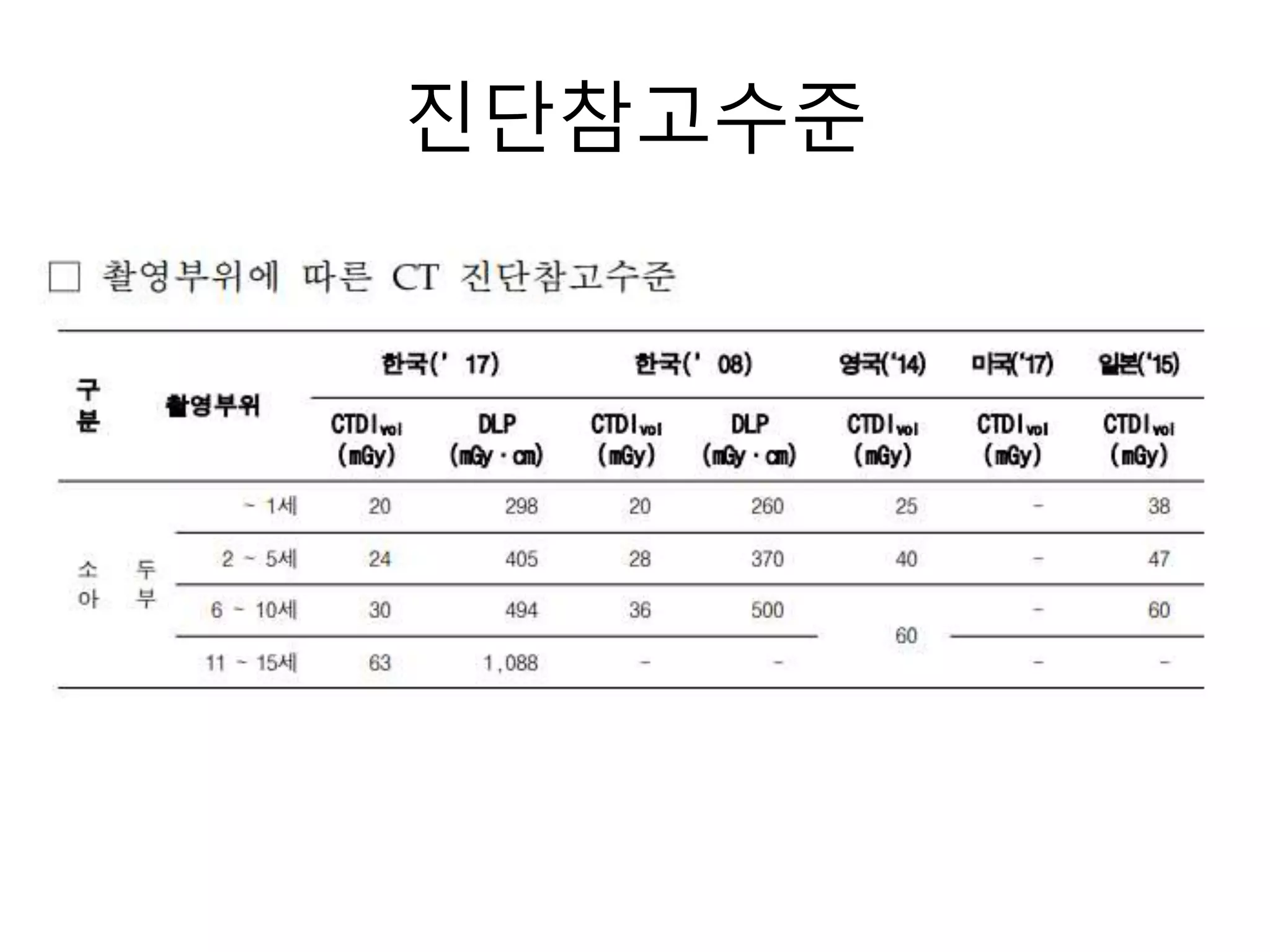
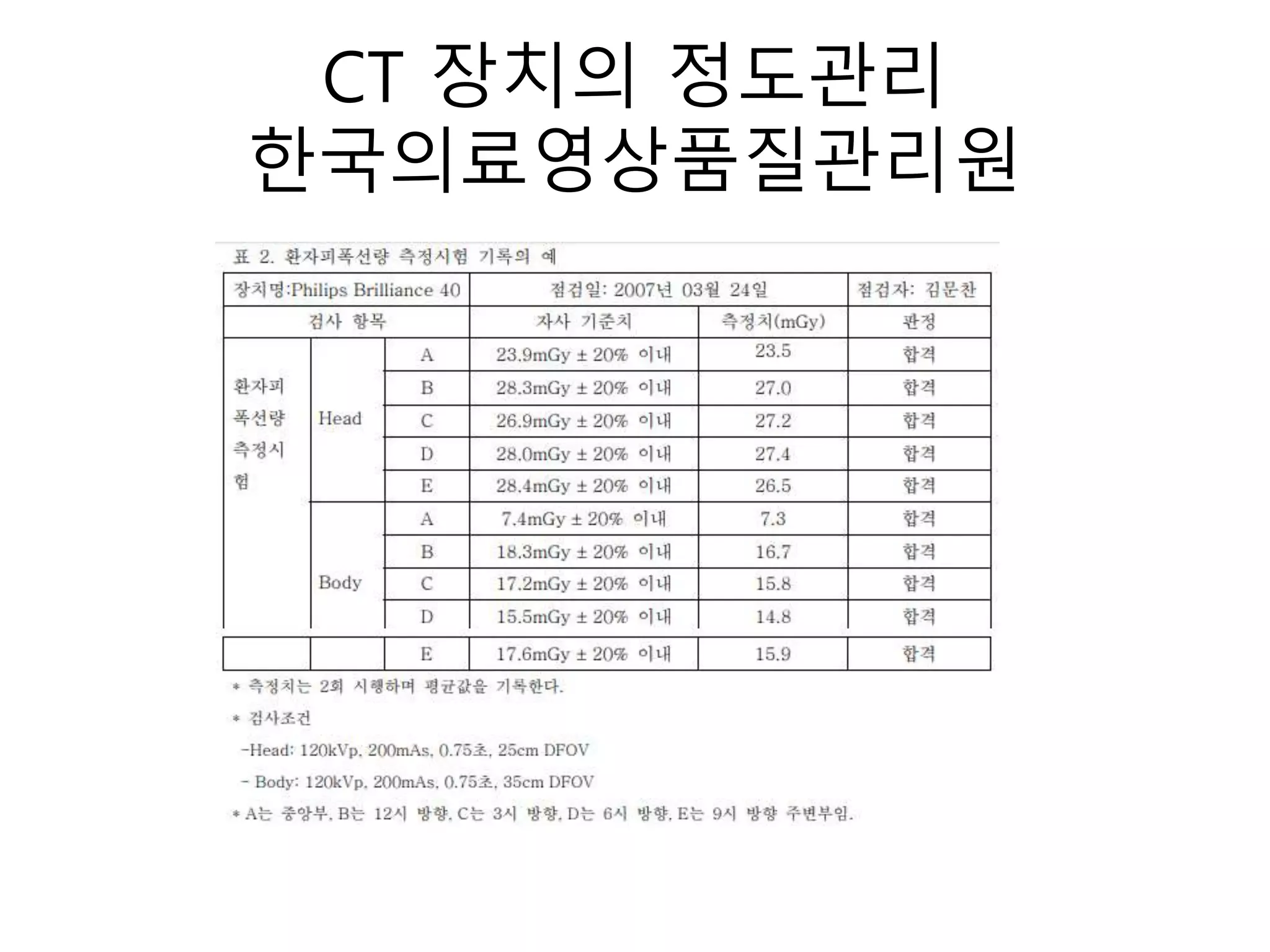
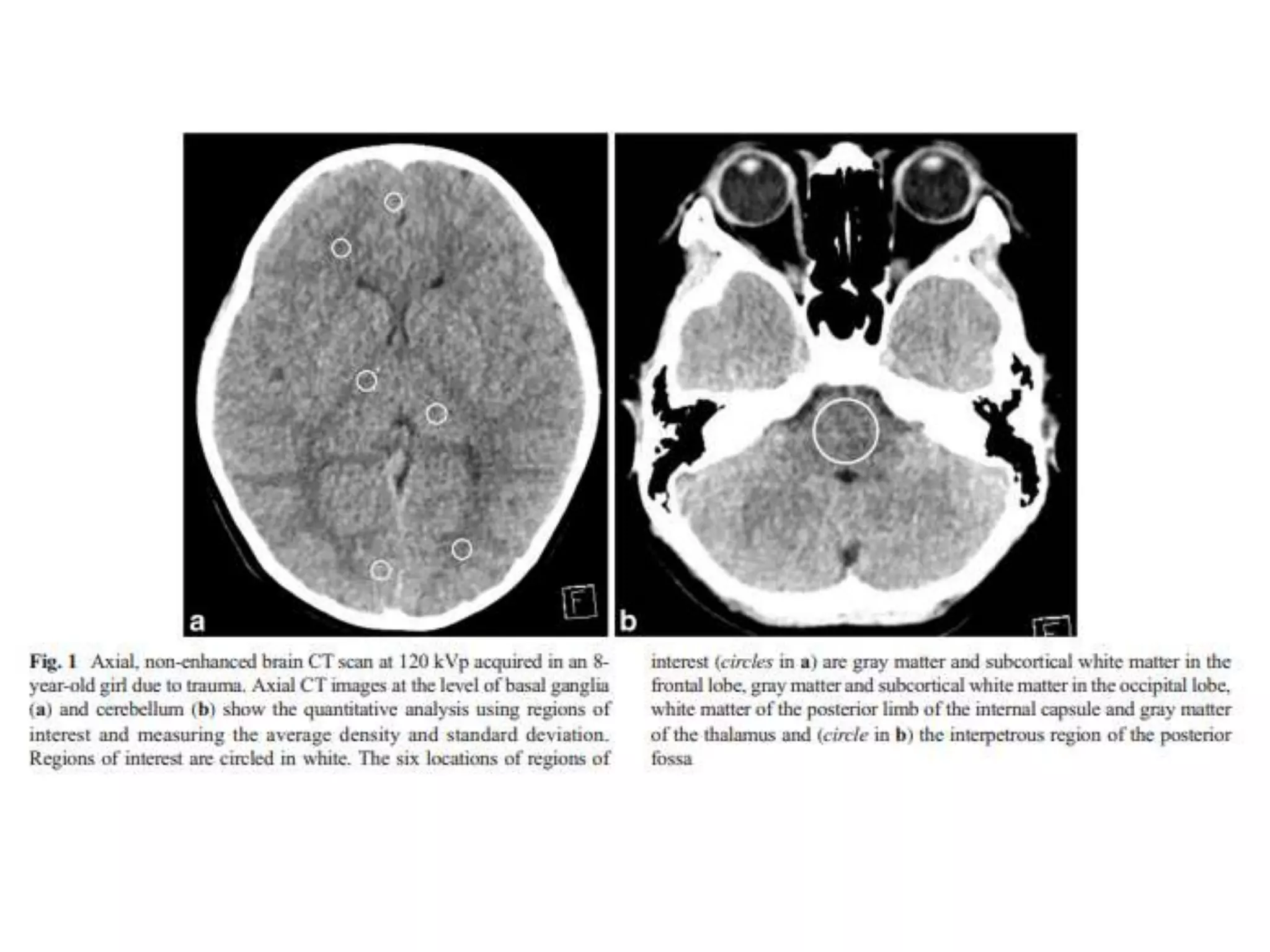
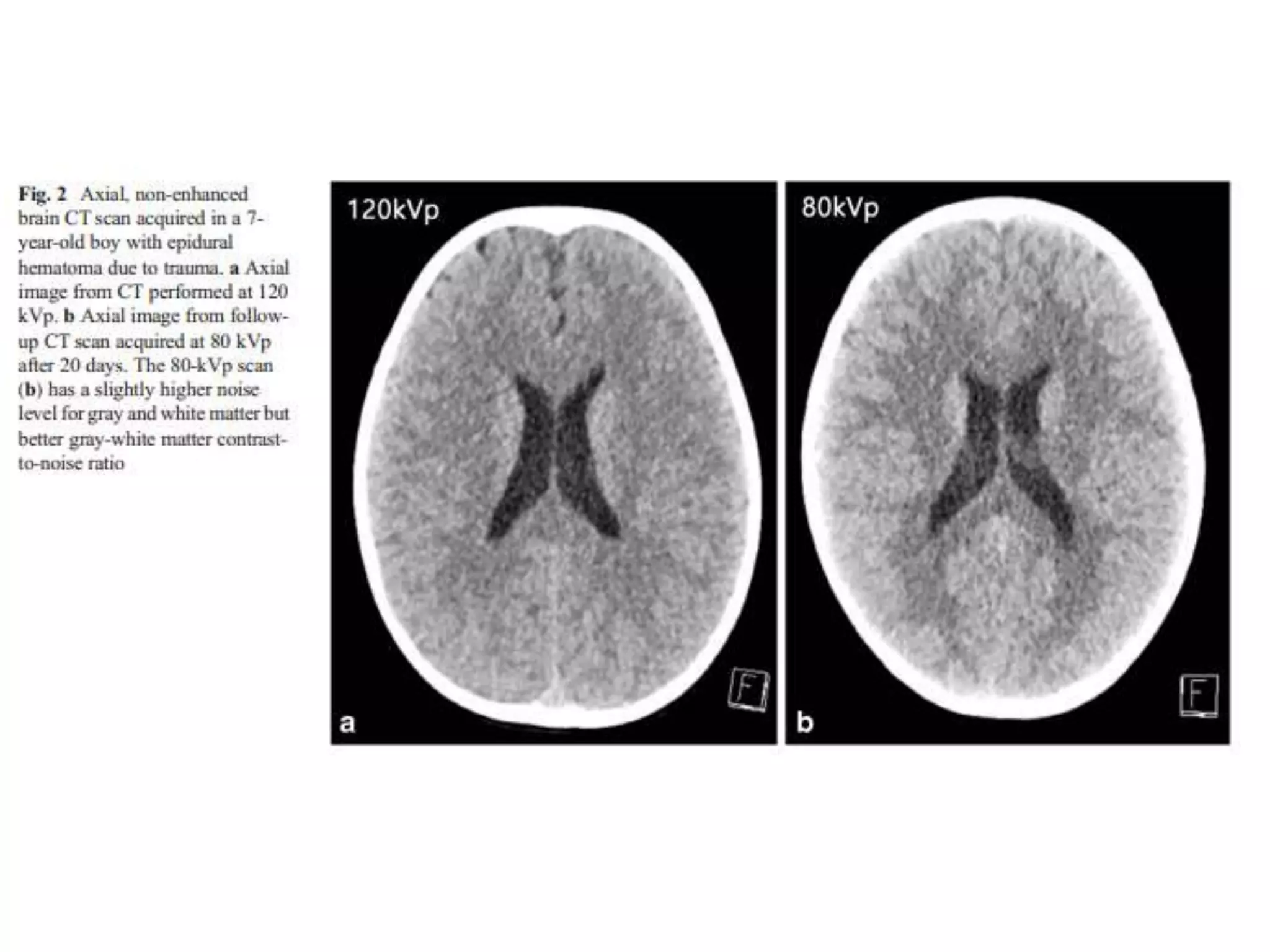
