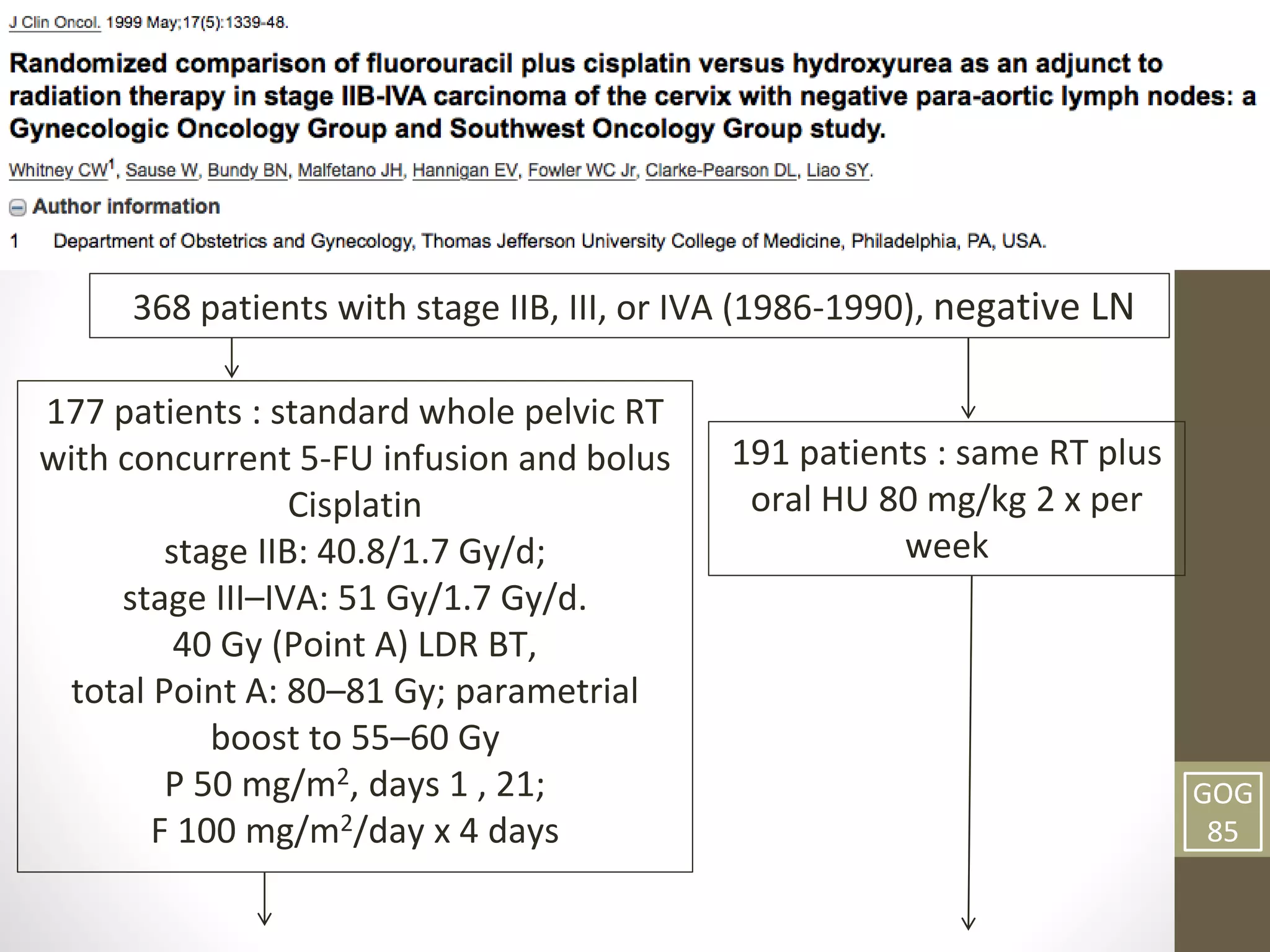
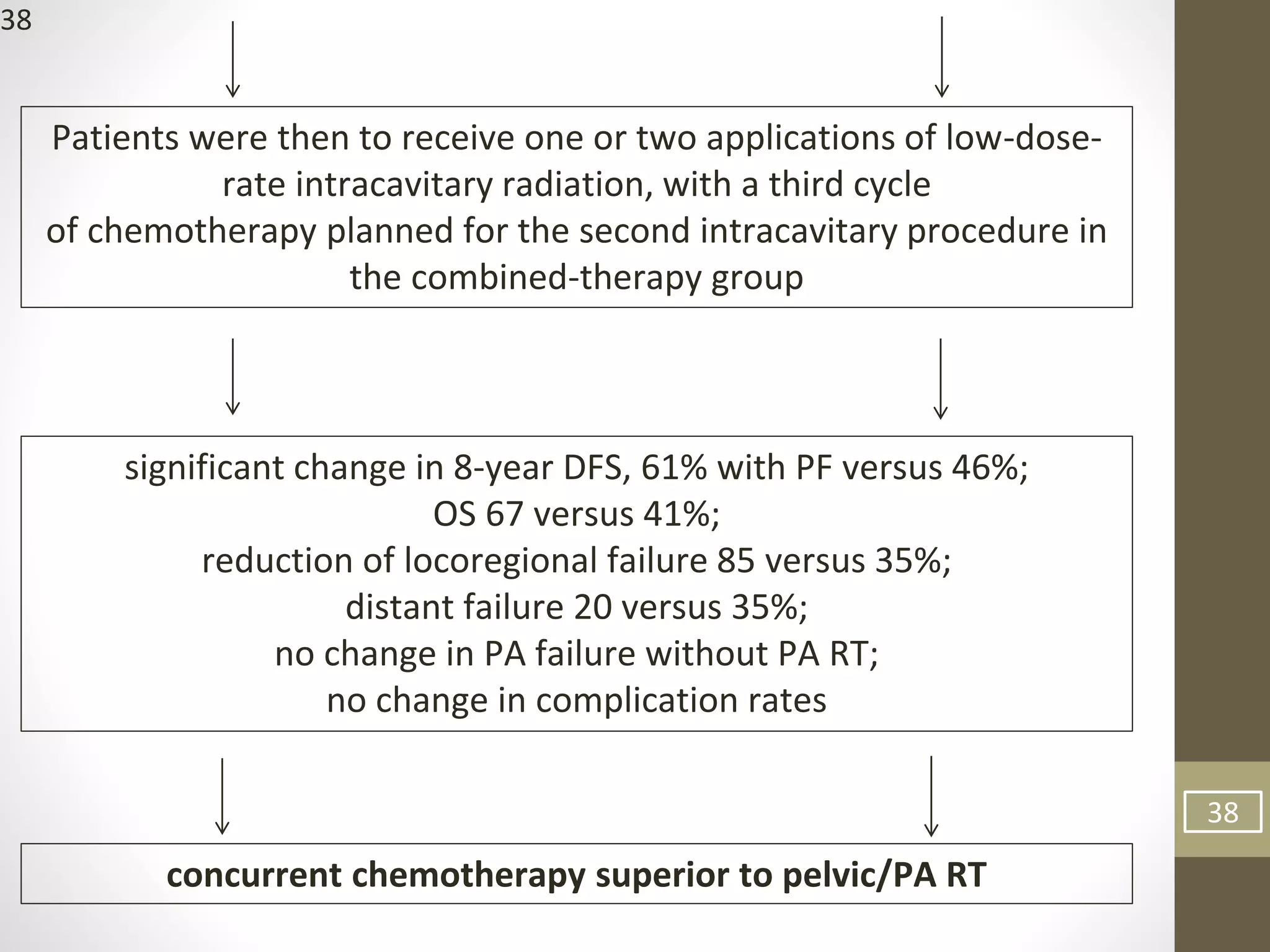
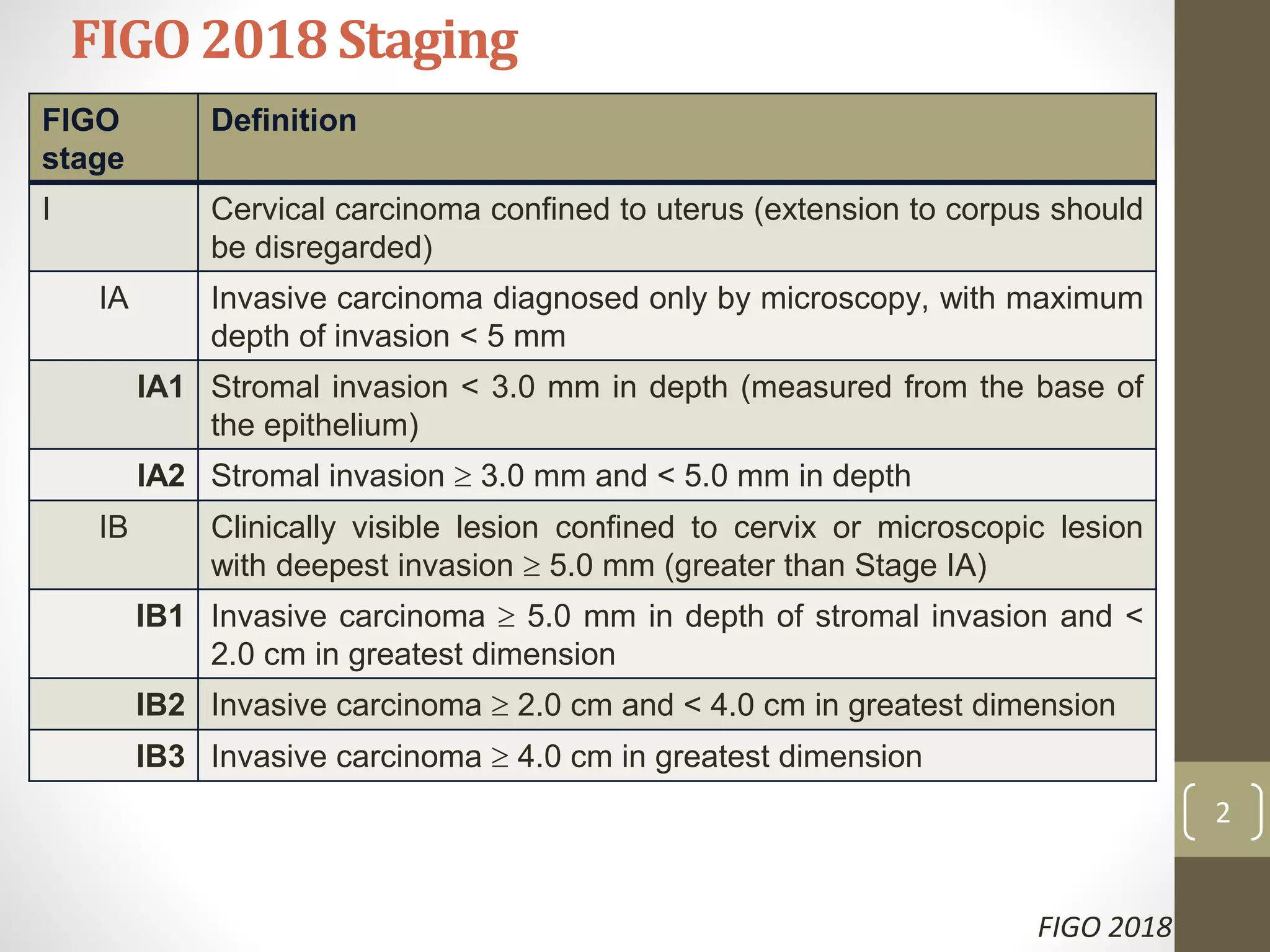
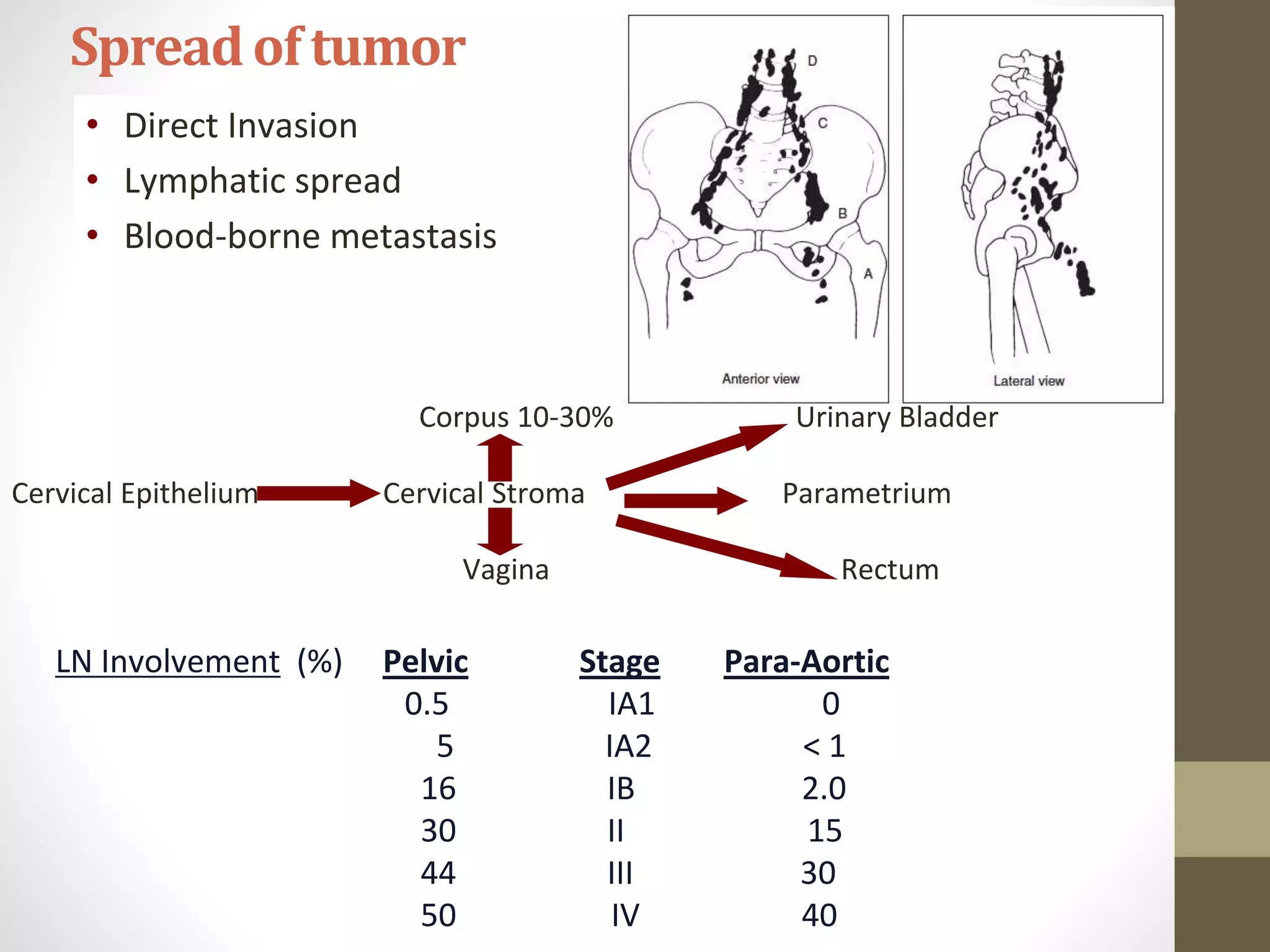
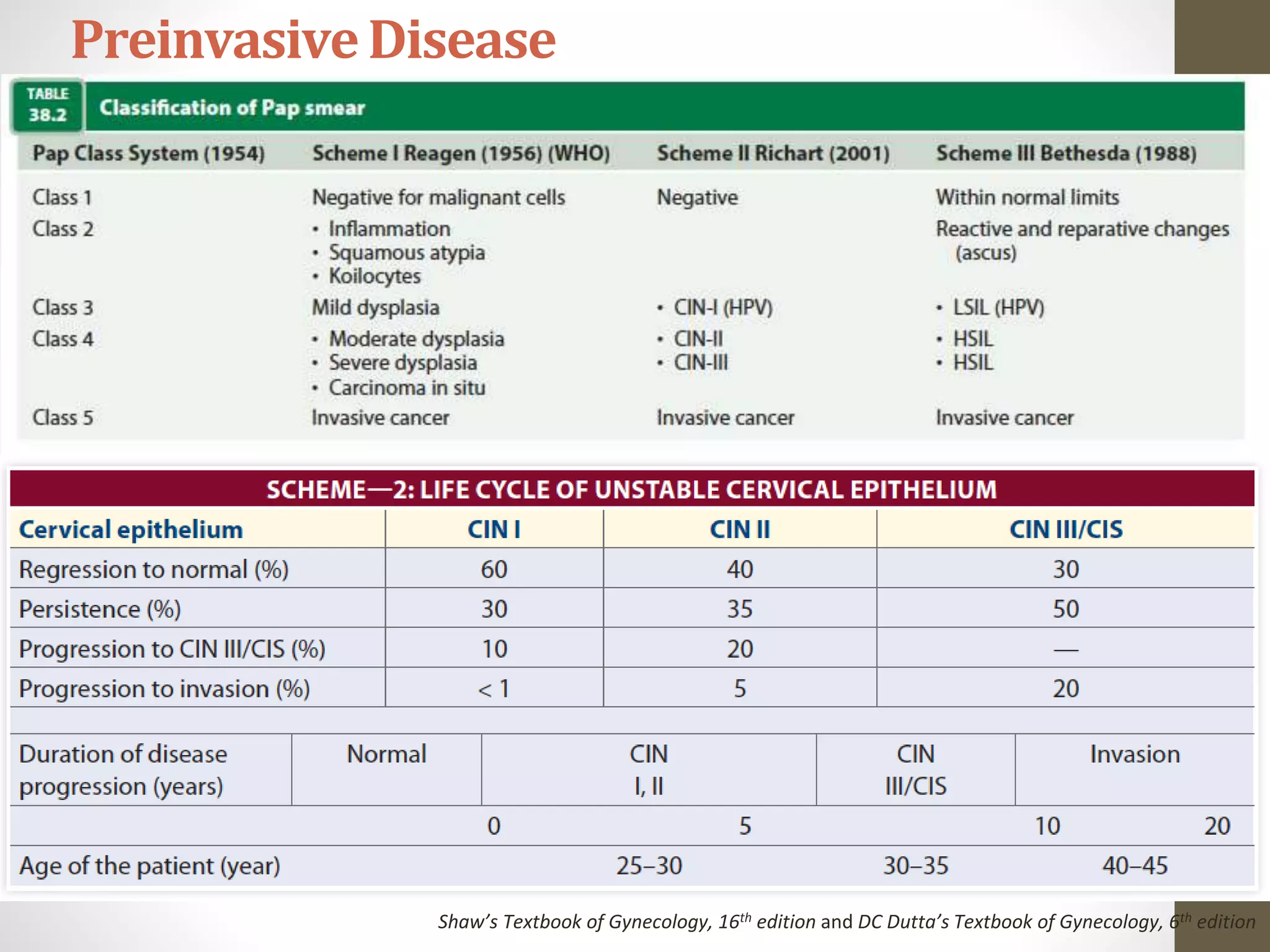
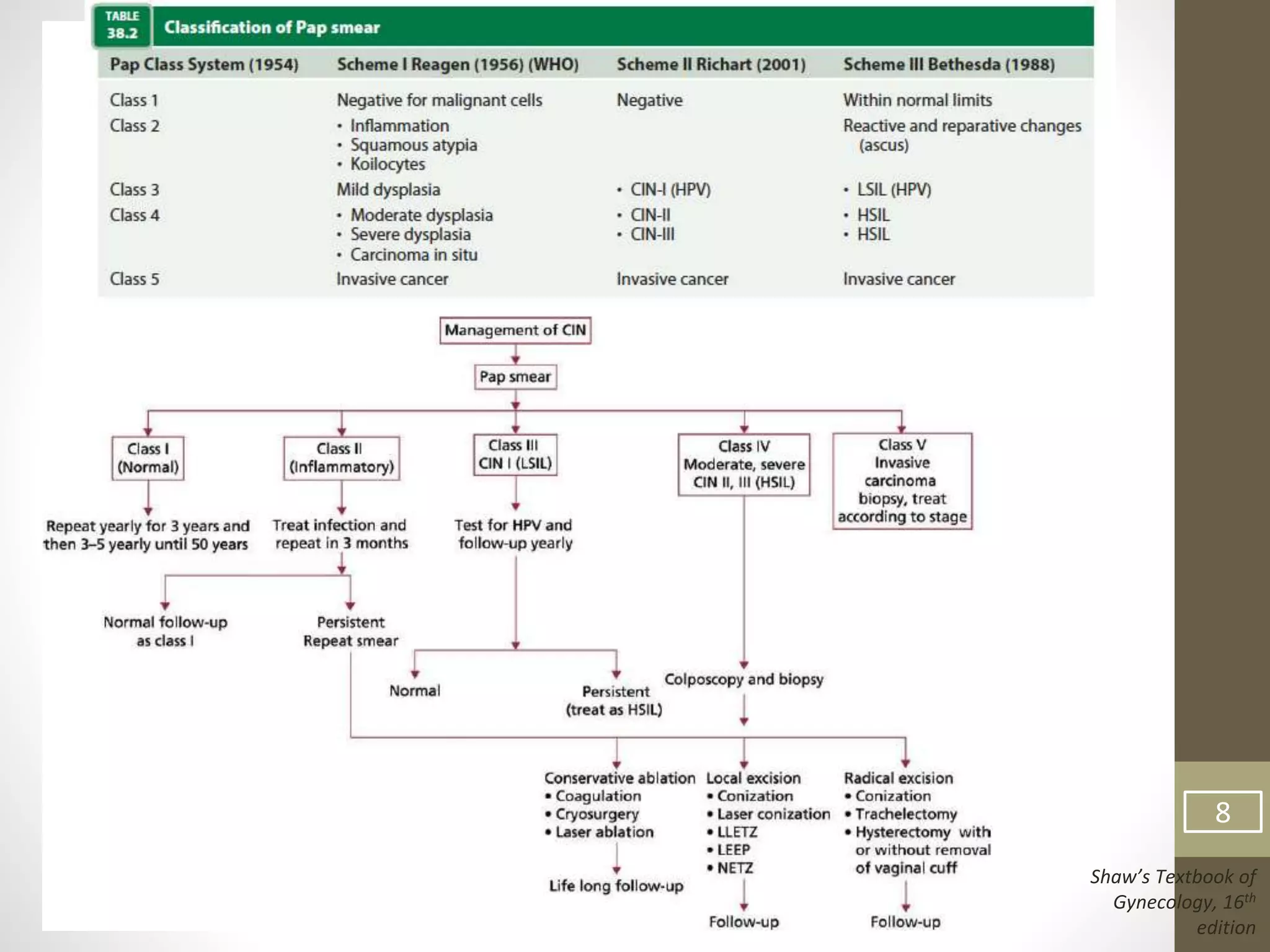
