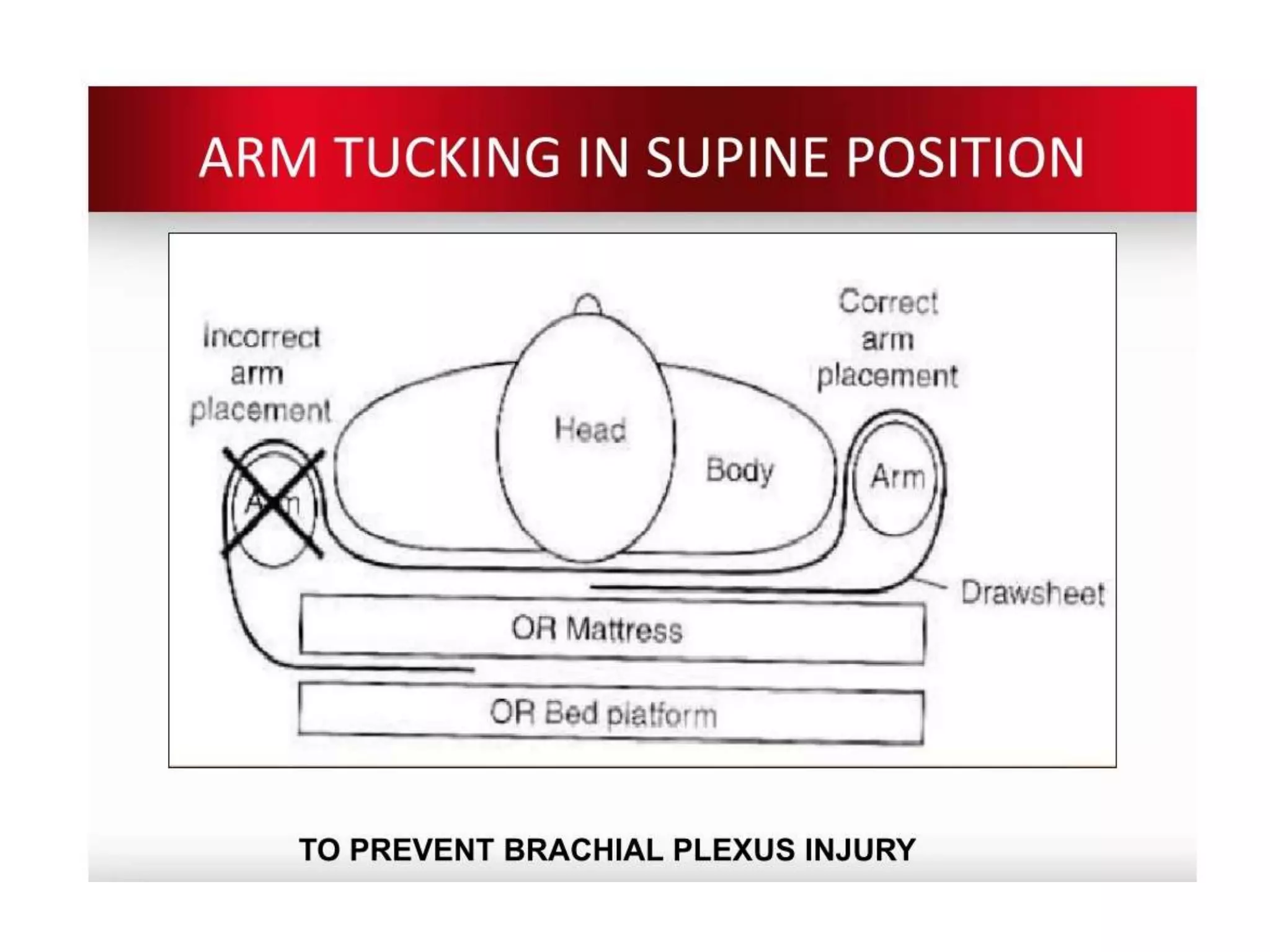
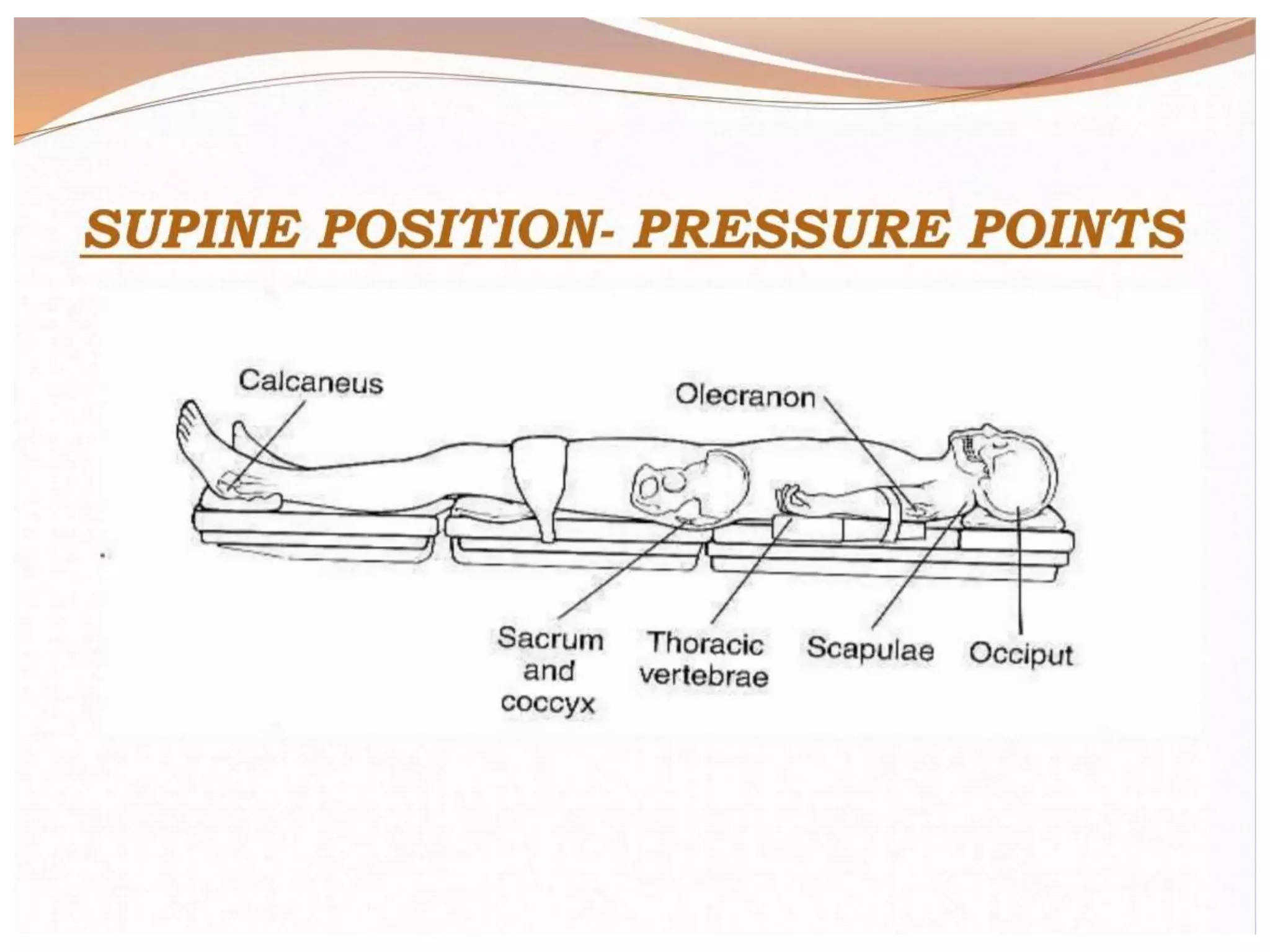
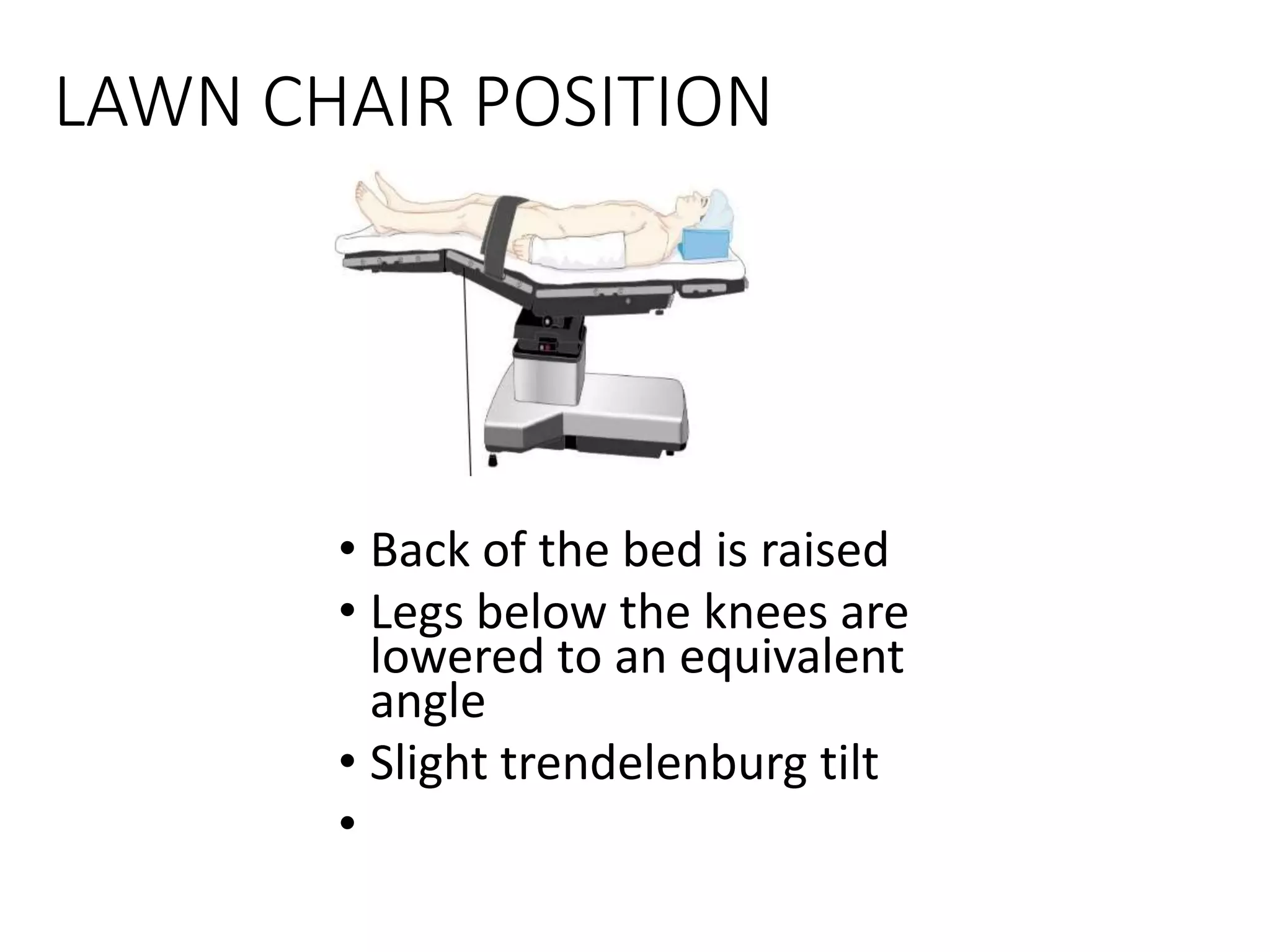
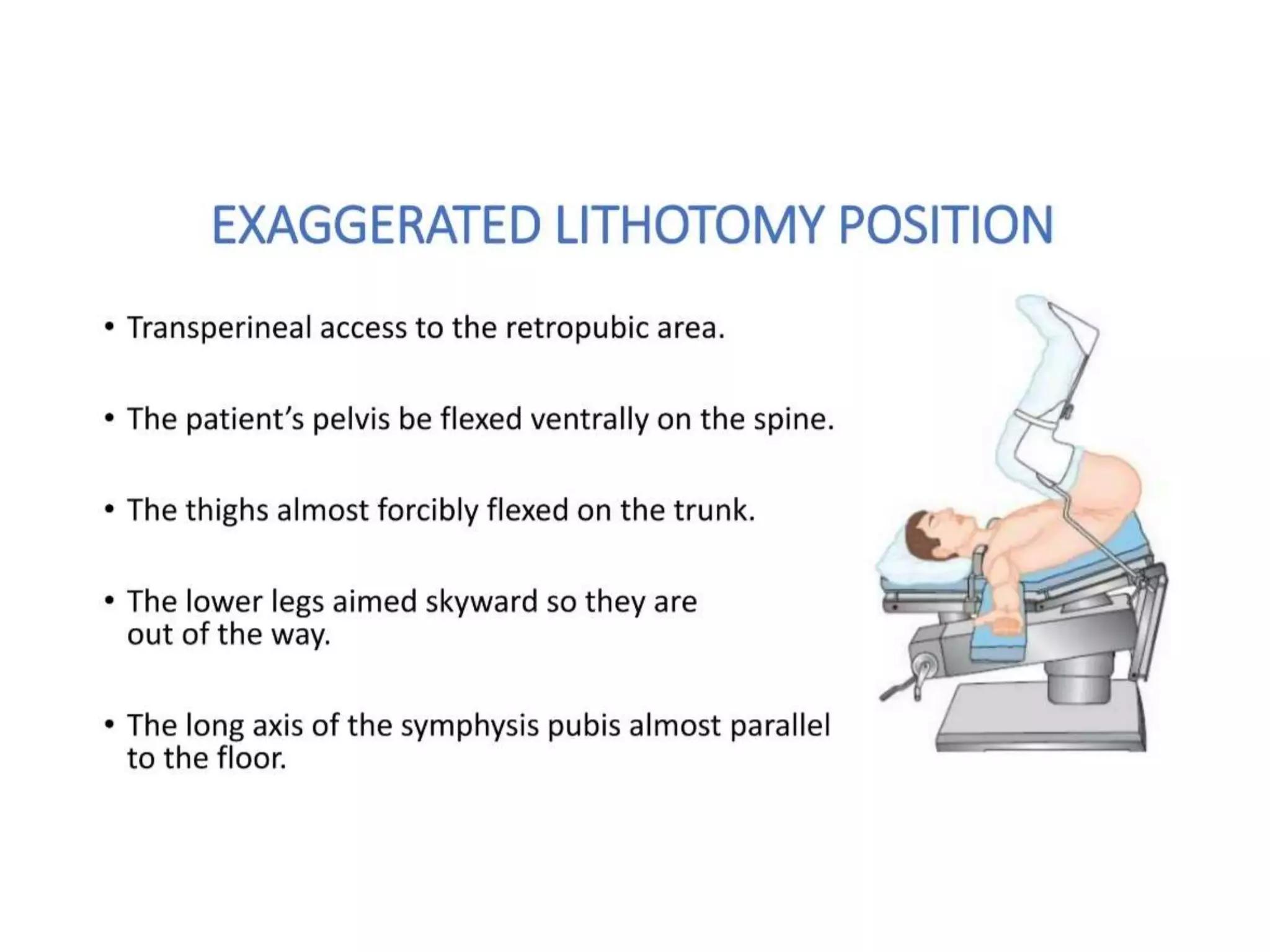
