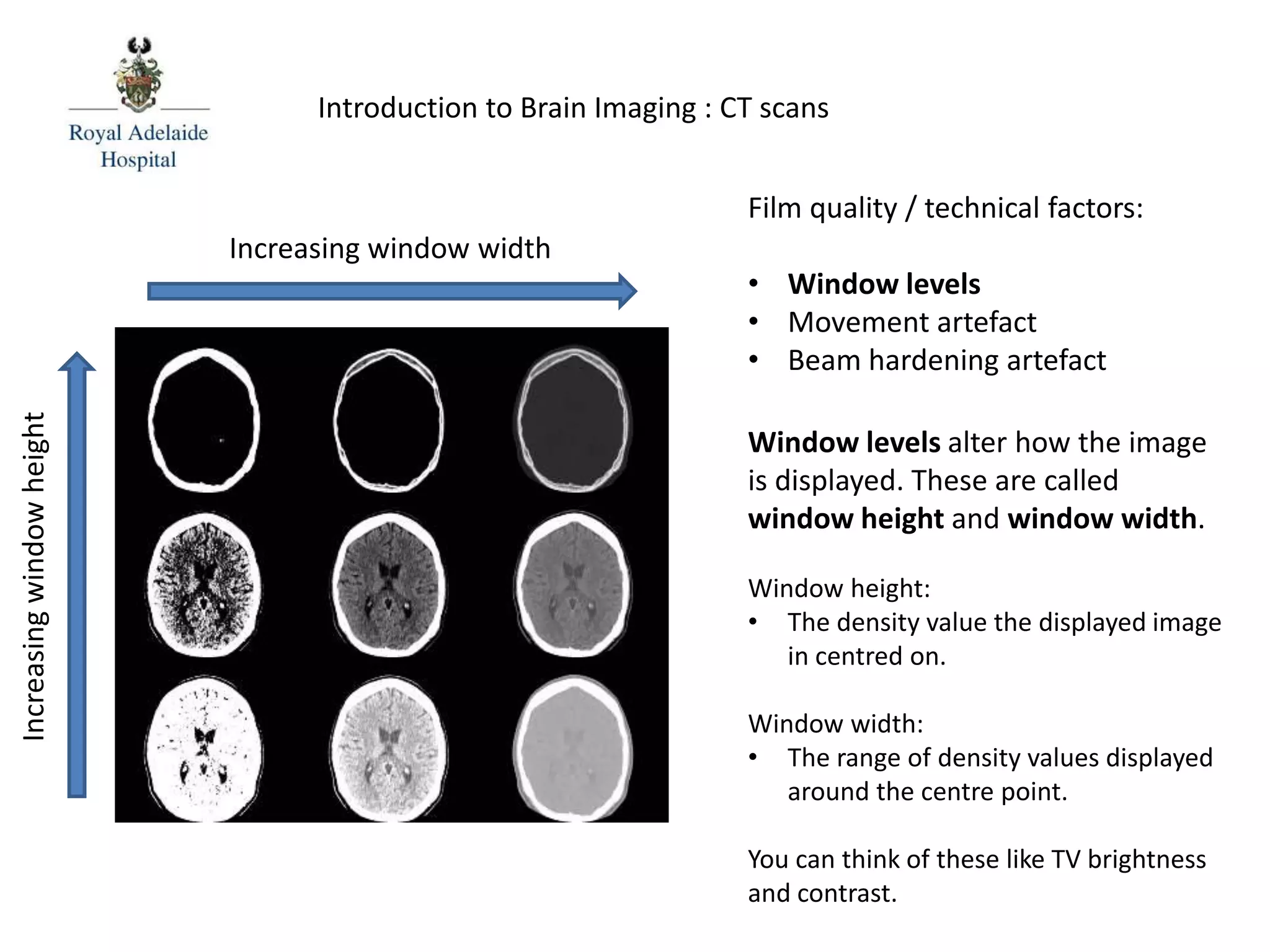
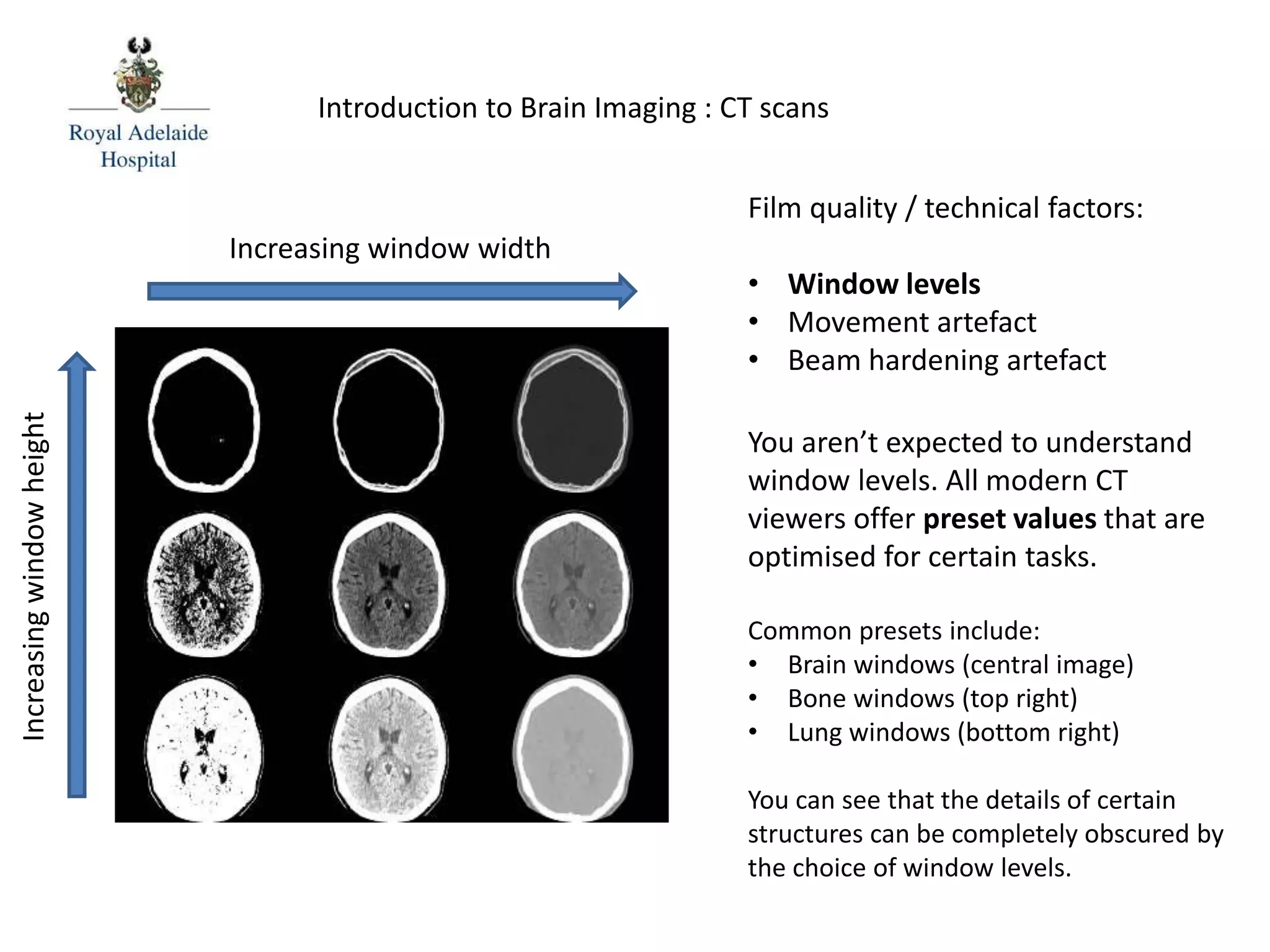
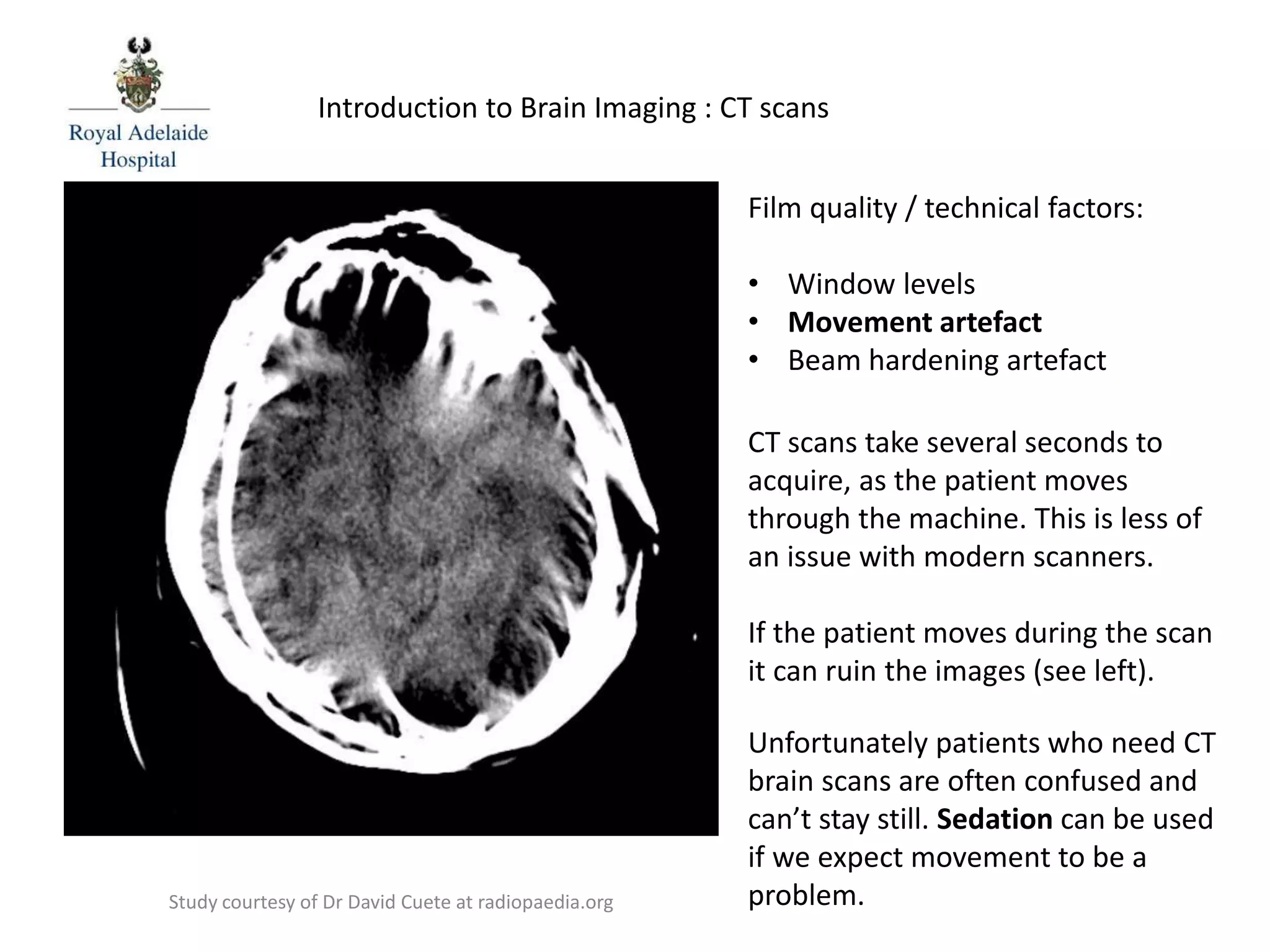
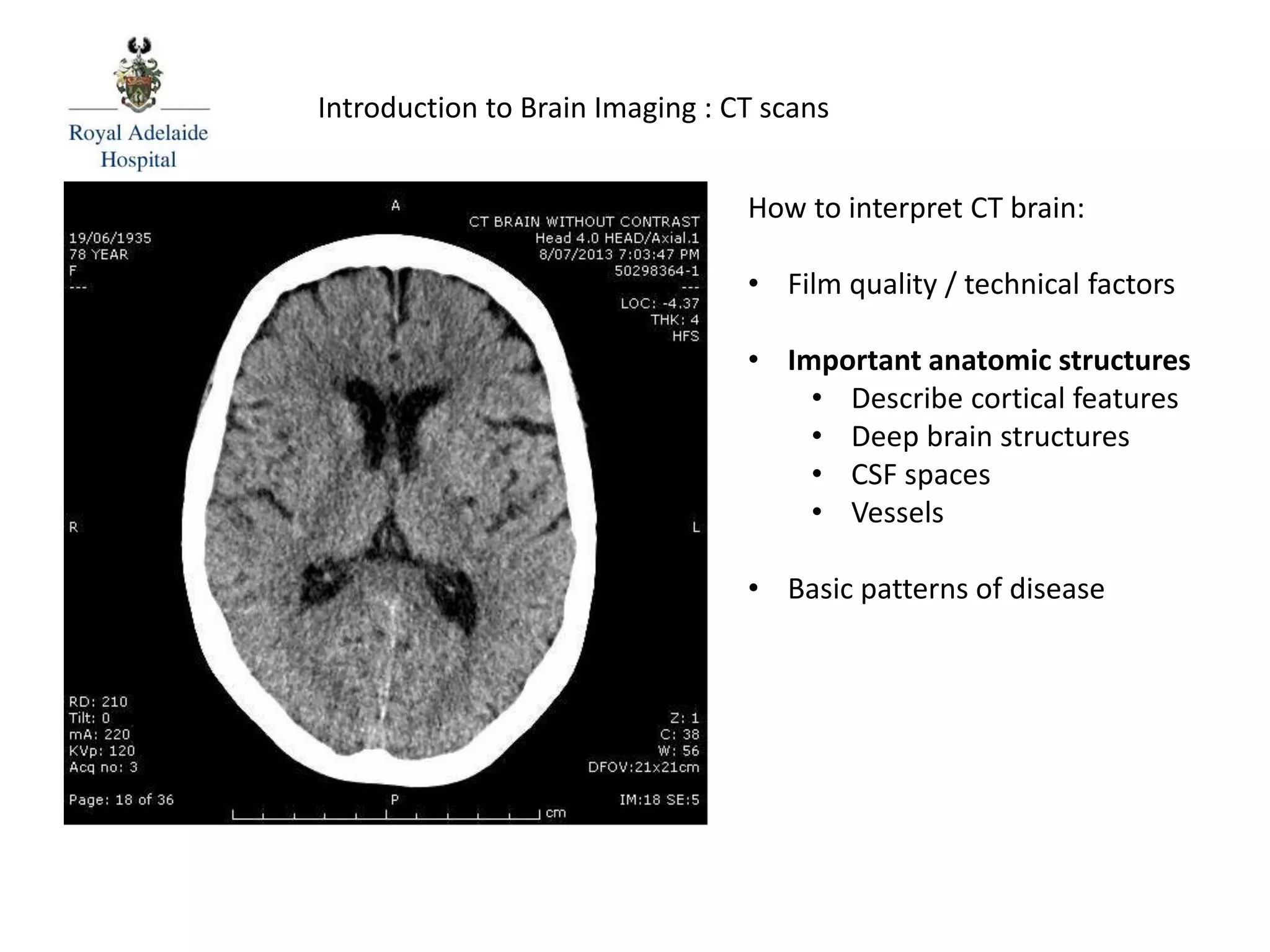
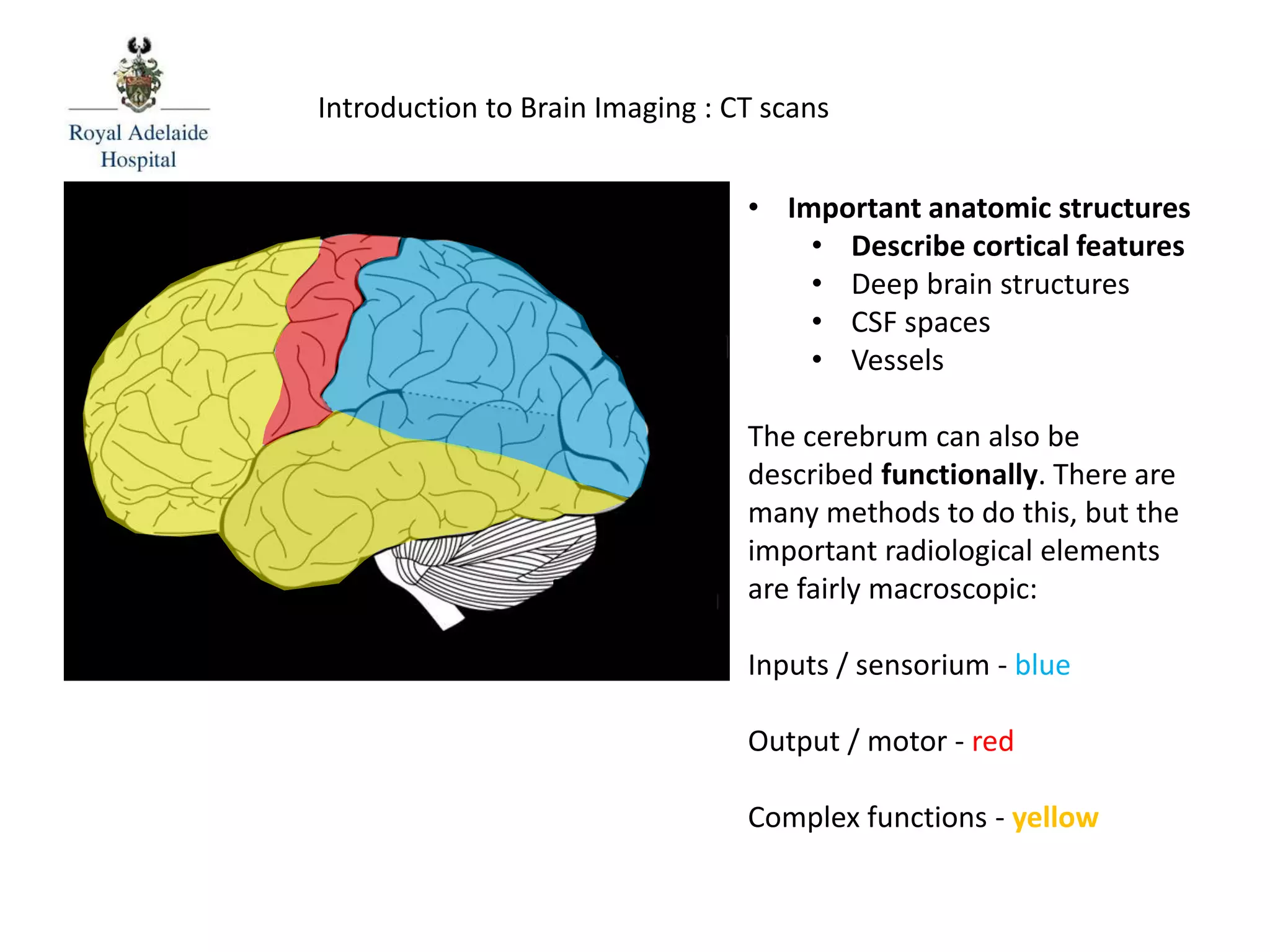