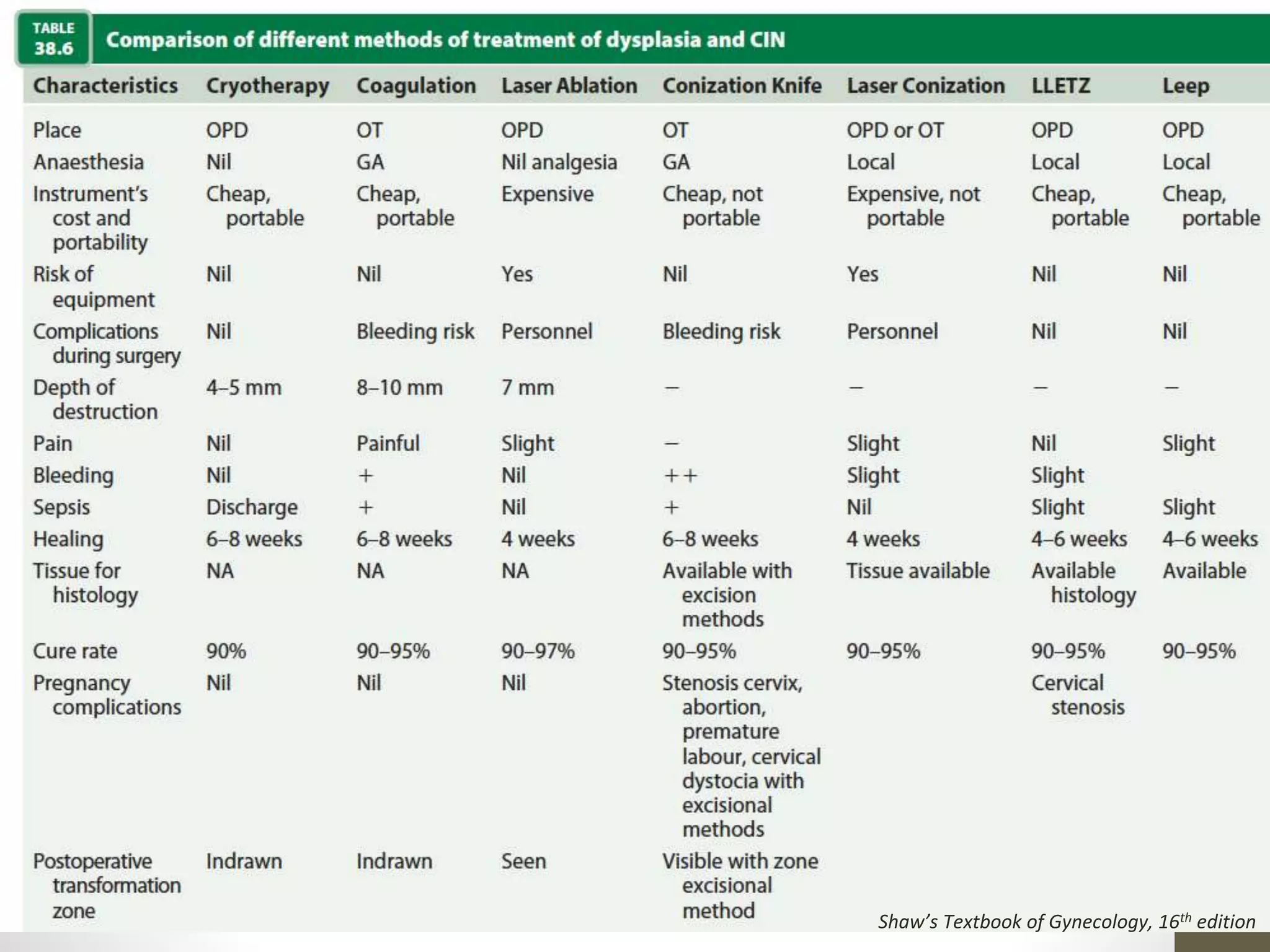
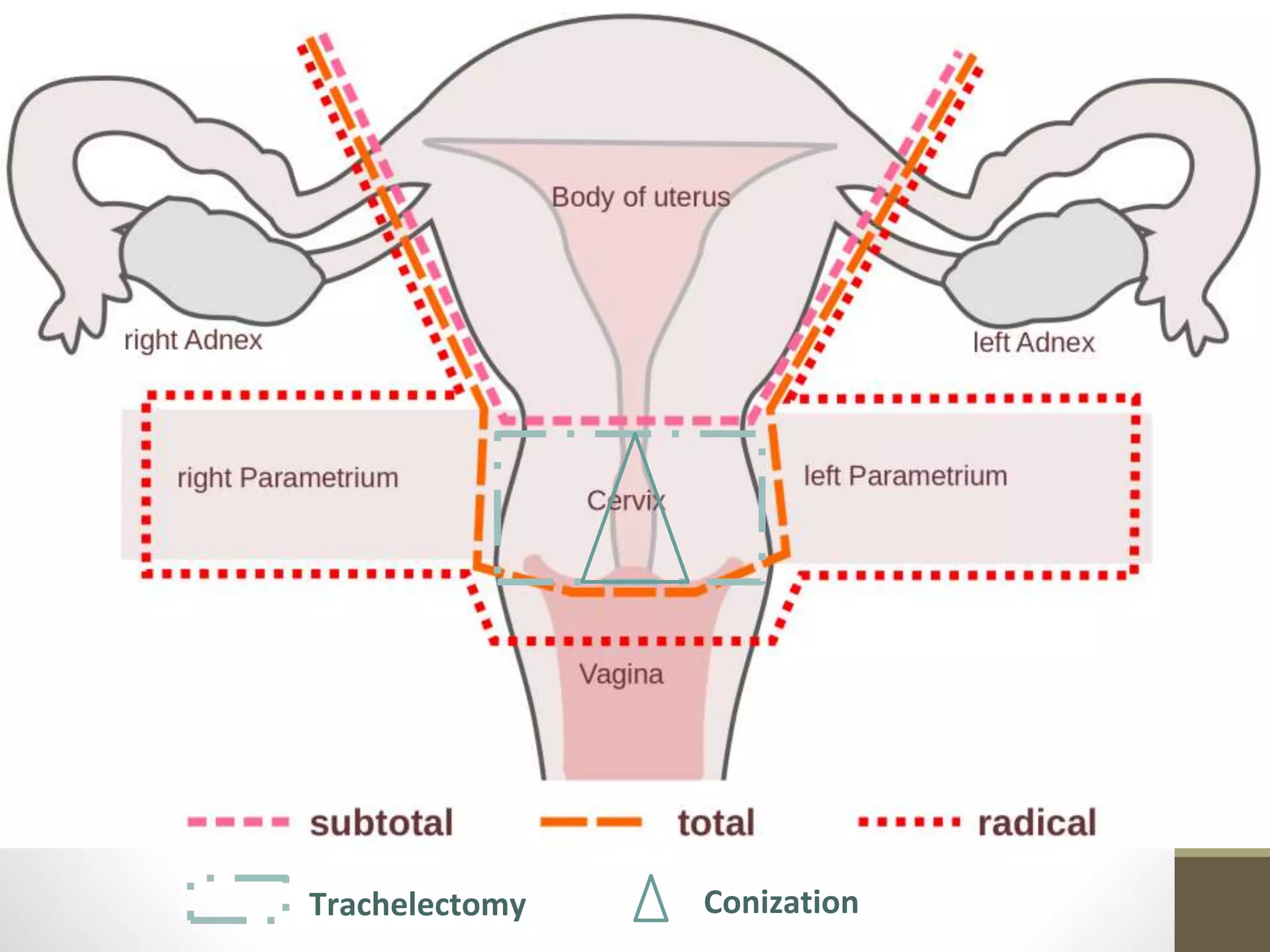
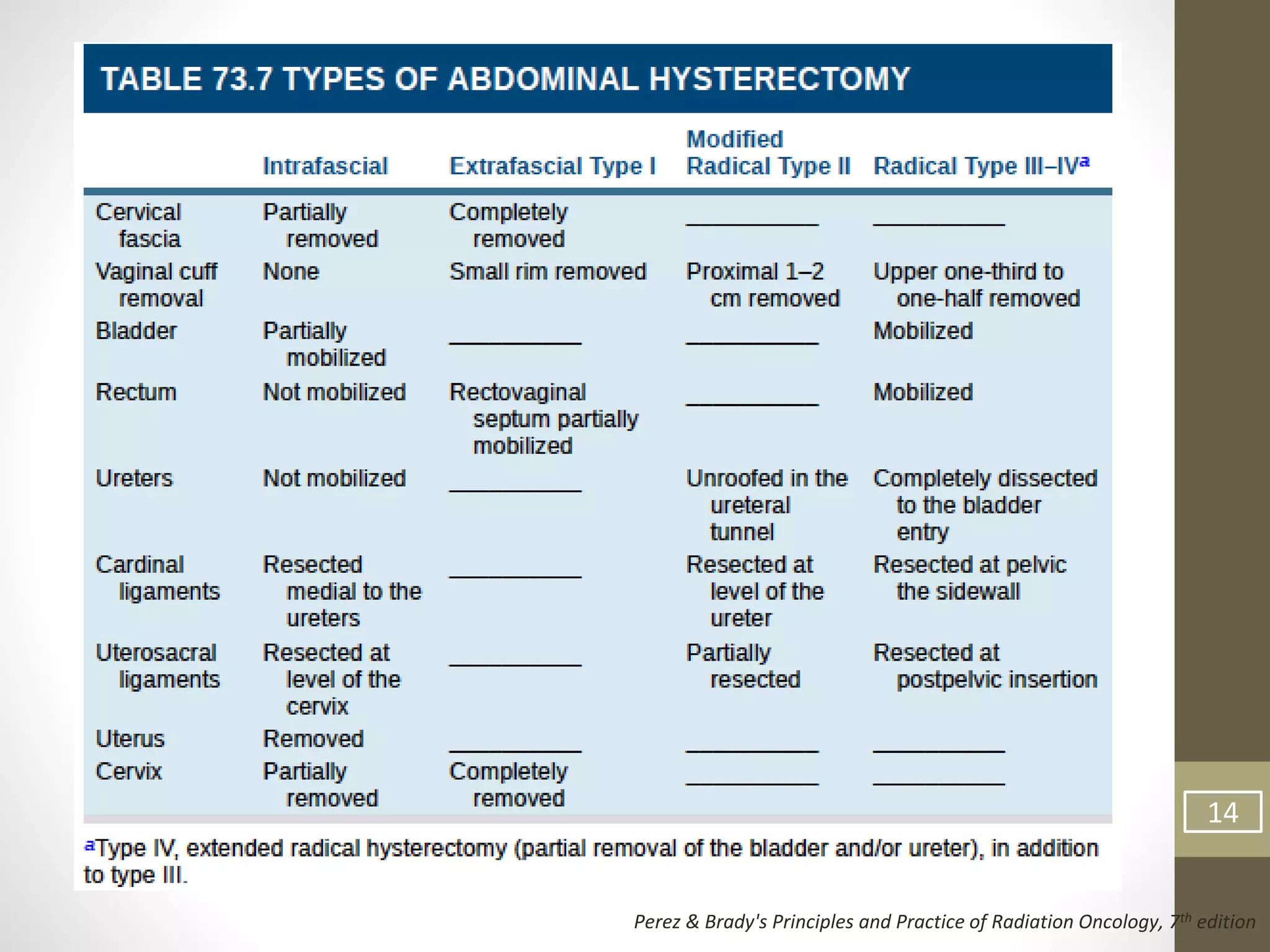
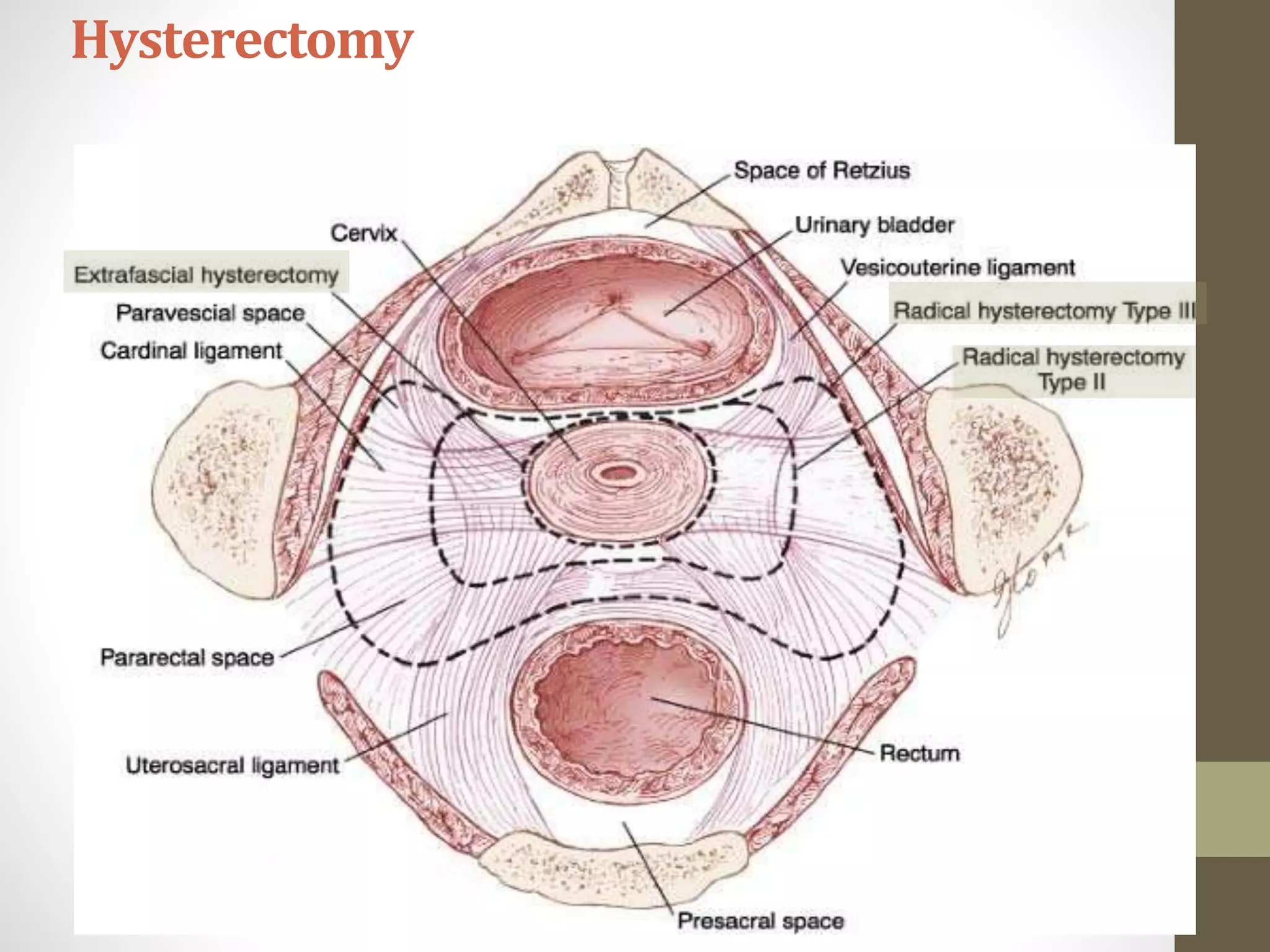
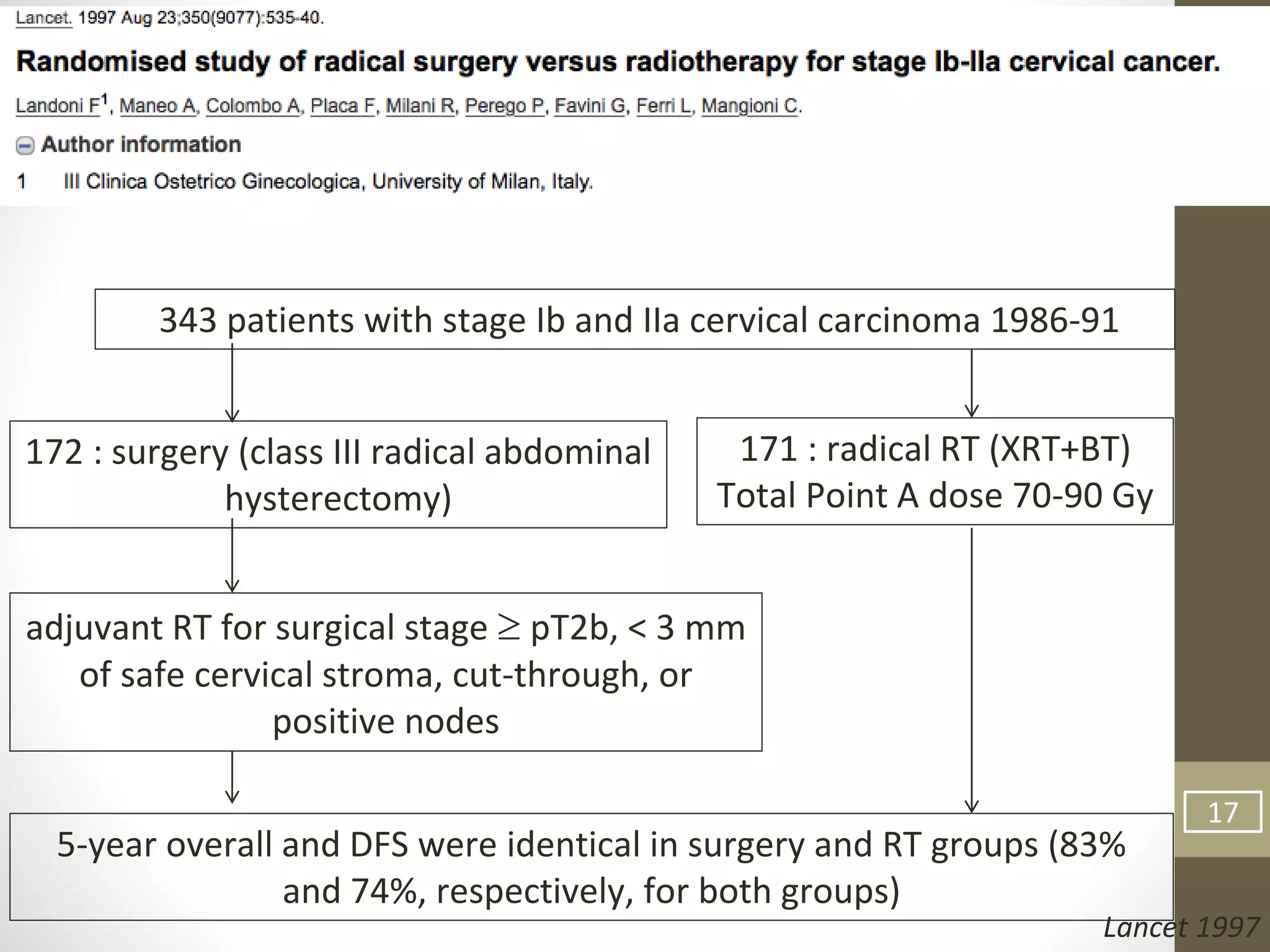
