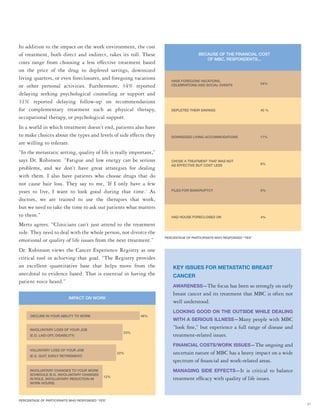
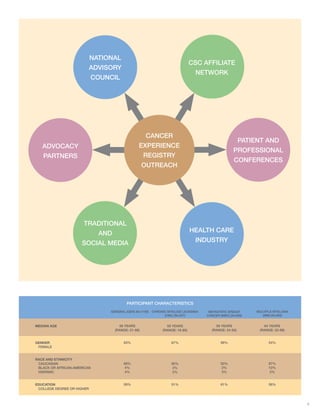
The document summarizes the Cancer Experience Registry, which collects information from cancer patients to understand their experiences and needs. It has expanded from an initial breast cancer registry to include over 7,000 participants with 35 cancer types. The goal is to empower patients by amplifying their voices and ensuring their perspectives inform healthcare. Key themes from patients include managing long-term side effects, the high cost of cancer care, and the ongoing need for emotional support. Expanding disease-specific registries allows capturing issues unique to certain cancer types.