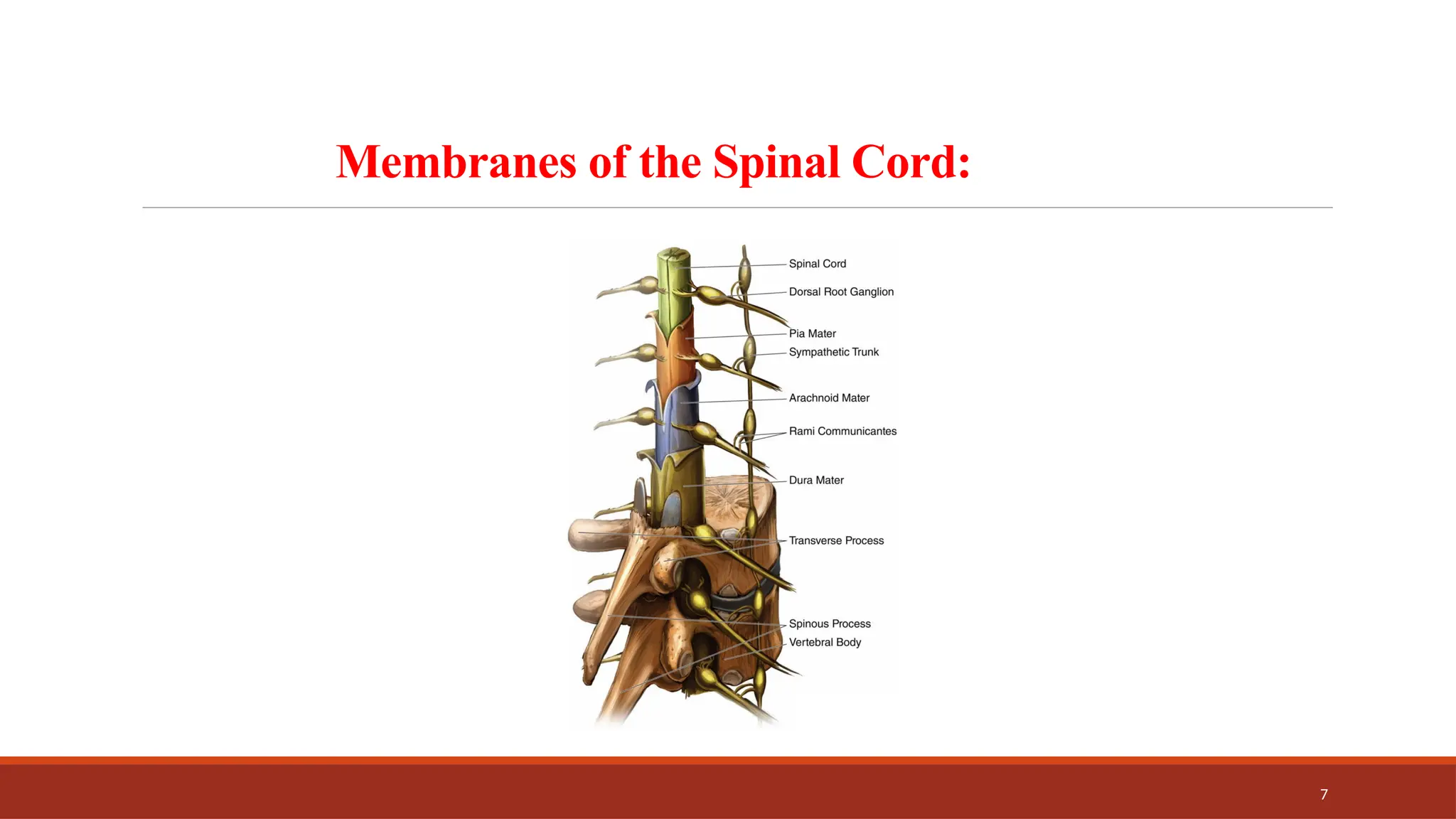
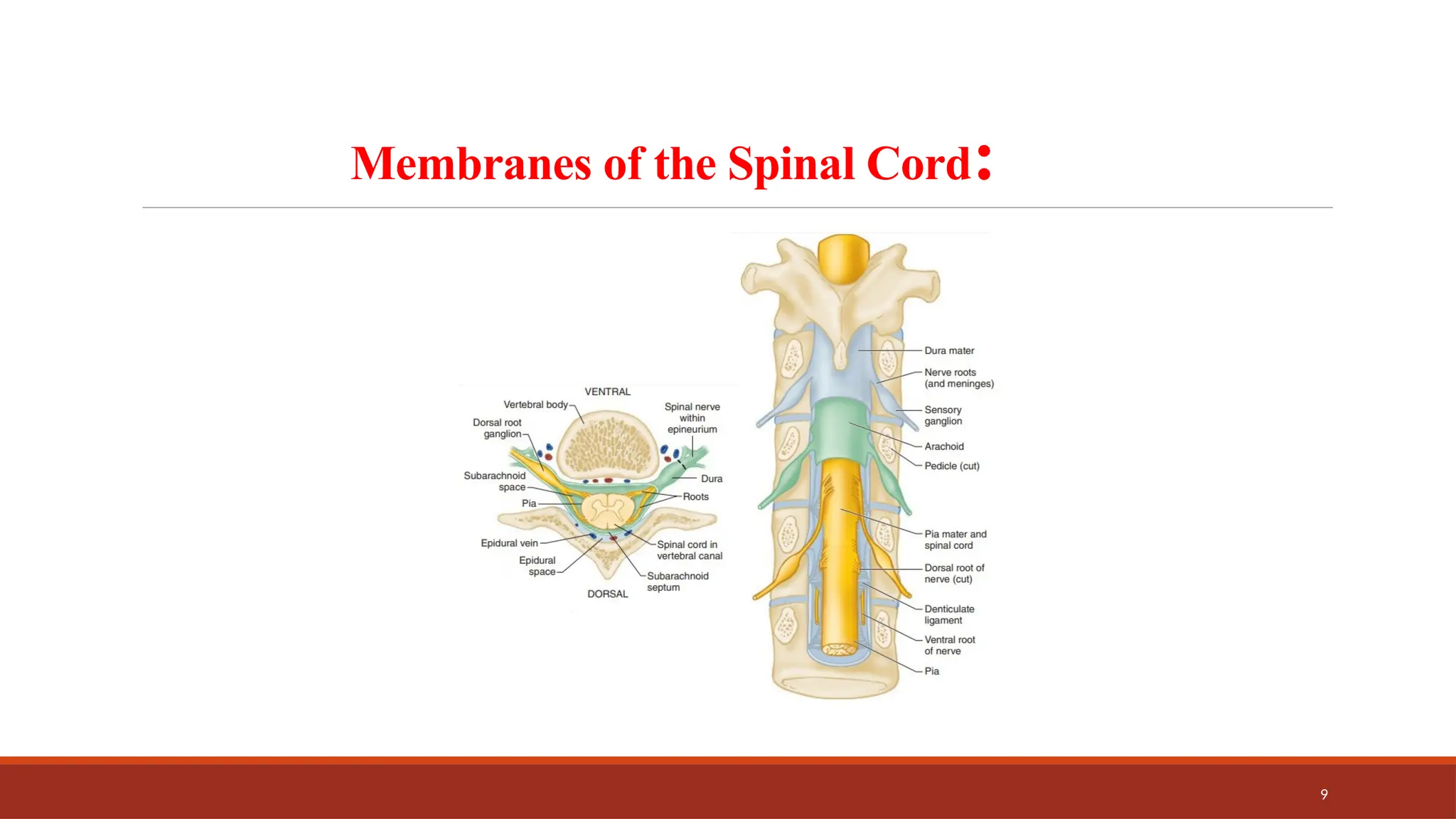