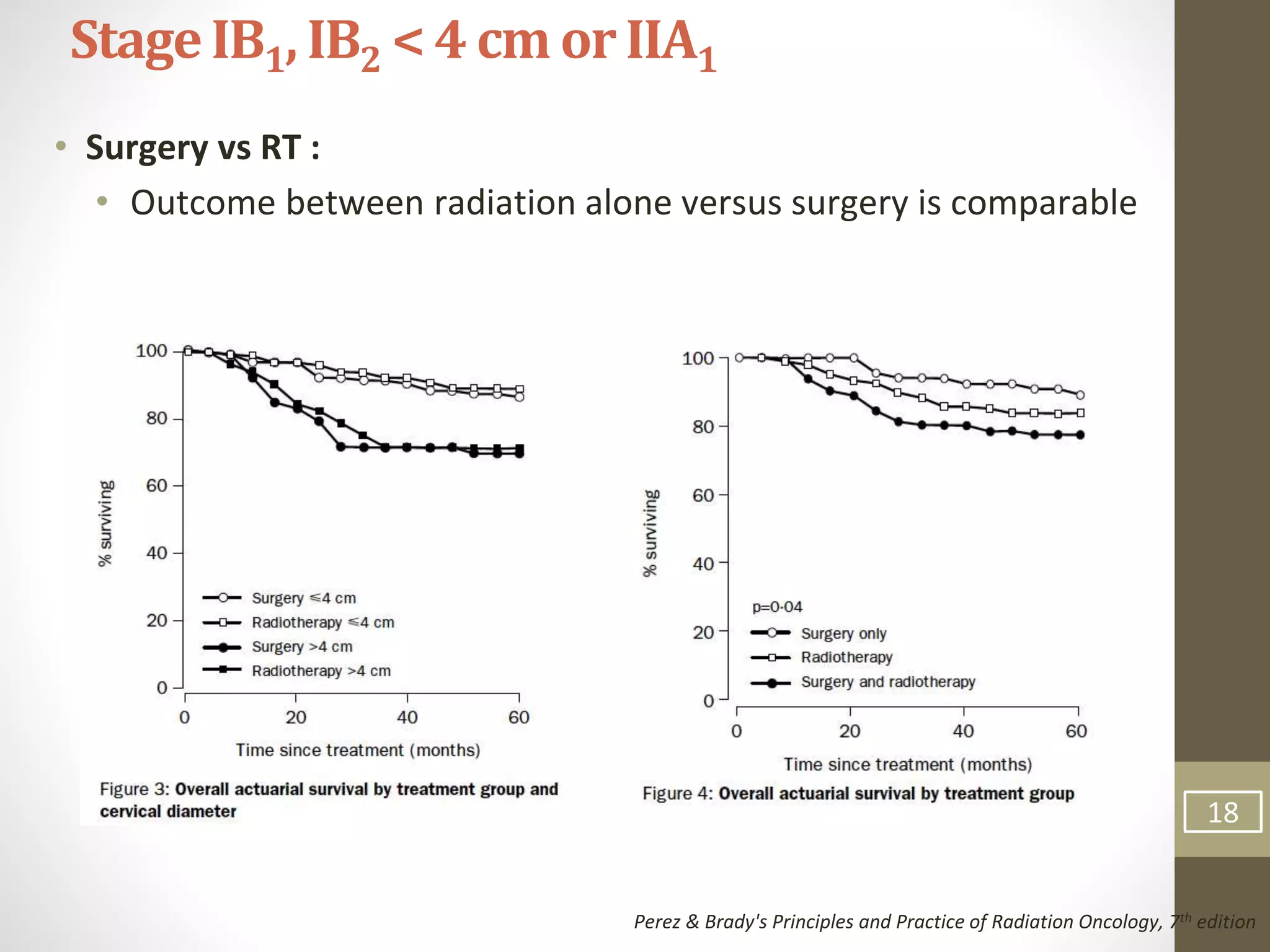
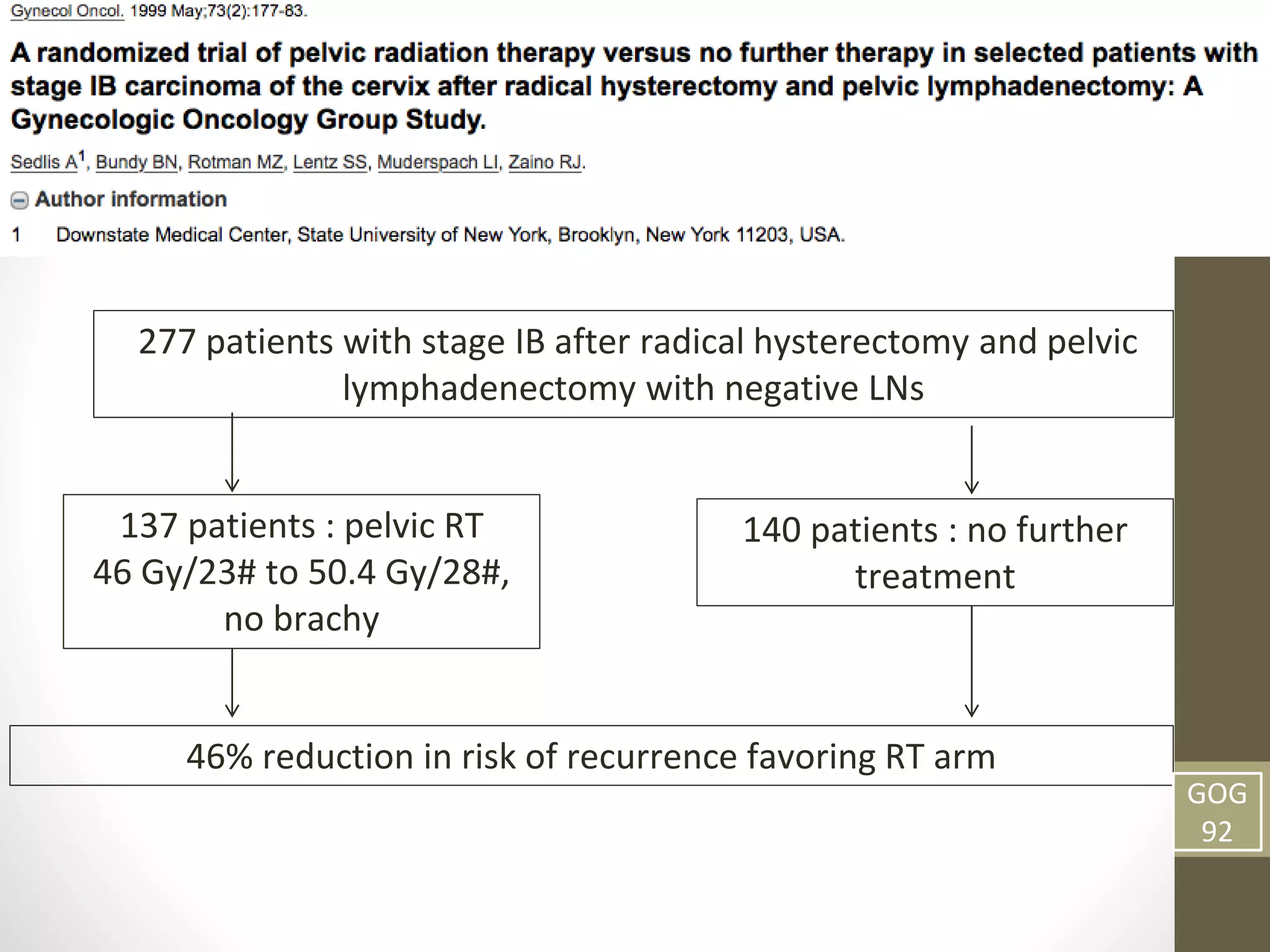
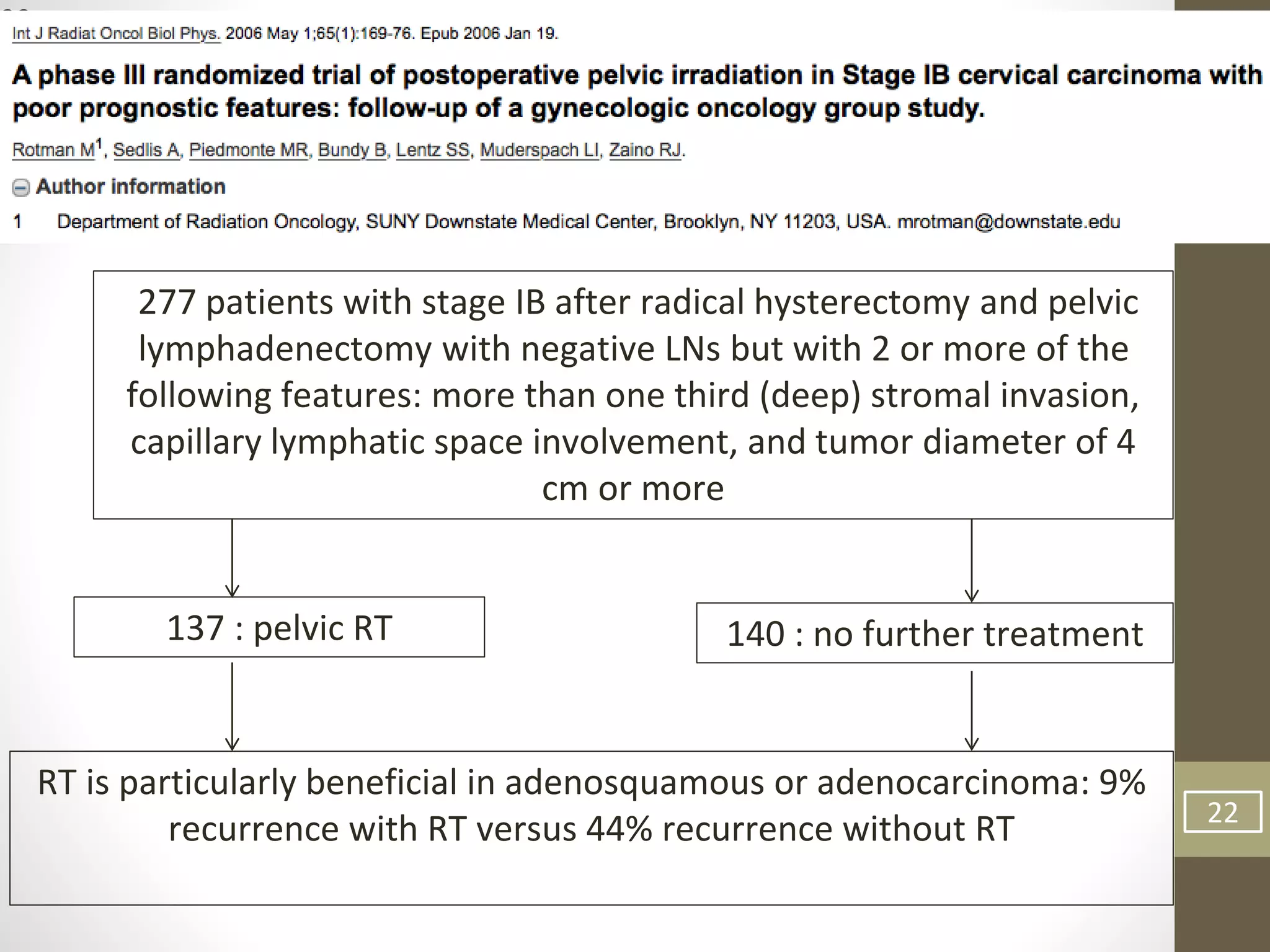
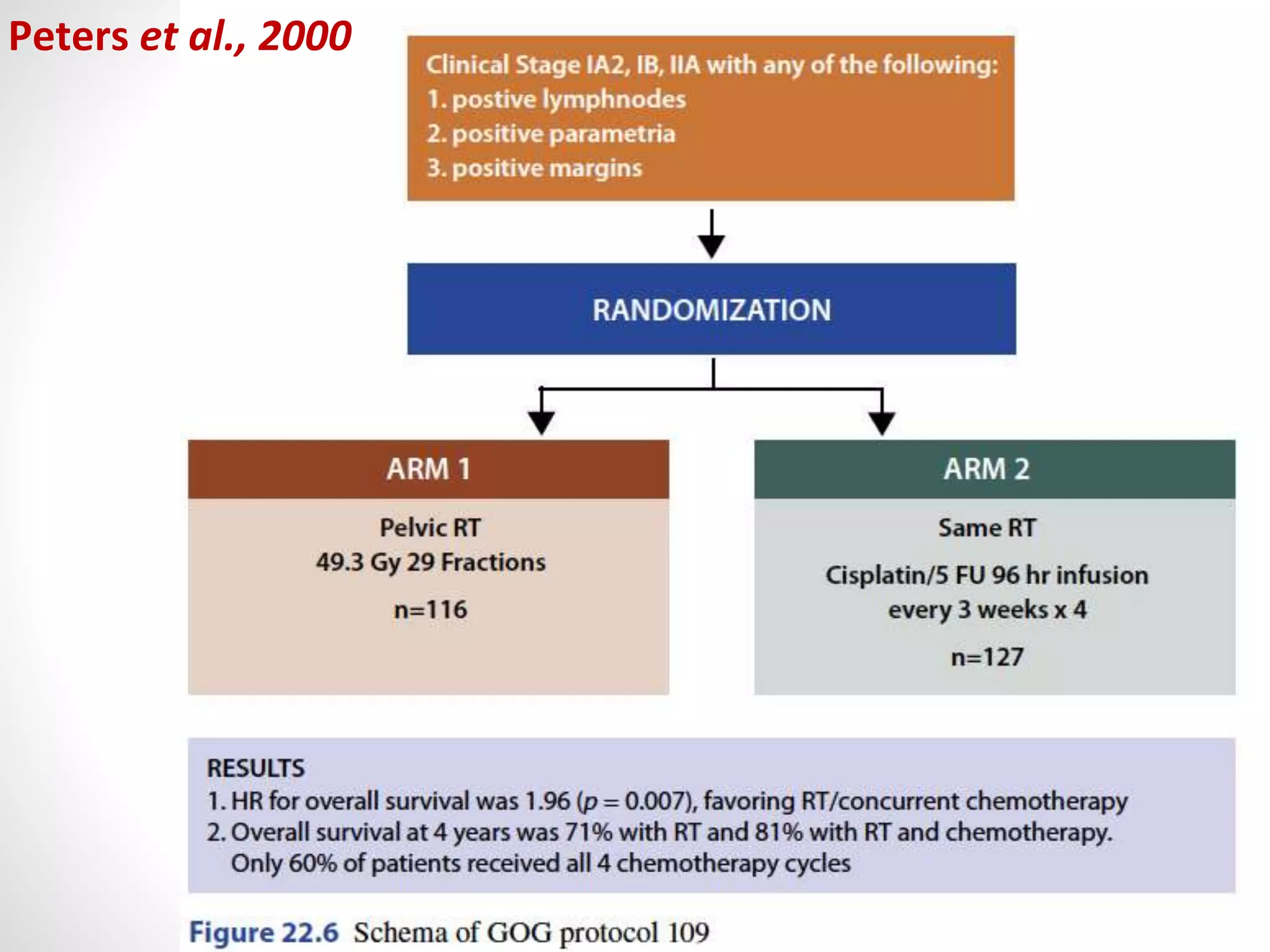
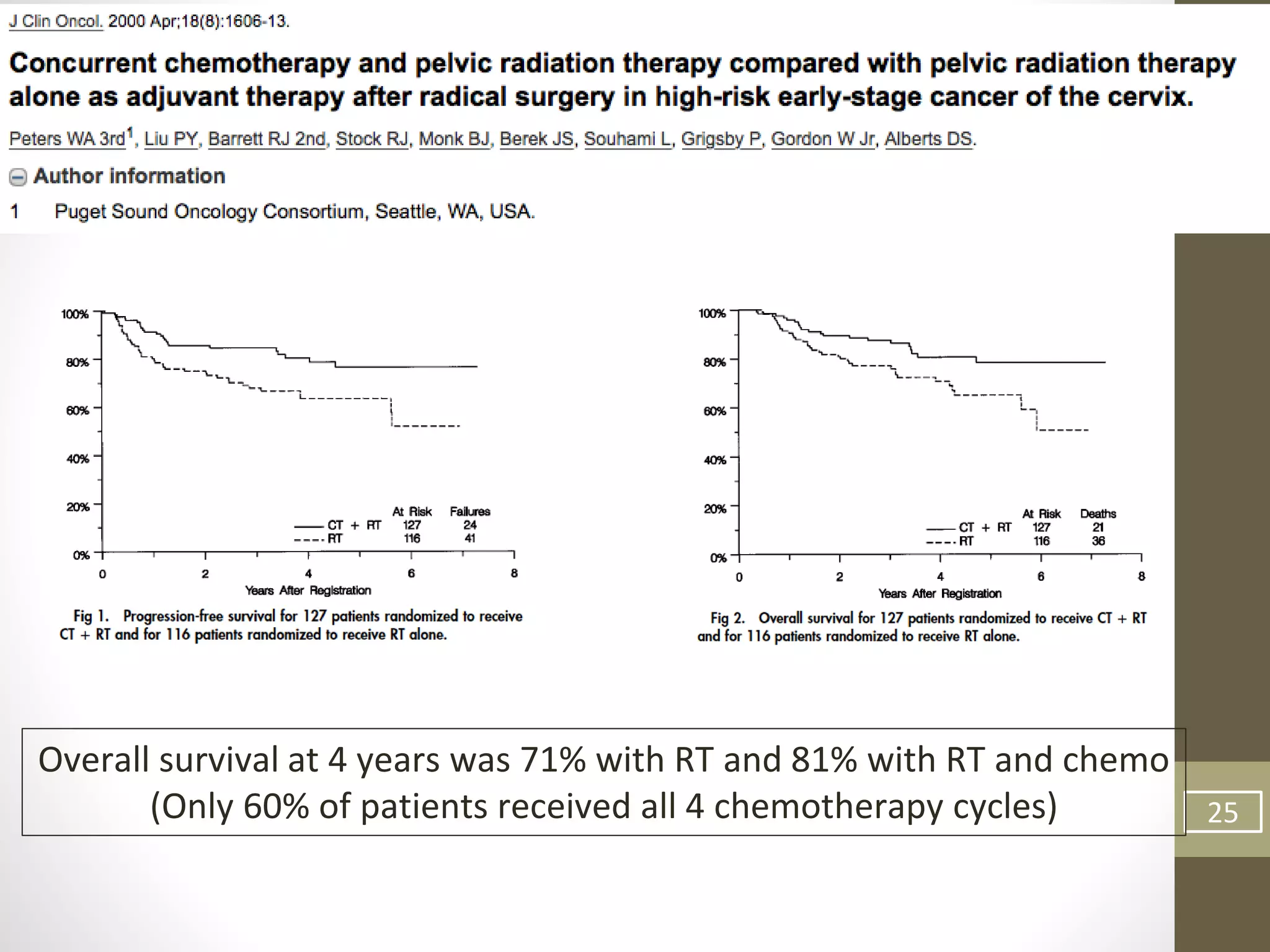
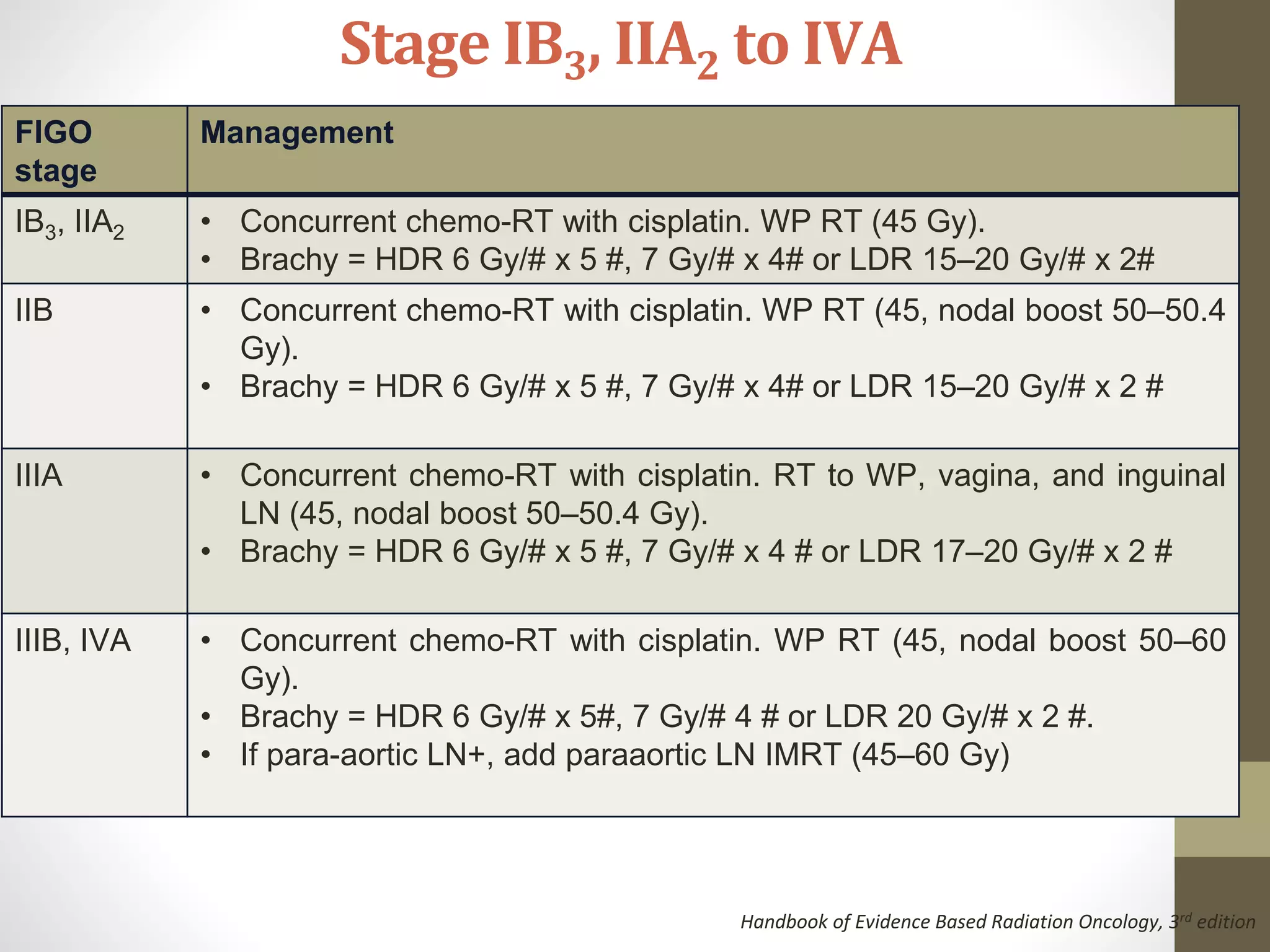
