Motivational Interviewing for Improved HIV Care Adherence
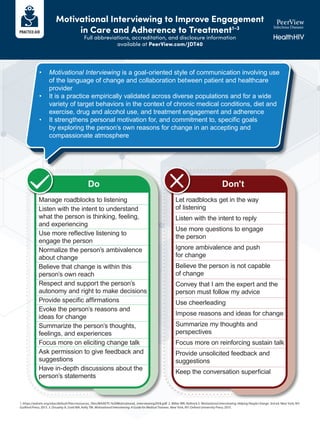
- 1. Motivational Interviewing to Improve Engagement in Care and Adherence to Treatment1-3 Full abbreviations, accreditation, and disclosure information available at PeerView.com/JDT40 1. https://aidsetc.org/sites/default/files/resources_files/MAAETC-%20Motivational_Interviewing2018.pdf. 2. Miller WR, Rollnick S. Motivational Interviewing: Helping People Change. 3rd ed. New York, NY: Guilford Press; 2013. 3. Douaihy A, Gold MA, Kelly TM. Motivational Interviewing: A Guide for Medical Trainees. New York, NY: Oxford University Press; 2015. • Motivational Interviewing is a goal-oriented style of communication involving use of the language of change and collaboration between patient and healthcare provider • It is a practice empirically validated across diverse populations and for a wide variety of target behaviors in the context of chronic medical conditions, diet and exercise, drug and alcohol use, and treatment engagement and adherence • It strengthens personal motivation for, and commitment to, specific goals by exploring the person’s own reasons for change in an accepting and compassionate atmosphere Manage roadblocks to listening Listen with the intent to understand what the person is thinking, feeling, and experiencing Use more reflective listening to engage the person Normalize the person’s ambivalence about change Believe that change is within this person’s own reach Respect and support the person’s autonomy and right to make decisions Provide specific affirmations Evoke the person’s reasons and ideas for change Summarize the person’s thoughts, feelings, and experiences Focus more on eliciting change talk Ask permission to give feedback and suggestions Have in-depth discussions about the person’s statements Let roadblocks get in the way of listening Listen with the intent to reply Use more questions to engage the person Ignore ambivalence and push for change Believe the person is not capable of change Convey that I am the expert and the person must follow my advice Use cheerleading Impose reasons and ideas for change Summarize my thoughts and perspectives Focus more on reinforcing sustain talk Provide unsolicited feedback and suggestions Keep the conversation superficial Do Don't
- 2. Rapid ART Restart1,2 Full abbreviations, accreditation, and disclosure information available at PeerView.com/JDT40 • Immediate antiretroviral therapy (ART) refers to starting HIV treatment as soon as possible after the diagnosis of HIV infection, preferably on the first clinic visit (and even on the same day the HIV diagnosis is made). This strategy also is known as "rapid ART," "same-day ART," and "treatment upon diagnosis” • Rapid ART is recommended by the Guidelines for the Use of Antiretroviral Agents in Adults and Adolescents with HIV from the U.S. Department of Health and Human Services to “increase the uptake of ART and linkage to care, decrease time to viral suppression for individual patients, and improve the rate of virologic suppression among persons with HIV” • Nearly all PWH who are re-engaging in care • PWH for whom the ART history is known, and HIV resistance is known or can be predicted • An appropriate ART regimen can be devised without information from current resistance test results • HIV RNA (viral load) • CD4 cell count • HIV resistance test • Creatine, liver transaminases • Other tests if not previously done • Persons with certain untreated opportunistic infections (OIs), such as CNS OIs, for whom a short period of treatment for the OI is recommended before ART initiation • An appropriate ART regimen cannot be devised without information from current resistance test results Rapid ART Restart for Persons Returning to Care • While a key goal of HIV care is for people with HIV (PWH) to achieve continuous viral suppression on ART, many PWH may stop ART or fall out of care for periods of time • It is important to re-engage these patients in care at the earliest opportunity, and to support them in restarting ART Immediate ART Restart Is Appropriate For Immediate ART Restart Is Not Appropriate For Laboratory Testing What Is Rapid ART?
- 3. Rapid ART Restart1,2 Full abbreviations, accreditation, and disclosure information available at PeerView.com/JDT40 1. https://aidsetc.org/sites/default/files/resources_files/ncrc-rapid-art-6-10-21_0.pdf. 2. https://clinicalinfo.hiv.gov/en/guidelines/adult-and-adolescent-arv. ART Regimens for Rapid Restart Regimens should be selected individually, based on the patient’s specific HIV, ART, and resistance history; as well as their comorbidities, tolerance of previous ARVs, adherence challenges, and other factors It is not possible to make recommendations for individual patients, but common ART restart scenarios include – The patient was taking a 1st or 2nd ART regimen and there is no suspected resistance: can start one of the regimens for initial immediate ART or (unless contraindications) can restart the patient’s previous regimen – The patient has a known or suspected history of virologic failure with acquired ART resistance: select the ART regimen based on the suspected resistance mutations – If there is concern for NRTI and/or NNRTI resistance, consider a boosted protease inhibitor + 2 NRTIs ± an integrase inhibitor – If there is concern for NRTI and/or INSTI resistance, consider a boosted protease inhibitor + 2 NRTIs ± a second-generation NNRTI – If more extensive resistance may be present, consider a multi-class regimen with a boosted darunavir + an integrase inhibitor ± an NNRTI ± NRTIs ± fostemsavir or other ARVs as indicated Consult with an HIV expert!
- 4. Tool and Steps for Identifying Evidence-Based Interventions for Retention and Re-Engagement of PLWH in Care1,2 Full abbreviations, accreditation, and disclosure information available at PeerView.com/JDT40 1. https://wwwn.cdc.gov/HIVCompendium/SearchInterventions. 2. https://www.cdc.gov/hiv/research/interventionresearch/compendium/lrc/index.html. The CDC provides a searchable Compendium of Evidence-Based Interventions and Best Practices for HIV Prevention1 as well as a separate list of interventions for linkage to, retention in, and re-engagement in HIV care2 4. Assemble a team with assigned roles 3. Select a plan that will work for your situation and clinical program 1. Enter your targeted population 2. Enter your desired effects or outcomes 5. Implement the intervention 6. Collect data 7. Evaluate 8. Adjust 9. Repeat as needed