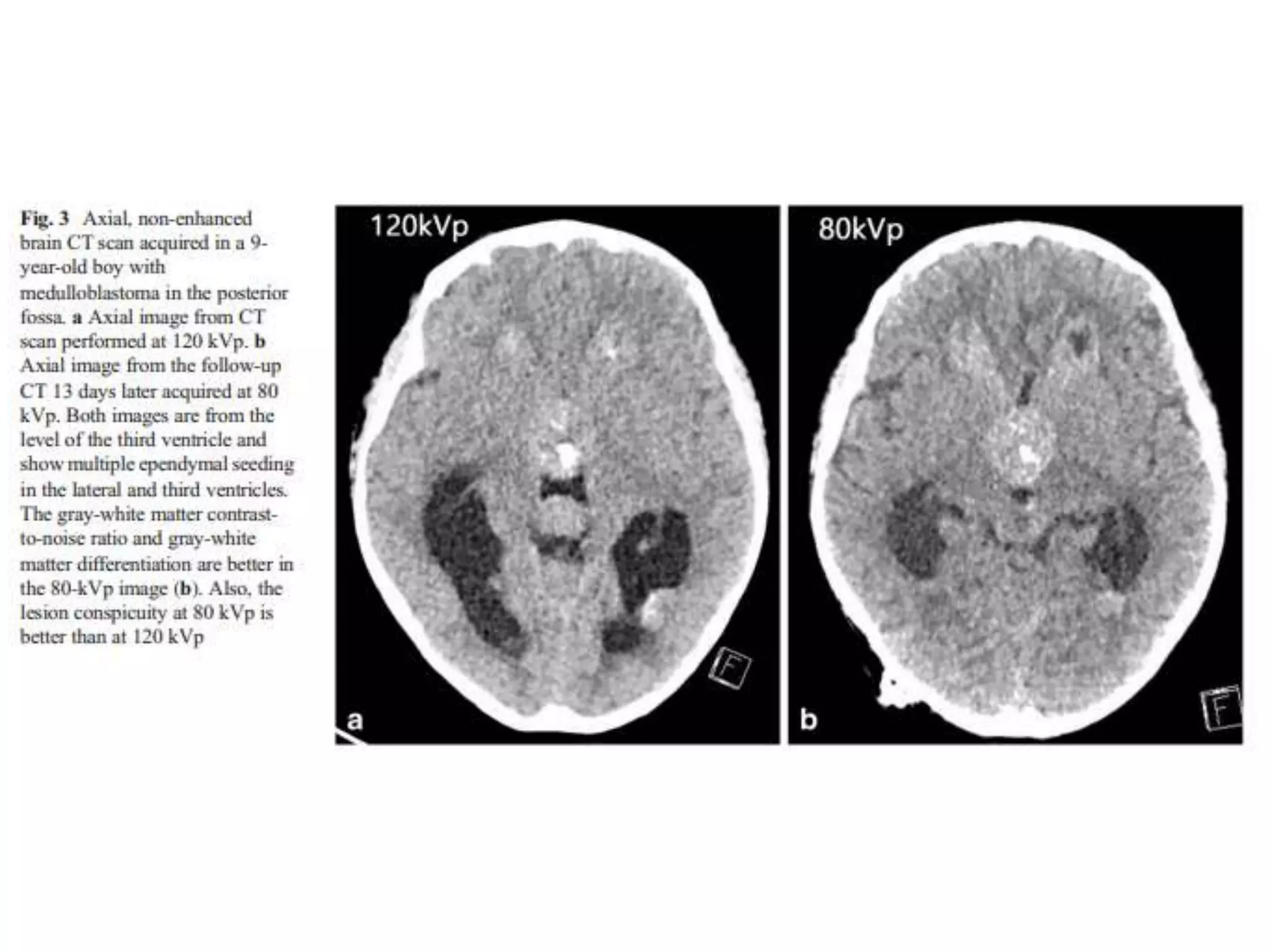
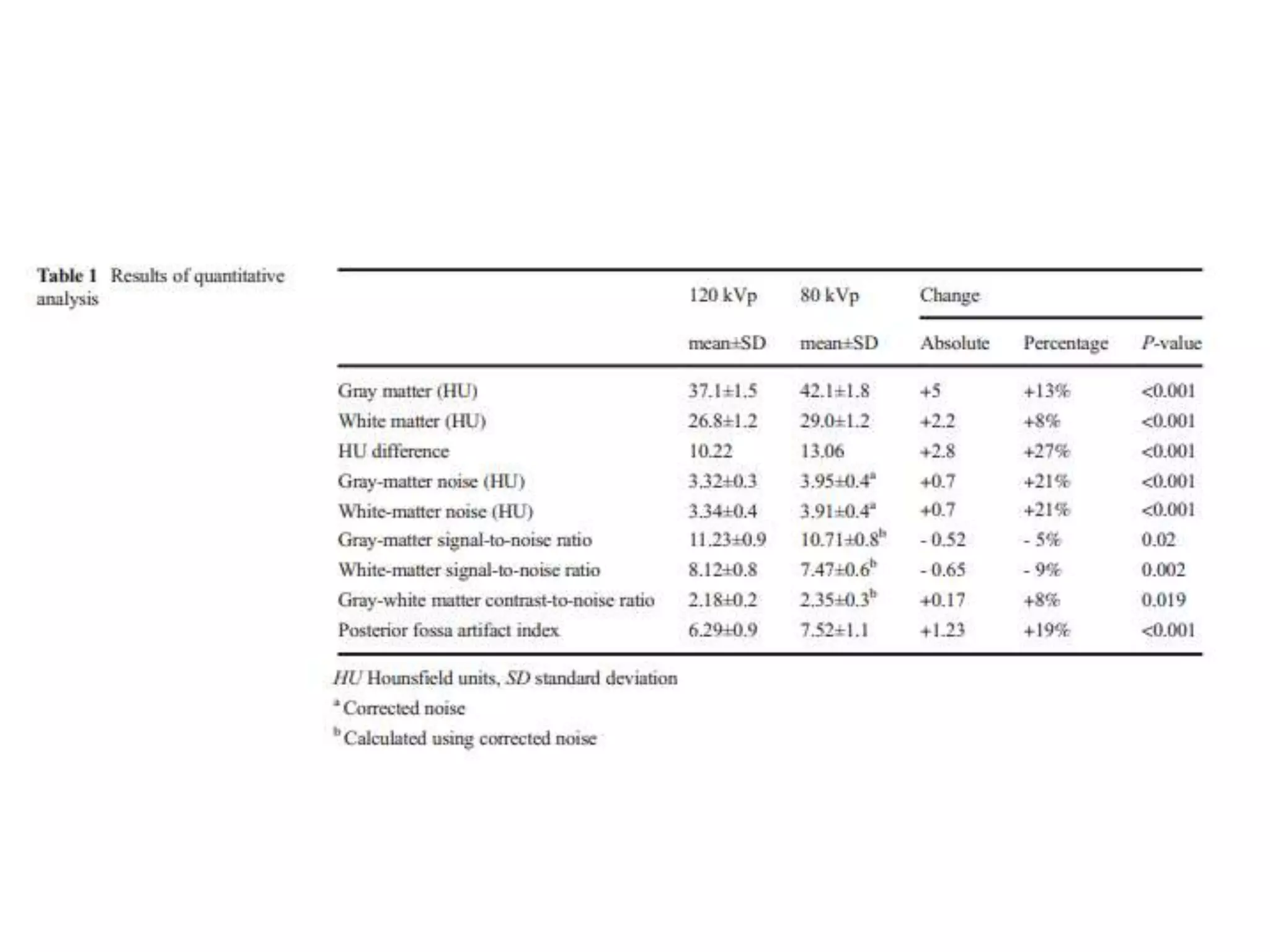
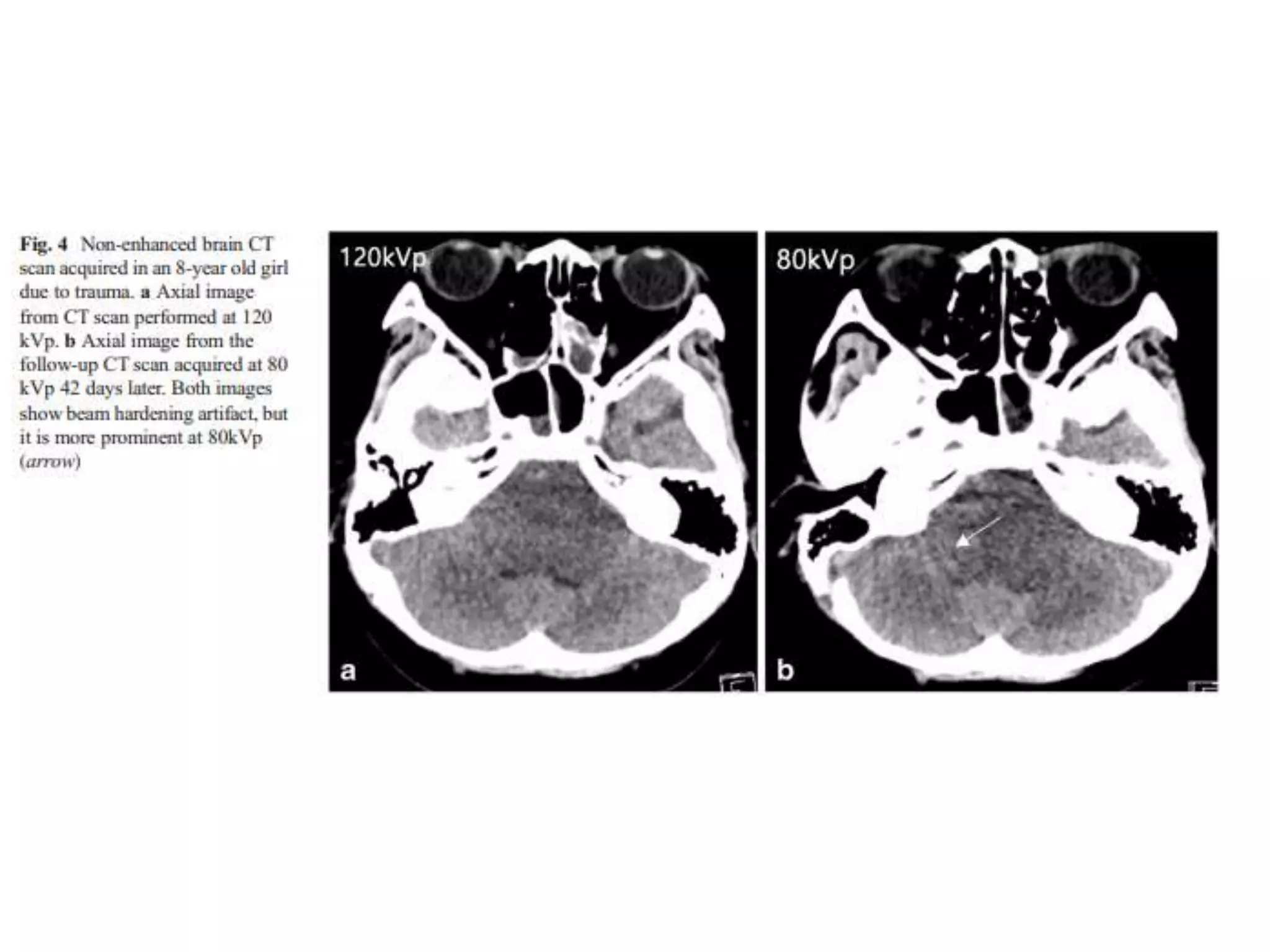
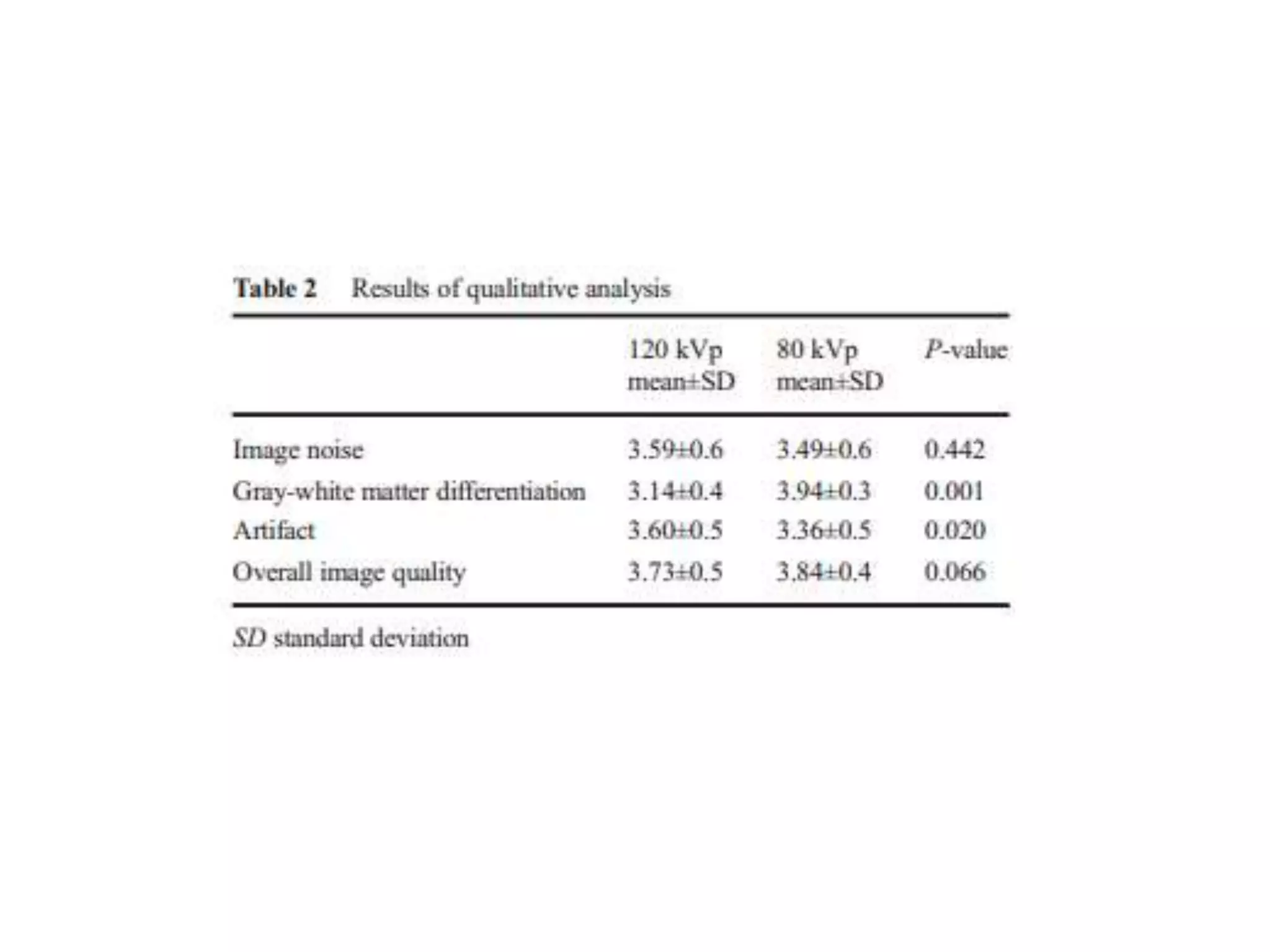