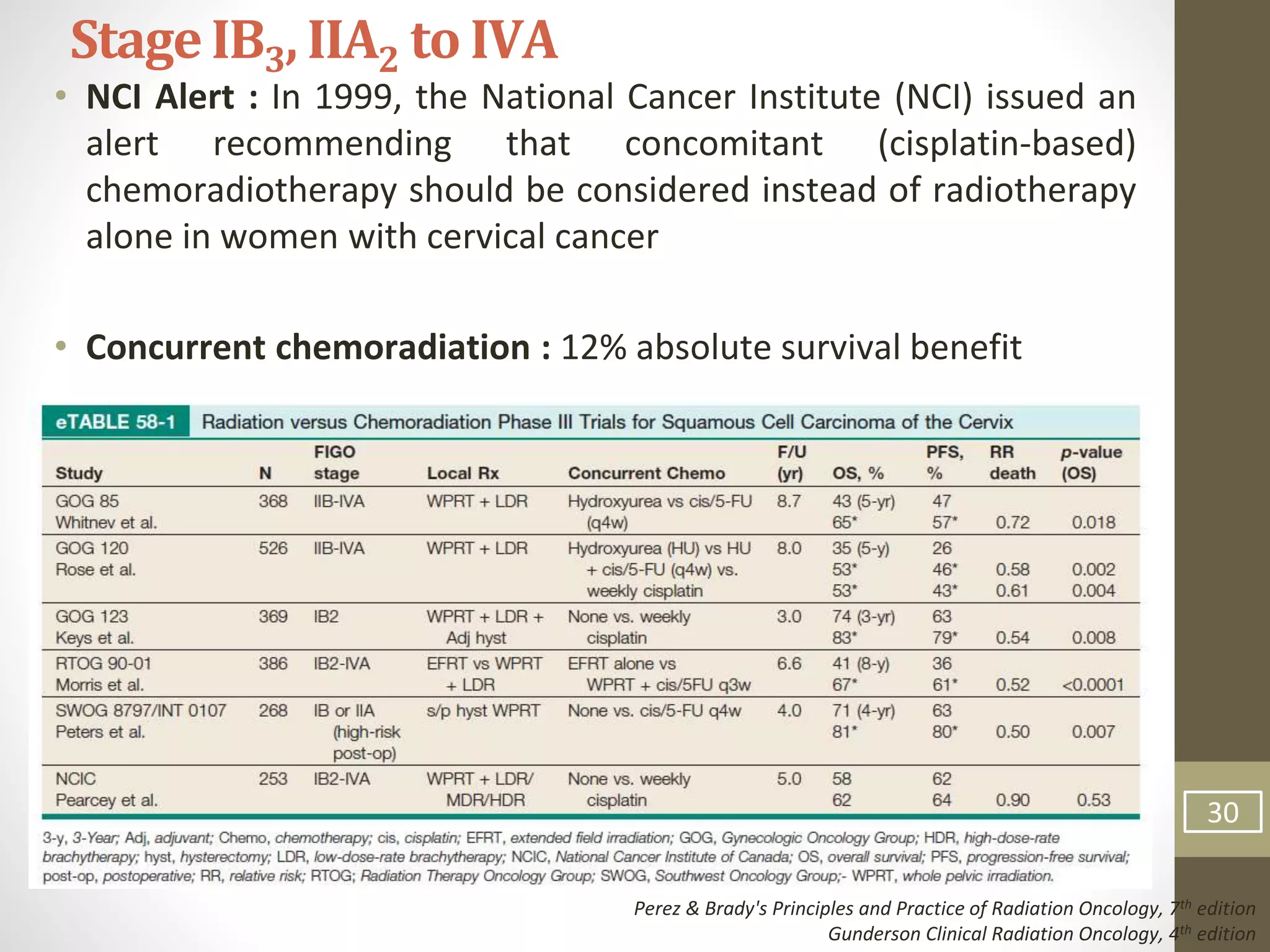
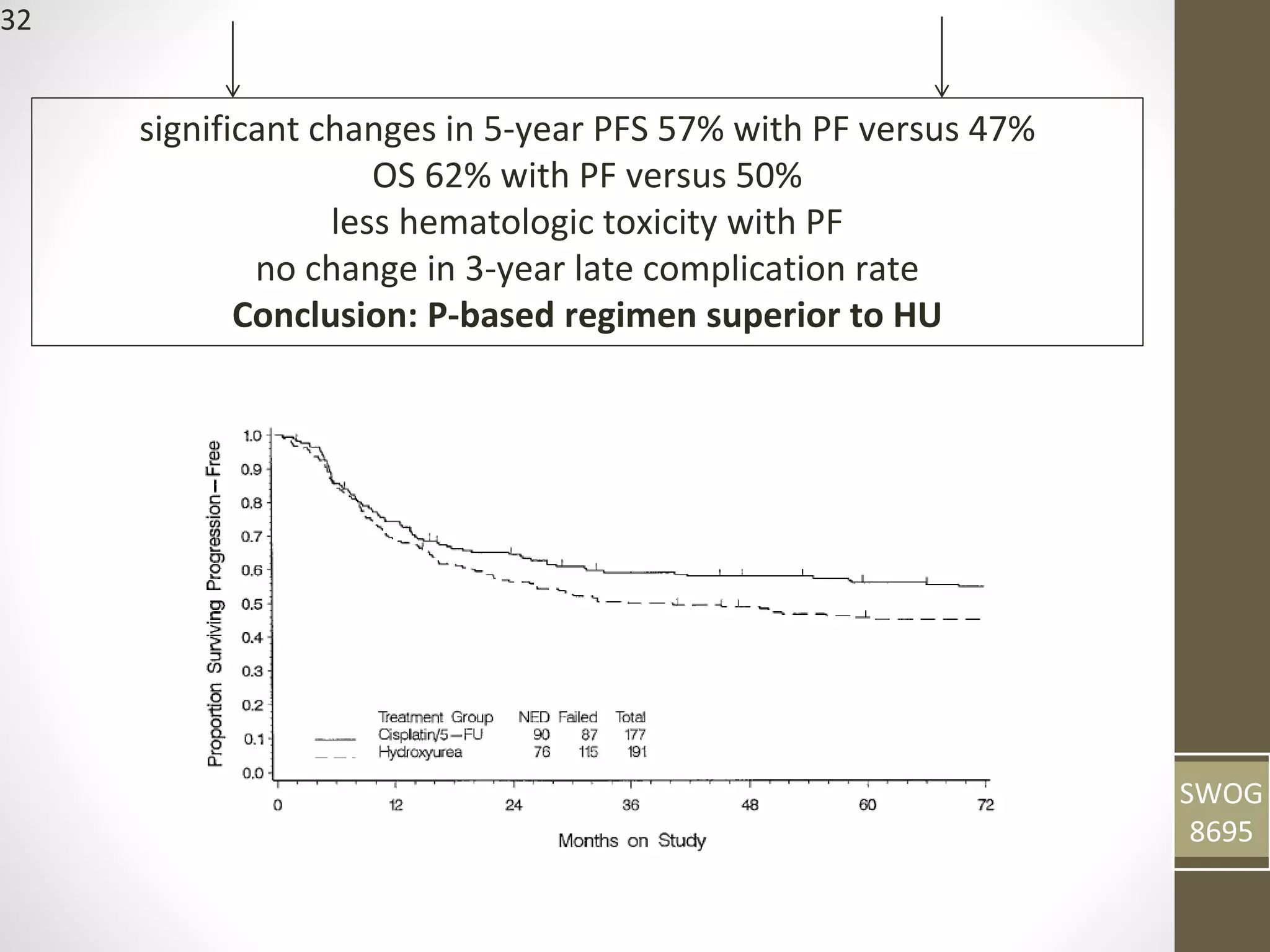
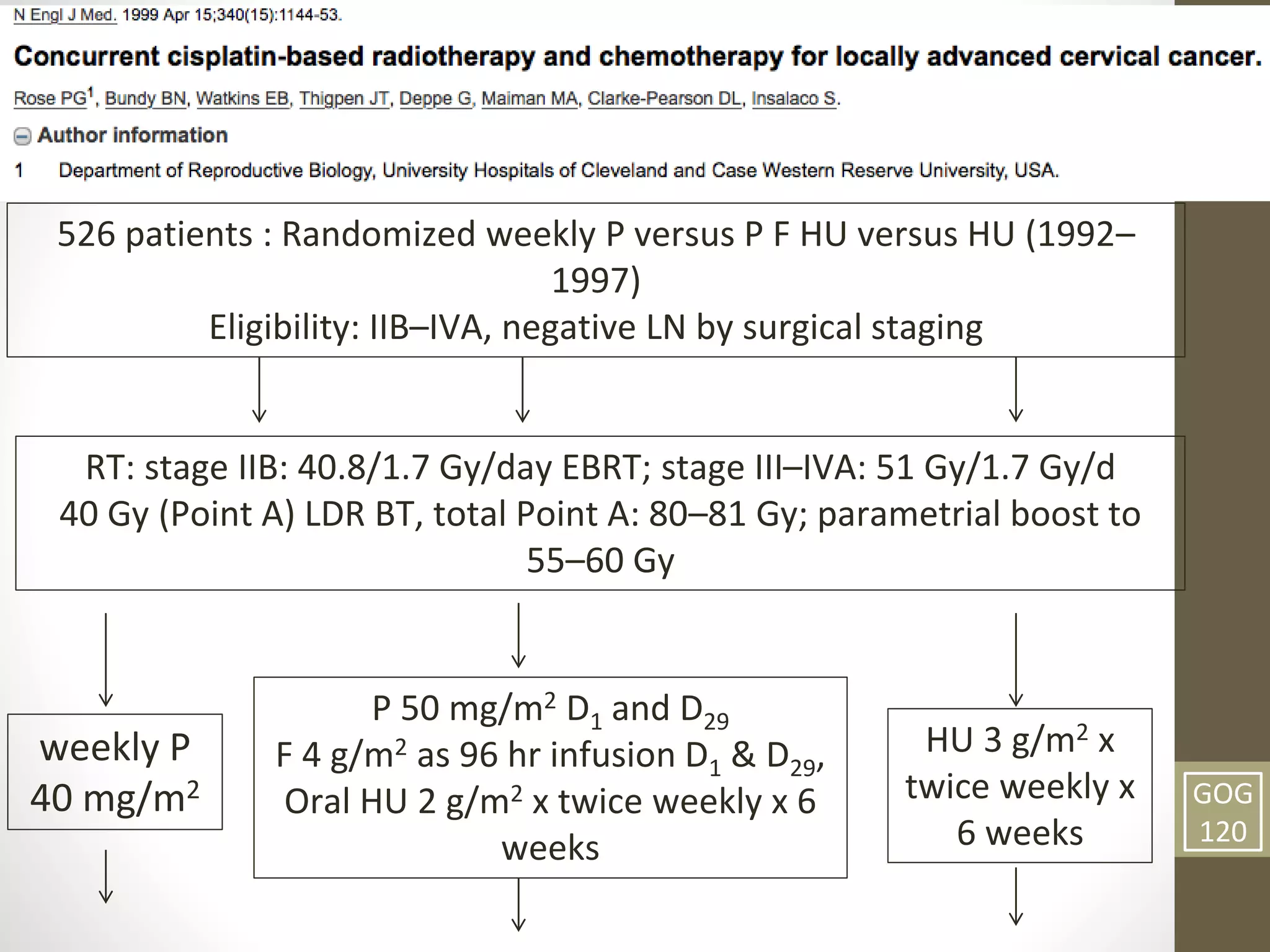
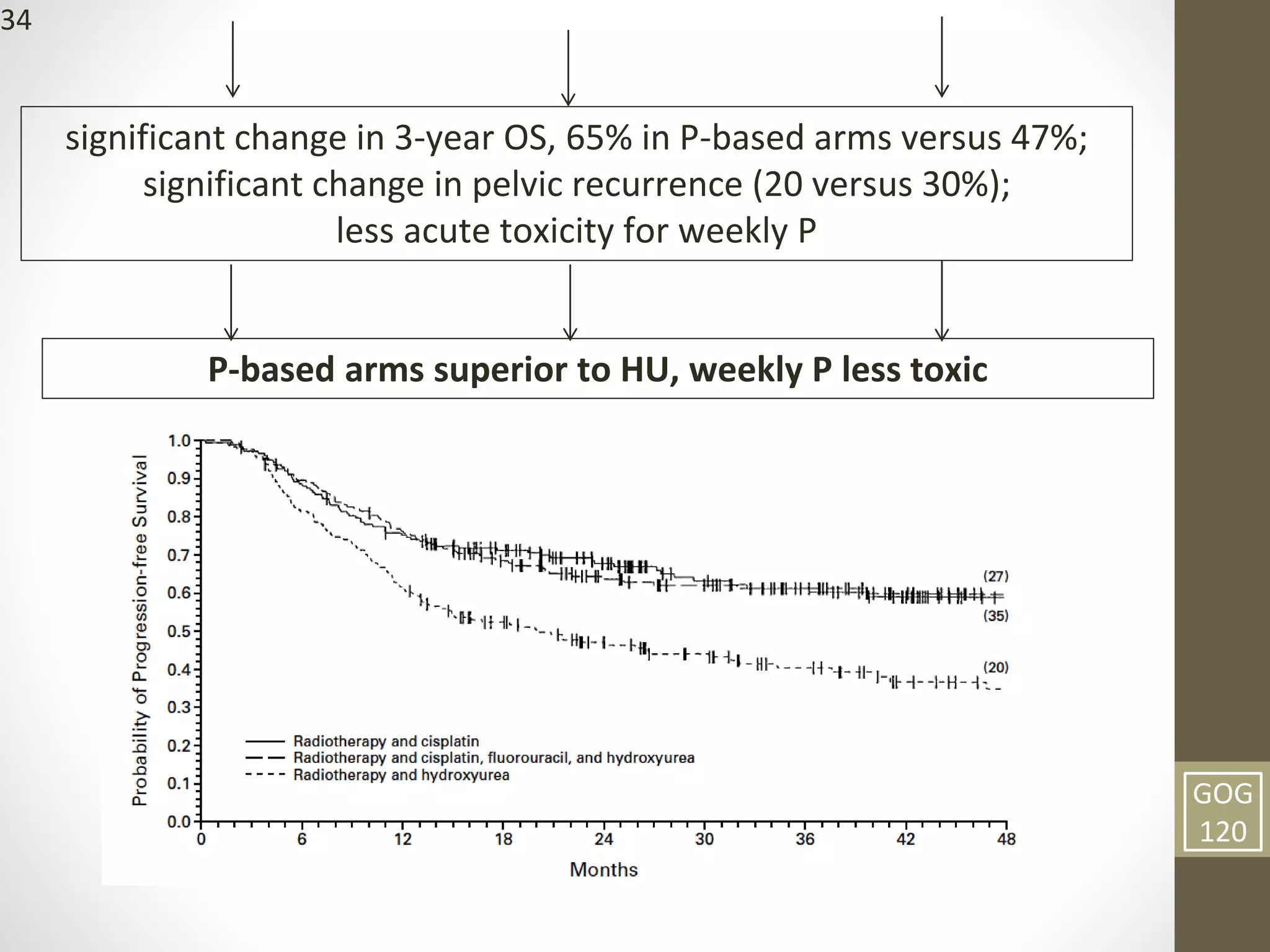
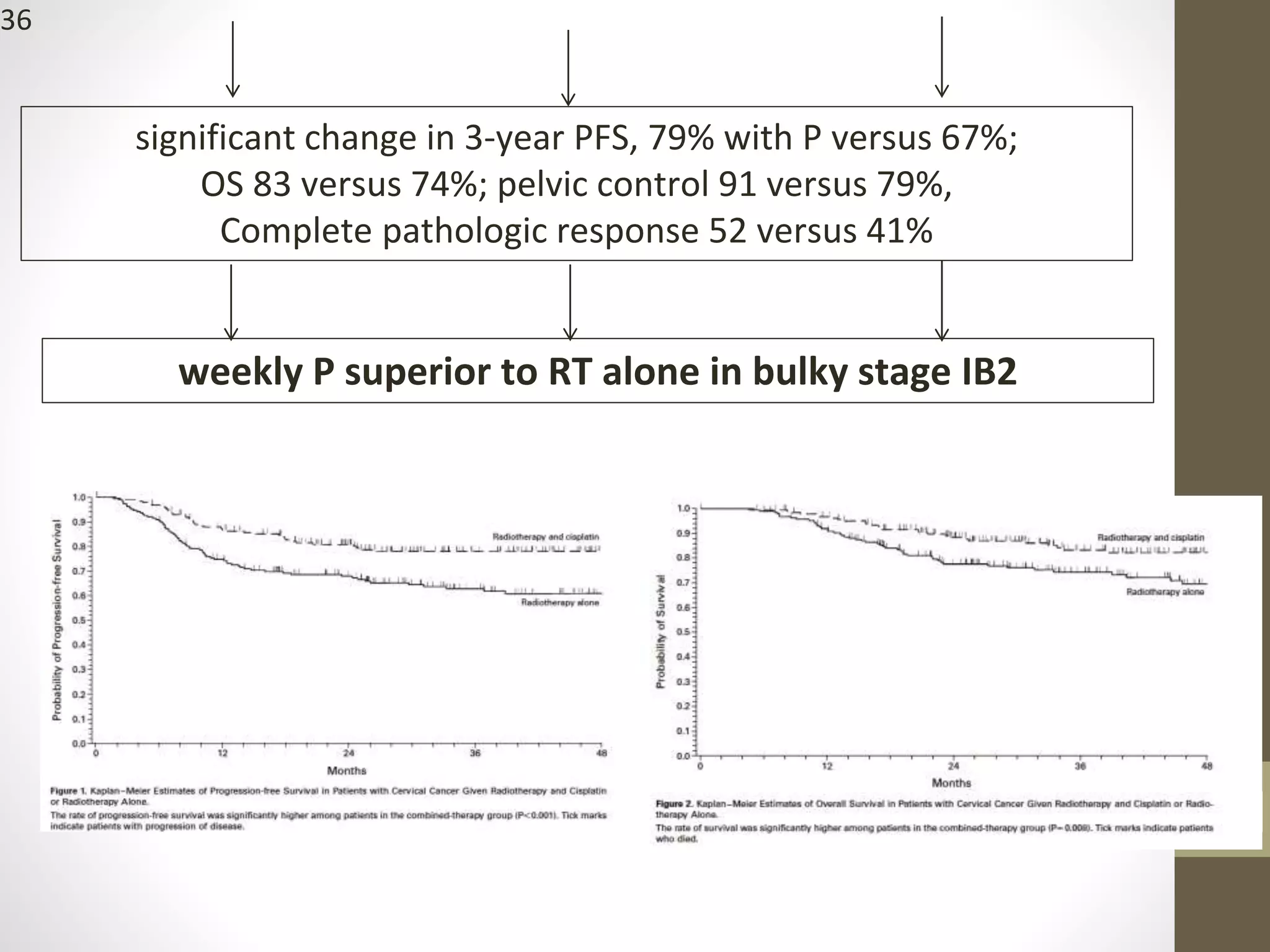