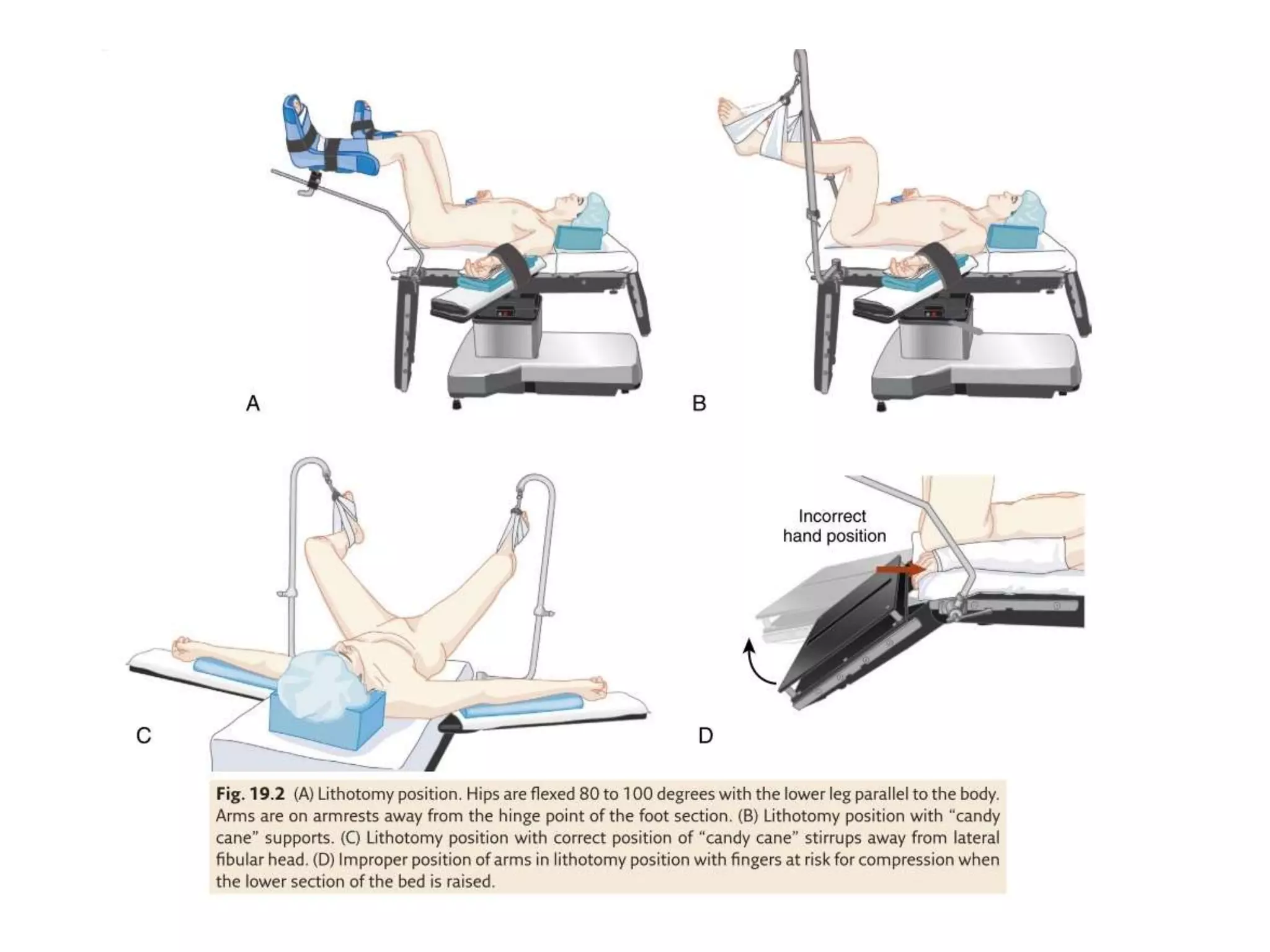
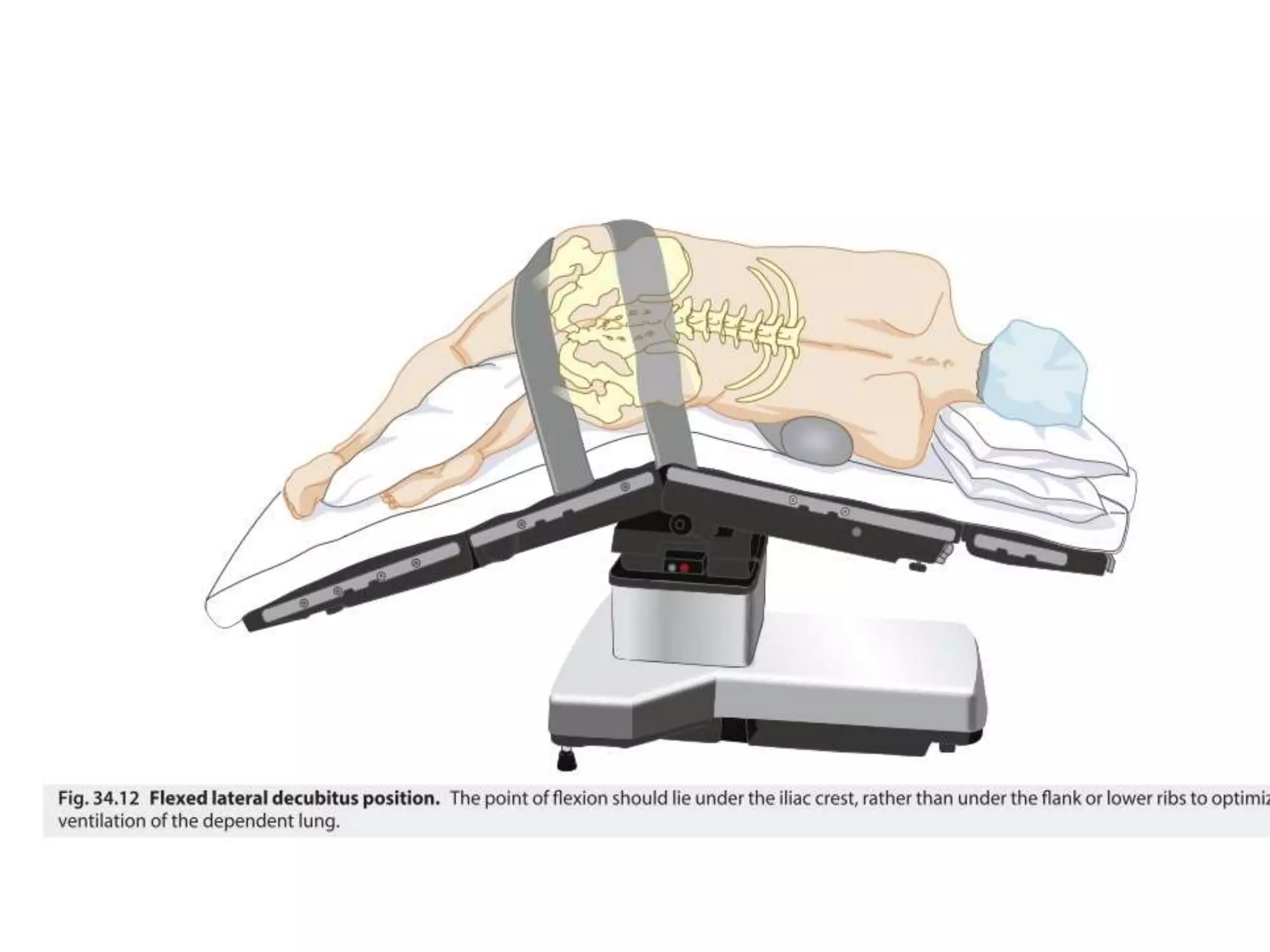
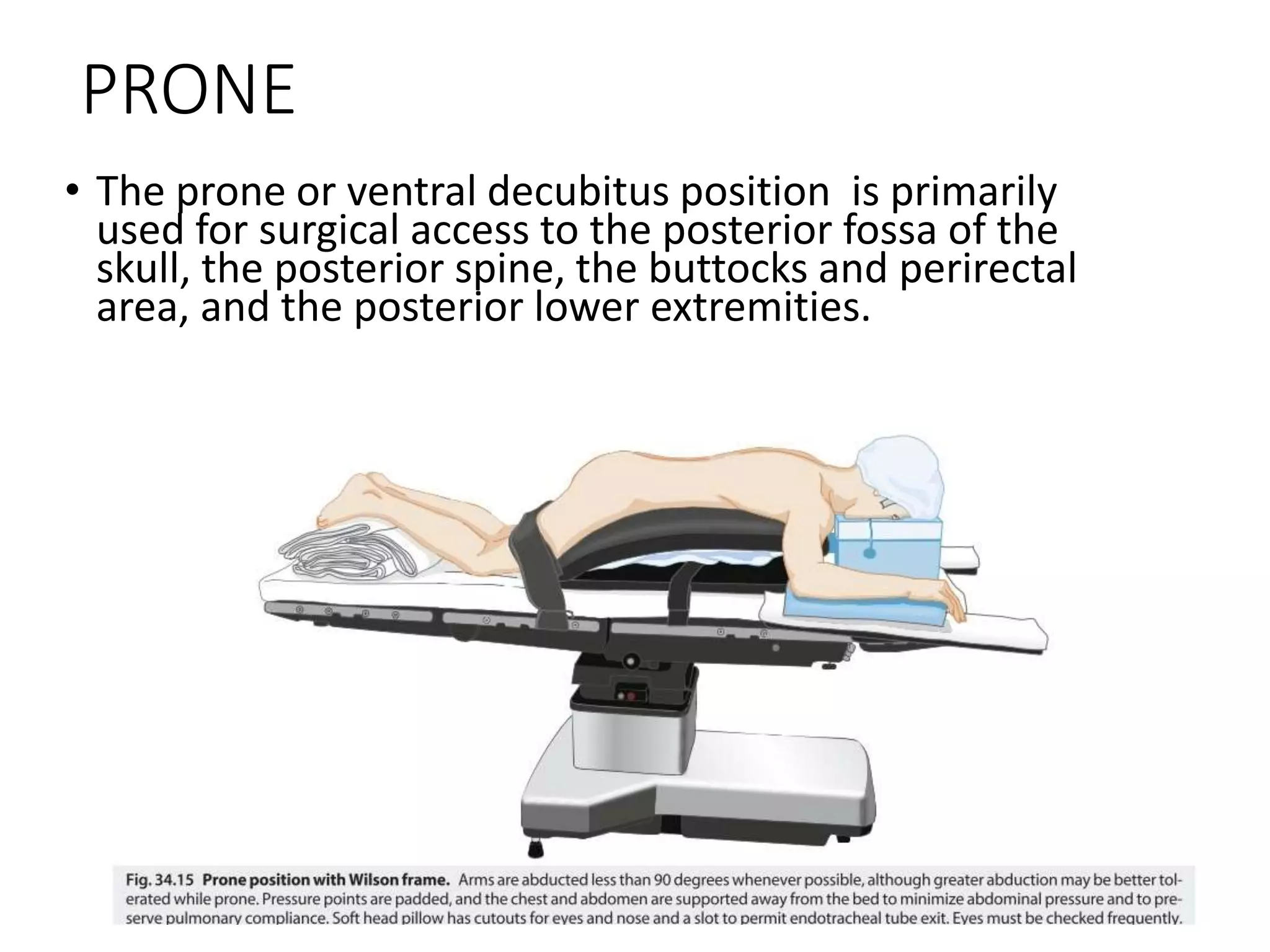
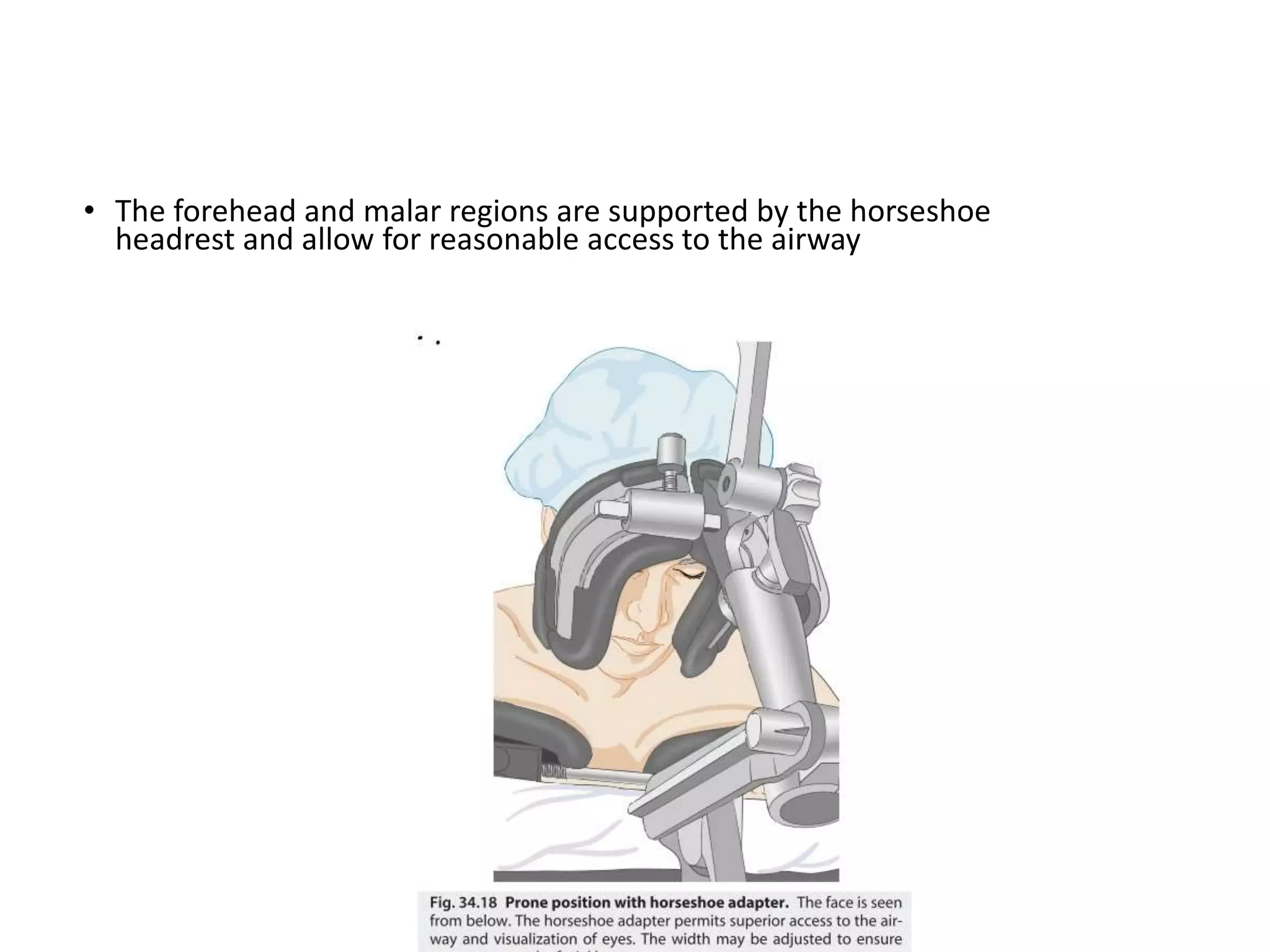