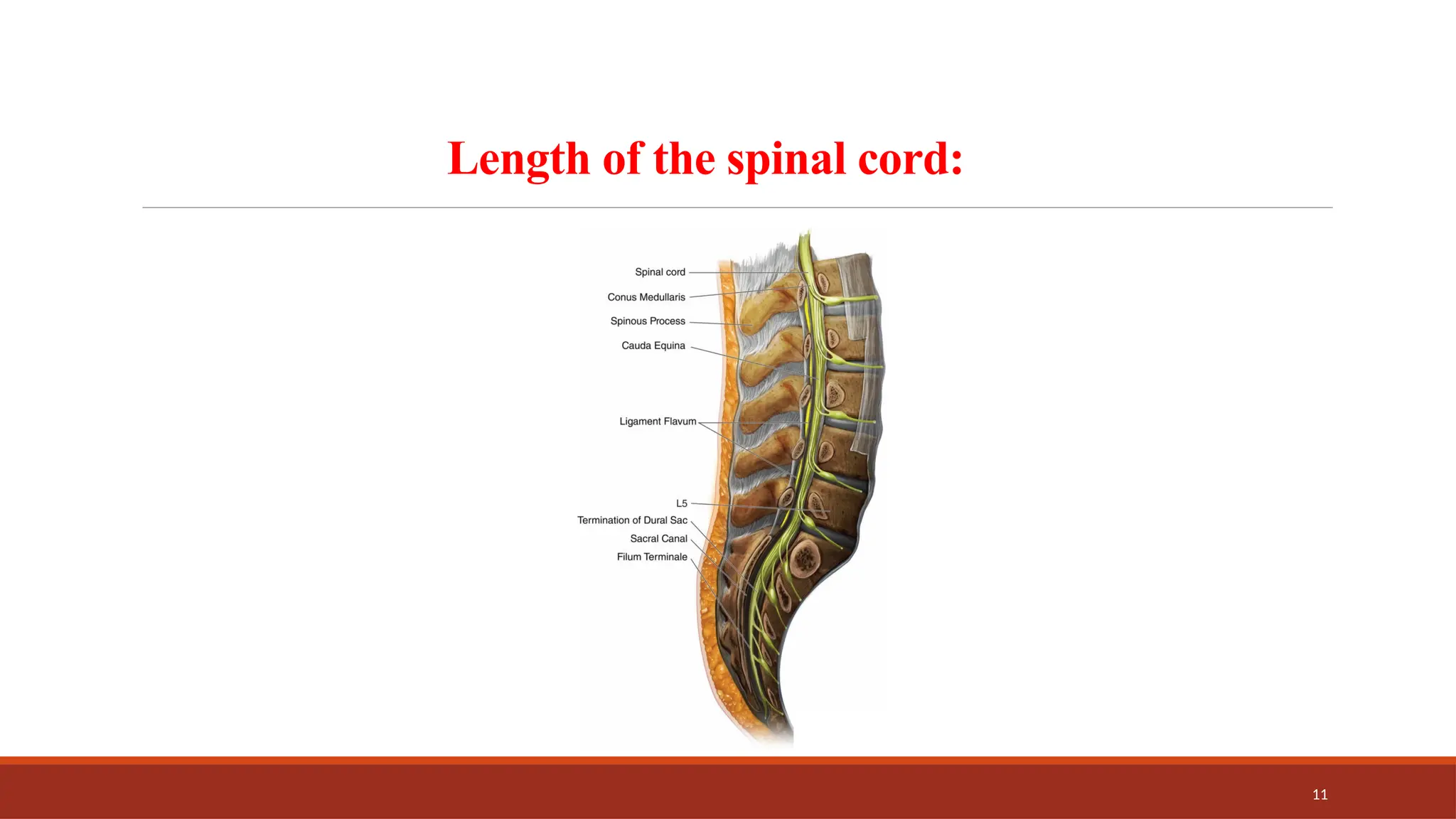
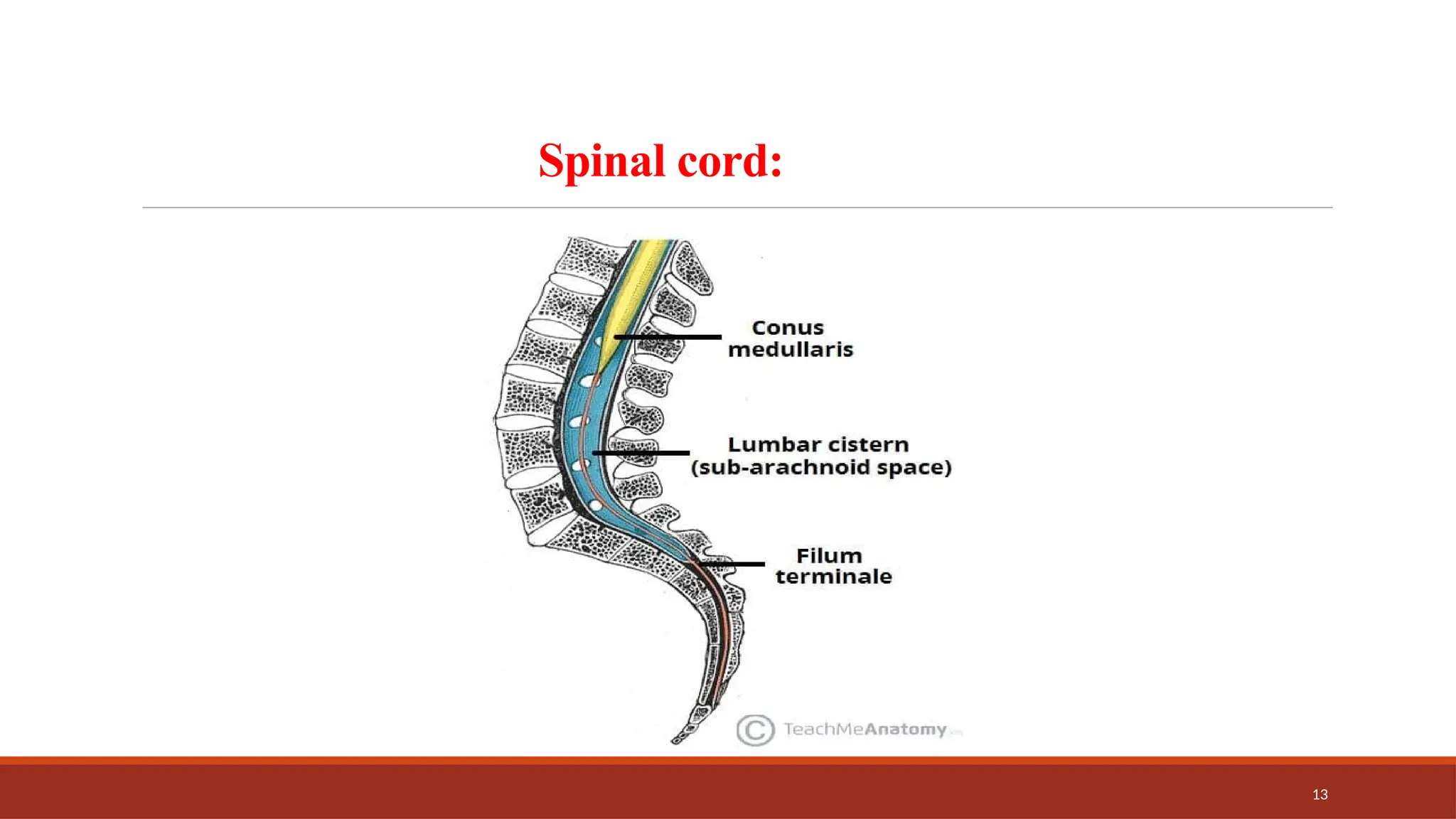
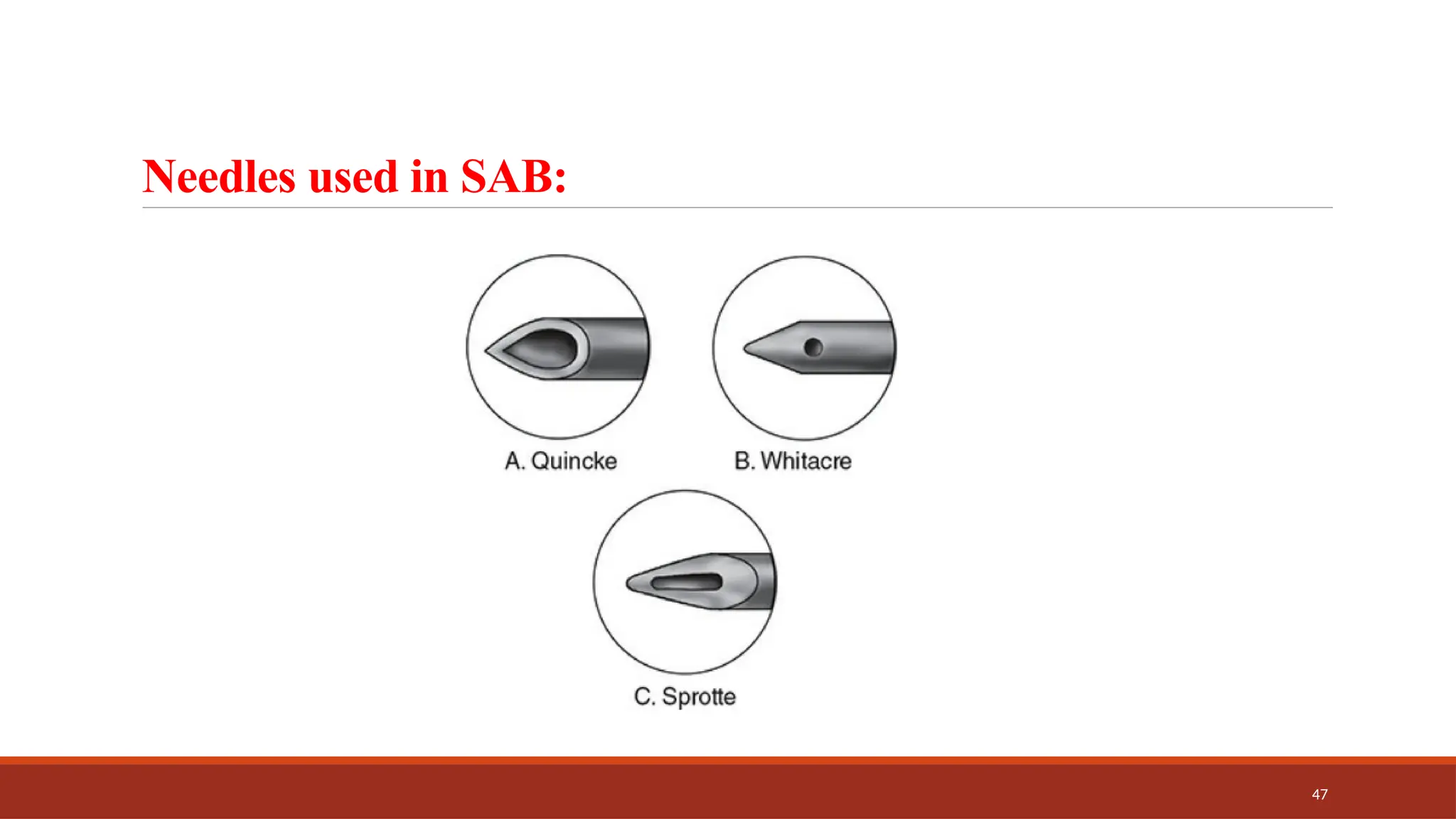
