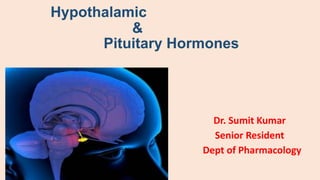
hypothalamus & Pituitary gland
- 1. Hypothalamic & Pituitary Hormones Dr. Sumit Kumar Senior Resident Dept of Pharmacology
- 2. Hormones: Chemical substances synthesized by specific endogenous glands and secreted directly into blood stream, to act far away from the site production and release, on the specific target organs.
- 3. Chemically hormones are classified into 7 major classes: • Amino acid derivative: dopamine, thyroid hormones etc • Neuropeptides: Gonadotropin releasing hormones, thyrotropin releasing hormone, somatostation. • Simple protein: Corticotropin • Large protein: Insulin, L.H, P.T.H • Glycoprotein: T.S.H • Steroids: Estrogen, Progesteron, glucocorticoids • Vitamins : Vit. D
- 4. Function: •Growth and differentiation •Maintenance of homeostatis •Reproduction and functional integration
- 5. • Pituitary gland often called as “ Master of endocrine orchestra” • Its function are primarily controlled by hypothalamus. • Pituitary gland consist of 3 different lobe: Anterior lobe ( adenohypophysis) Intermediate lobe Posterior lobe ( neurohypophysis)
- 6. Anterior pituitary hormones are produced by separate group of cells: Somatotrophs: Growth hormones Lactotrophs: Prolactin Gonadotrophs: FSH, LH Corticotrophs: ACTH Intermediate Lobe: Melanocyte stimulatory hormones Posterior lobe: Vasopressin and Oxytocin Anterior pituitary hormones are regulated by negative feedback mechanism. A long negative feedback loop A short negative feedback loop
- 7. Hypothalamus releasing factors/hormones Stimulates anterior pituitary Produce and secrete tropic hormones stimulate target glands to secrete hormones act on target organ.
- 8. Pharmacologic applications: • Replacement therapy • Antagonists for excess production of pituitary hormones. • Diagnostic tools for endocrine abnormalities.
- 10. Growth hormone: • Secretion is regulated by the action of growth hormone releasing hormone(GHRH) released by hypothalamus. • Sermorelin, a synthetic analogue of GHRH • Used as diagnostic agent for testing the pituitary GH secretion in suspected cases of childhood short stature. • Side effect: Flushing, injection site pain, dizziness, hyperactivity and urticaria.
- 11. Somatostatin: • It is growth hormone release inhibiting hormone (GHRIH). • Inhibits secretion of GH, also inhibits thyroid stimulating hormone, Insulin, prolactin, glucagon. Uses: • Use to prevent acute bleeding due to esophageal varices. • Upper git bleeding from haemorrhagic gastritis, intestinal or pancreatic fistula. • Hypersecretory tumour of intestinal tract. Limitation: short half life, lack of specificity, GH rebound after discontinuation.
- 12. Octreotide: • A long acting analogue of somatostatin. • 45 times more potent. • useful in acromegaly, some hormone secreting tumors and in bleeding esophageal varices. • Treatment of AIDS associated diarrhea, cushing syndrome and insulinoma. Adverse effect: abdominal pain, nausea, gallstones, long term therapy may lead to conduction defect, and vit B12 deficiency.
- 13. Lanreotide: • Long-acting analogue of somatostatin, • Similar in actions and specificity to octreotide • Indicated for pharmacotherapy of acromegaly. Pegvisomant: • Polyethylene glycol complexed mutant GH binds to the GH receptor but does not trigger signal transduction. • Acts as a GH antagonist. • Approved for treatment of acromegaly due to small pituitary adenoma
- 14. PROLACTIN: Physiological function: • Prolactin causes growth and development of breast during pregnancy. • Promotes proliferation of ductal as well as acinar cells in the breast and induces synthesis of milk proteins and lactose. • After parturition, prolactin induces milk secretion. Regulation of secretion: Prolactin is under predominant inhibitory control of hypothalamus through PRIH. Dopaminergic agonists (DA, bromocriptine, cabergoline) plasma prolactin levels. Dopaminergic antagonists (chlorpromazine, haloperidol, metoclopramide) and DA depleter (reserpine) cause hyperprolactinemia.
- 15. • Prolactin levels in blood are low in childhood, increase in girls at puberty and are higher in adult females. • A progressive increase occurs during pregnancy, peaks at term. • High prolactin secretion is maintained by suckling, falls if breast feeding is discontinued. • Stress, exertion and hypoglycaemia also stimulate prolactin release. • Hyperprolactinaemia is responsible for the galactorrhoea– amenorrhoea– infertility syndrome in women. • In males it causes loss of libido and decreased fertility.
- 16. Prolactin inhibitors: Bromocriptine: • Decreases prolactin release from pituitary by activating dopaminergic receptors on lactotrope cells. • Levodopa like actions in CNS—antiparkinsonian and behavioral effects. • nausea and vomiting by stimulating dopaminergic receptors in the CTZ. • Hypotension—due to central suppression of postural reflexes and weak peripheral α adrenergic blockade. • Decreases gastrointestinal motility.