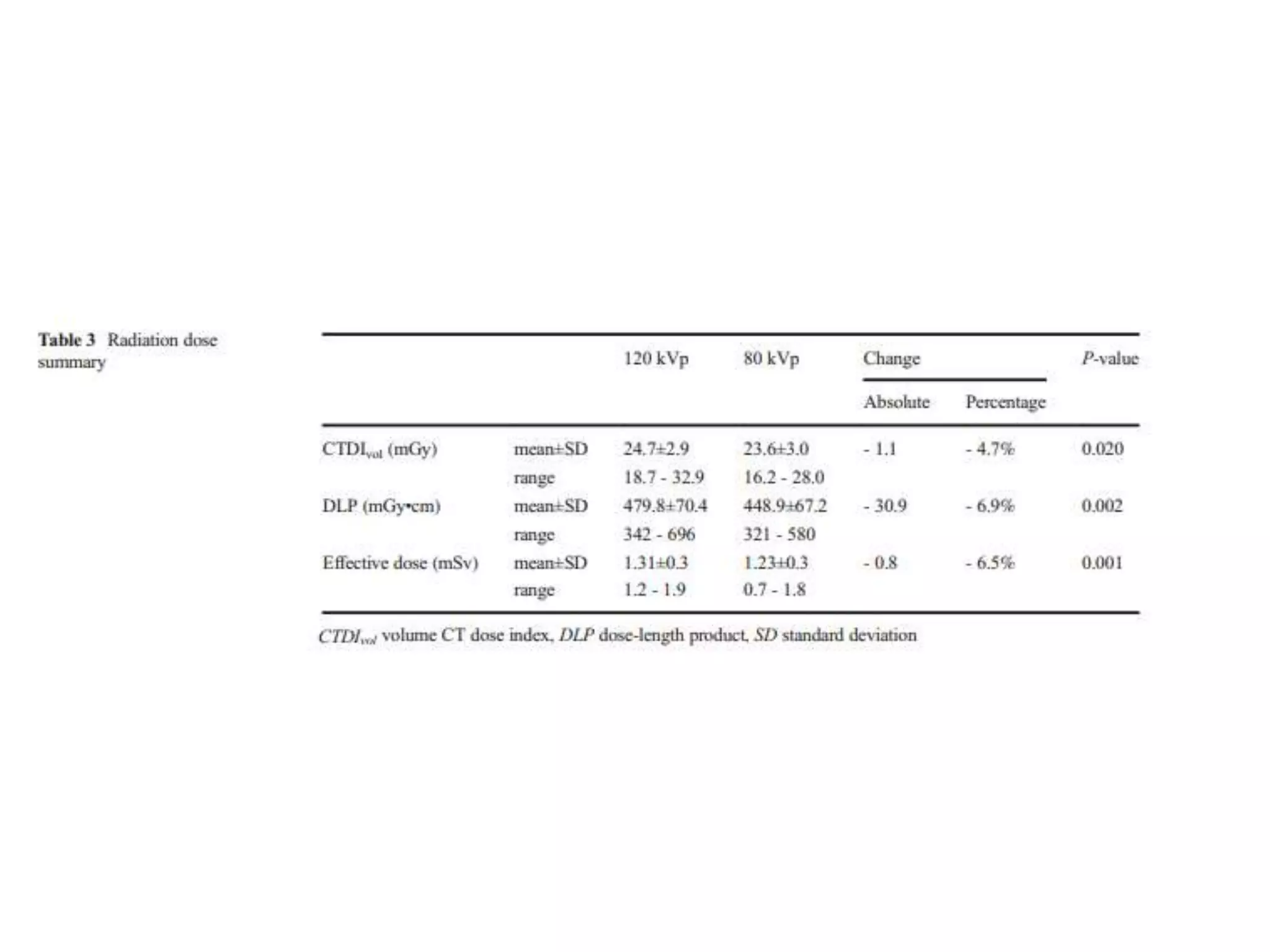
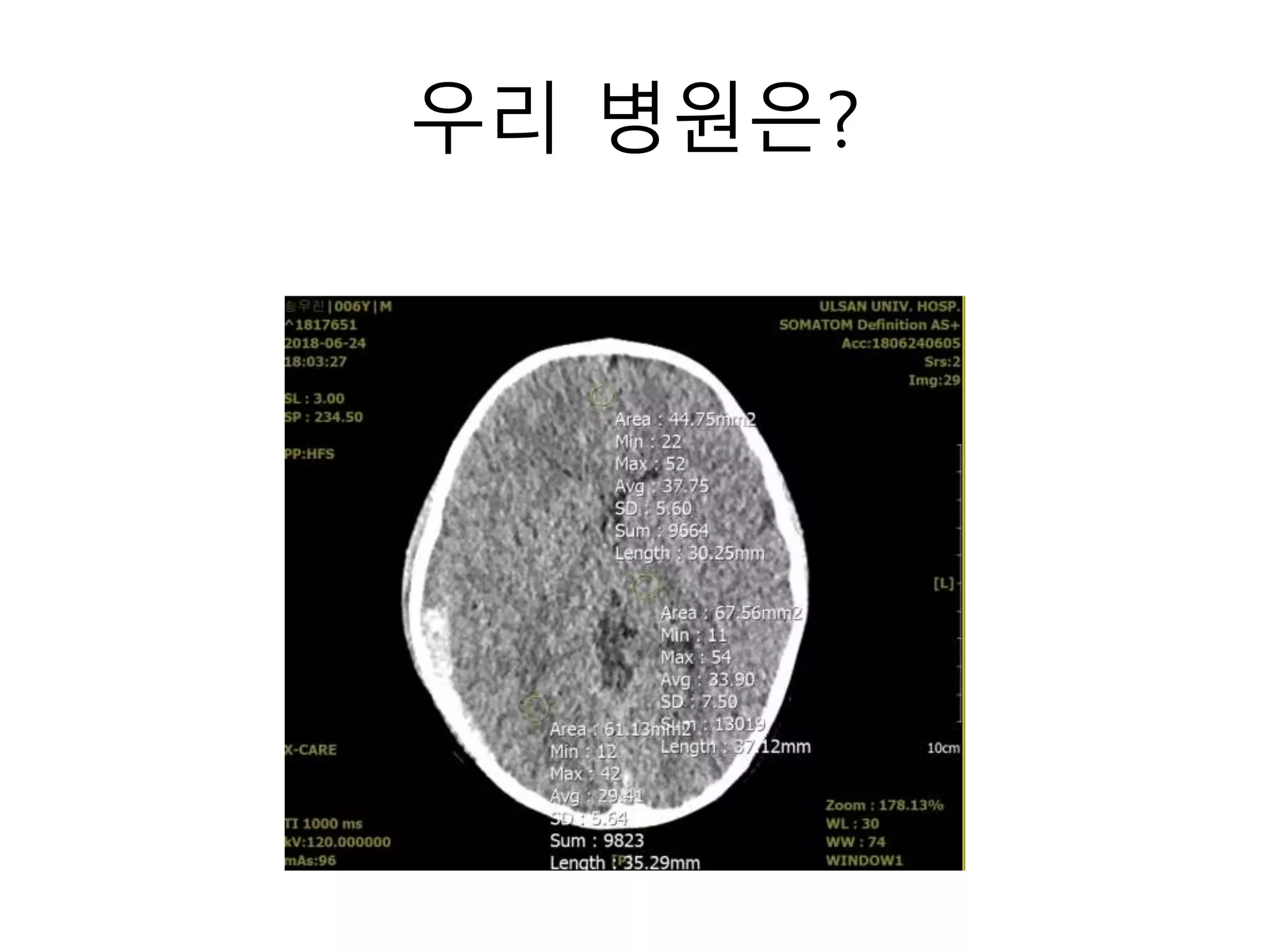
The document discusses the risks of brain tumor induction from head CT scans in children and adolescents. It notes that children are more susceptible than adults to radiation-induced cancer. Several large epidemiological studies have found an increased incidence of brain tumors and other neoplasms in pediatric patients who received head CTs, with one excess tumor estimated for every 3,000-10,000 CT exams in children under 10. The risk is very small but exists, so careful consideration of optimal scan frequency is warranted when head CTs are not definitively medically necessary. Lower dose 80 kV brain CT protocols have been shown to provide similar image quality to standard 120 kV scans with a 6.5% reduction in radiation dose.