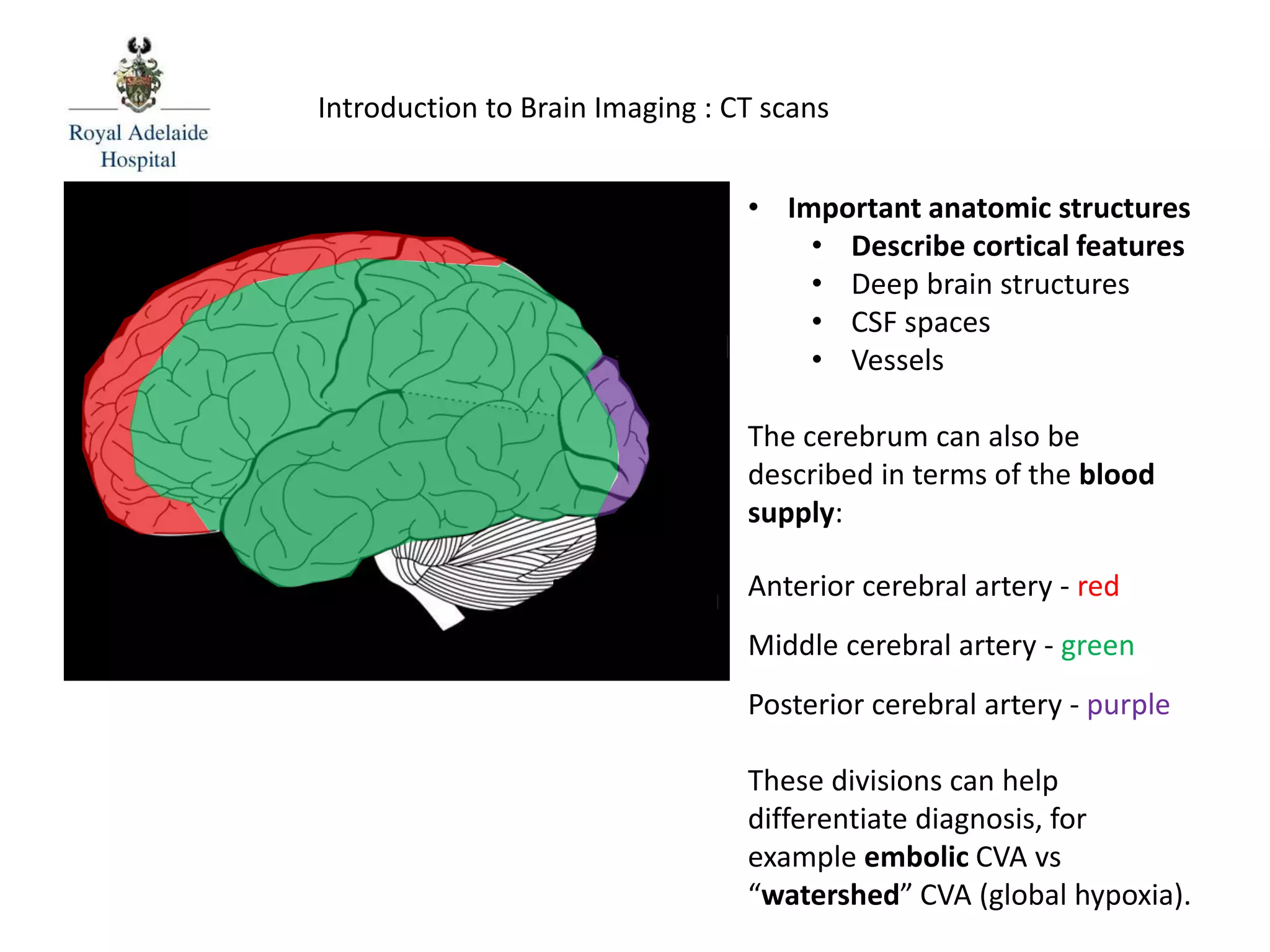
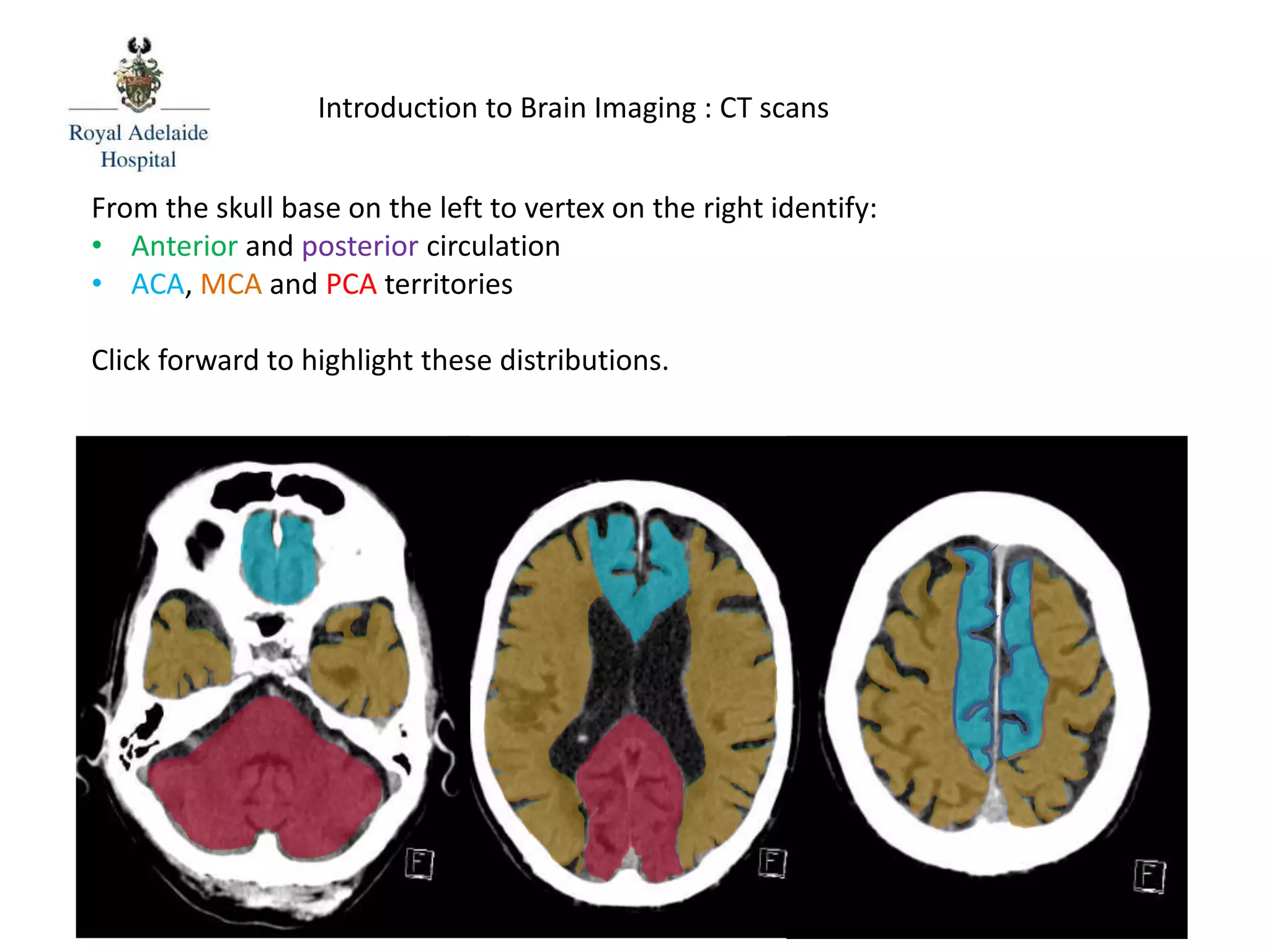
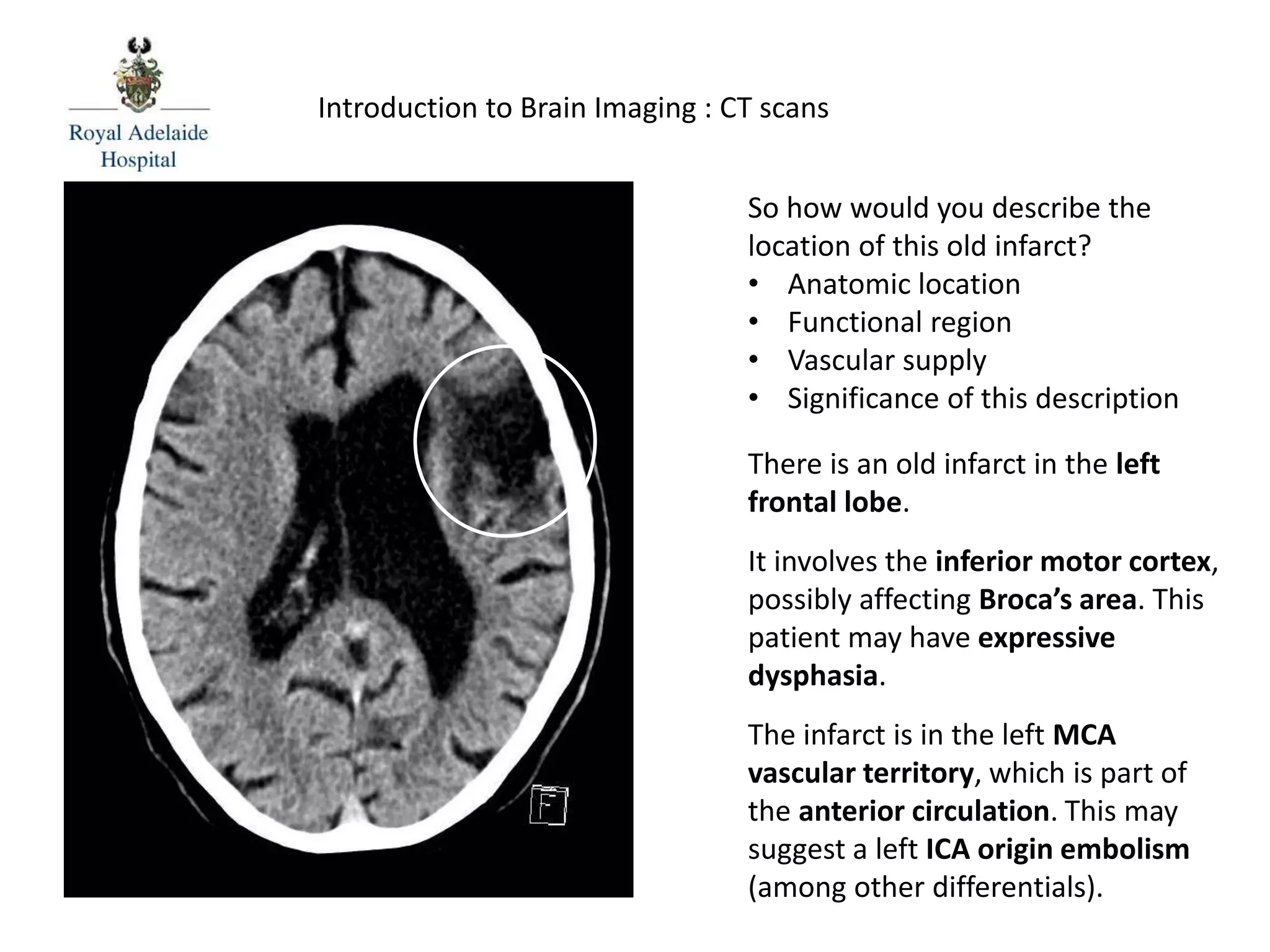
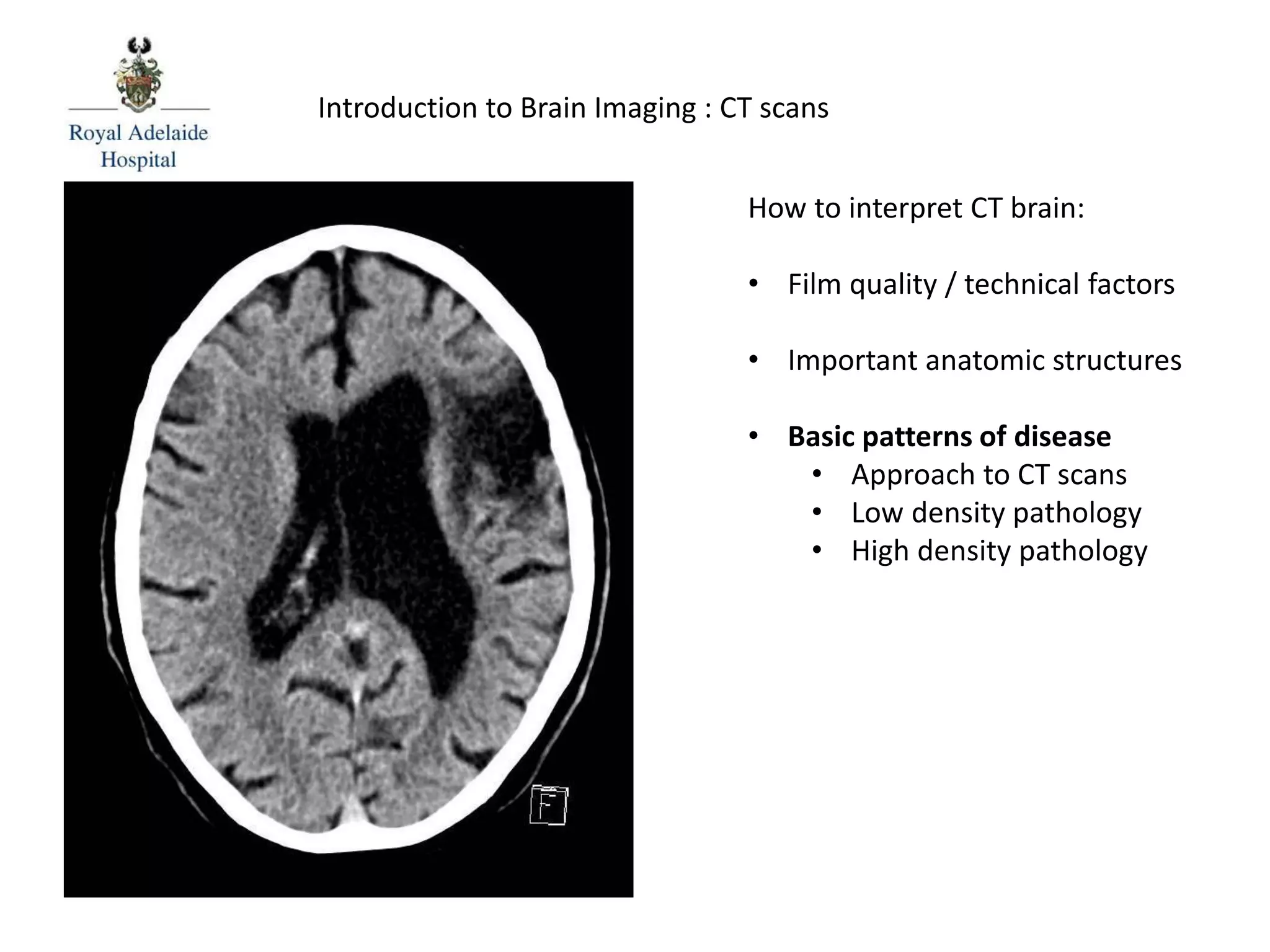
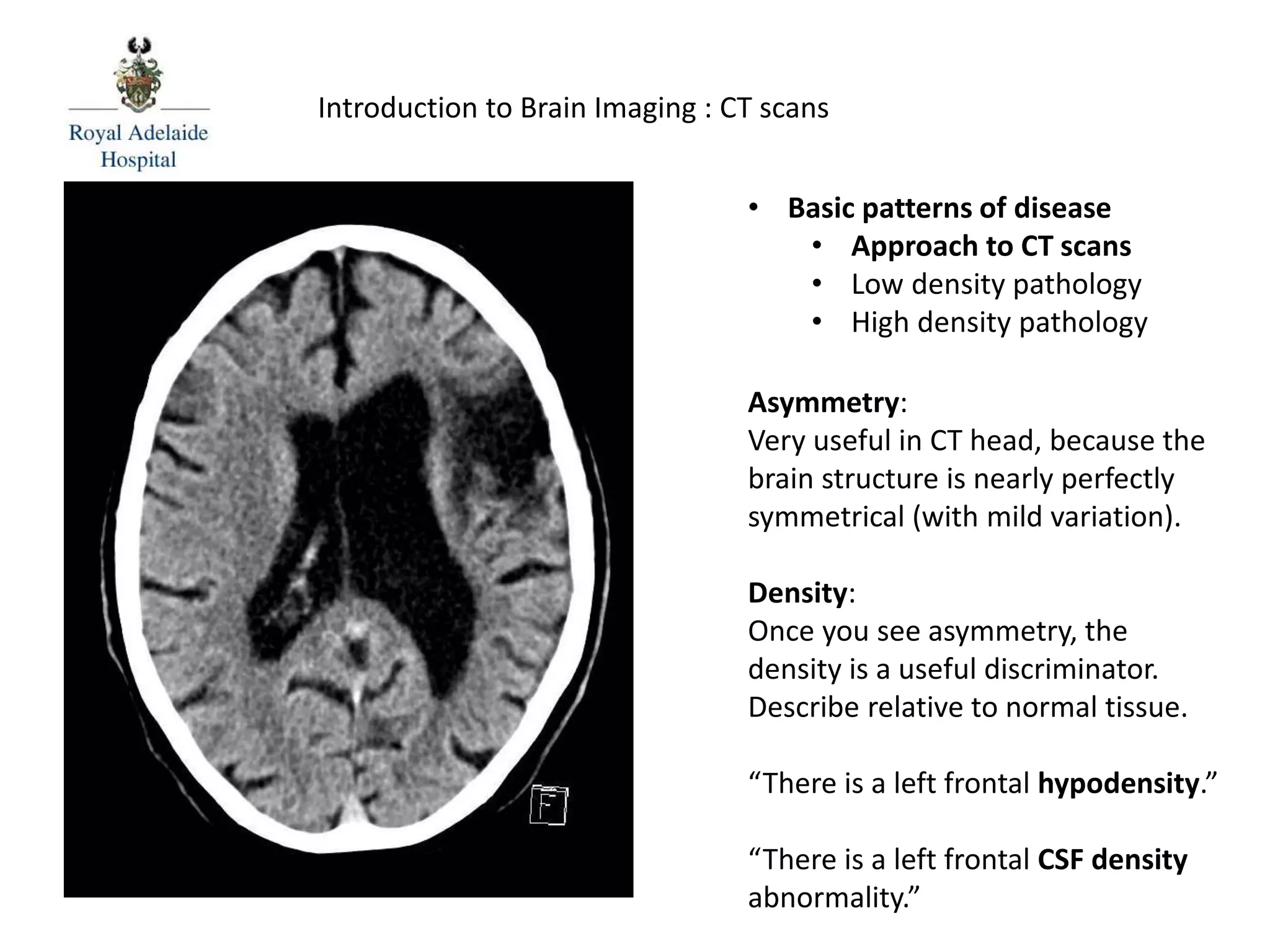