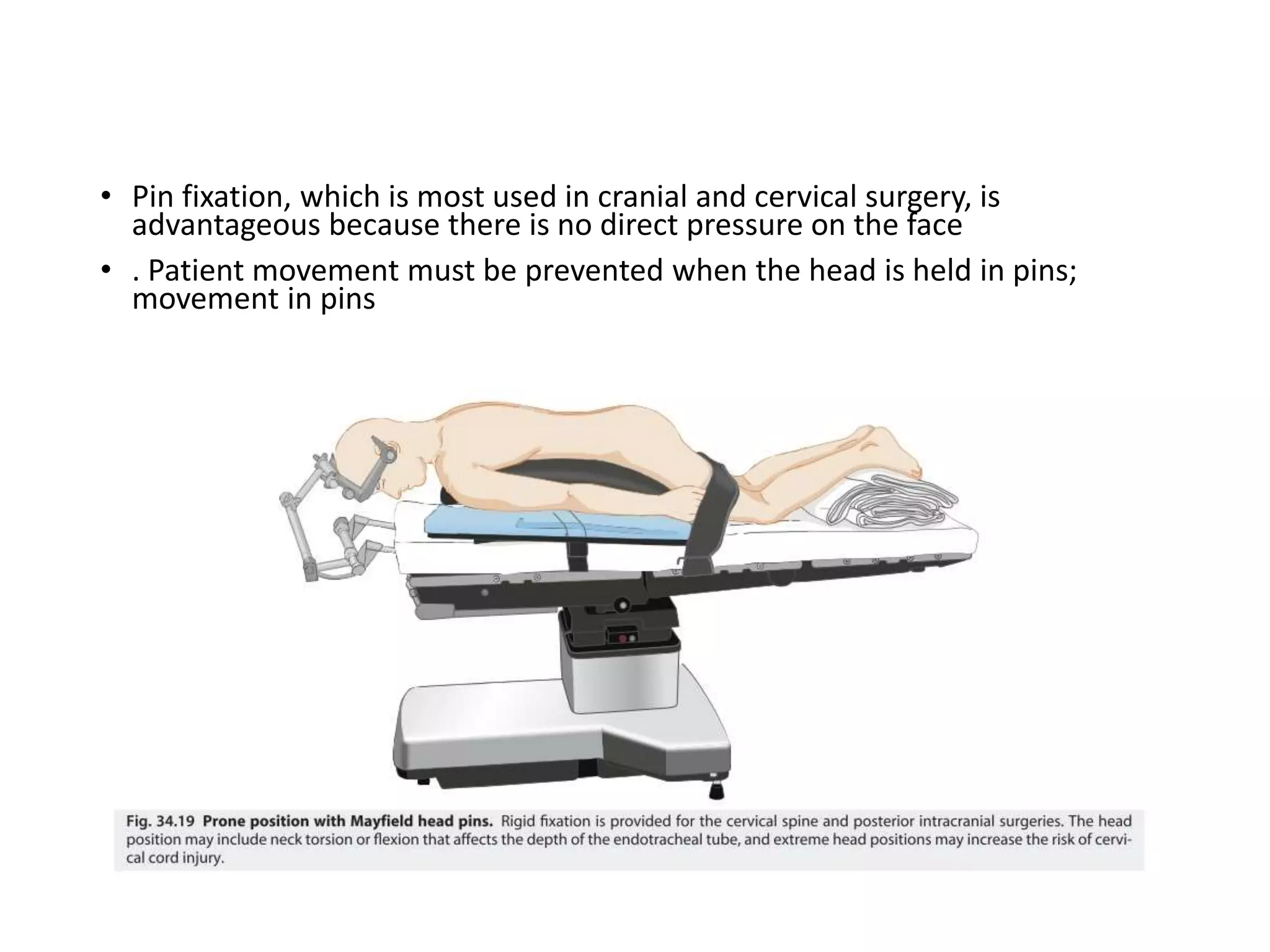
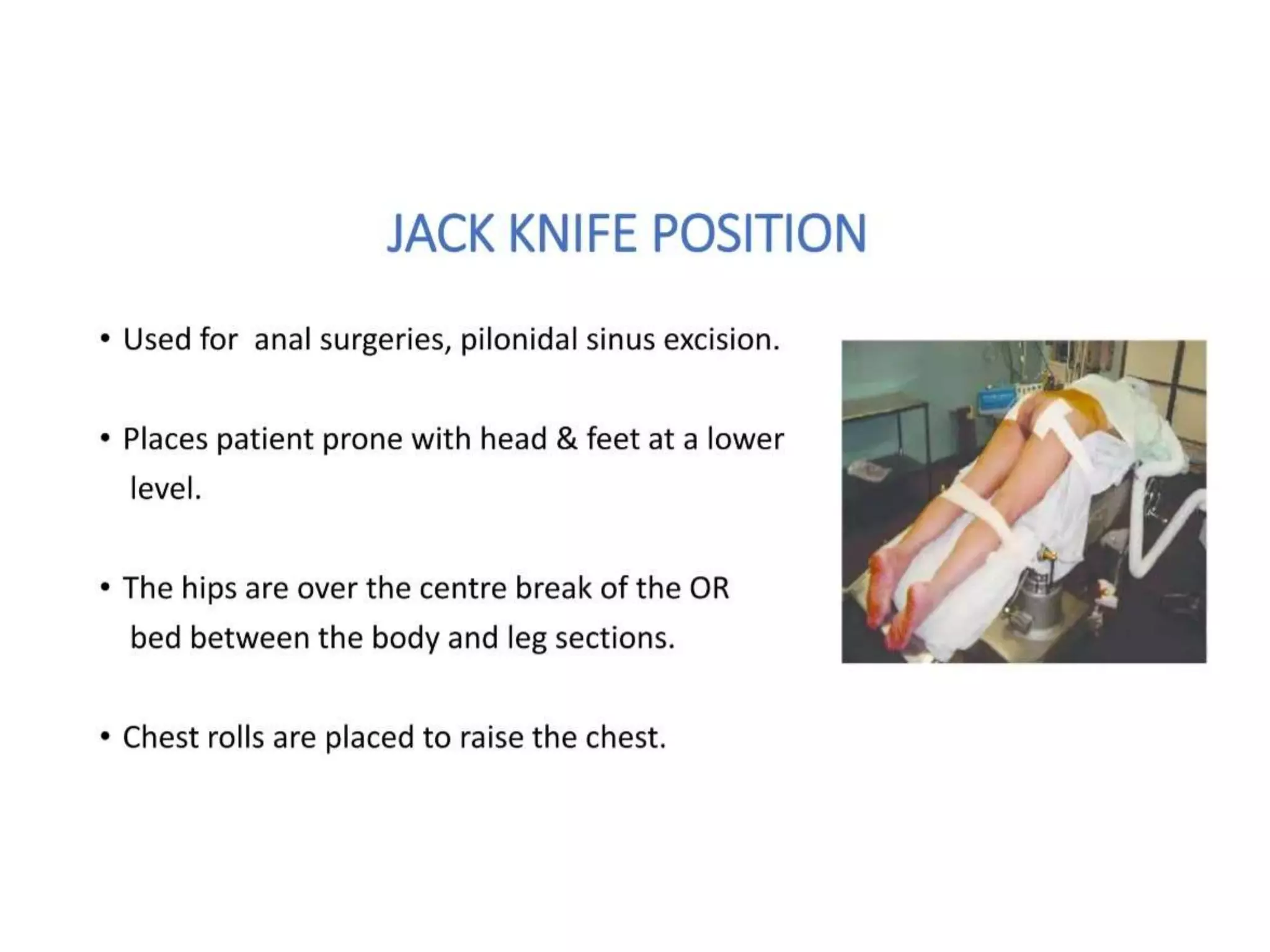
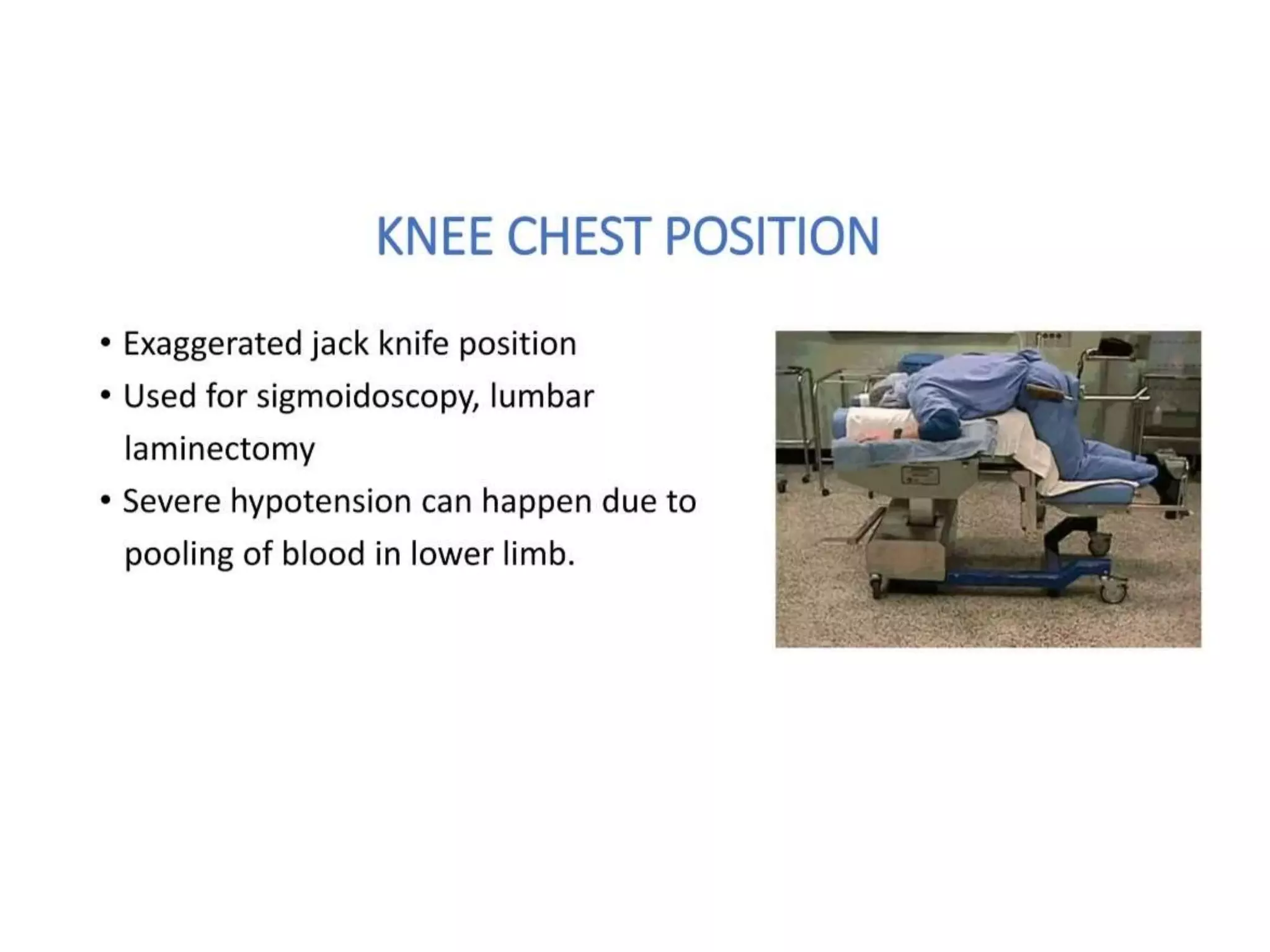
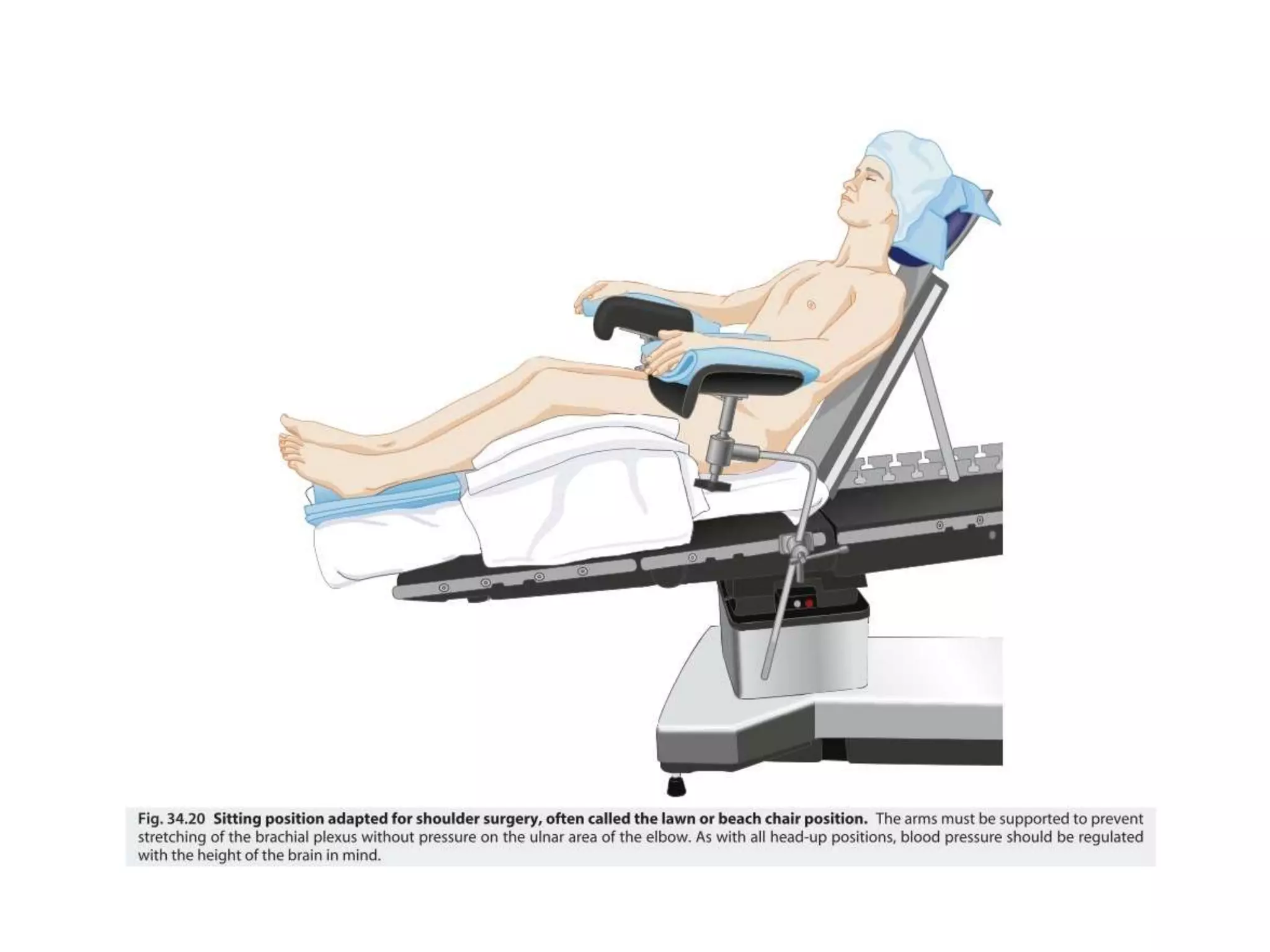