- 17. Uses: • Hyperprolactinemia due to microprolactinomas causing galactorrhoea, amenorrhoea and infertility in women; gynaecomastia, impotence and sterility in men. • Parkinsonism • Bromocriptine is used to suppress lactation and breast engorgement after delivery (like in stillbirth) and following abortion. Cabergoline: • It is a newer D2 agonist; more potent; more D2 selective and longer acting. • Lower Incidence of nausea and vomiting. • It is preferred for treatment of hyperprolactinemia and acromegaly
- 18. GONADOTROPINS (Gns): The anterior pituitary secretes two Gns viz. FSH and LH. FSH: • In the female induces follicular growth, development of ovum and secretion of estrogens. • In the male supports spermatogenesis and has a trophic influence on seminiferous tubules. • Ovarian and testicular atrophy occurs in the absence of FSH LH: • Induces ovulation • In male LH stimulates testosterone secretion.
- 19. Uses: • Gonadotropin deficiency in males. • Undescended testes. • Amenorrhea and infertility. • In vitro fertilization—to time the ovulation
- 20. Gonadotropin-releasing hormone (Gnrh): • Regulates the secretion of gonadotropins—FSH and LH • Secreted in a pulsatile manner. • Gonadorelin is synthetic GnRH, used in diagnostic tests in hypogonadism. • Pulsatile administration is used in infertility and delayed puberty. • Continuous administration inhibits gonadotropin secretion • used in prostatic cancers and some gynecological conditions like uterine fibroids and endometriosis. Ex- leuprolide, Goserelin, Nafarelin, Triptorelin,
- 21. In 1–2 weeks they cause desensitization and down regulation of GnRH receptors inhibition of FSH and LH secretion suppression of gonadal function. Spermatogenesis or ovulation cease and testosterone or estradiol levels fall to castration levels.
- 22. • Recovery occurs within 2 months of stopping treatment. • used as nasal spray or injected s.c. • Reversible pharmacological oophorectomy/ orchidectomy is used in precocious puberty, prostatic carcinoma, endometriosis, premenopausal breast cancer, uterine leiomyoma, polycystic ovarian disease and to induced ovulation. • Used as contraceptive for both males and females.
- 23. GnRH antagonists: • Some extensively substituted GnRH analogues act as GnRH receptor antagonists. • Inhibit Gn secretion without causing initial stimulation. • They block the pituitary GnRH receptors and thereby suppress the secretion of LH, FSH and delay ovulation. • They are used in in vitro fertilization and are also useful in prostatic cancer and in reducing uterine fibroids and endometriosis. Ex- ganirelix and cetrorelix
- 24. THYROID STIMULATING HORMONE (TSH, THYROTROPIN): TSH stimulates thyroid to synthesize and secrete thyroxine (T4) and triiodothyronine (T3). Its actions are: • Induces hyperplasia and hypertrophy of thyroid follicles and increases blood supply to the gland. • Promotes trapping of iodide into thyroid by increasing Na+: Iodide symporter (NIS). • Promotes organification of trapped iodine and its incorporation into T3 and T4 by increasing peroxidase activity.
- 25. Regulation of secretion: • Synthesis and release of TSH by pituitary is controlled by hypothalamus primarily through TRH, while somatostatin inhibits TSH secretion. • Dopamine also reduces TSH production induced by TRH.
- 26. ADRENOCORTICOTROPIC HORMONE (ACTH, CORTICOTROPIN): • ACTH promotes steroidogenesis in adrenal cortex. • Controls the synthesis and release of glucocorticoids, mineralocorticoids, and androgens from the adrenal cortex. • ACTH also exerts trophic influence on adrenal cortex. • High doses cause hypertrophy and hyperplasia. • Lack of ACTH results in adrenal atrophy. • It is used in the diagnosis of adrenocortical insufficiency.
- 27. HORMONES OF THE POSTERIOR PITUITARY • Vasopressin and oxytocin • Not regulated by releasing hormones. • They are synthesized in the hypothalamus, transported to the posterior pituitary, and released in response to specific physiologic signals, such as high plasma osmolarity or parturition. Oxytocin • Used in obstetrics, to stimulate uterine contraction to induce or reinforce labor. • Oxytocin causes milk ejection by contracting the myoepithelial cells around the mammary alveoli. • Toxicities are uncommon when used properly: hypertension, uterine rupture, water retention, and fetal death have been reported. • Contraindicated in abnormal fetal presentation, fetal distress, and premature births.
- 28. Vasopressin(antidiuretic hormone) • Vasopressin has both antidiuretic and vasopressor effects. • In the kidney, it binds to the V2 receptor to increase water permeability and reabsorption in the collecting tubules. • Major use of vasopressin is to treat diabetes insipidus, also used in the management of cardiac arrest and in bleeding due to esophageal varices. • Other effects of vasopressin are mediated by the V1 receptor, which is found in liver, vascular smooth muscle (where it causes constriction), and other tissues. • Major toxicities are water intoxication and hyponatremia. Headache, bronchoconstriction, and tremor can also occur. • Desmopressin: • Minimal activity at the V1 receptor, making it largely free of pressor effects.
- 29. Thank you