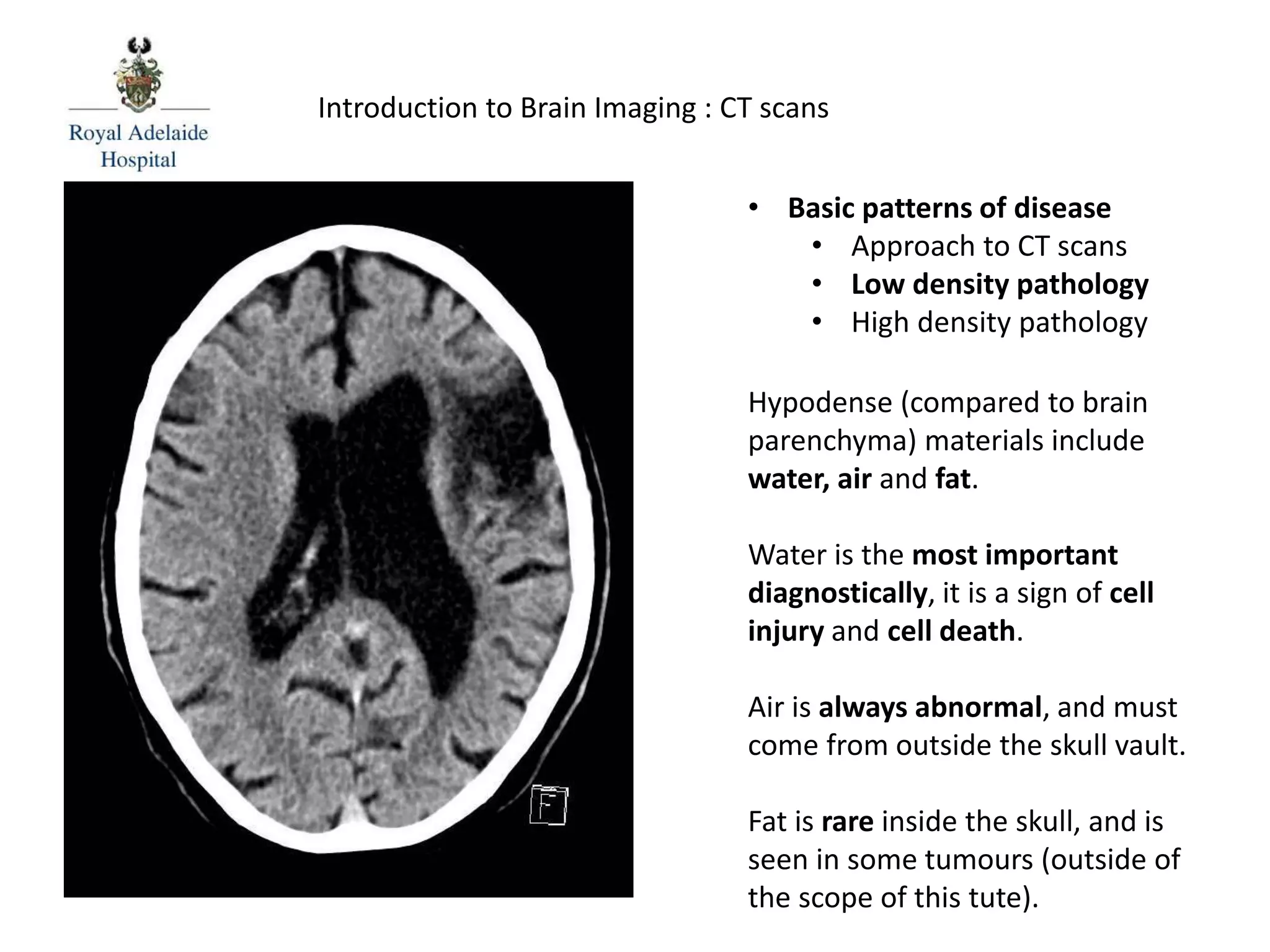
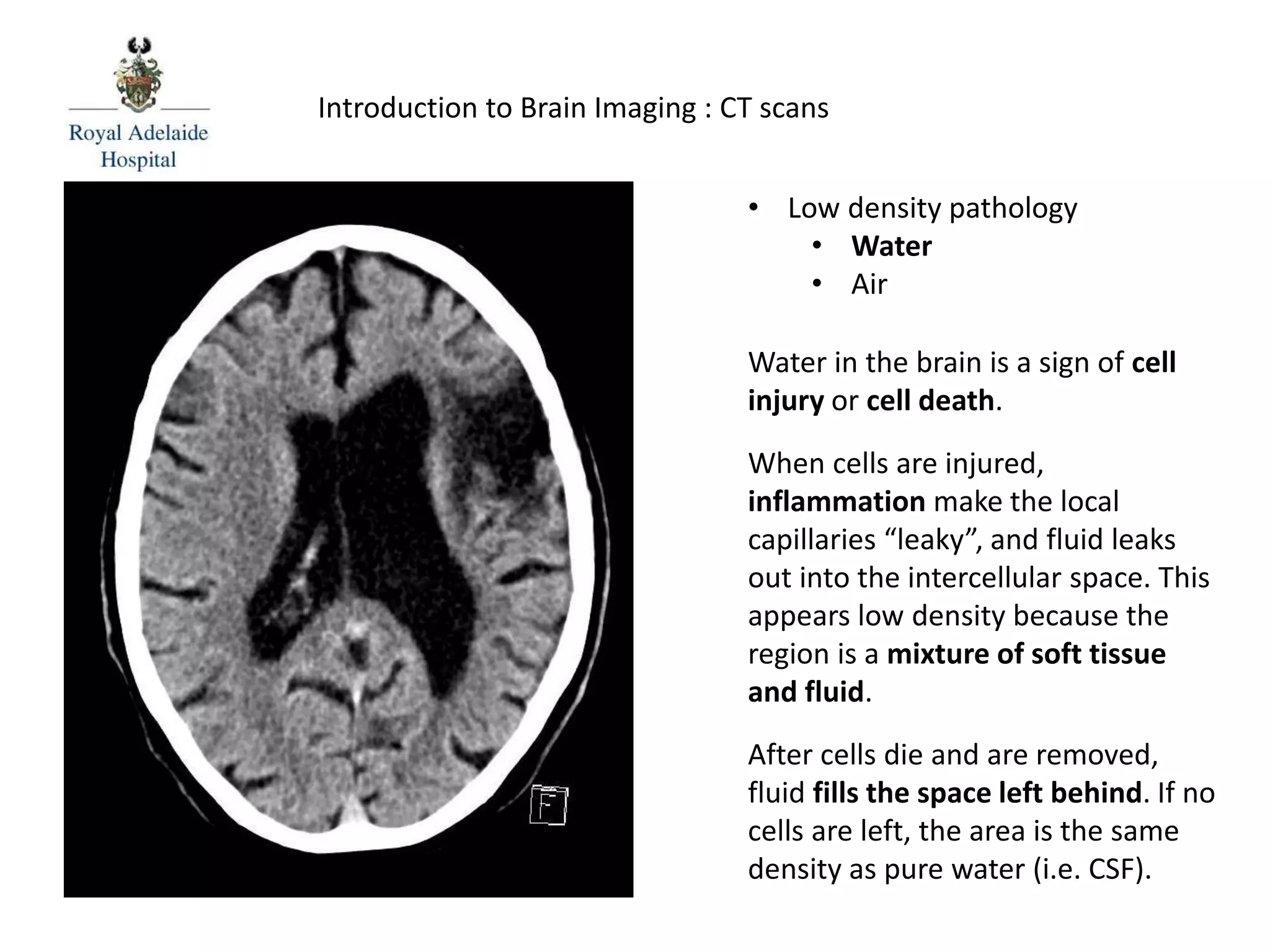
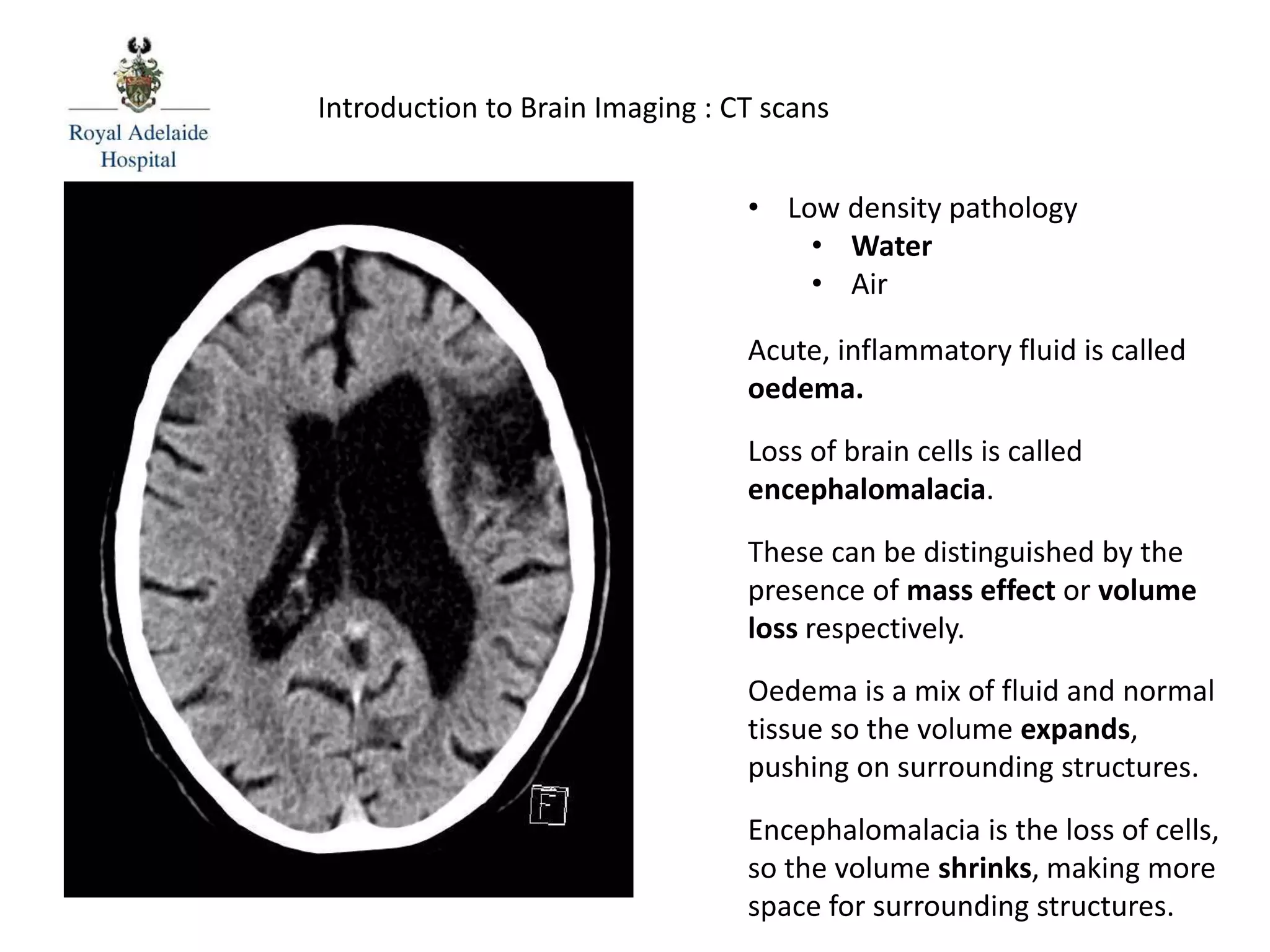
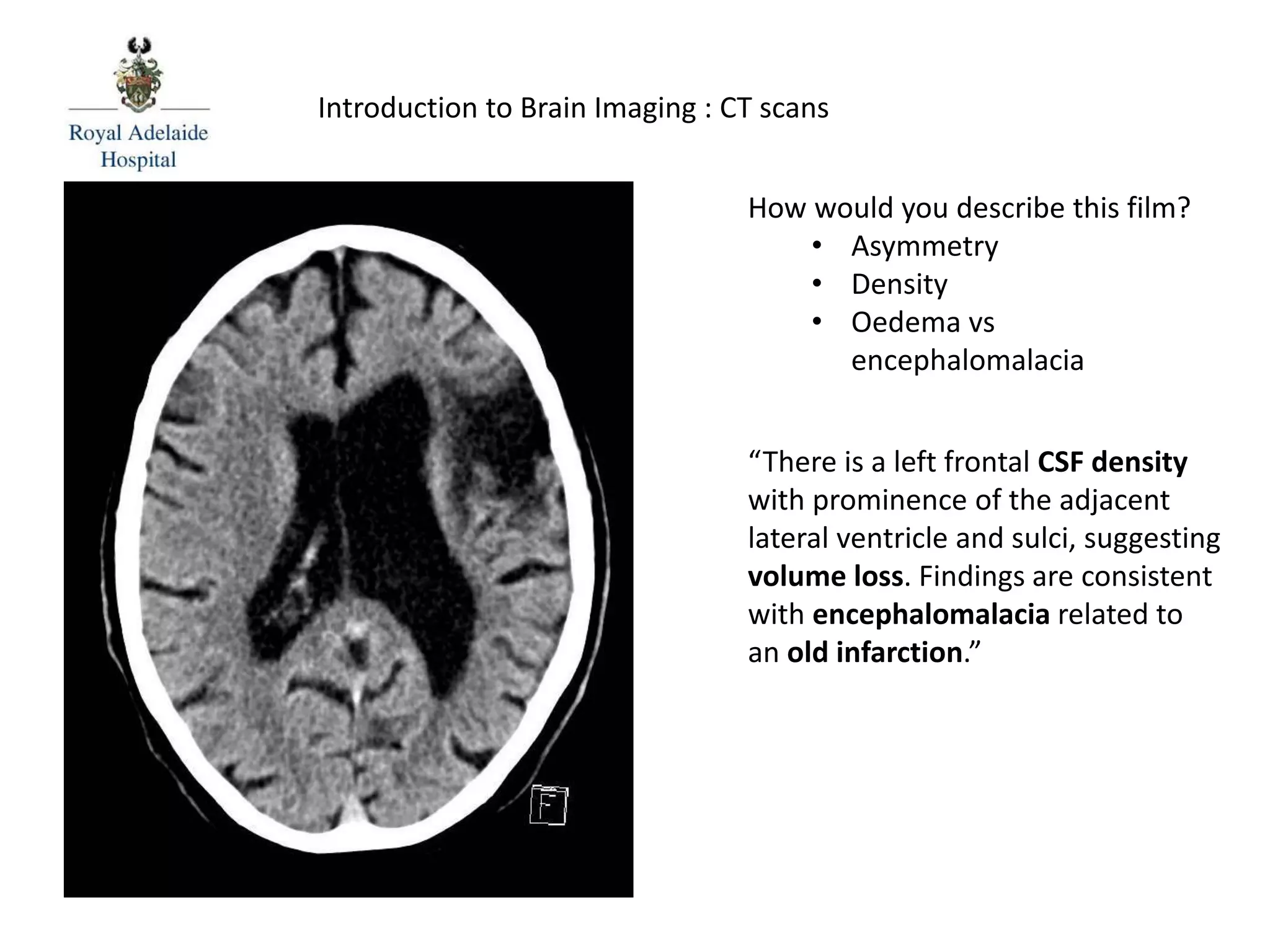
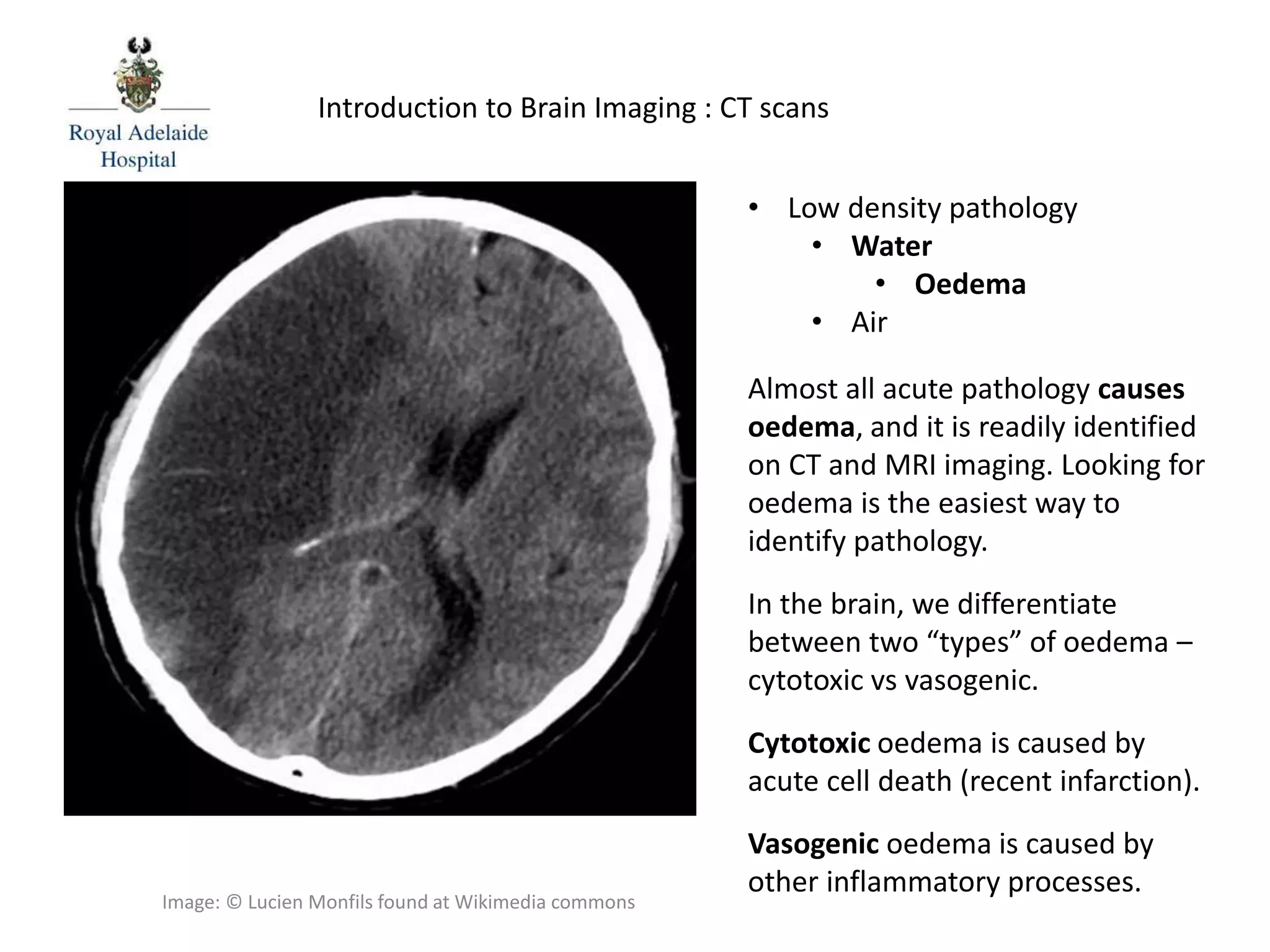