![Study selection
• The Preferred Reporting Items for
Systematic Reviews and Meta-Analysis
(PRISMA) guideline[21.22]](https://image.slidesharecdn.com/pediatricheadct-190124064959/75/Pediatric-head-CT-7-2048.jpg)

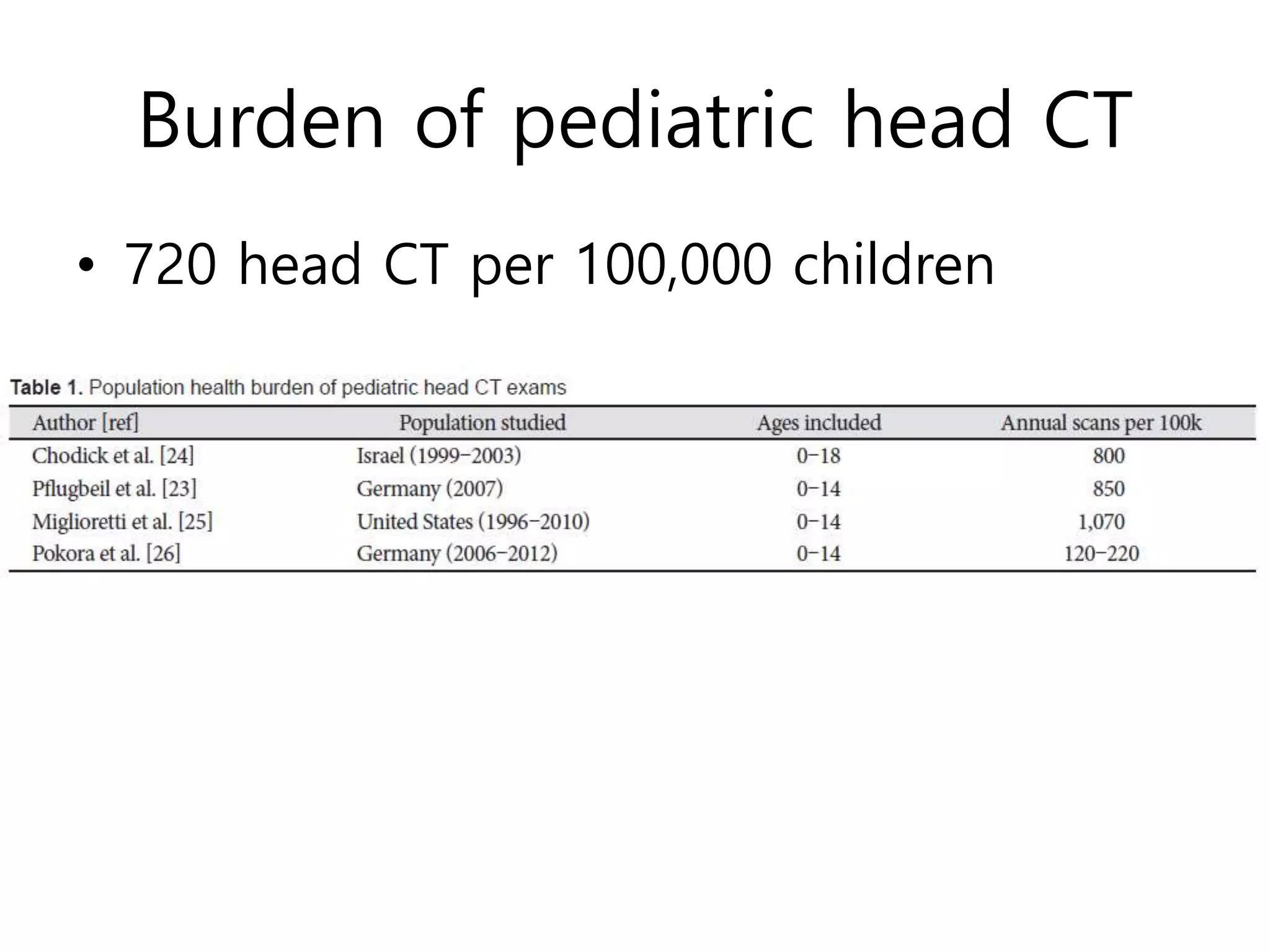
![Predicted Tumor risk
• Brain dose; 55 mGy
• Effective dose; 1.6 mSv
• LAR; 0.056% [23,25,27,29,30]](https://image.slidesharecdn.com/pediatricheadct-190124064959/75/Pediatric-head-CT-10-2048.jpg)
![Measured tumor risk
• 5 studies[14,31-34], re-analysis[35]
• 995,091 patients, brain dose 41±9 mGy](https://image.slidesharecdn.com/pediatricheadct-190124064959/75/Pediatric-head-CT-11-2048.jpg)



![Discussion
• Since 2012, Five large epidemiological
studies[14,31-34], increased incidence of
neoplasm (predominantly brain tumors)
in pediatric patients from head CTs
• One excess neoplasm may be expected
per 3,000 – 10,000 CT exams in children
under age 10](https://image.slidesharecdn.com/pediatricheadct-190124064959/75/Pediatric-head-CT-15-2048.jpg)