injury, following by swelling and pain on passive motion
- 95. Intraabdominal injures – target organ Liver Spleen Adrenal gland (breach presentation)
- 96. Intraabdominal injures Sudden presentation Shock Abdominal distension Bluish discoloration, jaundice, pallor Poor feeding Thachypnea, tachycardia history: difficult delivery
- 97. HIE Selective necrosis of the neurons of the deeper cerebral cortical layers is the hallmark of hypoxic injury to the perinatal brain in full-term babies, parasagittal cerebral injury occurs as a result of the generalized reduction in the cerebral blood flow. In preterm babies, the areas of infarction involve the deeper periventricular white matter. Neuronal necrosis may also entail basal ganglia.
- 98. HIE Some of the ischemic infants with encephalopathy gradually improve while others deteriorate. If not treated promptly, 20 to 30 percent of infants with severe ischemia die.
- 99. HIE
- 100. HIE
- 101. HIE
- 102. HIE
- 103. HIE
- 104. HIE HYPOXIA-ISCHEMIA ANAEROBIC GLYCOLYSIS ATP ADENOSINE ↑GLUTAMATE ↓ ↓ HYPOXANTHINE NMDA ↓ RECEPTOR XANTHINE ↓ Ca++ LIPASES NITRIC OXIDE ↓ SYNTHASE ↑ARACHIDONIC INHIBITORS ACID ↓ FREE RADICALS
- 105. Sarnat Level of consciousness Neuromuscular control Muscle tone Posture Stretch reflexes Segmental myoclonus Complex reflexes: Suck, Moro, oculovestibular tonic neck Autonomic function
- 106. Sarnat Pupils Respirations Heart rate Bronchial & salivary secretions Gastrointestinal motility Seizures EEG Duration of symptoms
- 107. Sarnat Outcome Mild: About 100% normal Moderate: 80% normal; abnormal if symptoms more than 5 to 7 days Severe: About 50% die; remainder with severe sequel
- 108. Sarnat
- 109. Diagnosis. A thorough neurological examination combined with a careful history is helpful for the diagnosis. Ultrasound examination of the brain, EEG, intracranial pressure measurement and computed scanning arc is valuable.
- 110. EEG
- 111. EEG
- 112. Treatment. Prevention of asphyxia remains the most important mode of treatment. Careful monitoring of the fetus during labor and prompt appropriate intervention at the earliest signs of fetal compromise is important in preventing perinatal asphyxia. The rapid responders from anoxia need observation in the nursery for only 12 to 24 hours. These babies become active, and start accepting feeds within a few hours. The slow responders need more aggressive management. Both: hypoxemia and hyperoxemia as well as hypercapnia should be circumvented, since they affect cerebral blood flow. These babies should be kept in ward, with a minimal noise level or in the nursery. Intravenous fluids should be restricted to two-third of the maintenance requirements and blood glucose levels must be maintained at 75-100 mg/dL. Acidosis, hypocalcaemia and hypoglycemia need correction. Seizures should be controlled with phenobarbitone but not in preterm babies who are severely disturbed and in those with decerebration.
- 113. Treatment curative and protective regimen in newborn Children with severe A or BT should be undergo strict regimen because the rest more frequently associated with emergency position if baby The infant must lie on the hard surface with fixated neck by collar The baby is observed in bed or incubator, is not washed and sometimes is turned side to side. The transport of this infant prohibitive. Oxygen (ingalation or mask or apparatus ) Feeding throught catheter 40-50% daily calories
- 114. Treatment curative and protective regimen in newborn Baby with subcompensation of all function must be undergo spareing regimen. May be washed (in bad) Feeding through catheter and spoon. If he can suck he may be apply to mother brest Common (general) regimen is administrated for healthy child or reconvalescents
- 115. Treatment Oxygenotherapy Hemostatics: 1% vit K 1mg/kg, dicinone 12.5 mg/kg Hypovolemia: 5% albumine, plasma, 5% glucose – 1-10 ml/kg Protect of nerve cells and anticonvulsants: 20% Natrium-oxybutirate 100 mg/kg, sibazone 0.3 ml/kg, Phenobarbital 20 mg/kg (5-10) 25% Magnesia 0.2 ml/kg
- 116. Treatment (underlying problems associated with BT) Hypoglycemia – 5% glucose i/v 1-10 ml/kg Hypocalciemia–10% Ca-gluconate 2 ml/kg Acidosis- 4.2% Sodium bicarbonate solution 2 meq/kg
- 117. Treatment (underlying problems associated with BT) RDS Hypoxia Hypothermia Hypotension Support cardiac output 0.5% dopamin 5 μg/kg/min & speed is 1 ml/hour
- 118. seizures
- 119. seizures
- 121. Treatment
- 122. I don’t want a trauma