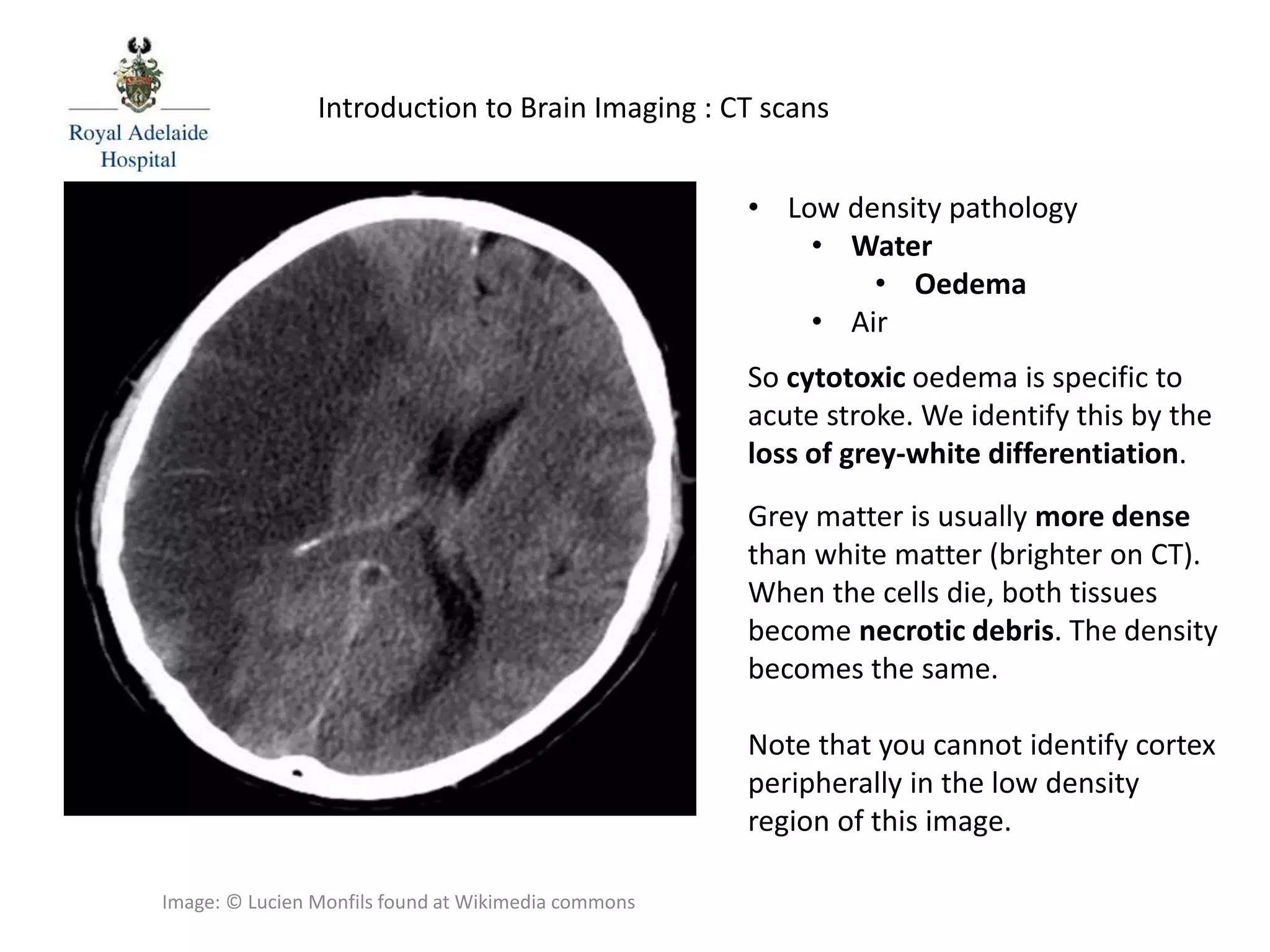
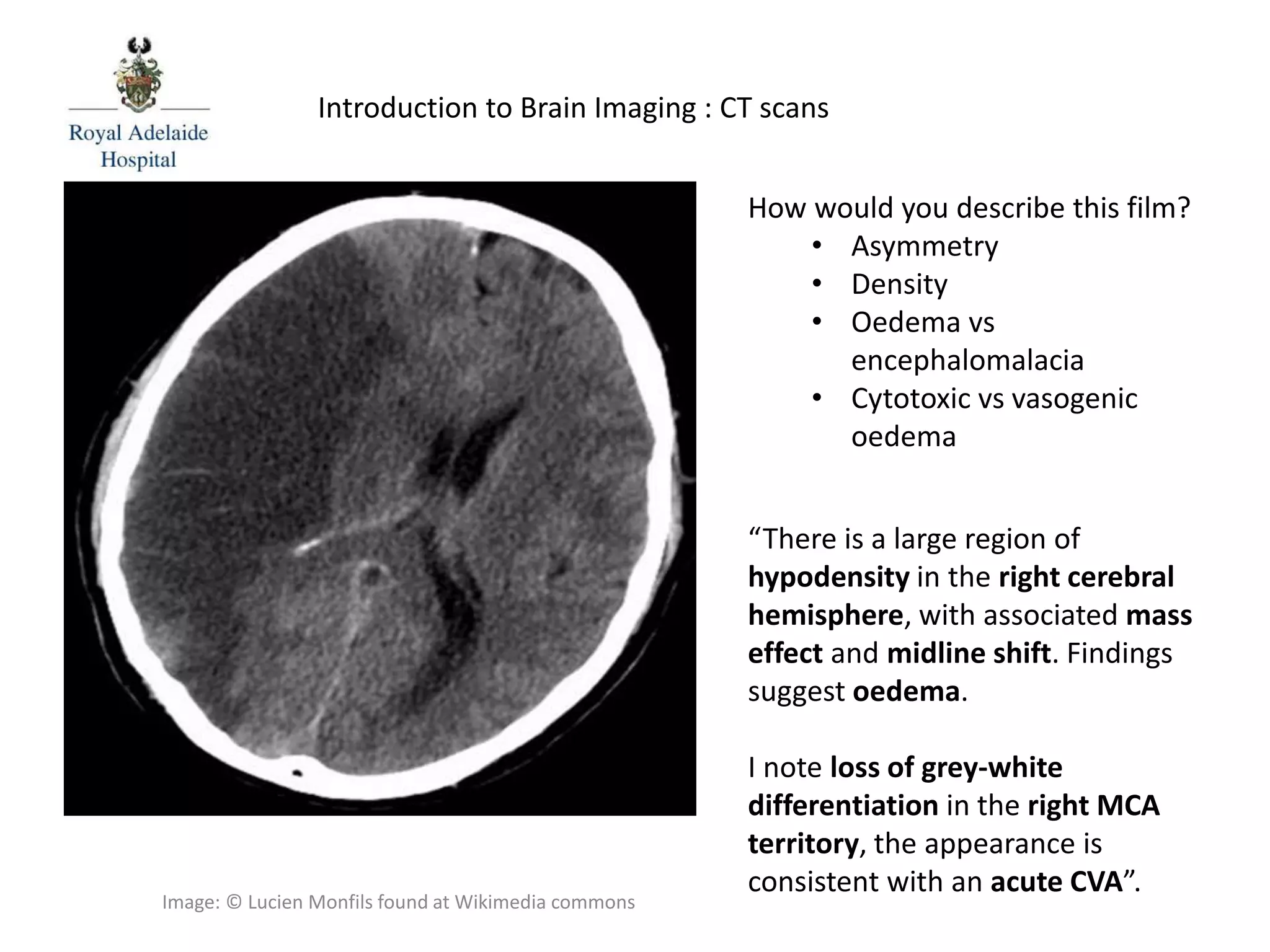
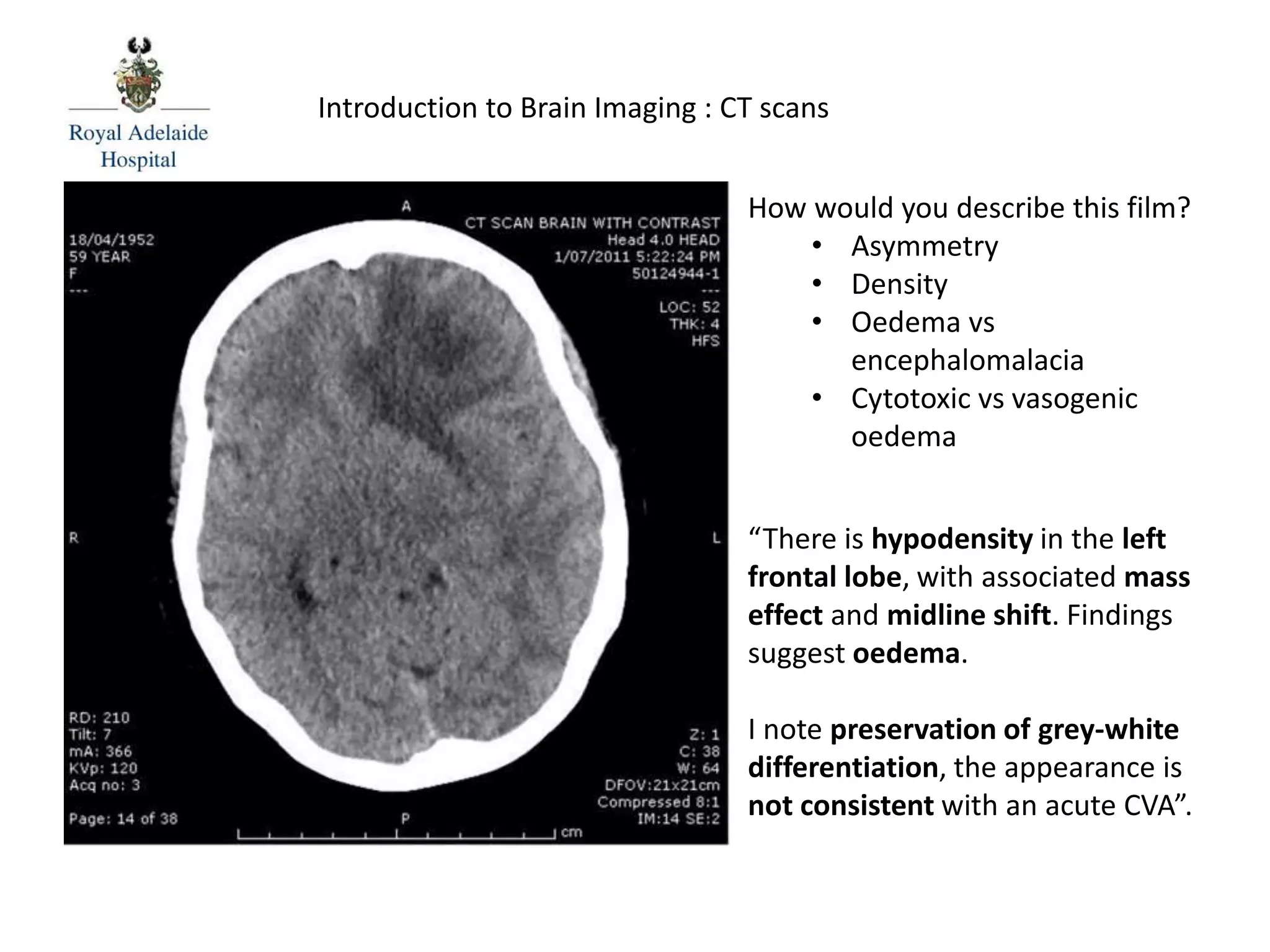
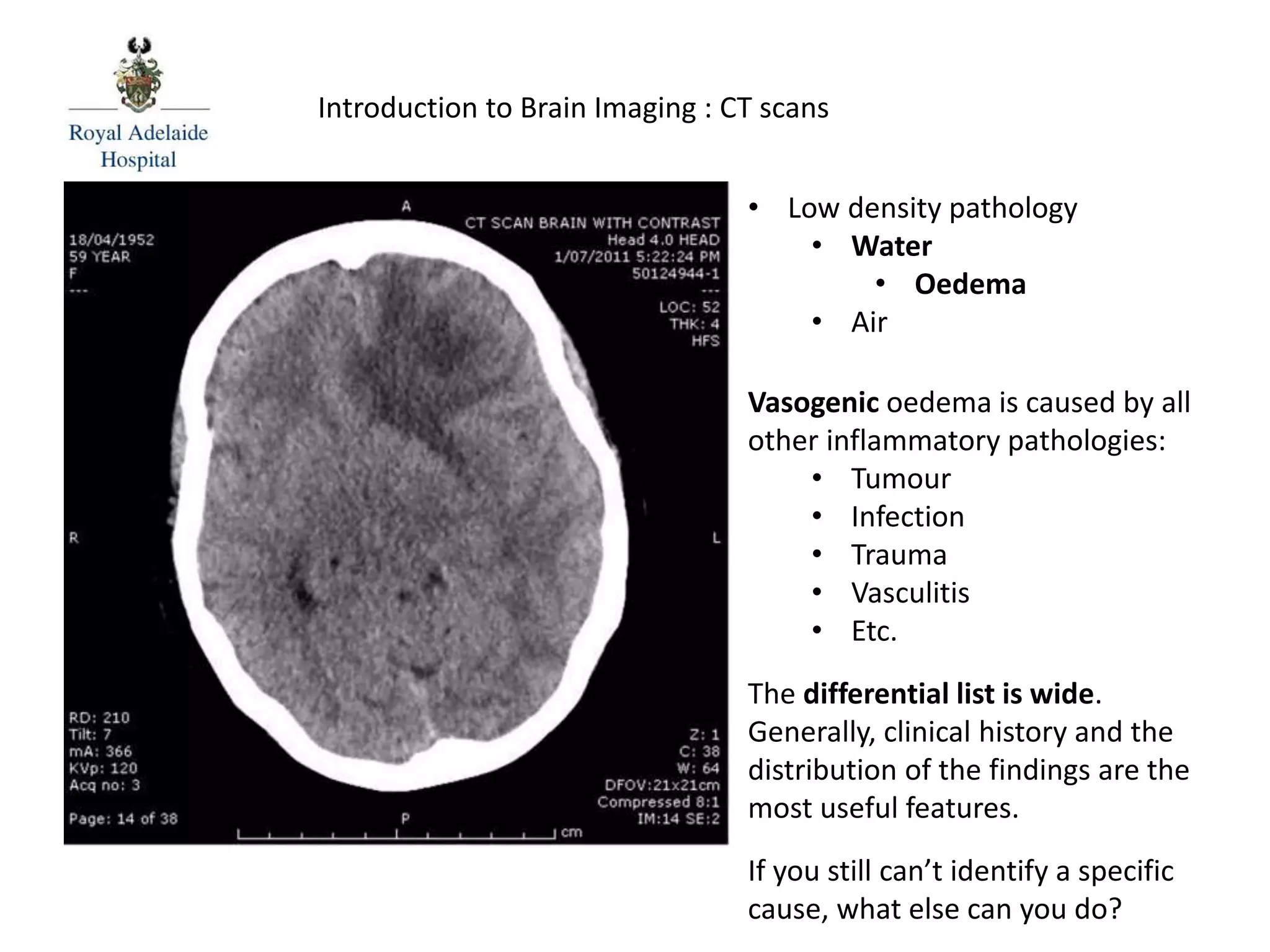
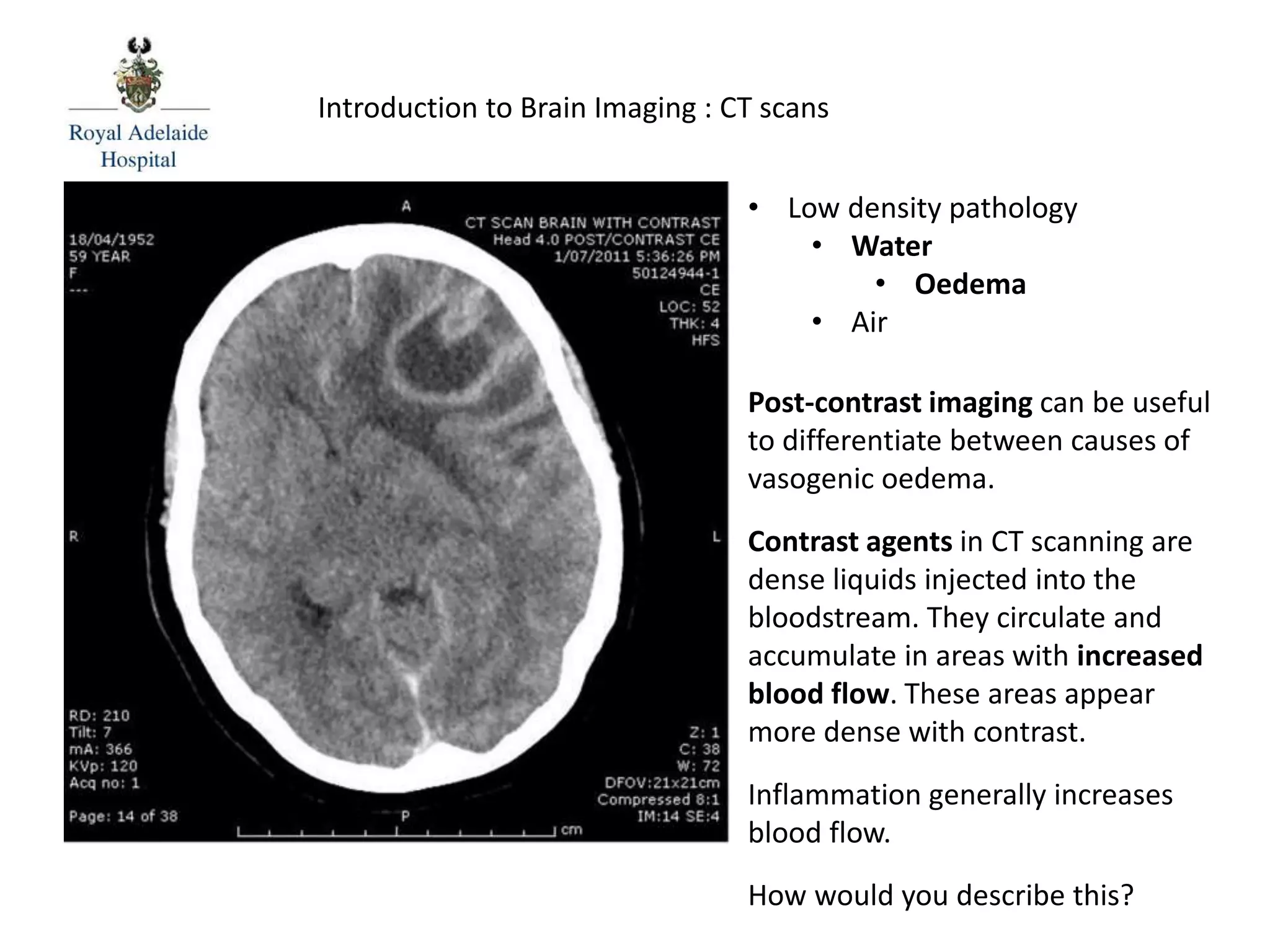