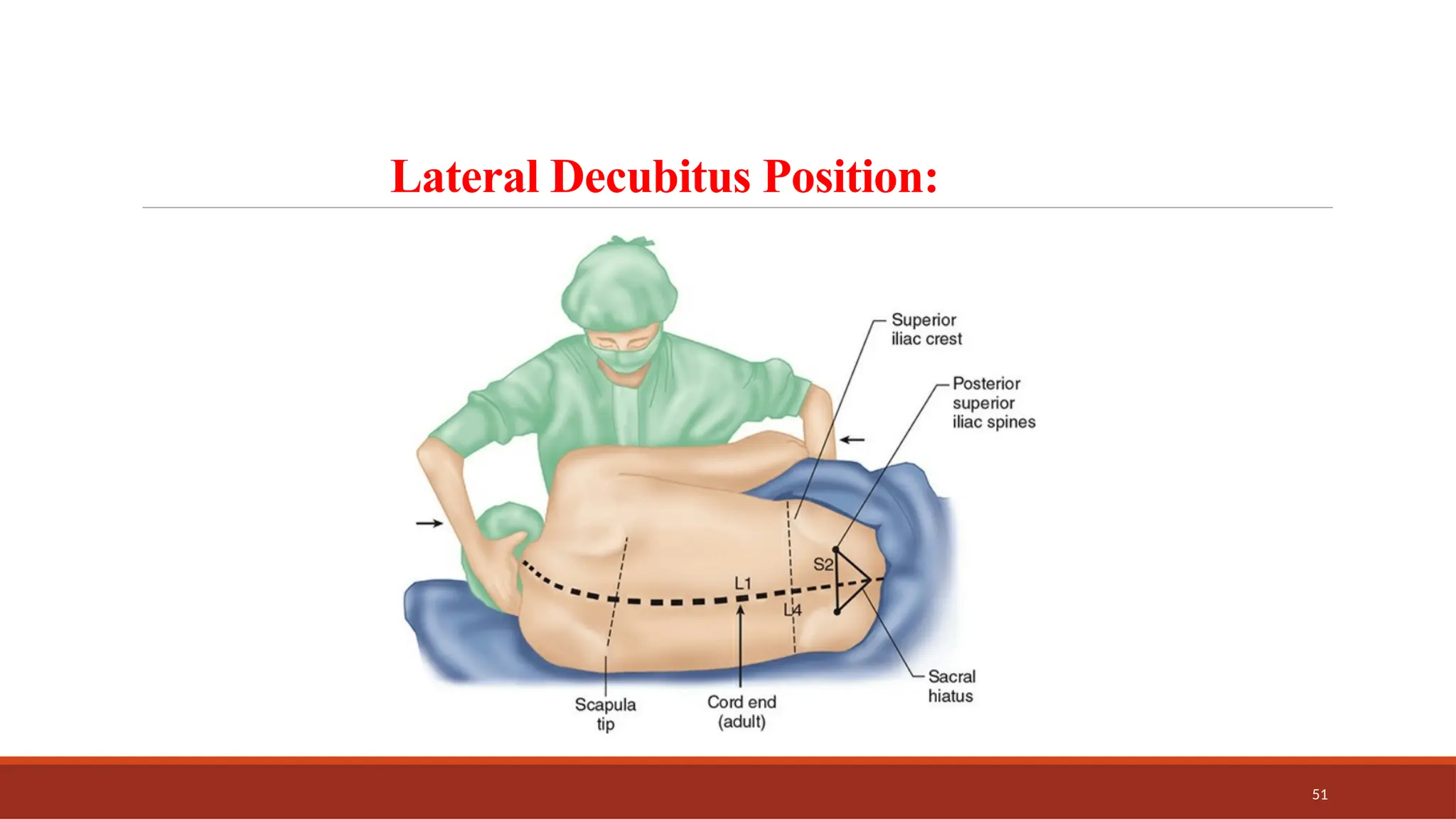
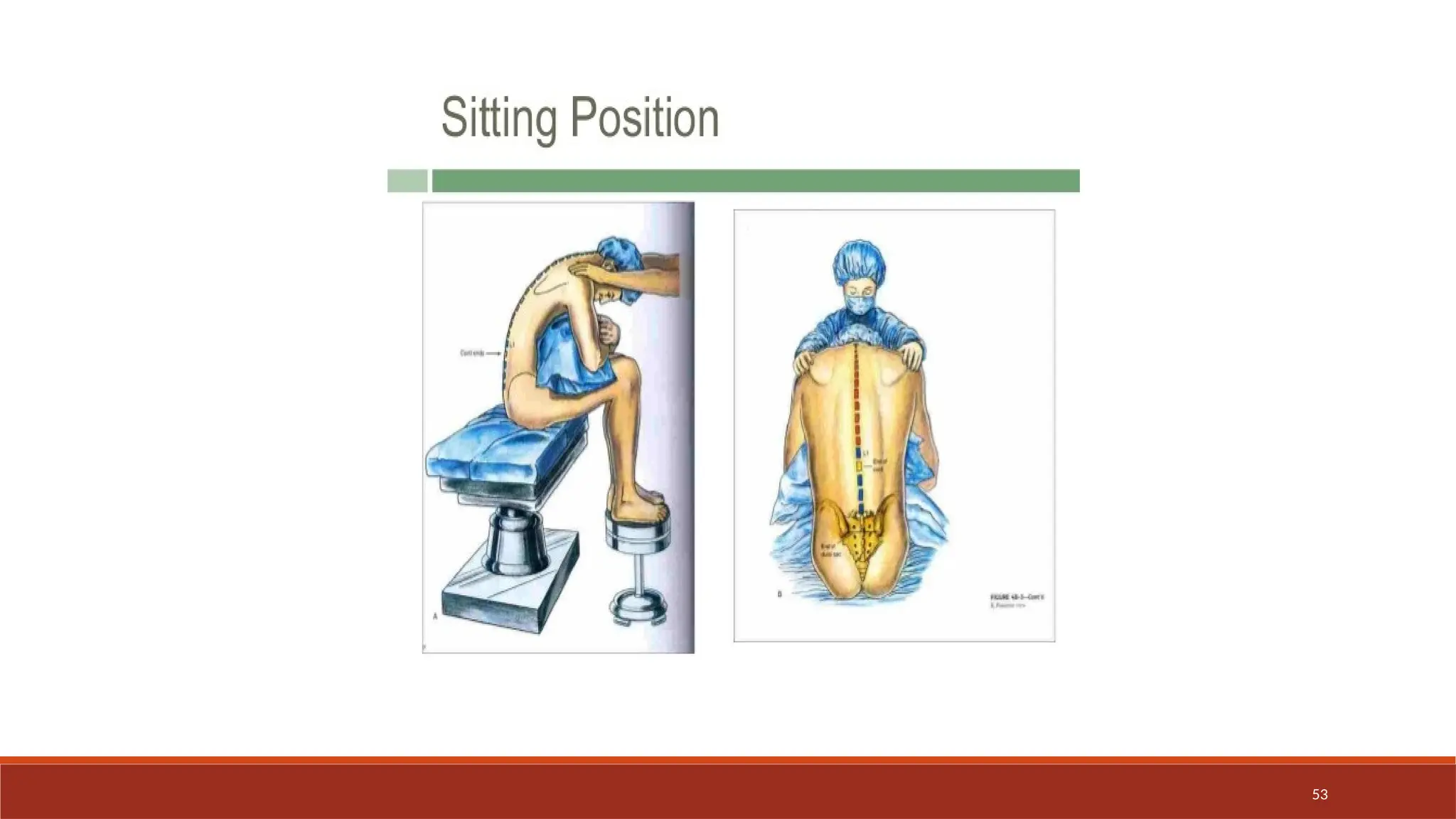