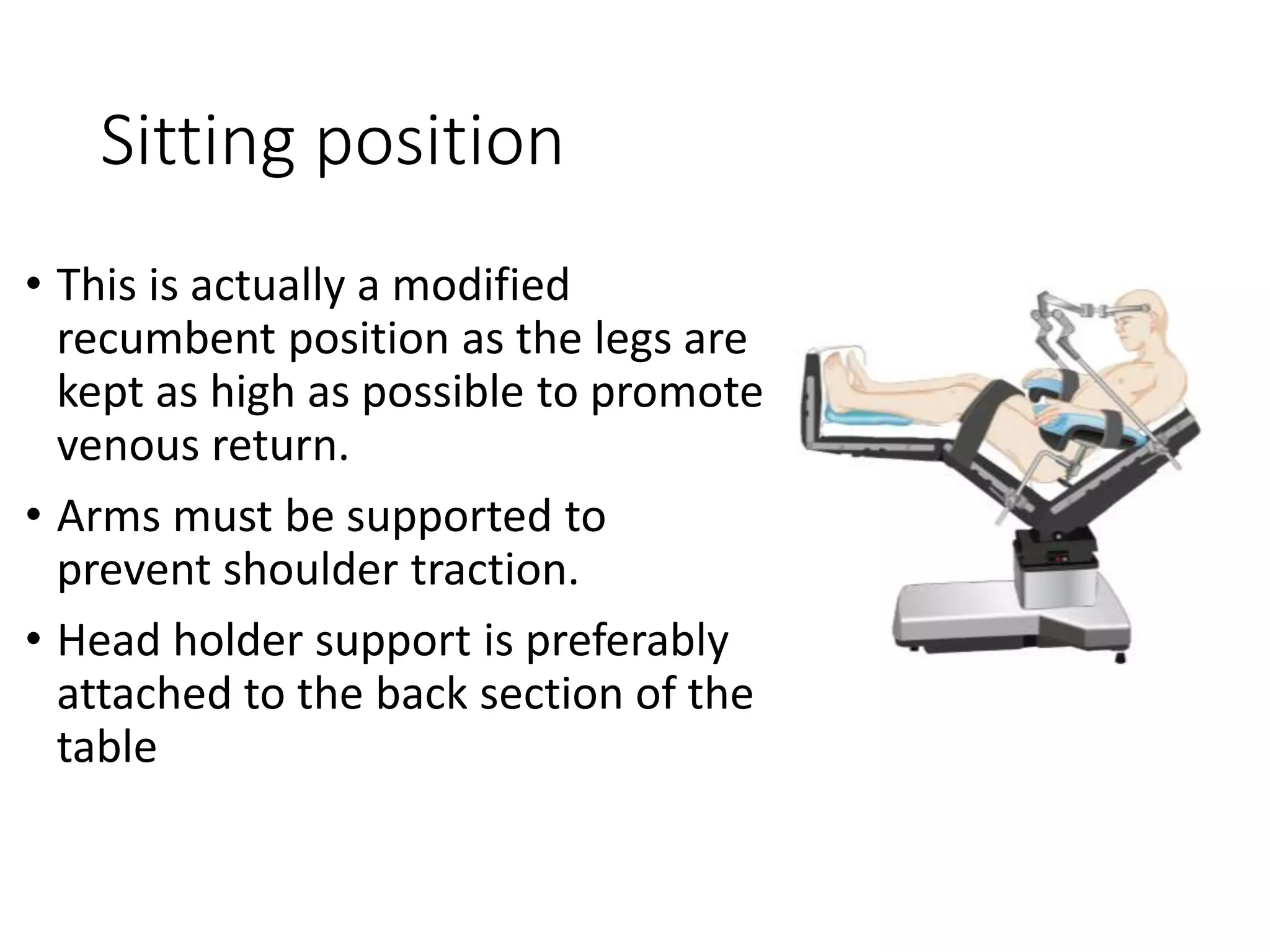
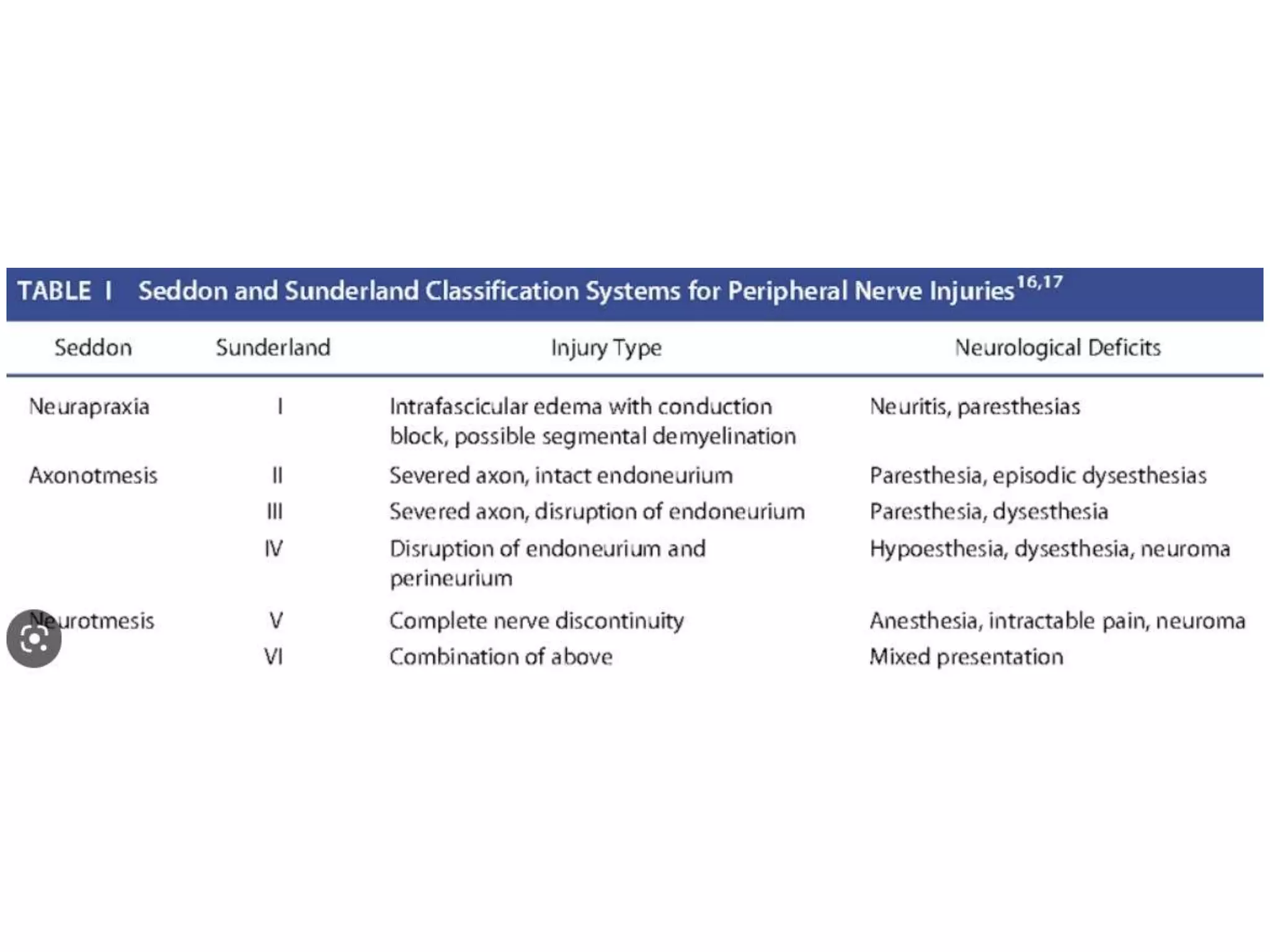
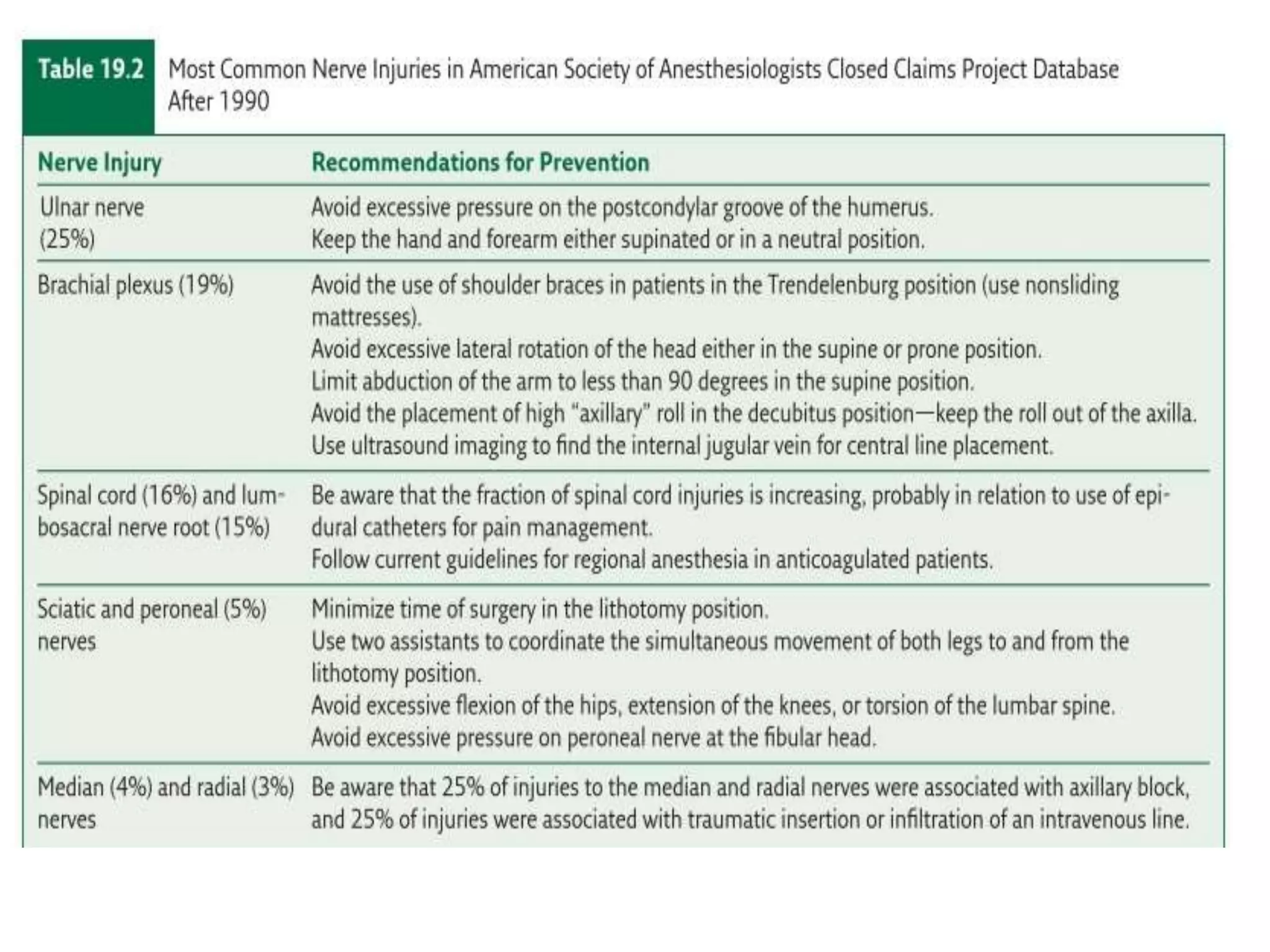
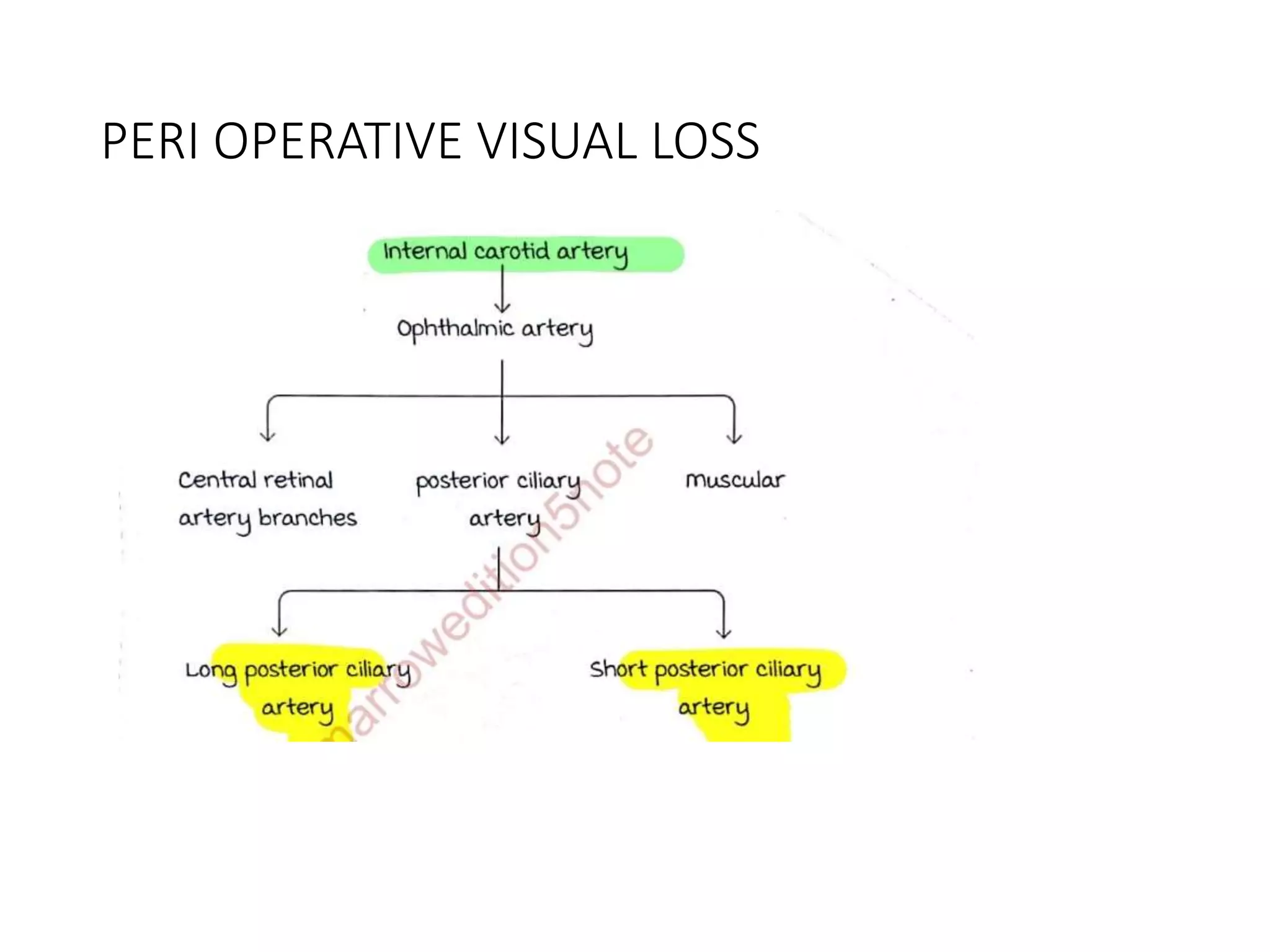