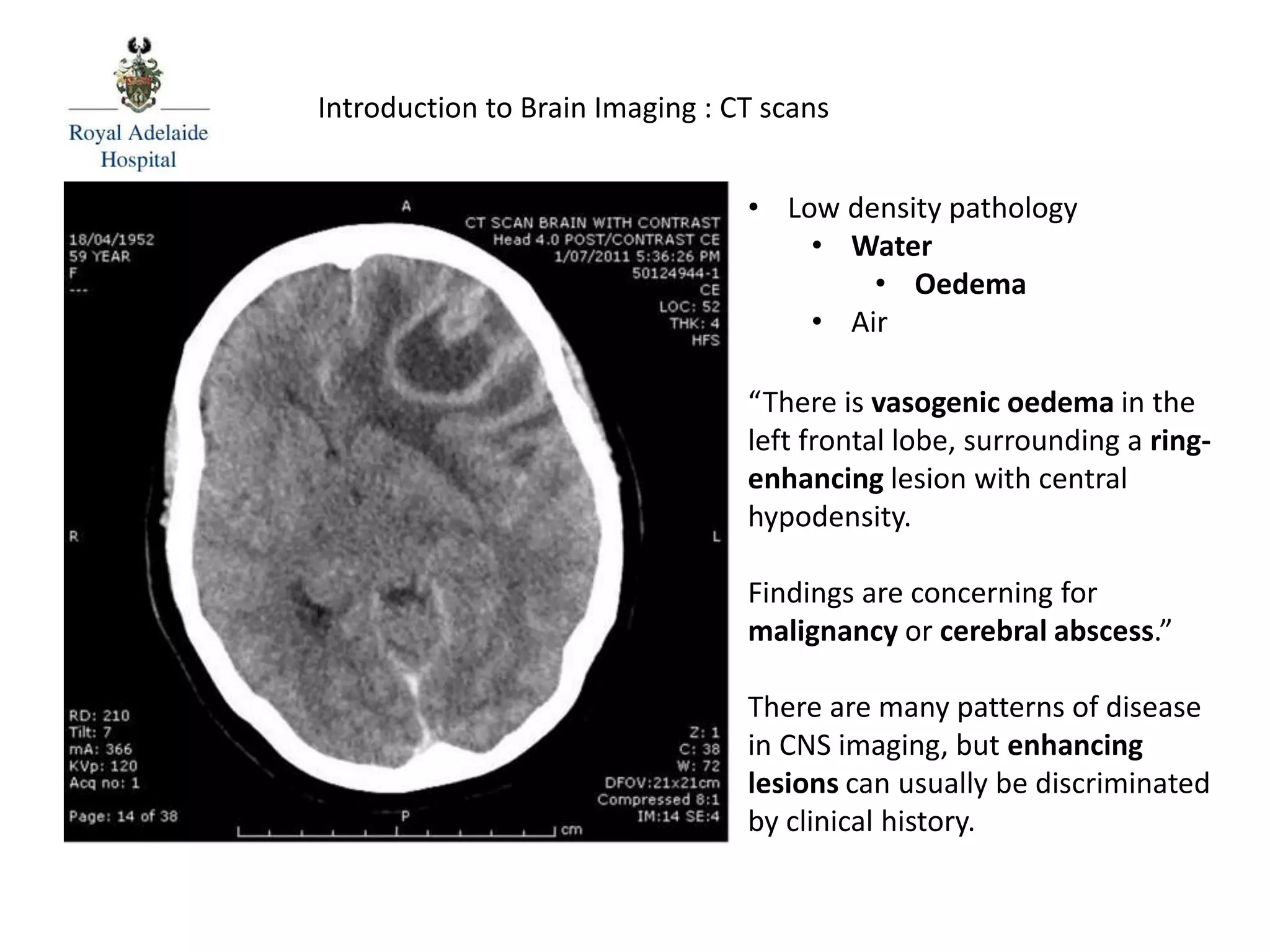
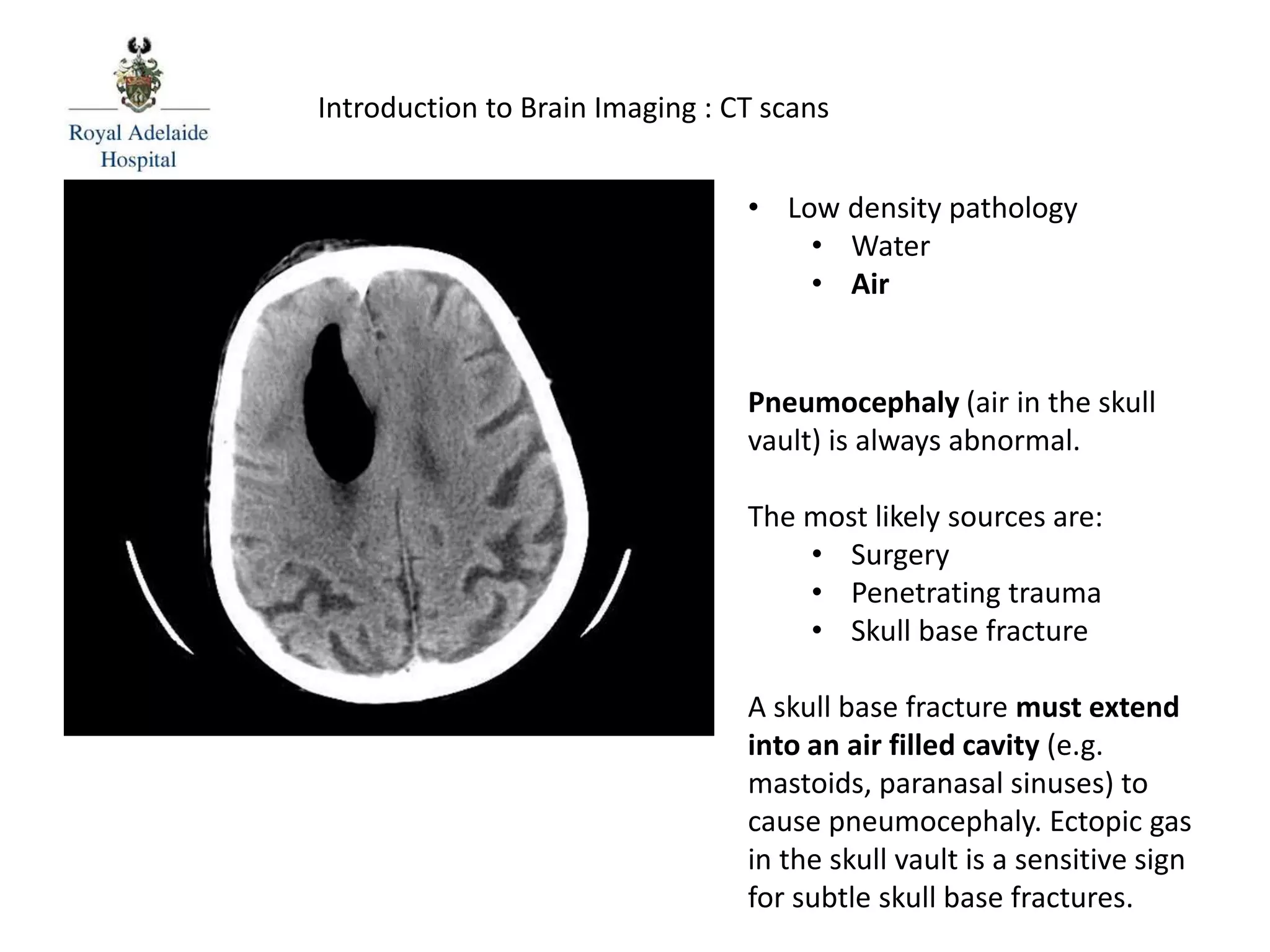
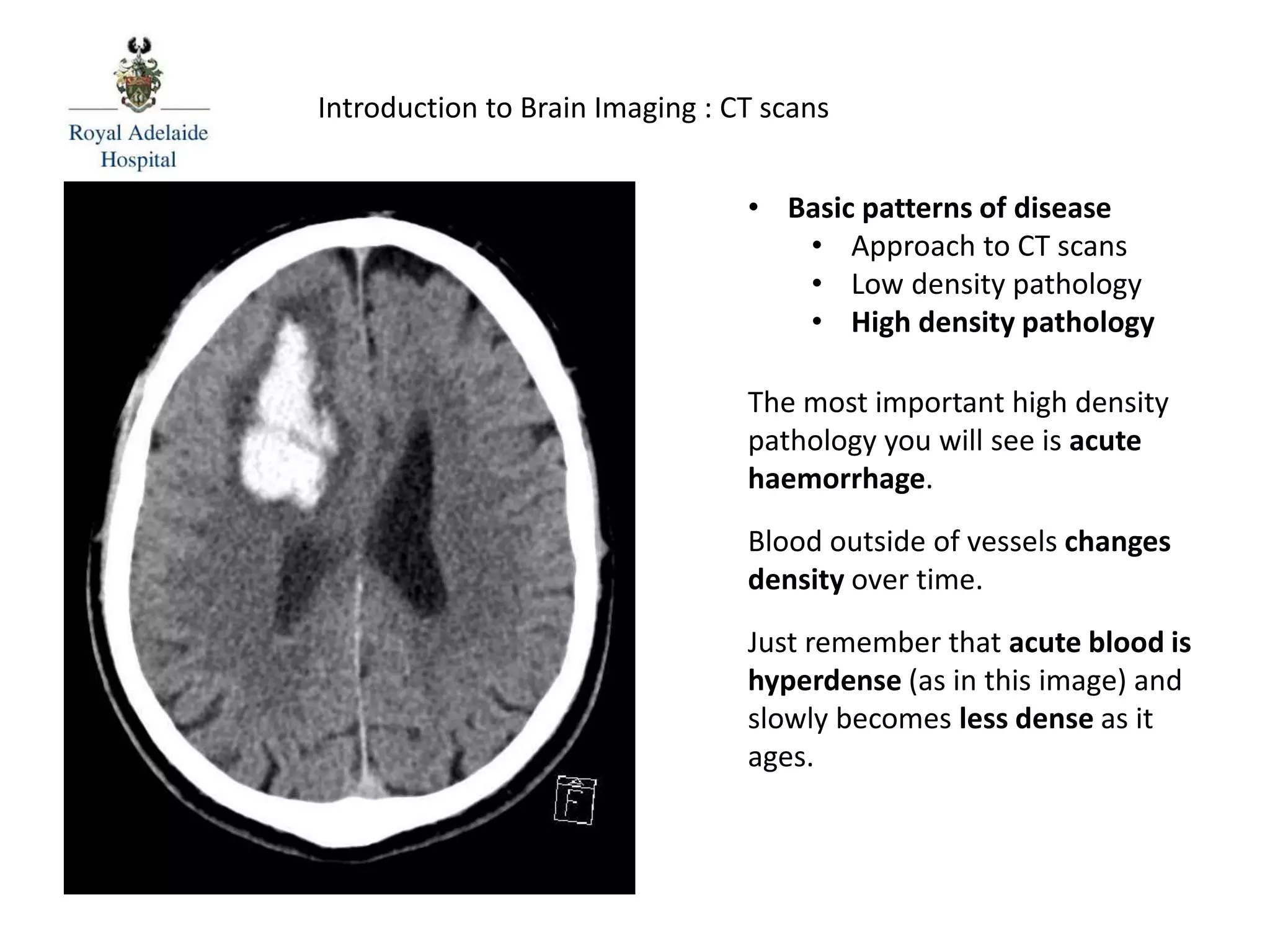
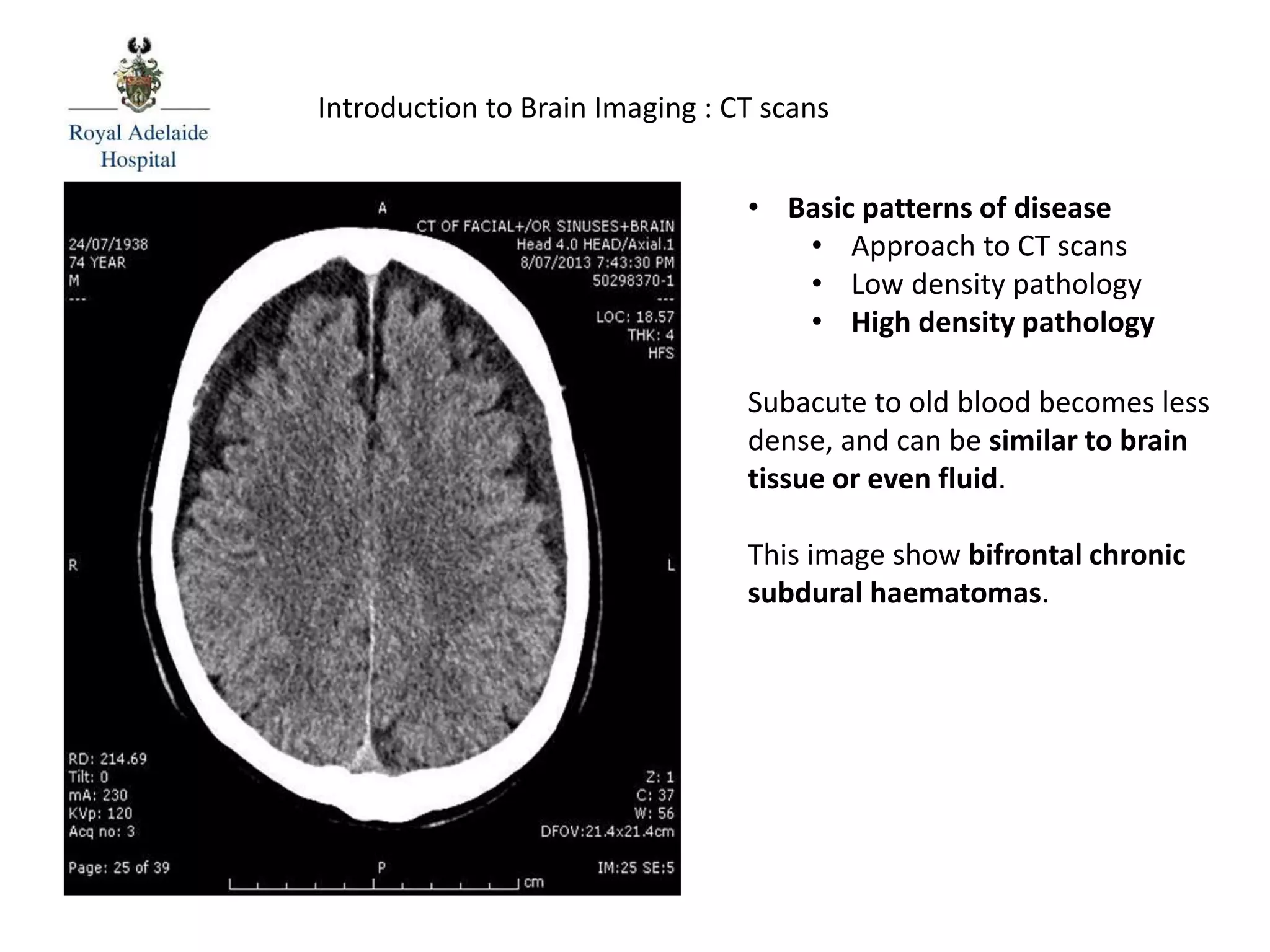