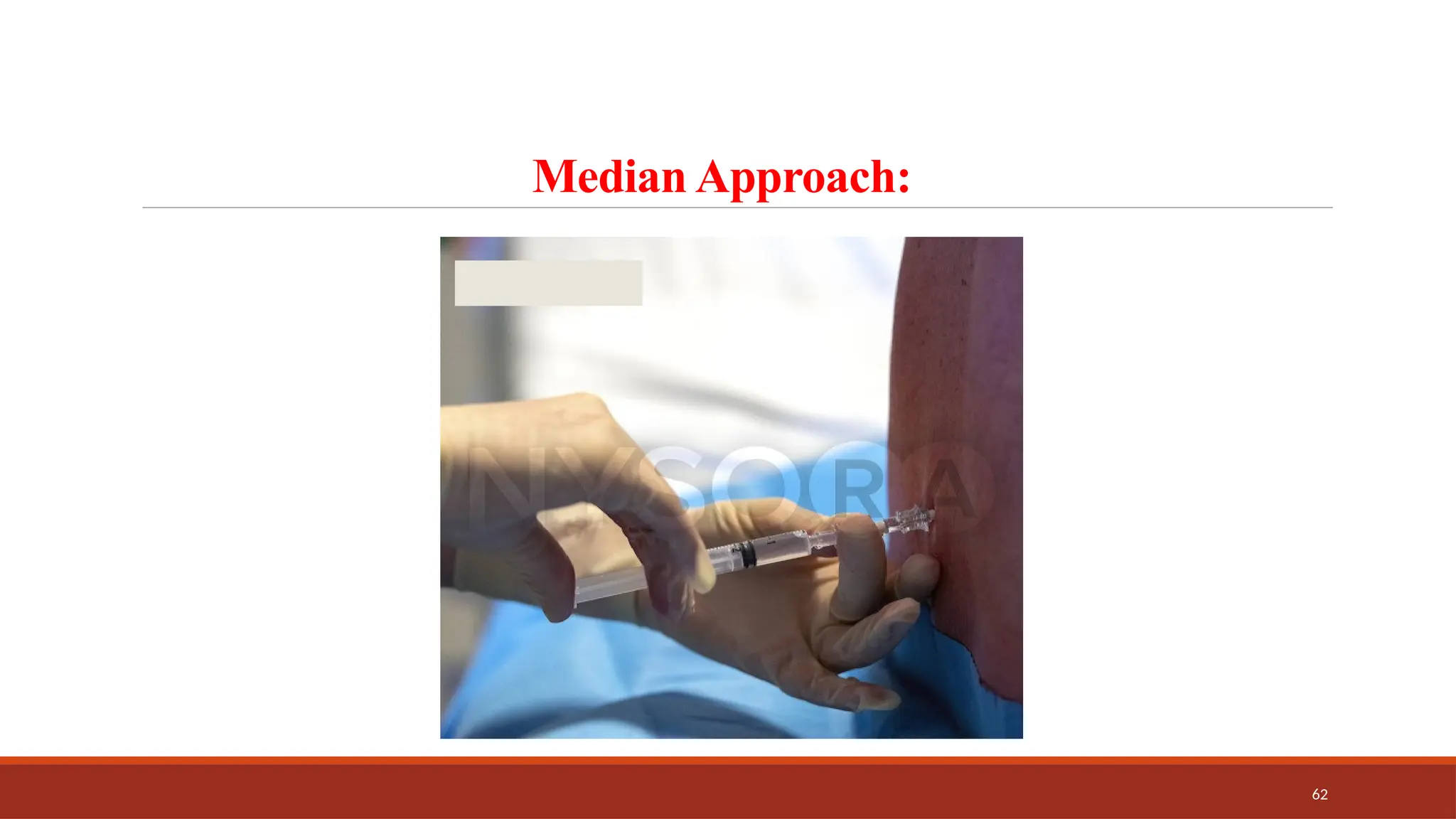
The document provides an overview of spinal anesthesia, detailing its history, anatomy, procedures, and factors affecting its application. It discusses the types of needles used, indications and contraindications for spinal anesthesia, and the physiological effects on various body systems. The document also emphasizes the importance of patient positioning and the techniques involved in lumbar puncture for effective administration of spinal anesthetics.