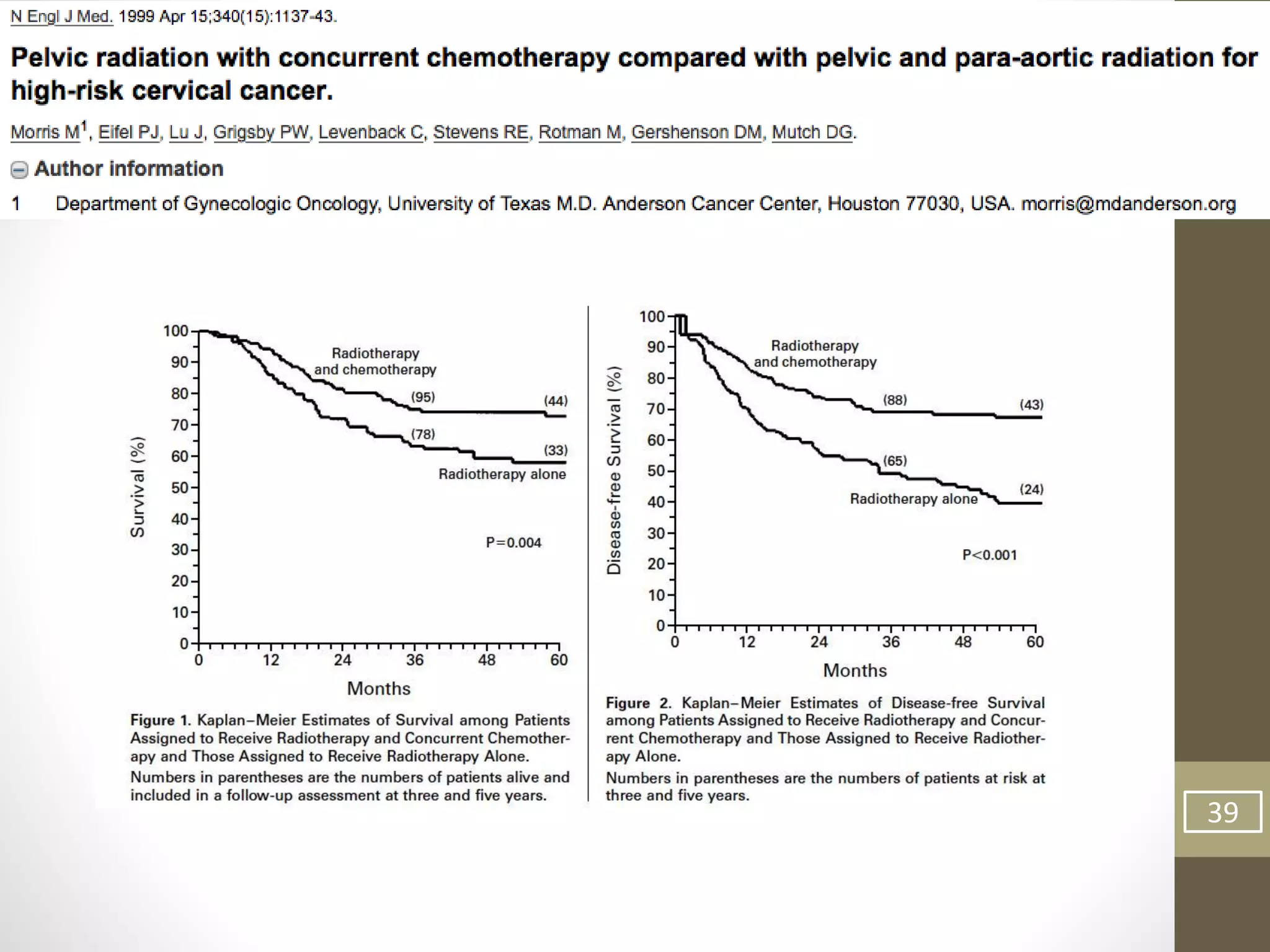
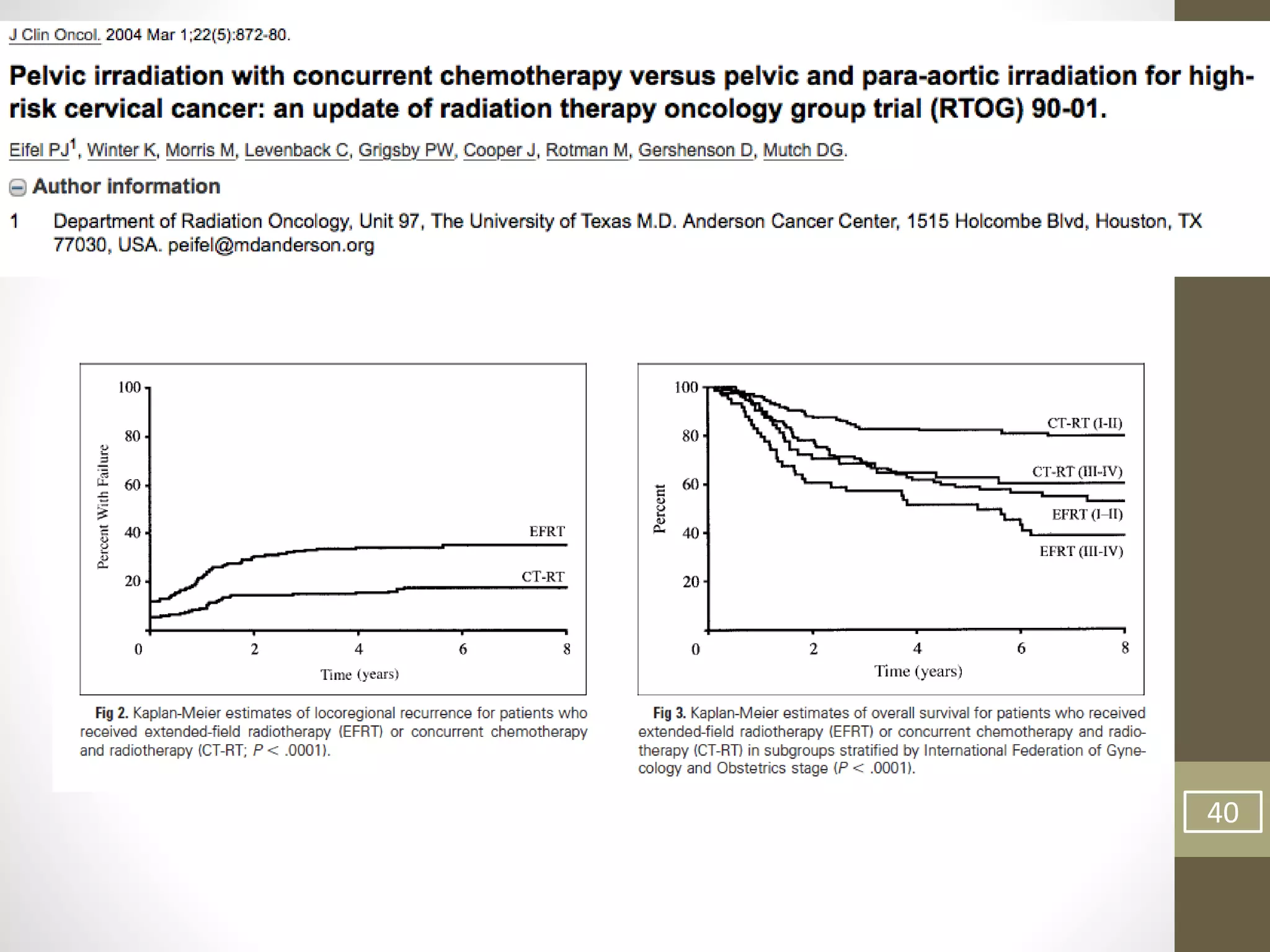
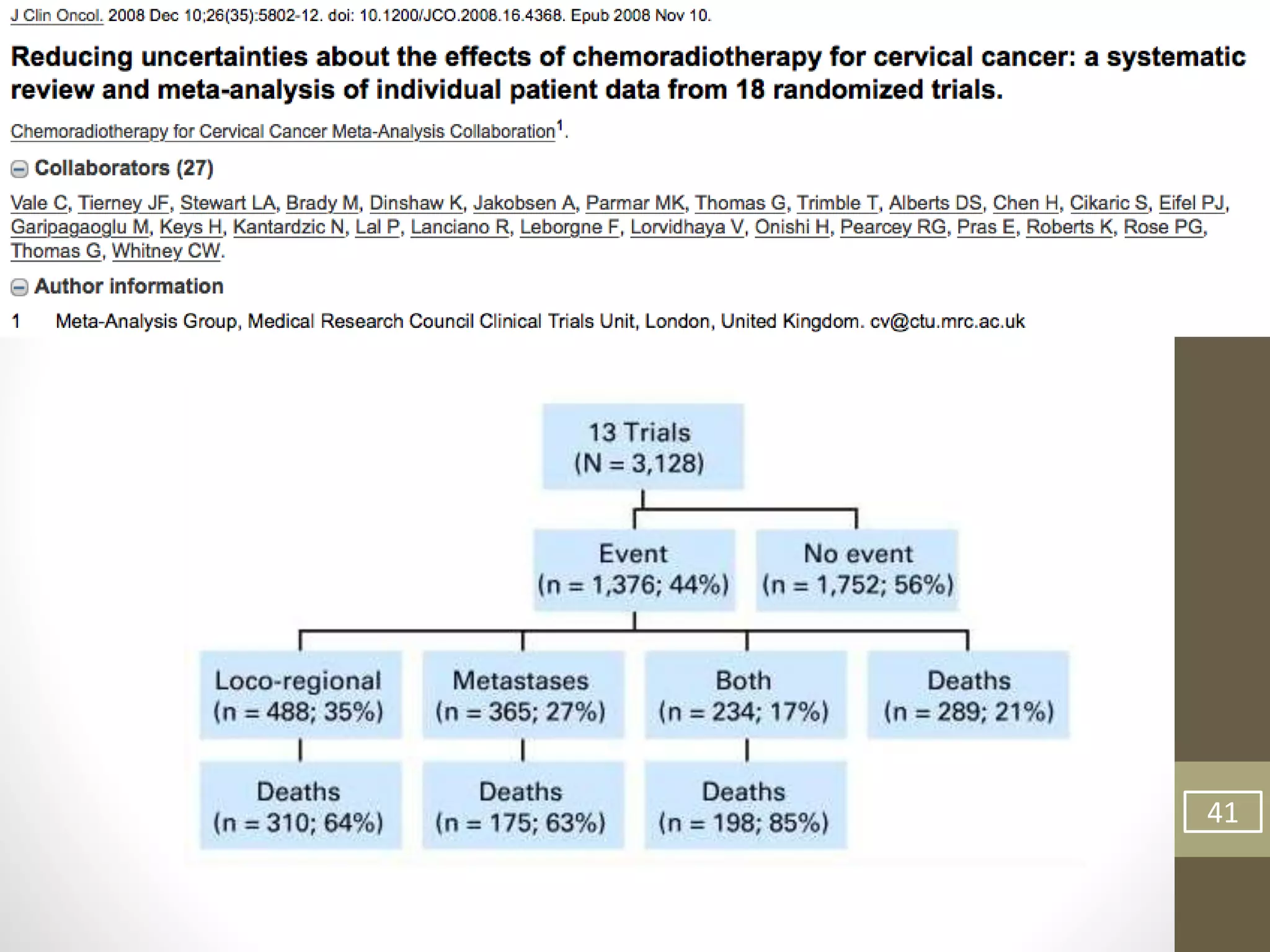
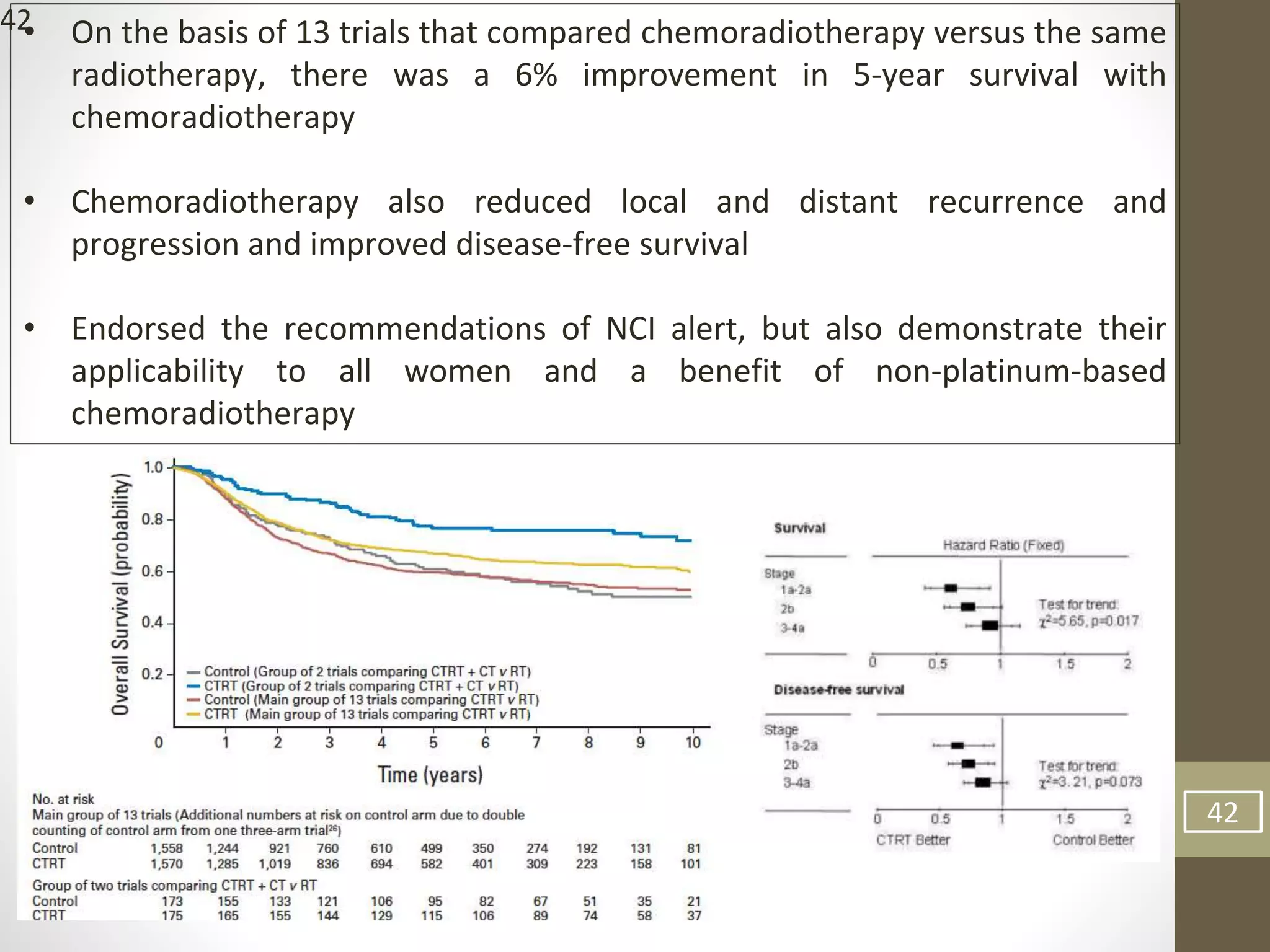
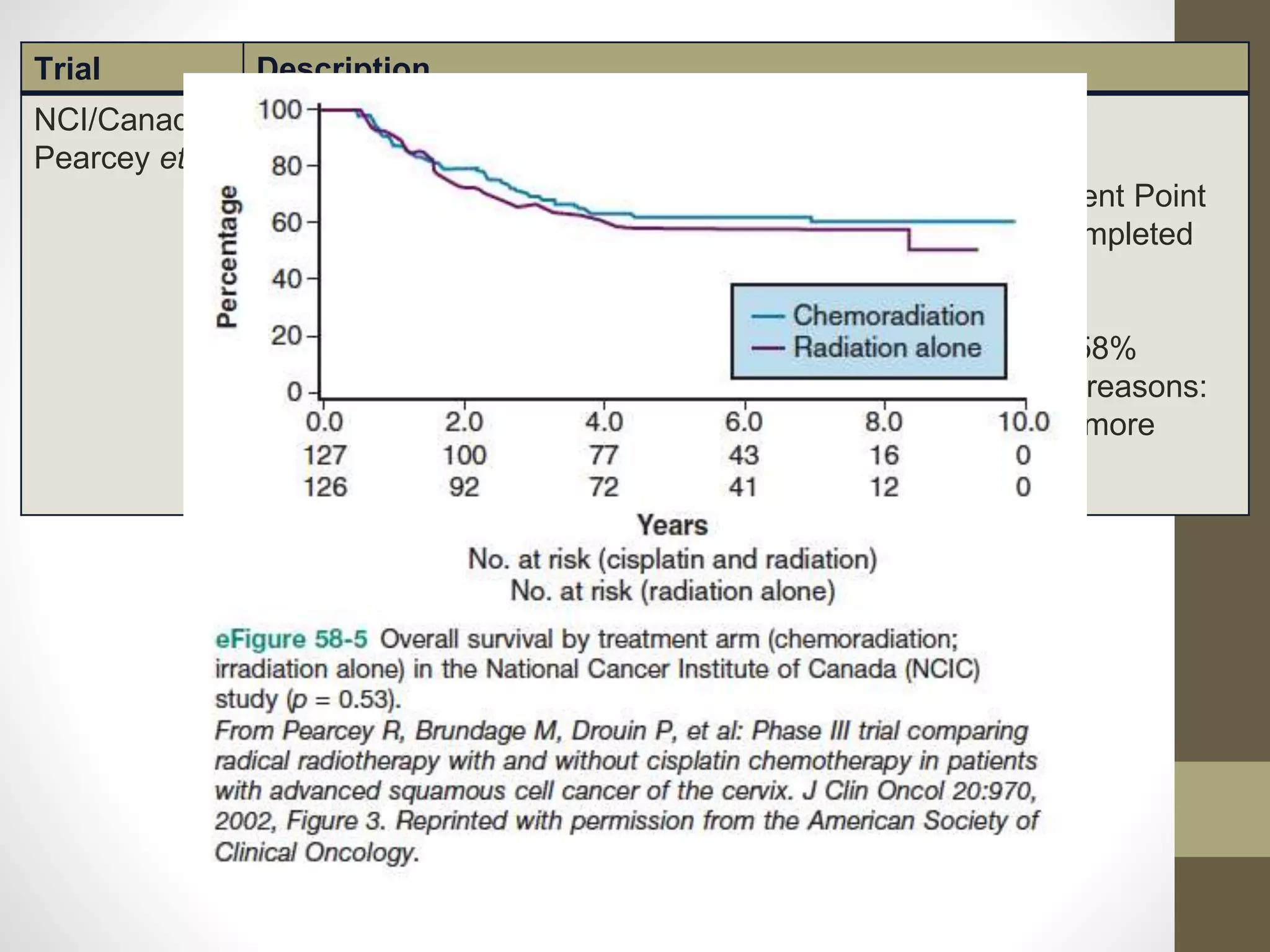
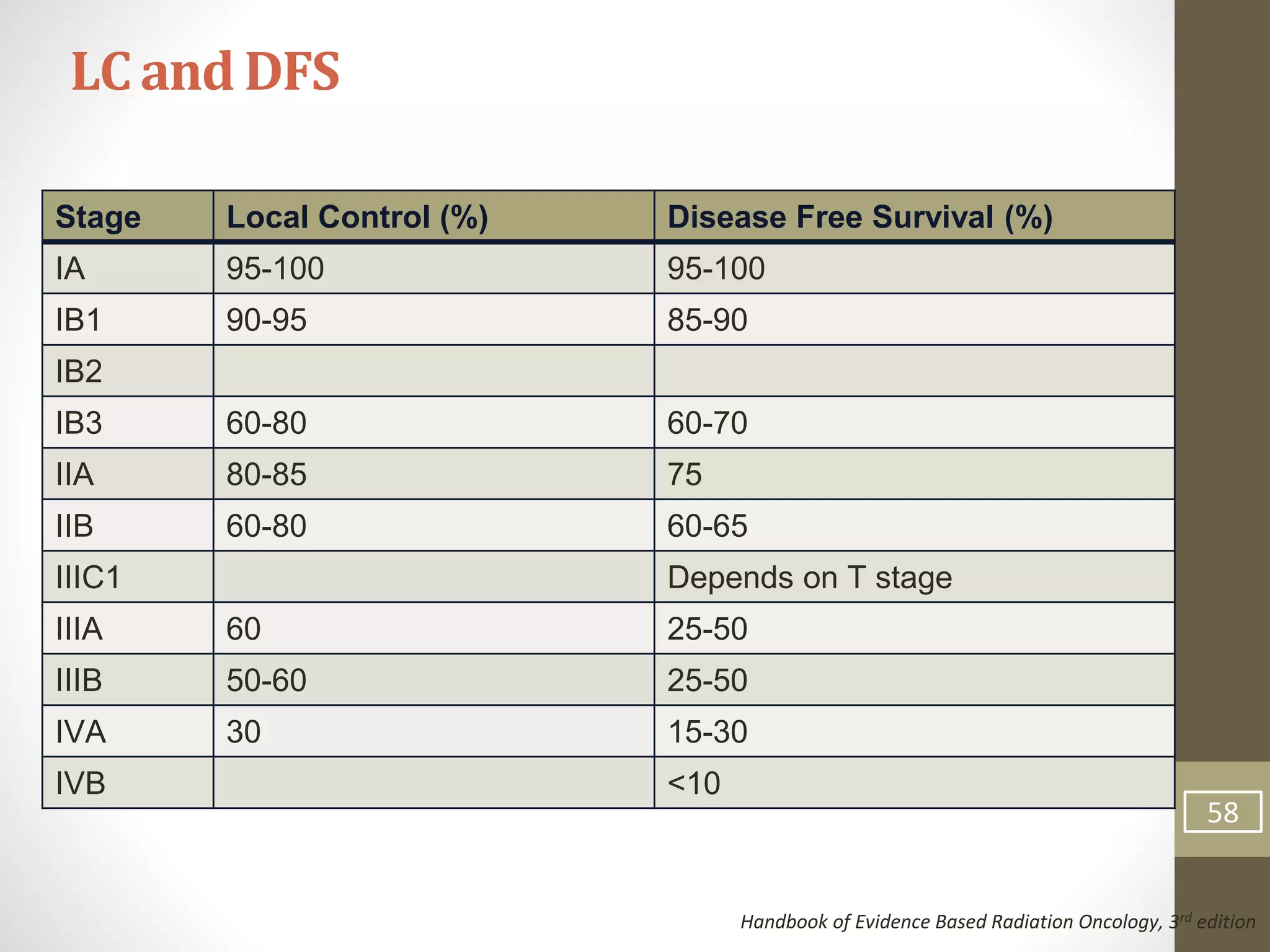