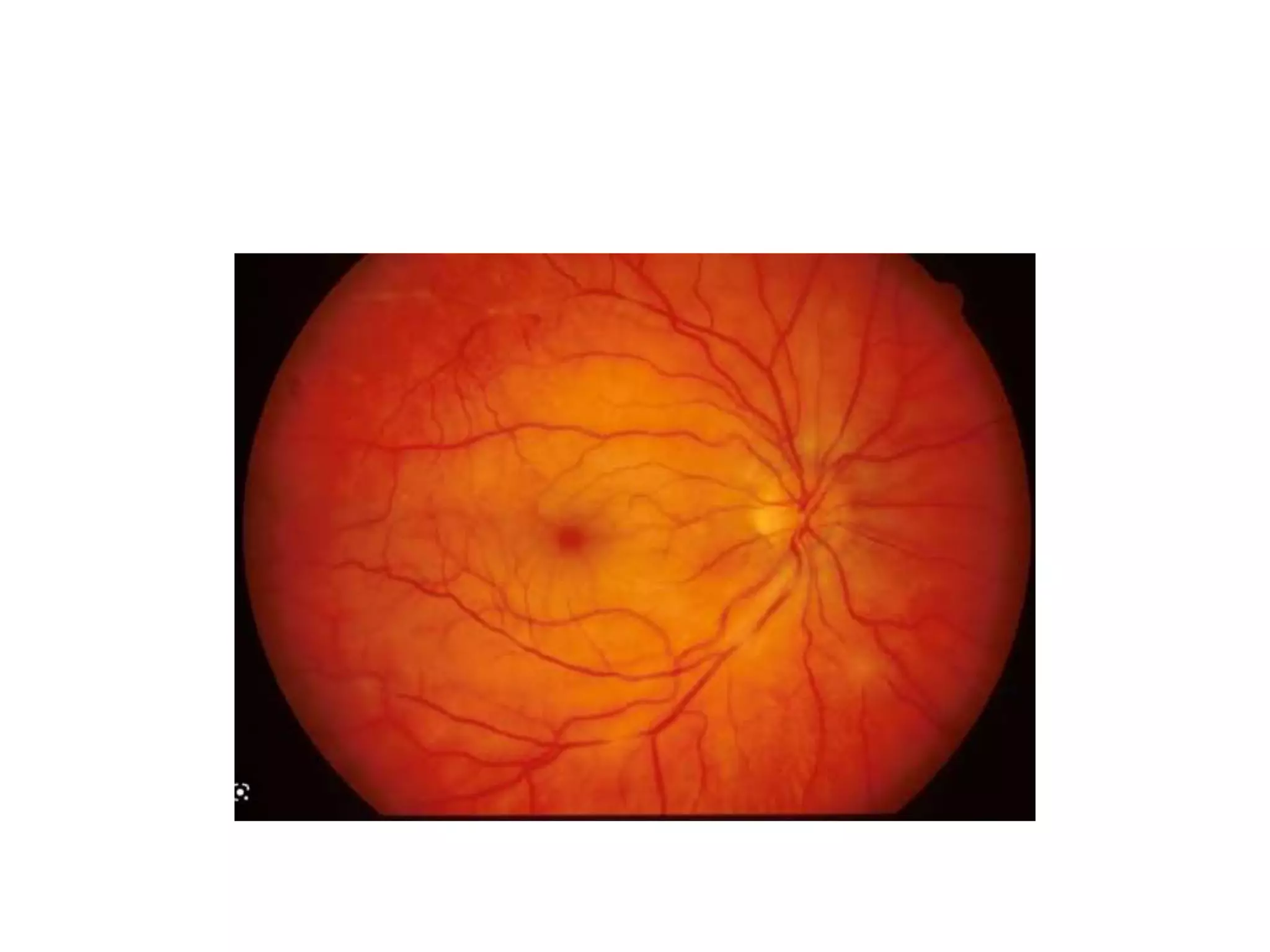
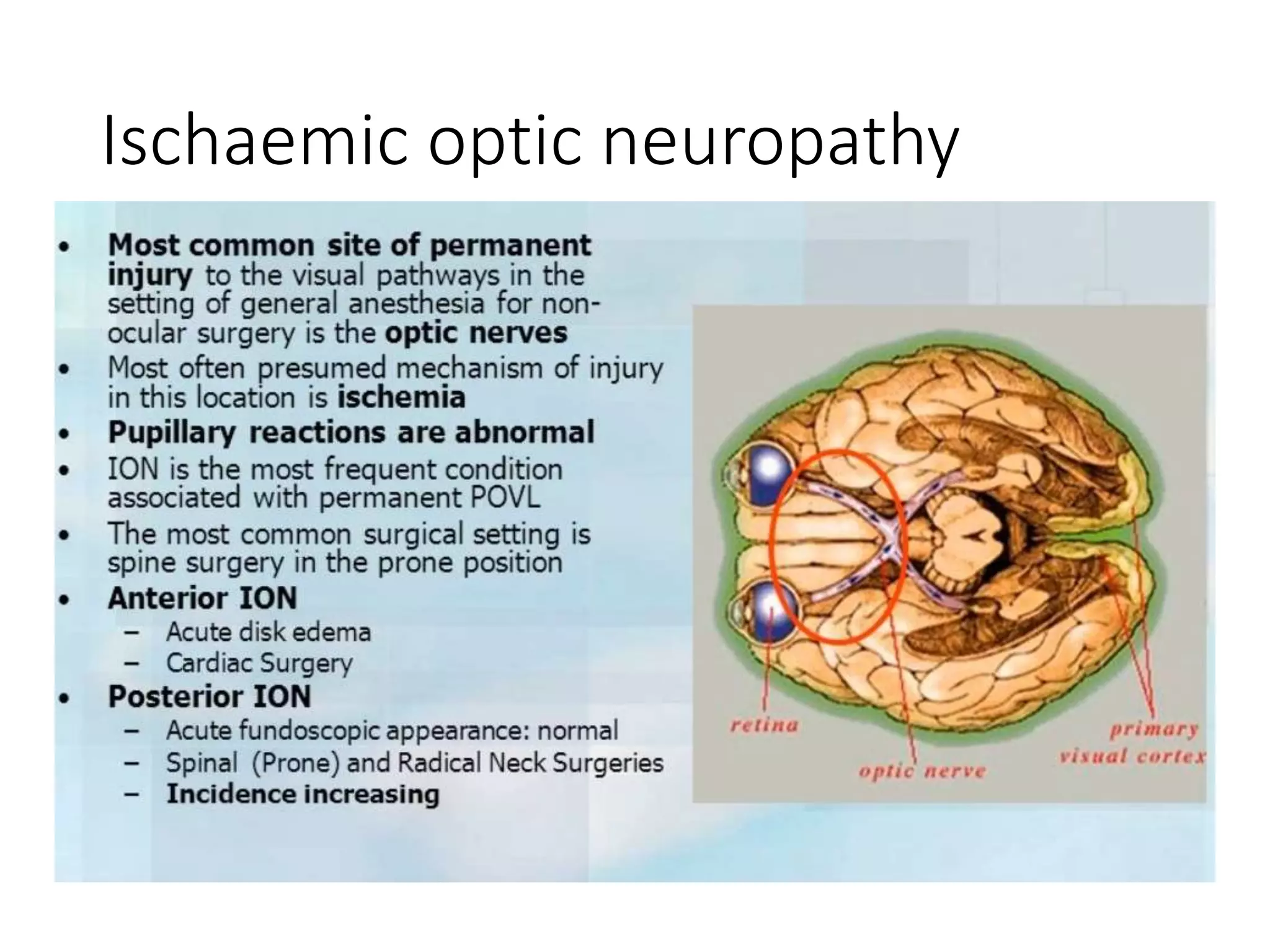
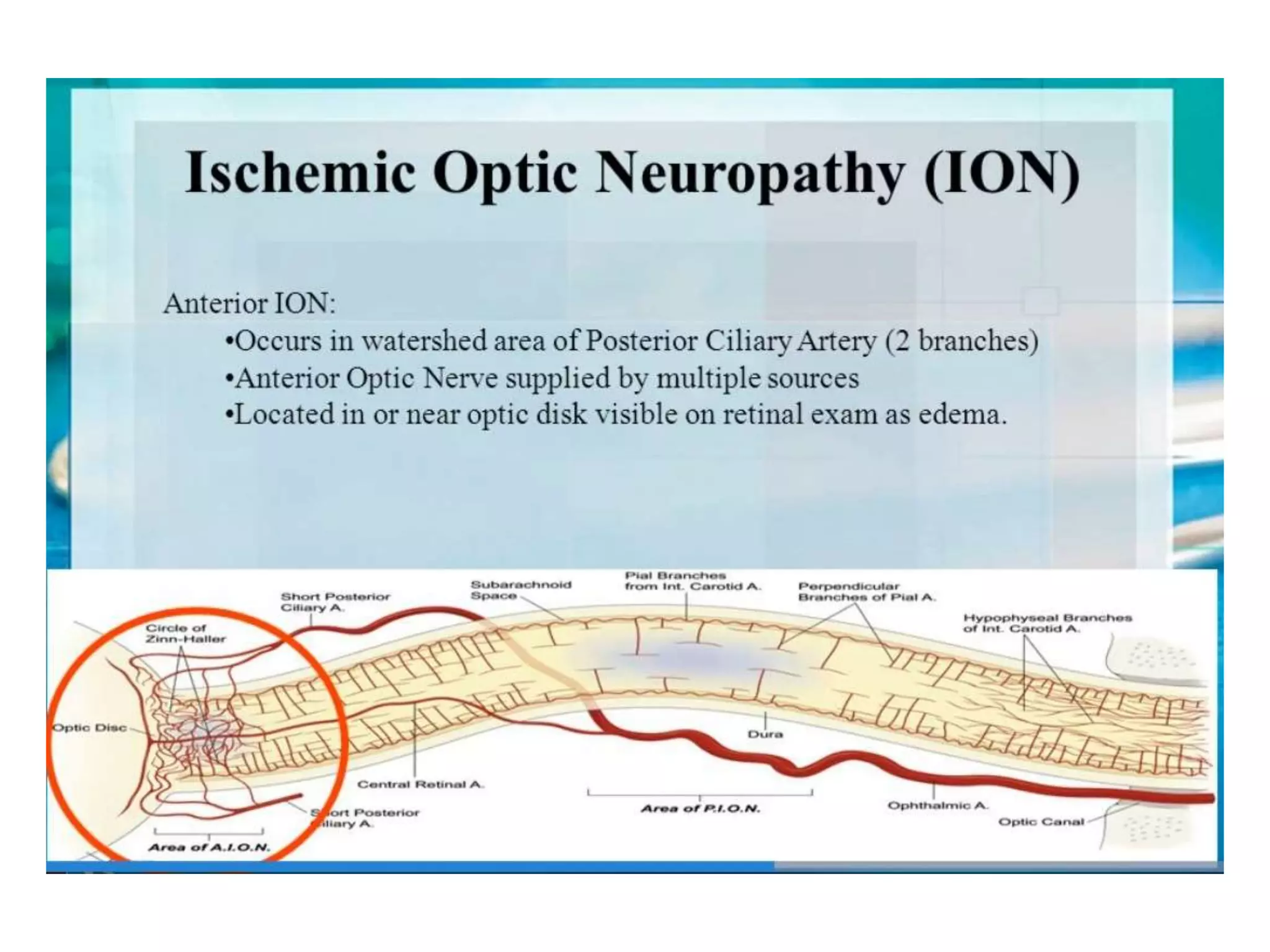
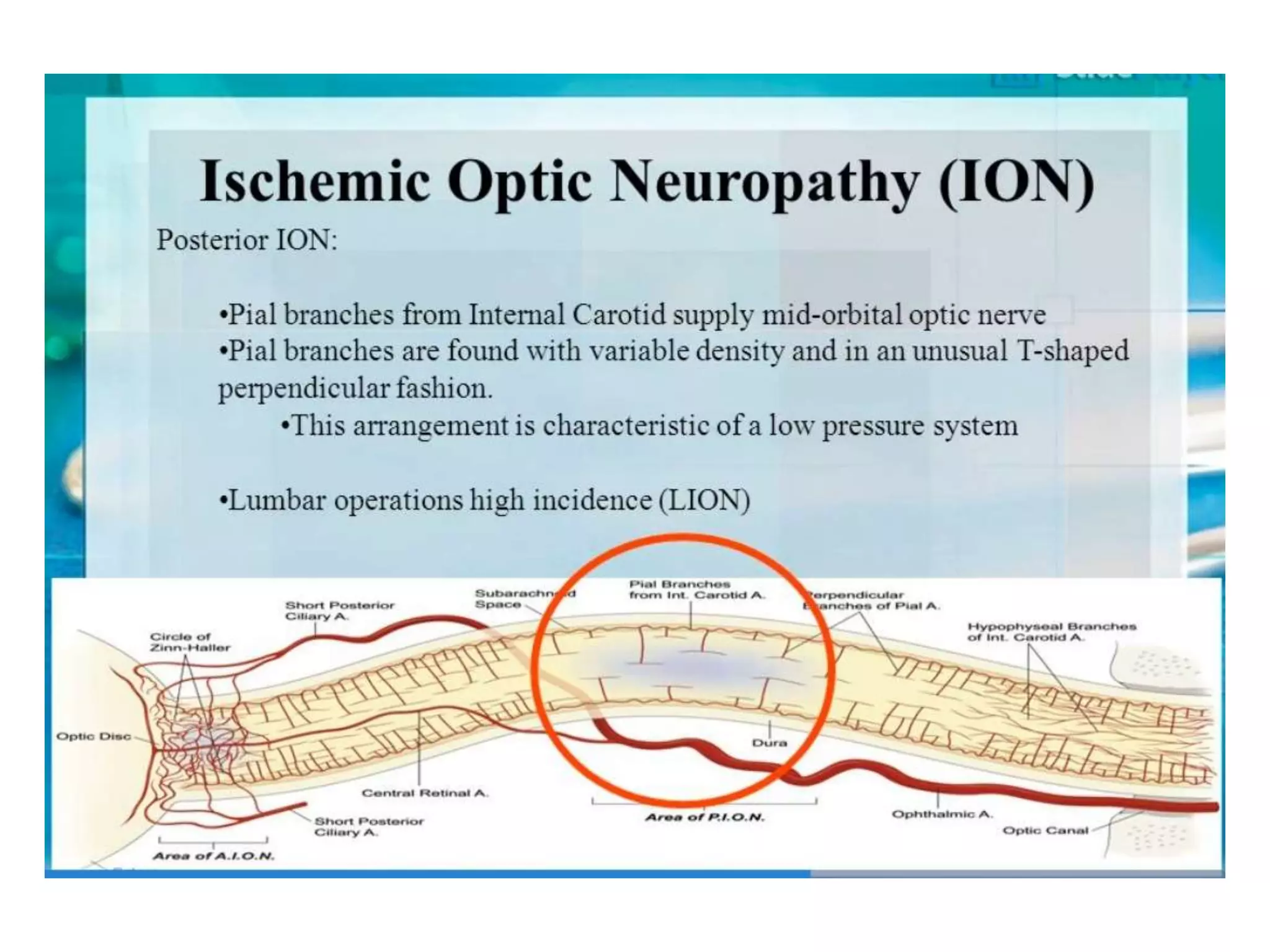
This document discusses various patient positions used during surgery and their associated risks. It describes positions such as supine, lateral, prone, lithotomy, and variations like Trendelenburg. For each position, it details anatomical support, physiological impacts, and potential complications. Positioning-related nerve injuries, pressure points, vascular complications, and retinal ischemia are addressed. Proper padding, stabilization, and frequent reassessment are emphasized to prevent issues from sustained pressures.