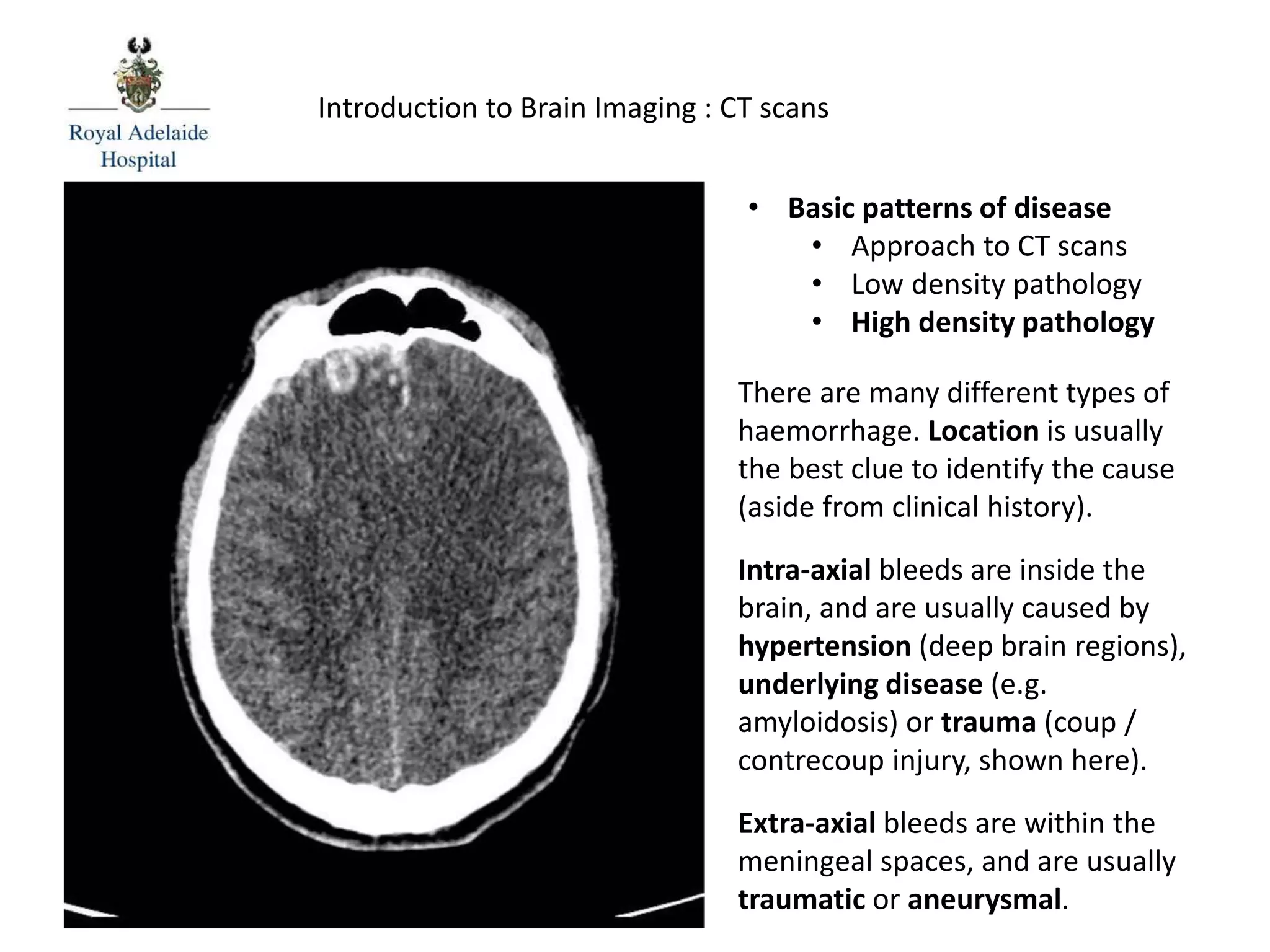
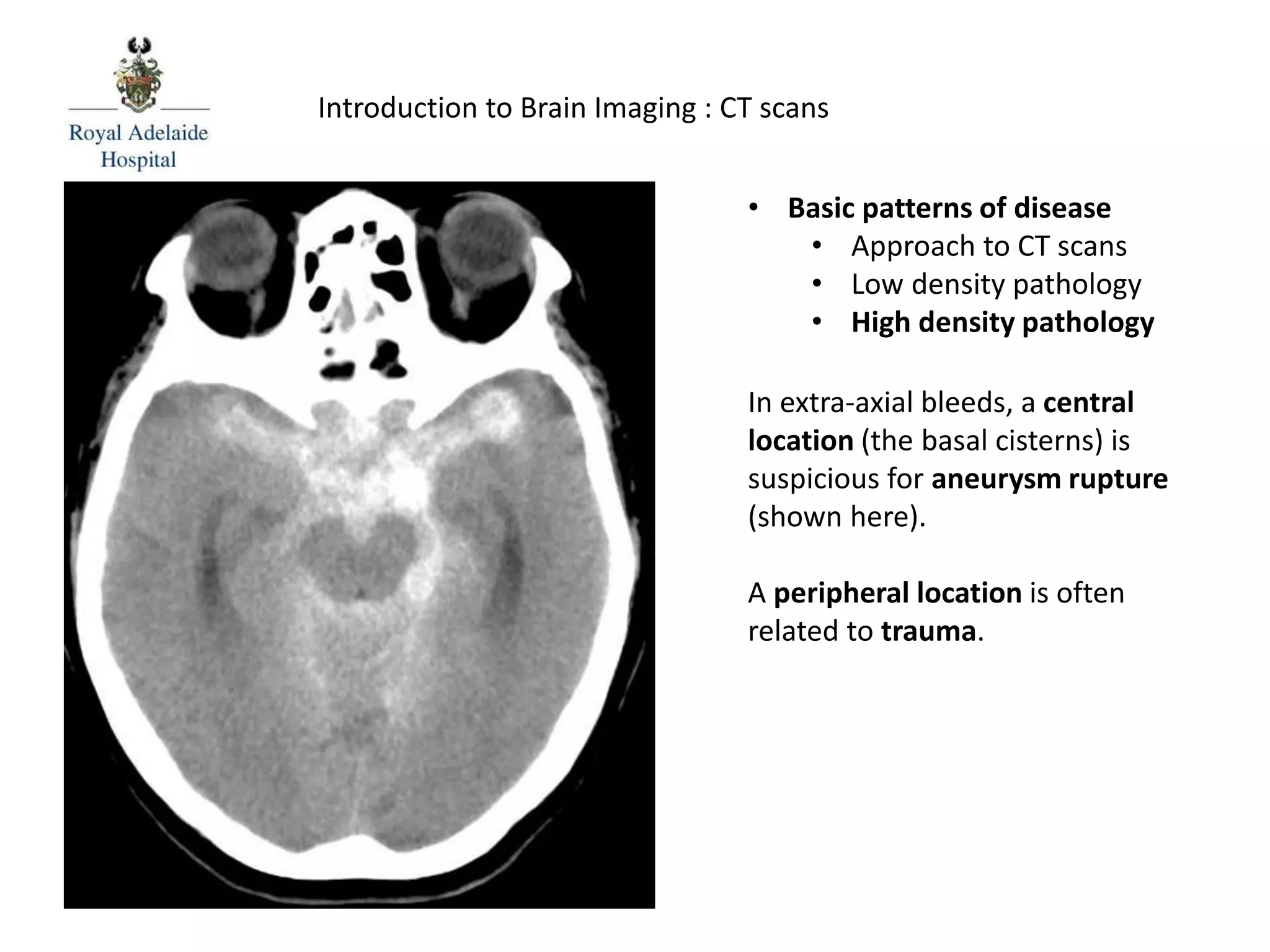
The document serves as an introductory guide to interpreting CT scans of the brain, covering essential concepts like film quality, window levels, movement artifacts, and basic patterns of disease. It explains the anatomical and functional organization of the cerebrum, emphasizing the importance of describing structures based on location, function, and blood supply. Additionally, it outlines various forms of pathology, including low and high-density lesions, edema types, and the significance of vasogenic edema in differential diagnosis.