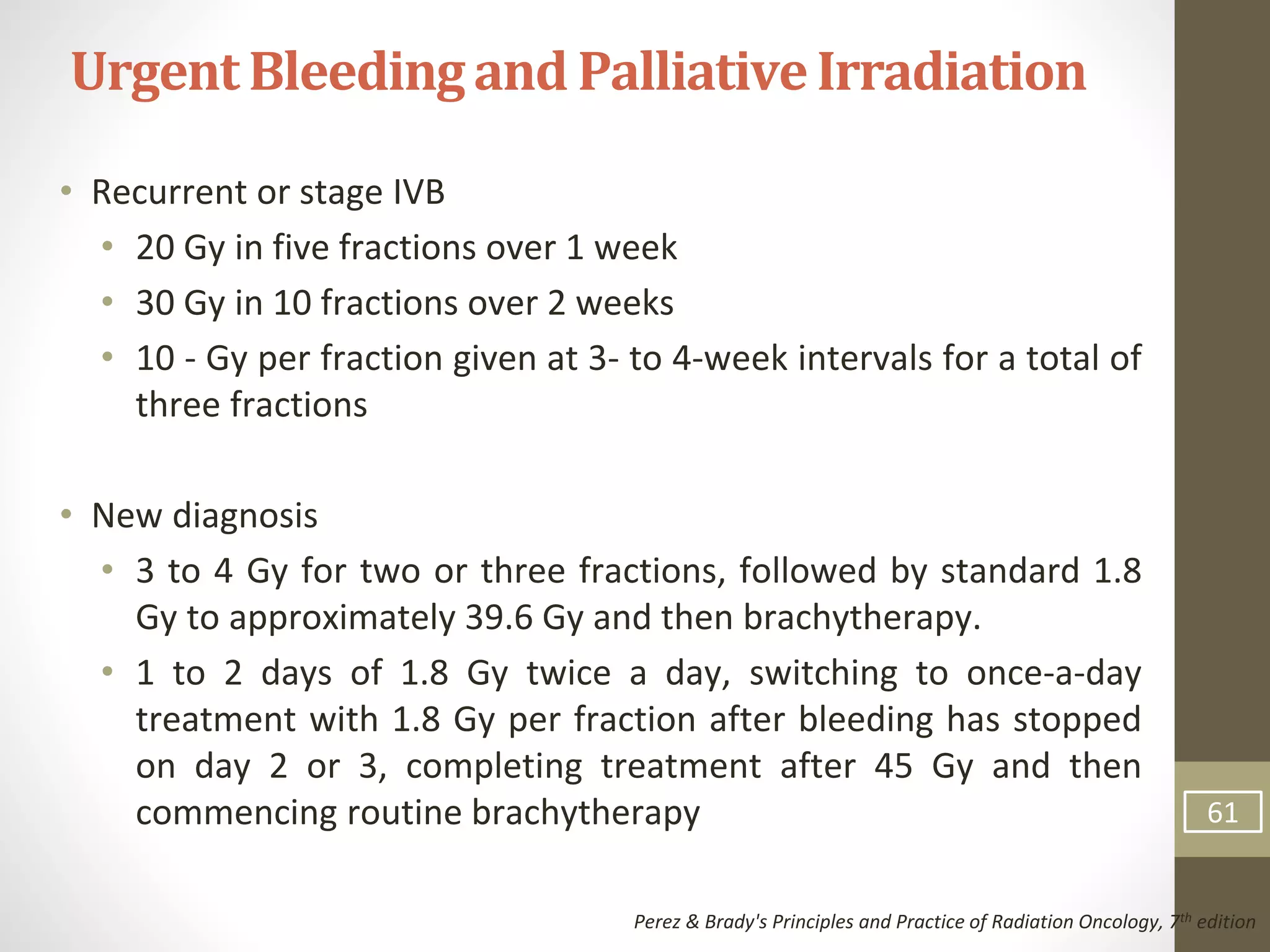
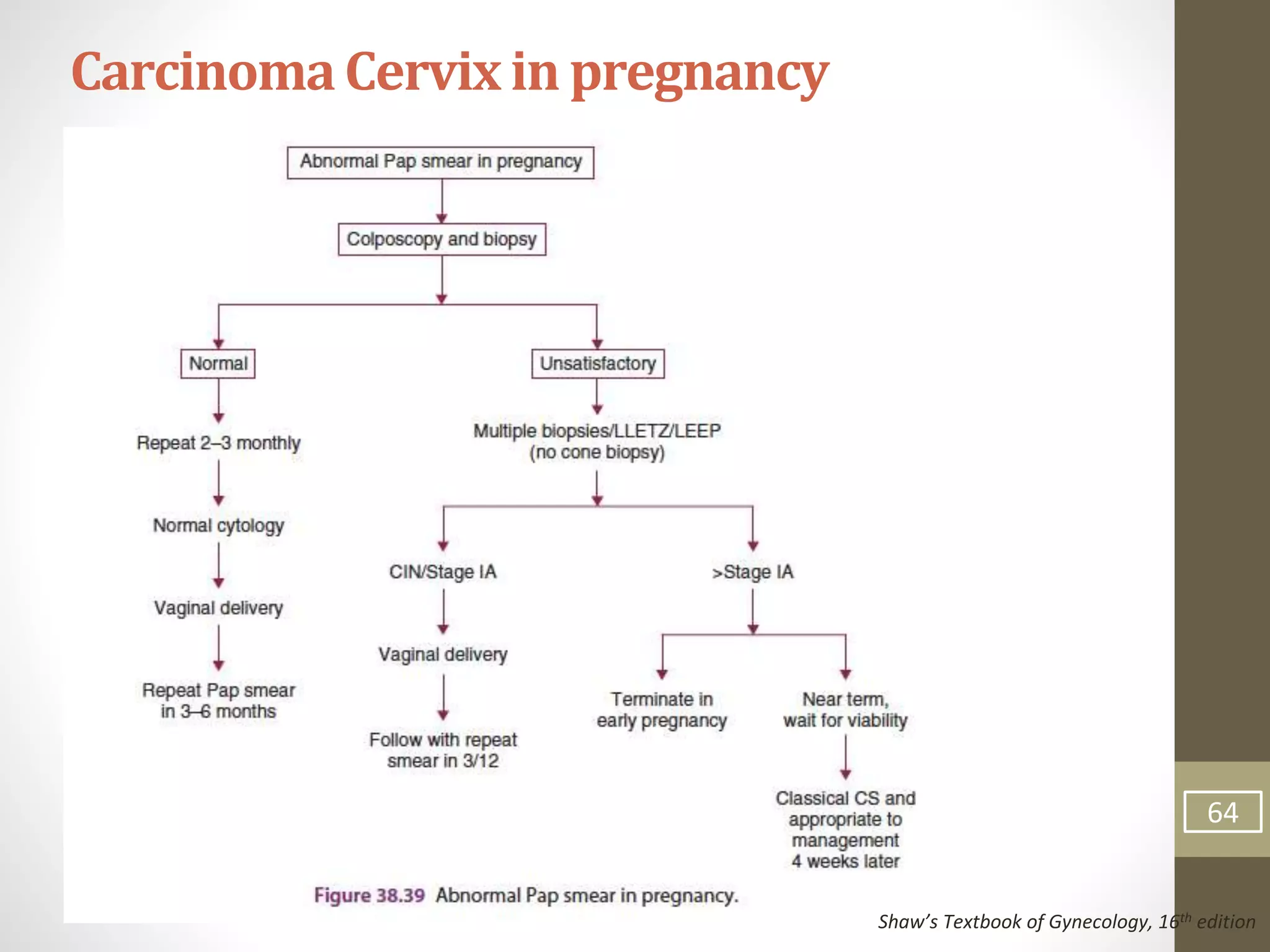
This document summarizes the management of carcinoma of the cervix according to the 2018 FIGO staging system and various medical textbooks. It discusses treatment options for preinvasive disease and early stage cervical cancer (Stage IA-IIA), including conization, loop electrosurgical excision, hysterectomy, and radiotherapy. For more advanced stages (IB3-IVA), the standard of care is described as concurrent chemoradiotherapy with cisplatin. Several landmark clinical trials are summarized that demonstrated improved survival outcomes with the addition of chemotherapy to radiotherapy.